Saudi Diabetes and Endocrine Association, Saudi Arabia
Background and Objectives:
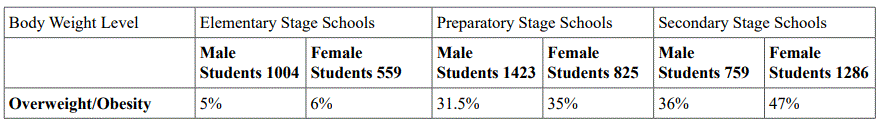
Method: Saudi Diabetes and Endocrine Association have measure BMI for male/female students to 20 schools (10 for males and 10 for femalesʼ including elementary, preparatory and secondary stages). The number of students enrolled in study were 6,171 (3,421 males and 2,750 females).
Result:
Discussion and Conclusion:
1. There is a low rate of overweight/obesity (5% for male students and 6% for female students) among the students in the elementary schoolsʼ stage.
2. The overweight/obesity rate has increased in the preparatory schoolsʼ stage and reached 31.5% for malesʼ students and 35% for females students.
3. The overweight/obesity rate has furtherly increases in the secondary schoolsʼ stage and reached 36% for malesʼ students and 47% for females students.
4. An action planwas developed to limit the fatty and salty snacks in the schoolsʼ canteens with more of educational programs for students, their families and teachers about health and strategies to combat obesity among students in this Kingdom of Saudi Arabia including performing one hour of physical activity per day, and to limiting TV/screen times.
Health Medical Clinics, Saudi Arabia
Almost a third of the adult population in Saudi is obese and of those 18% deserve to undergo bariatric surgery. Only 2% of those eligible present for bariatric surgery. The primary reason to undergo bariatric surgery in Saudi Arabia remains to be weight reduction and improvement of the quality of life (80%) rather than resolution of co-morbid conditions (18%). The health care delivery system is a combination of governmental, employer sponsored and third party payor. While care for chronic illnesses is mandated by law, bariatric surgery is not covered by most insurance providers limiting affordability but recent drop in cost due to competition has helped improve access to surgery.
Endocrinologists have been reluctant to refer patients for bariatric surgery due to short and long term safety concerns of bariatric surgery. Endocrinologist have been troubled by the ineffectively of band surgery which was the only procedure available during the 90ʼs and when more radical effective procedures with mal absorption were introduced, early complications during the learning curve and long term serious macronutrient and micronutrient deficiency and lack of surgical follow up in delayed surgical complications have caused them to be more reluctant to refer patients. The introduction of sleeve gastrectomy has solved many of these issues reducing nutritional deficiencies and long term surgical complications. The surgery community has been liberal in applying the new guidelines in low BMI The recent guidelines of offering metabolic surgery in diabetics with low BMI and even the new trend. A unique subset of patients are type 1 diabetics who are morbidly obese and the results in these patients have shown the importance of early post operative glycemic control and that there weight loss is identical to non diabetic patients.
Biography:
Dr. Osamah Alsanea graduated with honors from Kuwait University. He completed his did and early surgical training at King Faisal Specialist Hospital in Riyadh then was awarded a scholarship to complete his surgical training at Tufts University, Boston. He obtained a fellowship in Minimally Invasive Surgery under the Dr. Schwaitzberg past president of SAGES and Dr Shikora past president of IFSO then completed a completed a fellowship in Endocrine Surgery under Dr. Clark past president of AAES and ATA at UCSF California. Dr. Alsanea practice emphasizes minimally Invasive, bariatric and Endocrine Surgery in the first dedicated multidisciplinary diabetes therapy center
Saudi Diabetes and Endocrine Association, Saudi Arabia
Background and Objectives: For the past three decades the prevalence of overweight and obesity has increased dramatically worldwide, and becomes a global epidemic with more than one in five people qualifying as obese, at the same time, there has been a rising trend of obesity in the kingdom of Saudi Arabia which places it among the highest nations. The kingdom experienced a shifting from its cultural food to fatty-sugary-westernized food during the past few decades which has contributed to obesity among all generations.
The obesity exposes the individuals at higher risks of many non-communicable diseases, including diabetes type 2, cardiovascular disease, stroke, hypertension and some types of cancers.
Method: Saudi Diabetes and Endocrine Association has conducted this study to measure obesity rate among Saudi women, and developed a six month lifestyle, nutrition and physical activity program for weight management.
The participants were assessed nutritionally, anthropometrically and medically prior, during and at the end of the program, targeting 10% weight loss goal to the end of the program.
Results: 160 women with age between 20-40 years were enrolled in the program and assessed, and the overall prevalence of overweight and obesity was as follow, noting that 85% of the participants have achieved their set goals.
Conclusion: The study has shown high prevalence of overweight and obesity among younger group of Saudi women due to excessive caloric intake and lack of physical activity, noting that the majority of Saudi population is less than 30 years old at present time and accordingly, itʼs expected that the magnitude of obesity will be bigger in near future which mandates establishing of age specific obesity awareness programs for Saudi population and implementing preventative strategies to combat it.
