Case Report
Granulomatous Rosacea Histopathologically Confused with Papulonecrotic Tuberculid: A Case Report
1Department of Dermatology, Bahcesehir University, Istanbul, Turkey
2Pathology Clinic, Kartal Education and Research Hospital, Istanbul, Turkey
3Infectious Diseases and Microbiology Clinic, VM Medical Park Hospital, Kocaeli, Turkey
*Corresponding author: Berna Aksoy, VM Medicalpark Hospital, Ovacik Discreet, Beside D-100 Highway, No: 36 Basiskele, Kocaeli, GSM: 0905326665634, Turkey, E-mail: bernaaaksoy@gmail.com
Received: October 28, 2017 Accepted: November 9, 2017 Published: November 15, 2017
Citation: Aksoy B, Karadayi AN, Derin O, Tatlıparmak A, Koc E. Granulomatous Rosacea Histopathologically Confused with Papulonecrotic Tuberculid: A Case Report. Madridge J Dermatol Res. 2017; 2(1): 20-22. doi: 10.18689/mjdr-1000105
Copyright: © 2017 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
The differential diagnosis of facial granulomas can be challenging in some cases, as multiple diseases have similar histopathological findings. Herein we describe a 36-year-old male with granulomatous rosacea that was initially diagnosed as papulonecrotic tuberculid based on the initial histopathological sections analyzed. This case presentation aimed to highlight both the need for re-evaluation of clinical findings and that examination of new histopathologic sections may be necessary for a definitive diagnosis of facial granulomas.
Keywords: Caseification Necrosis; Granulomatous; Granuloma; Rosacea; Skin; Tuberculid; Tuberculosis
Introduction
The differential diagnosis of facial granulomatous lesions can be challenging in some cases [1]. Granulomatous rosacea, demodicidosis, sarcoidosis, granuloma faciale, perioral dermatitis, foreign body reactions, deep fungal infections, Crohn's disease, and Melkersson-Rosenthal syndrome are all characterized by facial granulomas [1,2]. Lupus miliaris disseminatus faciei, tuberculids, and skin tuberculosis are included in the differential diagnosis of facial granulomas that histopathologically show caseification necrosis [1]. Herein we present a patient with granulomatous rosacea that was initially diagnosed as papulonecrotic tuberculid based on histopathologically observed epithelioid granulomas with caseification necrosis.
Case
A 36-year-old otherwise healthy male presented with non-itchy red facial lesions. The lesions first appeared 3 months earlier and progressively increased in number.There was no pruritus or tenderness in the lesions. The patient did not complain of any cough, fatigue or night sweats. Dermatological examination showed erythematous scaly papular lesions on the eyelids, lips, cheeks, and temples. Via diascopy the lesions appeared granulomatous, but without scarring (Figure 1a and b).
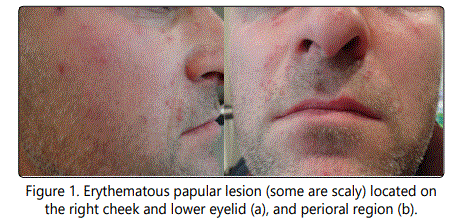
The patient's medical and family histories were unremarkable. The patient was a welder and thought that the lesions were related to welding fumes. He stated that the intensity of redness increases when he was at work and decreases in weekends.
First histopathologic sections prepared from a punch biopsy specimen taken from the right temple showed granulomas composed of epithelioid histiocytes and Langhans-type giant cells in the papillary and reticular dermis, with a tendency to fuse to each other and there was caseification necrosis or polymorphonuclear leukocytes in the centers of these granulomas. Based on those findings, the patient was diagnosed as papulonecrotic tuberculid (Figure 2).
