Case Report
Atypical Case of Hypertrophic Lichen Planus recognized by Dermoscopy
1Department of Dermatology, Hassan II University Hospital, Fez, Morocco
2Department of Anatomic Pathology, Hassan II University Hospital, Fez, Morocco
*Corresponding author: Safae Zinoune, Department of Dermatology, University Hospital Hassan II Fez, Morocco, Tel: 00212602841831, E-mail: dr.zinounesafae@gmail.com
Received: March 5, 2019 Accepted: March 26, 2019 Published: April 5, 2019
Citation: Zinoune S, Baybay H, Hammas N, et al. Atypical Case of Hypertrophic Lichen Planus recognized by Dermoscopy. Madridge J Dermatol Res. 2019; 4(1): 90-93. doi: 10.18689/mjdr-1000123
Copyright: © 2019 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
We present an atypical case of hypertrophic lichen planus (HLP) in a middle-aged patient. The presentation as a solitary, indolent, pigmented lesion in a photo-exposed area required further investigations to rule out malignancy, especially pigmented Bowen disease and pigmented basocellular carcinoma. Dermoscopy findings were found to be helpful in our case in addressing the correct diagnosis.
Keywords: Hypertophic lichen planus; Dermoscopy; Histology.
Introduction
Lichen planus (LP) is an inflammatory disease that affects the skin, the mucous membranes, the genitalia, the nails, and the scalp. There are several variants of lichen planus whose clinical, dermoscopic and histological appearance varies from one subtype to another. Hypertrophic lichen planus (HLP) is the second most common cutaneous variant of lichen planus. It is typically characterized as extremely pruritic, thick, and hyperkeratotic plaques, they are seen primarily on the shins or dorsal aspect of the foot and may be covered by a fine adherent scale. The lesions are usually symmetrical and tend to be chronic because of repetitive scratching [1,2]. The diagnosis of HLP is usually established clinically, based on the typical morphology of lesions and the coexisting of intense pruritus. However, atypical presentations requiring histopathologic confirmation of the diagnosis do exist [3].
Dermoscopy is a fast and non-invasive technique, increasingly applied in the diagnosis of a broad range of inflammatory skin diseases including HLP. This tool may have a significant interest in the atypical forms of this chronic condition, especially for solitary lesion [4].
In this report, we present a characteristic example of a patient with a misleading clinical aspect of HLP resembling maligned pathology. Application of dermoscopy was the key point in the diagnosis.
Clinical Presentation
A 50-year-old man was referred to our department for a solitary pigmented lesion of the neck of five years duration (Figures 1 and 2). Because of the slow growth of the lesion, the site involved and the age of the patient, a medical consult was requested to rule out malignancy. No relevant medical history was recorded.
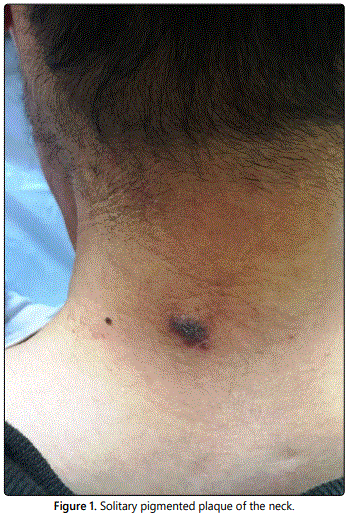
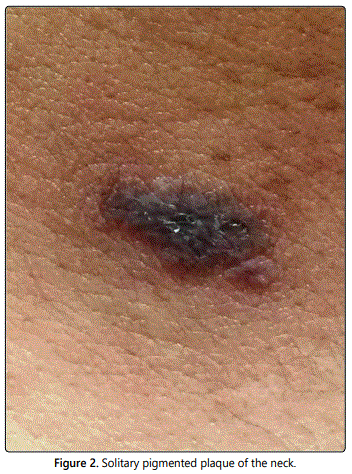
Dermoscopic examination revealed the predominance of a Brownish color on the background, with prominent pearly whitish structures, arranged in a reticulated pattern with peripheral striations and some comedo-like openings (Figure 3). At the periphery, areas of peppering were present.
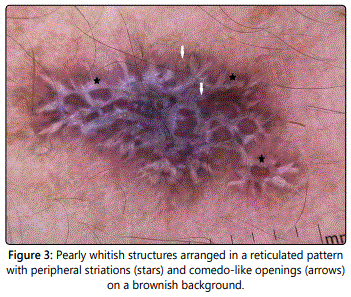
The diagnosis of hypertrophic lichen planus (HLP) was considered after clinical and dermoscopic correlation. A biopsy was then performed.