Biography:
Dr. Basem Mohammed Futa is Head of ‘Nutrition and Health Education Committee of Saudi Diabetes and Endocrine Association, Kingdom of Saudi Arabia (KSA). He completed his PhD in Nutrition, UK. He is a Blood Donation Ambassadorʼ from the Saudi Society for Promoting Organ Donation and a Professional Member in many national, regional and international healthcare associations, such as Saudi Diabetes and Endocrine Association, Saudi Cancer Foundation, Saudi Kidney Foundation
Health Medical Clinics, Saudi Arabia
More than two thirds of the adult population in Saudi Arabia are overweight and one third are obese. It is estimated that 4% of the adult population in Saudi Arabia are eligible for bariatric surgery based on weight criteria only and 9% are eligible if reversible metabolic disorders are included. Open bariatric surgery in Saudi Arabia started in the eighties with open Vertical banded gastroplasty. In 1993, laparoscopic gastric banding was introduced in Europe, and soon after was performed by Dr. Bukhari and Dr. Madani in Saudi Arabia. The first international laparoscopic gastric bypass surgery was performed in 1994 by Dr. Wittgrove in San Diego but was delayed in Saudi till 2000. Successful gastric bypass was performed in 2001. Perceptor and Proctorship Visiting bariatric surgeons influenced the type of surgery performed in different centers. Laparoscopic bilio-pancreatic diversion (Scopinaro Procedure) began earlier than gastric bypass based and resulted in significant weight loss and resolution of comorbid conditions but with a high price to pay due to severe nutritional deficiencies. Roux- Y gastric bypass became popular in th enew millenium with the return of western qualified young surgeons and the results were encouraging that made it the number one procedure for over a decade replacing Scopinaro and band surgery. Since 2007, Sleeve gastrectomy became the most popular gained momentum and in 2012 became the number one procedure in. Saudi. Worry about long term small bowel complications from R Y gastric Bypass and difficulty in addressing weight regain after the procedure and the simplicity with which one anastomosis gastric bypass can be performed has made the latter the more popular procedure second Sleeve thus far. Many lesser invasive but ineffective trial procedures including endoscopic procedures continue to be performed in a newly regulated heath care system but they fade quickly.
Biography:
Dr. Alsanea graduated with honors from Kuwait University. He completed his did and early surgical training at King Faisal Specialist Hospital in Riyadh then was awarded a scholarship to complete his surgical training at Tufts University, Boston. He obtained a fellowship in Minimally Invasive Surgery under the Dr. Schwaitzberg past president of SAGES and Dr Shikora past president of IFSO then completed a completed a fellowship in Endocrine Surgery under Dr. Clark past president of AAES and ATA at UCSF California. Dr. Alsanea practice emphasizes minimally Invasive, bariatric and Endocrine Surgery in the first dedicated multidisciplinary diabetes therapy center
International Association of Sport Kinetics, Poland
Contemporary man no longer listens to signals which his organism sends to inform him about his needs. Man has started to act against his own good, indulging into improper, i.e., physically inactive, life.
The aim: of the paper is to a) indicate to possibility to diagnose manʼs state of health on the basis of his movement activity; b) point out the importance of movement activity and its conditioning for the improvement of manʼs health.
Conclusions: 1. Movement activity is manʼs biological need and indispensable component of his life to guarantee the maintaining of good health.
2. Movement activity should accompany man all through his life.
3. On the basis of manʼs movement activity, and in particular the quality of performing movements, it is possible to evaluate the level of his movement coordination.
4. Movement activity adequate to manʼs possibilities, strengthens manʼs health.
5. Movements should be accompanied by various kinds of respiration suitable for the changing character of exercises and their intensity.
6. Kinds and intensity of movement activity depend on age.
7. Kinds and intensity of movement activity depend on the particular character and system of movement education and tradition popular in a given country. Europeans could follow patterns of movement activity popular among inhabitants of Japan or China.
Keywords: movements, health, life, respiration, age, body weight, movement education.
Biography:
Prof. Dr. habil., Dr h.c. Wlodzimierz Starosta. Education: University School of Physical Education in Poznan (Poland) 1951-1952; Institute of Physical Culture in Leningrad (Soviet Union) 1952-1956; Institute of Physical Culture in Leningrad Ph. D. -1963; University School of Physical Education in Warsaw (Poland) habilitation (second doctor degree)- 1977. Full prof. from 1990. Visiting Professor: University School of Physical Education in Moscow; University Saarbrucken, Greifswald and Magdeburg (Germany); Zagreb (Croatia); Ljubljana (Slovenia); Izmir (Turkey); Preśov (Slovakia), Tartu (Estonia), Bologna and Urbino (Italy); Italian Olympic Committee. Membership of professional bodies: International Society of Sport Genetic and Somatology (general secretary) 1983-1990; International Association of Sport Kinetics-IASK (president) 1990-2011; member of Executive Board and Regional Coordinator Eastern Europe of ICSSPE (2004-2008); International Ringo Federation (president from 2004). Doctor honoris causa of Open International University for Complementary Medicines in Colombo (1996); Meritorious professor of Kinesiology Faculty of University of Zagreb (2009); Distinguished Service Award of United States Sport Academy (2015). Honorary member of: International Academy of Integrative Anthropology, Academy of Science of Technological Cybernetics of Ukraine, International Academy of Gerontology, Politechnical Academy of Belarus. Editorial Committee of journals: “Human Kinetics”; “Biology of Sport”; „Acta Kinesiologiae Universitatis Tartuensis”; “Kinesiology”; “Kinesiologia Slovenica”; “Studies in Physical Culture and Tourism”; “Anthropomotorics”; “Sport Medicine”; “Acta Facultatis Educationis Physicae Universitatis Comenianae”. Publications: over 800 research papers publish in 32 countries of the world including 60 Monographs in Polish, English, Italian, Russian, German. Personal Achievements in sport: sportsmen in 20 sport disciplines, in 12 classified. Greatest achievements in ice figure skating, wrestling and ringo (18 medals on International Polish, European and World Championships). Coach 1 class in ice figure skating – practicing 20 years as a coach.