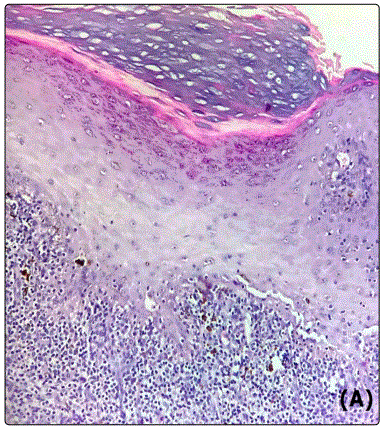
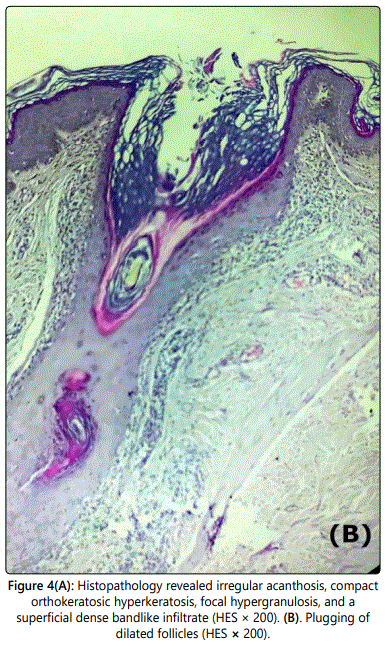
The histopathologic examination found a marked orthokeratosic hyperkeratosis, irregular acanthosis, focal hypergranulosis with follicular dilatation and plugging, and a superficial dense bandlike infiltrate (Figure 4). All findings were in keeping with the final diagnosis of hypertrophic lichen planus.
The patient was treated with topical corticosteroids class I with good improvement.
Discussion
Dermoscopy is a non-invasive diagnostic procedure that allows a rapid in vivo evaluation of morphologic structures of the epidermis, the dermo-epidermal junction, and the papillary dermis, not visible to the naked eye. Given that dermoscopic structures have been assessed to correlate well with the underlying histopathologic alterations, the method can be regarded as a link between clinical and histopathologic examination [3]. This diagnostic tool has allowed the identifications of several skin diseases, both neoplastic and non-neoplastic [5,6]. Regarding inflammatory conditions in dermatology, specific dermoscopic patterns have been well defined for a non-invasive diagnosis [6]. These peculiar clues are somehow easy to identify when the history, distribution, and morphology of lesions are evocative for a specific disease. However, things are less straightforward when we face unusual clinical scenarios [7].
In the current case, clinical manifestations as a solitary pigmented lesion, the slow growth of the lesion, the site involved and the age of the patient, were highly suggestive of pigmented basocellar carcinoma (BCC) and pigmented Bowenʼs disease included in the differential diagnosis. However, the application of dermoscopy significantly influenced our diagnostic thoughts. On one hand, this was because the lesion deviated from the standard dermoscopic pattern of pigmented BCC, which are composed of arborizing vessels, superficial fine telangiectasias, blue-grey ovoid nests, blue-grey globules, In-focus dots, maple leaf-like areas, spoke-wheel areas, concentric structures, ulceration, multiple small erosions, shiny white-red structureless areas, and white streaks [8]. On the other hand the usual dermoscopic pattern of pigmented Bowenʼs disease is characterized by glomerular vessels that are arranged in clusters, white to yellow scales and brown dots with a linear arrangement that usually seen at the periphery of the lesion [9]. These features are not found in our case either. The prevailing dermoscopic features were the pearly white crossing lines, corresponding to the so-called Wickham striae, which are known as a highly specific criterion of Lichen Planus [10]. The presence of yellowish round structures (comedo-like opening), the brownish background, the very itchy character as well as the clinical aspect of the lesion, makes the diagnosis of HLP.