University of Chicago, USA
Up to a third of adults in Europe and more than one-third of adults in the United States suffer from the disease of Obesity. Obesity is intimately linked with many of the most common chronic illnesses like hypertension, hyperlipidemia, heart disease, sleep apnea, stroke, type 2 diabetes and 13t types of cancer. Despite the prevalence and impact of Obesity, many physicians report insufficient training in obesity management. This session will offer participants the opportunity to learn about obesity pharmacotherapy and their role in weight management. When used appropriately and in combination with lifestyle modification, pharmacotherapy has an important role in the treatment of obesity and improves both short-term and long-term outcomes. The session will cover the efficacy and risks of the drugs currently approved for obesity, with reference to the main clinical trials, clinical practice guidelines and consideration when using anti-obesity drugs, with emphasis on recently approved drugs.
Additionally it will give a brief overview on drug induced weight gain and suggest that knowledgeable prescribing of medications, choosing whenever possible those with favorable weight profiles, can aid in the prevention and management of obesity.
University of Calgary in Qatar, Qatar
Obesity is a global public health problem The World Health Organization (WHO) estimates that there are more than 1 billion overweight adults, of whom at least 300 million are considered obese, the state Qatar like all other high income, oil-producing countries has also affected. Qatar has placed significant collective efforts and enormous resources to combat this health issue and prevent its complications, in my talk I will measures, initiatives, and national programs that been established in Qatar at both organizational and national level in response to high prevalence of obesity in the country (published work).
Biography:
Dr. Rasmeh AL- Huneiti is Clinical Guidelines Specialist in Healthcare Quality and Patient Safety Department in Ministry of Public Health in state of Qatar and Adjunct Professor in Calgary University Qatar. She graduated from University of Jordan, 1991 with Bachelor in General Nursing. Her post basic qualifications include; Diploma in Primary Healthcare 1995, Master in General Nursing Education 1999, International Diploma in HR Management, 2009, and PhD in Medical Education from Brunel University in UK.
She developed an E-learning Model for E-health Education in Developing Countries. Rasmeh has many yearsʼ experiences in a variety of challenging roles, including clinical nursing, education, administration, training and staff development and regulation, research, and clinical guidelines development. She is a volunteer in Qatar Red Crescent Society and Reviewer and Editing Board member in many international conferences and peer reviewed Journals she published her research work internationally.
Ministry of Health and Quality of Life, Mauritius
Introduction: The findings of the continuing rise in the prevalence of obesity in Mauritius mandates that current obesity prevention activities are reviewed against the worldʼs best practices as established both in developed and developing countries
Obesity Prevention Programme:
A National Service Framework for Diabetes has been developed for the prevention, treatment and control of diabetes in Mauritius A Mobile Clinic Programme has been implemented to carry out screening for NCDs in the Community / Worksite / Secondary School Physical Activity Programme is being enhanced
Empowerment Programme are organized to empower Health Personnel and Community Health Leaders
Some of the sensitization programs are also backed up by the media campaigns
Sensitization Campaigns are organized regularly to sensitize the community at large
National Plans of Action on Physical Activity and Nutrition have been developed
Findings of the Mauritius Type 2 Diabetes Prevention Study which was a 3-year study
Achievements:
The prevalence of Diabetes has remained stable
Pre-diabetes has declined
There is an increase in prevalence in physical activity among both male and female adults aged 20 to 74 years.
Conclusions: Various measures for the prevention of obesity in Mauritius have been undertaken. However, though some positive points have been noted, yet more efforts are required to combat obesity in Mauritius.
Biography:
Mr Sudhir Kowlessur, Chief Health Promotion and Research Coordinator is the Head of NCD and Health Promotion Unit at the Ministry of Health and Quality of Life, Mauritius. He is responsible to coordinate NCD and Health Promotion Activities at National Level. He is also involved in research and training programmes. Mr S. Kowlessur holds a MA in Health Promotion and Communication from Middlesex University, UK. He has been actively involved in the Mauritius NCD / Nutrition Surveys since 1987 and he also coordinated the Mauritius Type 2 Diabetes Prevention Study (2013 – 2016). He participated and made presentations at several International Conferences as follows: Diabetic Summit, Nairobi in Kenya, 5th World Congress on Prevention of Diabetes in Helsinki, Finland, 20th World Diabetes Congress in Montreal, Canada, 6th World congress in Prevention of Diabetes in Dresden, Germany, 7th World Congress on Prevention of Diabetes and its Complications, Madrid, Spain, 8th Global Conference on Health Promotion, Helsinki, Finland, World Diabetes Congress, Melbourne, Australia, 8th World Congress on Prevention of Diabetes and its Complication, Colombia, 9th World Congress on Prevention of Diabetes and its Complication, Atlanta, USA, World Diabetes Congress, Vancouver, Canada. Mr Kowlessur is the Co-Author of publications resulting from analysis of data on the Mauritian studies on Diabetes / NCDs in several journals such as the International Journal of Cancer, Obesity Journal, Bio Med Research International Journal, Epidemiology / Health Services research Diabetes Care Journal, among others. He is also the recipient of First Prize for its creative and innovative solutions provided in the struggle against NCDs at the All Africa Public Sector Innovation Award 2010.
Shanghai Jiaotong University, China
Keywords: Severe Obesity, Thinness, low Birth weight, Children
Background: The aim of this study is to investigate the relationship between low birth weight (BW) and thinness or severe obesity during maturation.
Methods: A large-scale school-based cross-sectional population-based survey was conducted in 3 to 12-year-old children in Shanghai, China. BW was divided into low (< 2500 g) and normal (2500–4000 g) group. International Obesity Task Force BMI cutoffs were used to define grade 1, 2, 3 thinness, overweight, obesity and severe obesity. Logistic regression was used to estimate the association.
Results: Total 70,284 children participated in the survey. The percentage of grade 1 thinness and severe obesity in children with low birth weight is significantly higher than that with normal birth weight (P < 0.05). Low BW correlated with an increased risk of grade 1 thinness (OR = 1.56, 95%CI = 1.38–1.75), grade 2 thinness (OR = 1.34, 95%CI = 1.10–1.64), grade 3 thinness (OR = 1.99, 95%CI= 1.63–2.42) and severe obesity (OR = 1.27, 95%CI = 1.03–1.55) but did not correlate with overweight.
Conclusion: The relationship between low BW and thinness or severe obesity risk is associated.
Sina Hospital, Iran
Aim: The aim of this study is to show: is weight loss secondary to restrictive bariatric surgery although completely different to just diet, physiologic and can body composition after 6 months of operation, be accepted as a normal physiologic condition or not?
Method: The protein mapping of 30 morbid obese patients calculated by high performance liquid chromatography before and after 6 months of operation. Body composition of patients checked as well. The rate of weight loss and the changes of body composition and protein mapping analyzed.
Result: The mean weight before and after 6 months of operation was 116 and 79. The mean BMI was 44 to 30. Fat percentage 46.1 to 28.3 and predicted muscle mass was 33.3 to 30.1. The body composition after 6 months of gastric plication was highly suggestive to normal, very superior to pre operation condition. About 10% of protein was lost due to protein catabolism secondary to aggressive calorie restriction
Conclusion: Although the rate of weight loss is too much faster in compare to diet and exercise, it is physiologic and is the result of hormonal changes based on change of protein mapping due to accelerated lipolysis. It is with 10% protein lose which can be controlled by at least 100 gr protein intake daily. Exercise has shown increase the muscle mass and decrease the risk of protein catabolism during rapid weight loss.
Biography:
Dr. Mohammad Talebpour was born at Tehran, Iran, 1964. He passed general doctorate and general surgery in Tehran University of Medical science (TUMS) from 1982 to 1993. He is faculty of TUMS from 1994 up to know. He has started basic laparoscopy from 1994. He passed active fellowship of advanced laparoscopy at Ninewells Hospital, Dundee, UK under supervision of Prof Cuschieri and at IRCAD Center under supervision of Prof Marescaw and Prof Leroy at 1999. He has started advanced laparoscopy from 2000 including bariatric surgery. He introduced gastric plication as the new novel physiologic restrictive bariatric method at 2000 and has the most experience in this field during 18 years with about 2000 cases. He is associate Prof and head of laparoscopic ward in TUMS, Sina Hospital, Tehran, Iran. He is a member of IFSO, IEF and IAS. He is a delegate of Iranian IFSO branch. He has published 25 papers, presented up to 100 oral lectures and was invited speaker in 18 international meetings.
1ALS Taranto, Italy
2ASL Savonese, Italy
3ASL Brindisi, Italy
4National Institute for Gastroenterologic Disease, Italy
Background: Nephrolithiasis is a widespread disease: the prevalence is estimated to be 7-13% in North America, 5-9% in Europe, 1-5% in Asia. Obesity and Arterial Hypertension are associated with NL, with high acute and chronic morbidity.
Aim: Demonstration of: a) Correlation between O, AH, NL; b) Correlation between NL and high salt intake, fructose drinks, water intake.
Methods: This study has recruited a sample of 1086 adolescents (age: 15.6÷24.6) of both sexes (M:478, F:598). All the patients have been examined as follows: BP, HR, BMI, WC, urinalysis (fresh sample), kidney ultrasound. The sample has been split in case (NL) (157: M 43.9%, average age: 17.75±0.88) control (354: M 45.8%, average age: 17.77±0.84), administering a survey: sport; daily water intake; high sodium, oxalates, urates, fructose foods.