Typical dermoscopy of HLP show pearly white lines, Comedo-like openings (CLO), Gray-blue globules and Red dots wich arranged diffusely in the lesions [11]. Each of these dermoscopic signs has a histological correspondence. Pearly white areas (Wickham striae) correspond histopathologically to compact orthokeratosis above zones of wedge-shaped hypergranulosis and acanthosis. CLO correspond to dilatation, plugging and hypergranulosis of the infundibulum and they are suggestive of transepithelial elimination. In HLP, histopathologic changes, namely, epidermal hyperplasia, acanthosis, hypergranulosis, and compact and lamellated hyperkeratosis, are centered on follicular infundibula and acrosyringia [12]. Hence, CLO are very specific to hypertrophic LP, they are also demonstrated in the early stages of lichen sclerosis and in basal cell carcinoma and seborrheic keratosis [13,14]. Gray-blue globules represent melanin pigment in the dermis due to melanin incontinence as a result of vacuolar degeneration in perifollicular and interfollicular areas. Red dots correspond to dilated capillaries in histopathology [14]. The presence of all of these features in dermoscopy establishes a certain diagnosis of HLP.
As shown in our case, dermoscopy may change our diagnostic thoughts, saving us from misdiagnosis and potential inappropriate management.
Conclusion
Dermoscopy is a fast and noninvasive technique that contributes to the early recognition and treatment of HLP, which is important considering the possible development of squamous cell carcinoma in longstanding nontreated lesions, hence, its possible role also in the monitoring of these patients [15].
References
- Shiohara T, Kano Y. Lichen planus and lichenoid dermatoses. In: Bolognia JL, Jorizzo JL, Schaffer JV (eds). Dermatology. 3rd edition. New York: Elsevier Saunders. 2012: 183-202. doi: 10.5826/dpc.0602a03.
- Russo T, Piccolo V, Lallas A, Argenziano G. Recent advances in dermoscopy. F1000Res. 2016; 5. doi: 10.12688/f1000research.7597.1
- Lallas A, Zalaudek I, Argenziano G, et al. Dermoscopy in general Dermatology. Dermatol Clin. 2013; 31(4): 679-694. doi: 10.1016/j.det.2013.06.008.
- Borsari S, Pampena R, Lallas A, et al. Clinical indications for use of reflectance confocal microscopy for skin cancer diagnosis. JAMA Dermatol. 2016; 152(10): 1093-1098. doi: 10.1001/jamadermatol.2016.1188.
- Lallas A, Kyrgidis A, Tzellos TG, et al. Accuracy of dermoscopic criteria for the diagnosis of psoriasis, dermatitis, lichen planus and pityriasis rosea. Br J Dermatol. 2012; 166(6): 1198-1205. doi: 10.1111/j.1365-2133.2012.10868.x.
- Papageorgiou C, Apalla Z, Lazaridou E, et al. Atypical case of lichen planus recognized by dermoscopy. Dermatol Pract Concept. 2016; 6(4): 39-42. doi: 10.5826/dpc.0604a09
- Wozniak-Rito A, Zalaudek I, Rudnicka L. Dermoscopy of basal cell carcinoma. Clin Exp Dermatol. 2018; 43(3): 241–247. doi:10.1111/ced.13387.
- Zhou LL, Mistry N. Pigmented Bowen disease. CMAJ. 2017; 189(47): E1462. doi: 10.1503/cmaj.170810.
- Friedman P, Sabban EC, Marcucci C, Peralta R, Cabo H. Dermoscopic findings in different clinical variants of lichen planus. Is dermoscopy useful? Dermatol Pract Concept. 2015; 5(4): 51-55. doi: 10.5826/dpc.0504a13
- Ankad BS, Beergouder SL. Hypertrophic lichen planus versus prurigo nodularis: a dermoscopic perspective. Dermatol Pract Concept. 2016; 6(2): 9-15. doi: 10.5826/dpc.0602a03.
- Busam KJ. Dermatopathology: Foundations in Diagnostic Pathology. Philadelphia: Saunders Elsevier Health Sciences. 2010: 11-81.
- Shim WH, Jwa SW, Song M, et al. Diagnostic usefulness of dermatoscopy in differentiating lichen sclerosus et atrophicus from morphea. J Am Acad Dermatol. 2012; 66(4): 690-691. doi: 10.1016/j.jaad.2011.06.042
- Braun RP, Rabinovitz HS, Krischer J, et al. Dermoscopy of pigmented seborrheic keratosis: a morphological study. Arch Dermatol. 2002; 138(12): 1556-1560. doi: 10.1001/archderm.138.12.1556
- Singh SK, Saikia UN, Ajith C, Kumar B. Squamous cell carcinoma arising from hypertrophic lichen planus. J Eur Acad Dermatol Venereol. 2006; 20(6): 745-746. doi: 10.1111/j.1468-3083.2006.01500.x