Results: BMI: 22.8% >25 (Overweight/Obesity); WC: 10,2%, compatible with abdominal obesity; BP: 11.0% >140/90 [M: 3.98 (p< 0.0001; age: 1.028 (p=0.75); O: 1.859 (p< 0.05)], showing correlation with Obesity. Urinalysis: 11.4% albuminuria; 24.3% hematuria. Multivariate analysis has not shown correlation between NL, AH, O, tap or mineral water, sport, food (high-sodium, fructose, oxalates, urates). Correlation between NL and daily water intake <1 lt. Correlation between Obesity (7,4%) (case-control) and sugary snacks (OR: 1.19; IC:028-4.99), but not with sugary and carbonated drinks (OR: 3.16; IC: 055-18.27).
Conclusions: In adolescents NL is related to pathological alterations but not to glucose, lipid and protein metabolism. On the contrary, metabolism disorders are the main determinant of NL in adult population with increased cardiovascular risk. Primary prevention is therefore important: in Primary Care the adolescents should be encouraged to avoid the risk factors for the development of these diseases with a healthy lifestyle.
Biography:
Since 1984, Dr. Giovanni Colucci carries out the activities of General Practitioner in Martina Franca, and since 2001 operates in association Medica network with nine other colleagues. Animator Training in General Practice since 1998 Physician General Tutor since 1998 Researcher SIMG Network for Pharmacovigilance active Farma Search 2002. Co-author of the guidelines SIO (Italian Society of Obesity) Apulia. Collaborated in the research activities, updating and training carried out by the Department of Clinical Pharmacology and Epidemiology at the Mario Negri Sud Consortium in the area of General Medicine (2007/13). Founder / coordinator of the “Supplementary Training Project for the Degree Course in Nursing Students Training Centre IRCCS Castellana Grotte”. Course Tutoring students at the family doctor (Martina Franca). Co-author of the guidelines SIO (Italian Society of Obesity) Apulia: Guide lines for physical activity aimed at the prevention and treatment of overweight and obesity in adulthood. Author and coadjutor of 103 publications on national journals, conference proceedings, a popular science brochures and compact disc (C. D.)
1Muhammad Nawaz Shareef University of Agriculture, Pakistan
2University of Agriculture, Pakistan
3University of Animal and Veterinary Sciences, Pakistan
Low fat Cheddar cheese is the demand of present era, but lacks the quality and functionality. Guar gum shows stability during freeze-thawing cycles and it can retard ice crystal growth by slowing mass transfer across solid and liquid interfaces. Guar gum is added to low fat milk to maintain texture and rheology of cheese similar to full-fat cheese. Guar gum was used at 0.15, 0.30 and 0.45% in Cheddar cheese with 2% fat level of milk. The result regarding analysis of variance for low fat Cheddar cheese revealed highly significant (p<0.01) effect on gumminess and chewiness and Significant (p<0.05) effect on hardness, melt-ability and yield. Cohesiveness, springiness and flow-ability showed non-significant (p>0.05) effect of different levels of guar gum. By increasing the level of guar gum, cheese become softer, maximum hardness was found in cheese with less concentration of gum. Gumminess and chewiness decrease by increasing the level of gum. Melt-ability and flow-ability increased by increasing gum level. The decrease in hardness of cheese containing guar gum was probably due to change in protein matrix compactness since addition of guar gum increases water binding capacity of protein matrix. Decrease in fat with incorporated fat mimetic ingredients could increase protein water interaction enhancing adhesiveness in cheese. Scanning electron microscopy results showed that cheese with guar gum has better texture as compared with other samples, it shows more homogeneous structure. The addition of guar gum as fat replacement improved the sensory characteristics of low fat cheese samples when added up to the level of 0.45% guar gum.
Keywords: Cheddar cheese, Gumminess, Chewiness, Melt-ability, Flow-ability
Technion-Israel Institute of Technology, Israel
Obesity is a common problem among women of reproductive age. According to the World Health Organization (WHO), if the body mass index (BMI) equals to or is greater than 25 kg/m2, it is considered overweight, whereas if the BMI equals to or is greater than 30 kg/m2, it is considered obesity. Obesity plays a significant role in reproductive disorders, particularly in women. It is associated with anovulation, menstrual disorders, infertility, difficulties in assisted reproduction, miscarriage, and adverse pregnancy outcomes. Moreover it brings out many problems such as social, psychological, demographic, and health problems. It is related to increased health risks such as diabetes mellitus, hypertension, coronary heart disease and is linked to various malignancies, particularly endometrium, breast, and colon cancers. Obesity is a complex disease resulting from the interactions of a wide variety of hereditary and environmental factors. The combined progress in quantitative genetics, genomics and bioinformatics has contributed to a better understanding of the genetic and molecular basis of obesity. Moreover, environmental factors can affect pregnancy and may cause epigenetic changes in the fetus leading to obesity and its complication in the later life. The new concepts of the etiology of obesity, its impact on fertility and general health will be briefly discussed.
Biography:
Dr. Adrian Ellenbogen, Clinical Ass. Professor in Obstetrics and Gynecology at the Rappaport School of Medicine, Technion Israel Institute of Technology, Haifa, Israel, Founder and Director (retired) of in vitro fertilization unit at Hillel Yaffe Medical Center, Hadera, Israel. Fertility Advisor and Head- Fertility Clinic, Meuheded Female Health Center, Bnai-Brack, Israel, Director of the postgraduate course in Obstetrics Gynecology and Infertility, Rappaport School of Medicine, Technion- Israel Institute of Technology, Haifa, Israel. He is a Member of many international (ASRM, ESHRE, ISMAAR, ISIVF, ISGE) and national societies (Israeli Fertility Association, Israeli Society of Obstetrics and Gynecology). Editorial Board Member of the Journal of Reproduction System & Sexual Disorders.
Reviewer: Fertility and Sterility, the Journal of Reproduction System & Sexual Disorders, Harefuah, IVF Lite, Dr. Ellenbogen presented more than 110 lectures in different international and national scientific meetings and published many peer review papers in top rated scientific journals.
Received 2003 Israeli Ministry of Health and Israeli Civil Service Commission Award for Excellency in labor.
Receives 2012 and 2013, 2014 and 2015 Star Award of American Society of Reproductive Medicine.
Nepalgunj Medical College Chisapani, Nepal
Purpose: Obesity is associated with metabolic risk factors such as high blood pressure, blood fat abnormality, and glucose intolerance which may influence the morbidity and mortality of cardiovascular diseases. Beside being a risk factor for cardiovascular disease, certain cancers and type II diabetes, obesity has also been associated with change in autonomic function in human. Although a lot of progress has been achieved in past decade on accessibility and awareness about health, the obesity remains impending and burgeoning health concern in Nepal. With this trend, we can foresee that the Body Mass Index (BMI) one of the commonly used indirect measure of obesity might potentially turn out to be one of the leading factor of autonomic dysfunction.
Methods: 100 healthy subjects were screened and divided into 2 groups- Group I(BMI>30) and Group II (BMI< 30). Height was measured by stadiometer with subjects having their shoes removed. Weight was measured with weighing machine in light clothes. BMI was calculated using the formula: BMI= weight (kg)/ height (m2)
Resting heart rate (RHR) was recorded with Lead II of ECG. Blood pressure (BP) and Heart Rate (HR) were recorded in supine position and on immediate standing. Cold pressure test: Resting BP was recorded in sitting position. Then the subjects were asked to immerse the hand in cold water, and the BP was measured from other hand. Data was analyzed using SPSS 16 (Statistical Package for Social Science).
Result: Our result showed that RHR of Group I (79.32 ± 4.22) was higher than that of Group II (74.38 ± 7.26). However, on student –T test, BP and HR response to immediate standing (P =0.34&P=0.23 respectively) were non-significant between obese and non-obese person. When the correlation was done for the change in BP in response to cold pressor test in between obese and non obese person it was found to be significant (P = 0.04).
Conclusion: Our data suggests that the BMI can be a predictor of autonomic dysfunction.
Keywords: Body Mass Index, Autonomic Function, Resting Heart Rate, Cold pressortest
Charles University, Czech Republic
Overweight and/or obesity is a growing problem over the world. Alongside a range of health problems associated with increased body mass (BM) – adiposity and reducing of fitness level it is an important limiting factor for realization of regular physical exercise and quality of life. The study goal was to assess the effect of movement intervention in women differing in the BM. Study was carried out in 42 women with normal BM (mean age=42.6±3.6 years; BM=69.3±3.7 kg; height=167.5±4.6cm; %BF=25.1±2.5%), 40 overweight women (42.0 ± 2.9; 80.9±3.9; 169.1±4.0; 28.9±2.9%) and 38 obese women (43.8±3.0; 90.4±4.6; 168.3±3.5; 32.1±3.4%). Body composition was assessed by bioimpedance method using prediction equations that are valid for the Czech middle aged women population, functional variables were assessed on a treadmill. The energy content of weekly movement program for women with normal BM ranged from 990 kcal to 2350 kcal (mean 1590±350 kcal) in females with overweight from 1230 kcal to 1980 kcal (1640±290 kcal) and in obese women from 1510 kcal to 2180 kcal (1780±370 kcal). Reduction in %BF ranged from 15.6% in obese to 16.4% in normal BM of starting value and in VO2peak increased from 13.9% in normal BM to 15.7% in obese. In middle aged women differing in BM are absolute changes in adiposity and aerobic fitness like a result of imposed movement intervention substantively and statistically significant. On the contrary, differences in percentages of pre-intervention values are non-significant. We can conclude that an exercise program with a similar energy content, form and intensity causes the similar changes in adiposity and in motor and functional performance in women, differing in BM.
Biography:
Václav Bunc - graduated from Technical University Prague, professor in the Exercise Physiology from Charles University Prague Main topics: application of mathematical methods and models in PE and sport, using of biocybernetics by evaluation of physical fitness, exercise physiology, obesity reduction, functional and physical testing in laboratory and field, body composition, BIA methods, moving regimes for prevention in cardiac and obese patients. He is member of Czech and International scientific societies, head of many research projects, author of the great numbers of research reports.
Institute of Postgraduate Medical Education and Research, India
Introduction: The metabolic effects of obesity are a result of increased adiposity in the ectopic sites. Ectopic fat deposition in the liver, skeletal muscle and visceral adipose tissue promotes insulin resistance and increases cardiovascular risk. Epicardial adipose tissue (EAT) is the visceral fat of the heart. Increased EAT is a measure of ectopic obesity. Increased epicardial ectopic fat is proposed to increase the incidence of cardiac dysfunction by release of inflammatory adipokines which act in a paracrine and endocrine fashion. Indian phenotype is different in many sense, despite of low body mass Index (BMI), they have high abdominal and visceral fat, high insulin resistance, low level of adiponectin, high CRP, low HDL and high small dense lipoprotein and triglyceride. It has been seen that metabolic complications are more pronounce in same BMI Indian phenotype compare to western counterpart. The purpose of this study was to detect the presence and extent of left ventricular dysfunction in relation with EAT among patients with Indian phenotype and its correlation with already known metabolic parameters i.e. fasting insulin, LDL cholesterol, triglyceride level, BMI, waist circumference, inflammatory markers like hS CRP and uric acid.
Method: Overweight and obesity was diagnosed based on BMI (Body MassIndex) which is weight in kg divided by height in m2. All overweight and obese individuals were screened for obesity related complications and classified according to stage. Visceral obesity was diagnosed based on waist circumference (WC). The measurement of EAT thickness and left ventricular dysfunction was performed by transthoracic echocardiography. Biochemical and inflammatory parameters were assessed. Data thus obtained analysed by standard statistical software.
Results: Among 146 obese and overweight patients were assessed, the mean EAT thickness was 5.607 (SD 1.59). Patients having left ventricular diastolic dysfunction (LVDD) had a mean EAT thickness of 5.60 (SD 1.66) compare to 4.80 (SD 2.2) among normal persons (two-tailed P= 0.011,<0.05), which is statistically significant. Left ventricular Systolic dysfunction (LVSD) patients had mean EAT thickness of 6.33 (SD 0.94) compare to 5.35 (SD 1.58) in normal patients (tow-tailed P=0.0001, <0.05), that is statistically significant. Moderate insulin resistance patients had a low mean EAT compare to sever insulin resistance patients. Mean EAT was poorly correlated with waist circumference and BMI in this study. EAT thickness was significantly correlated with LVDD and LVSD, even after adjusting for other cardiometabolic risk factors such as age, systolic blood pressure, BMI, blood glucose and LDL cholesterol and triglyceride.
Conclusion: Greater EAT is found in subjects with higher insulin resistance. EAT is significantly associated with LVDD and LVSD even after adjusting for other risk factors. Waist circumference, although a marker of visceral adiposity was poorly correlated with EAT as patients even with low WC had higher EAT same as to say for BMI. It can certainly be said that EAT is an individual risk factor for LVSD and LVDD after adjusting all known risk factors among patients with Indian phenotype.
King Abdulaziz University, Saudi Arabia
Background: In Saudi Arabia, the prevalence of obesity has dramatically increased and affects more than half the population in all age groups. One of the prevalent treatment options for obesity include bariatric surgery and Saudi Arabia is the fifth in order country that perform bariatric procedures. Registered dietitians (RDs) are members of bariatric surgery teams and play a critical role in pre and post-operation stages. This study aims to evaluate the dietetics practice in the scope of bariatric surgery in Saudi Arabia.
Methods: A descriptive cross-sectional to evaluate dietetics practice and nutrition and dietetic services in the scope of bariatric surgery included registered dietitians and bariatric surgery patients from twelve governmental and private hospitals in Jeddah city.
Results: All RDs reported that their departments are not accredited by any of the international associations or organizations. All RDs are accredited by the Saudi Commission for Health Specialties (SCFHS), 81.3% (n=13) of dietetics staff those providing bariatric services are RDs, only one was general dietitian (GD) and two were diet Technician (DT). Fifty-percent (n-=8) of surgical RDs reported practicing in a specific field, of which 37.5% (n=3) are specialized in bariatric surgery. RDs (25.0%) seeing 3 to 10 patients/month and mainly they see bariatric only before operation. About 34%, (n=12) of patients reported never be seen by a dietitian, while 28.6% were seen by a dietitian before and after surgery. The majority of patients 77.8% (n=21) were satisfied about the delivered nutritional care plan by RDs and 60.7% (n=17) believe that RDsʼ involvement in their nutrition care was excellent.
Conclusion: This is the first study to evaluate nutrition and dietetics services delivered to bariatric surgery patients for obesity management and involved feedback surveys from RDs and bariatric patients to assess their satisfaction about the provided nutrition and dietetic services in Jeddah city, Saudi Arabia. Further studies are needed in different regions of Saudi Arabia to evaluate the dietetics practice in the scope of bariatric surgery and other scopes related to nutrition and dietetics
Kuwait University Faculty of Public Health, Kuwait
Chronic cardio-metabolic disorders such as type 2 diabetes mellitus (DM2) have become an uncontrolled epidemic and a burgeoning cause of morbidity and mortality worldwide. In 2011, more than 170 M people had a diagnosis of DM2 with projected increase to 366 M by 2030. The Arab world, the countries with the highest prevalence of DM2 are: Saudi Arabia, Oman, Kuwait, Bahrain and UAE, whilst the countries with the lowest prevalence are Mauritania and Somalia. This prevalence was significantly associated with high GDP per capita and energy consumption.
As a consequence of rapid increase in combustion of fossil fuels for power generation and transportation, air pollution (indoor and outdoor) has been deemed a major risk factor for death and disability particularly in rapidly developing countries of the world. Increasing evidence from the literature review supports the role of occupational and environmental chemicals in diabetes development. Both epidemiologic studies and experimental evidence support adverse cardio-metabolic consequences of air pollution exposure, including worsening of whole body insulin sensitivity, promotion of hepatic endoplasmic reticulum stress, brown adipose dysfunction, and peripheral inflammation.
Articles on the link between Diabetes and environmental and occupational exposures that were published up to 2017 were retrieved from Highwire, PubMed, Embase, Web of Science, Global Index Medicus, and Medline search engines. The culprit chemicals include toxic metals, persistent organic pollutants (POPs), and bisphenol A (BPA) which impact health at the cellular level, and they have been linked to the development of DM. The difference observed between countries in the Middle East with regard to the levels and trends in causes of DALYs (disability-adjusted life-years), LE (life expectancy), and HALE (healthy life expectancy) can be attributed to a myriad of determinants, including social, cultural, ethnic, religious, political, economic, and occupational and environmental factors as well as the performance of the health system.
Biography:
Dr. Janvier Gasana, MD, PhD, is a professor and chair of Department of Environmental and Occupational Health of Kuwait University Faculty of Public Health since January of 2016. Previous faculty positions were held for 4 years at the National University of Rwanda Faculty of Medicine and for 20 years at Florida International University in Miami, Florida. His research focuses on exposome which represents a concept that incorporates the complex environmental and occupational exposures we face as humans. The current specific focus is on the mounting evidence of link between environmental and occupational exposures and NCDs (Non-Communicable Diseases) including Obesity and Diabetes.
1Sun Yat-sen University, China
2The University of Hong Kong, China
The 2011 United Nations political declaration against non-communicable diseases (NCDs) targeted four major risk factors: tobacco use, harmful use of alcohol, an unhealthy diet, and a lack of physical activity. The Framework Convention on Tobacco Control (FCTC), MPOWER strategies, and the four-stage model of the tobacco epidemic are useful references for the prevention and control of other risk factors and NCDs. Obesity control is a more complex challenge. Herein we propose a stage of obesity epidemic model (SOEM). Obesity is in the early stages in most countries with increasing prevalence, but its effects on mortality will increase rapidly, even if its prevalence may have reached a peak and be declining. Based on current relative risk, obesity kills one in three obese people. Like tobacco, epidemiological studies of obesity in the early stages would underestimate the risks and disease burden. Further research will reveal more harm, especially from long-term obesity since childhood. The prevalence of obesity will likely overtake smoking prevalence, but commitments to obesity control are too weak. The SOEM is needed and should be useful to forewarn against the expanding public health problems attributable to obesity, and challenges in epidemiology and interventions. Learning from tobacco control, we advocate for a framework convention on obesity control. Framing obesity control initiatives in the spirit of MPOWER strategies against tobacco should be considered to prevent and control obesity and obesity-induced diseases. Healthcare professionals should take leading roles in these initiatives and obese individuals should reduce their weight and ‘quit’ obesity.
Zhejiang University School of Medicine, China
Obesity has heterogeneity. Obesity has different metabolic status as: metabolically abnormal obesity (MAO) and metabolically normal obesity (MNO). This study investigated the prevalence and distribution of MNO in Chinese population and explored the determinants of heterogeneity. Obesity has heterogeneity. Obesity has different metabolic status as metabolically abnormal obesity (MAO) and metabolically normal obesity (MNO). In a cross-sectional investigation on metabolic syndrome in China, The study investigated the prevalence and distribution of MNO in Chinese population and the determinants of heterogeneity. Then in a prospective cohort, we explored the effect on metabolic components in the subjects with MNO and the effect of weight change on the metabolic components. The Long-term effect of MNO on mortality of diabetes, cardiovascular diseases, and cancers were evaluated with meta-analysis. The results indicated the prevalence of MNO of obesity in China was 27.9%, which was lower than those in most of countries in the world. The determinants of metabolic heterogeneity were central obesity, Physical activity, sedentary time, Fruits/vegetables intake and Family history of MD and CVD, respectively. Comparing with the subjects with metabolically health (MNNW), normal weight, MNO increased the risk of the incidences of abnormal metabolic components and mortalities of diabetes and cardiovascular diseases, however, these risks were significantly lower than those in the subjects with MAO. Weight loss could reduce the risk of abnormal metabolic components. In conclusion, obesity has metabolic heterogeneity and MNO increase the risks of mid and long term outcome comparing with the subjects with MNNW and decrease the risks comparing with the subjects with MAO. This finding have significance on public health and provides the evidence on classification and individual management of obesity.
Biography:
Dr. Yimin Zhu Ph.D, & Professor, vice director of Department of Epidemiology & Biostatistics, School of Public Health, Zhejiang University. His major research interests include molecular epidemiology, genetic susceptibility, epigenetics and metabonomics in obesity, metabolic syndrome. His team has screened multiple biomarkers of these diseases using multi-omics technologies such GWAS, RNA-seq, Medip-seq and metabonomic, and also systematically investigated the metabolic heterogeneity in obesity and its mid and long-term adverse effect.