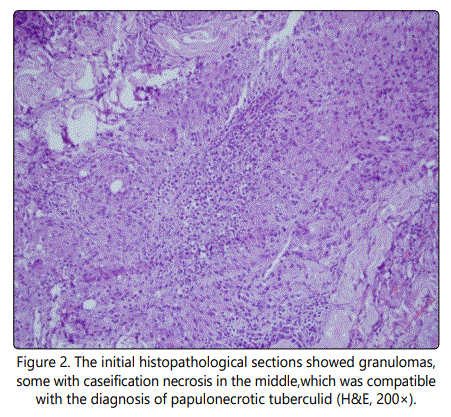
Subsequently, it was determined that patient had never been exposed to Mycobacterium tuberculosis based on detailed anamnesis, physical examination, radiological examination, and TB-IGRA testing (T-spot), which were performed to rule out any tubercular focus. Histopathological examination of newly prepared sections showed granulomas composed of lymphocytes, epithelioid histiocytes, and Langhans-type giant cells, chronic inflammation, and some ectatic vessels in the papillary and reticular dermis, neighboring hair follicles, and adnexal structures (Figure 3). The patient was then definitively diagnosed as granulomatous rosacea following clinicopathological reassessment.
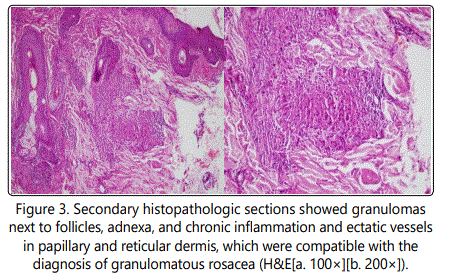
Discussion
Rosacea is a chronic inflammatory skin disorder mostly affecting light skinned middle aged people, seen up to 10% of the population and mostly in females [3]. Rosacea was diagnosed based on the presence of fixed centrofacial erythema or phymatous changes which are accepted as diagnostic; or based on presence of 2 and more of the followings which may be considered as diagnostic: flushing, papules and pustules, telangiectasia and ocular manifestations [4]. There are four principal rosacea type as erythematotelangiectatic (neurovascular), papulopustular (inflammatory), phymatous, and ocular types [4]. Rosacea is differentiated from acne based on the absence of comedones. Granulomatous rosacea is accepted as a variant of rosacea [3].
Granulomatous rosacea is more prevalent in ethnic dark skin of African Americans [3]. Granulomatous variant of rosacea manifests clinically as firm papules and nodules similar to those seen in cutaneous sarcoidosis, tuberculids or cutaneous tuberculosis [3]. Granulomatous rosacea is classically associated with widespread telangiectases, and various types of non-caseificating granulomas found diffusely in the superficial and middle dermis based on histopathological examination [5]. In addition, histopathological examination of skin tuberculosis and tuberculid lesions, granulomatous rosacea, demodicidosis, and lupus miliaris disseminatus faciei lesions can show caseification necrosis [1]. Epithelioid granulomas with caseification necrosis is the most common histopathological finding in cases of skin tuberculosis, independent of anatomic region [1]. Microscopy-based diagnosis of skin tuberculosis and tuberculids can be challenging, and their histopathological characteristics are similar to those of other granulomatous lesions [1]. Ferrara et al. [1] reported 4 patients, of which— interestingly—the patient with the most caseification necrosis was diagnosed as granulomatous rosacea and the patient without caseification necrosis was diagnosed as skin tuberculosis. Definitive diagnosis of skin tuberculosis and tuberculids should be confirmed via PCR and culture methods, as well as microscopic examination [1].
The presence of intradermal Demodex parasites within the perifollicular granulomatous and inflammatory infiltrate is diagnostic for granulomatous rosacea-like demodicidosis [6]. Lupus miliaris disseminatus can mimic rosacea and is characterized by midline facial papular lesions that spontaneously disappear, but leave scarring [7]. Histopathological examination of lupus miliaris disseminatus faciei lesions shows dense granulomatous infiltrate with central caseification [7].
Burns,and eye and ear injuries are among the occupational hazards associated with welding. Angiolymphoid hyperplasia with eosinophilia, localized neutrophilic dermatosis, and lichen sclerosus et atrophicus has been reported in burn scars caused by welding [8-10]. Another study on welders reported a self-report skin disease rate of 24% and presence of skin diseases increased with exposure to dust/smoke and radiation [11]; however, even though that study considered burns as a skin disease, the other skin diseases were not described. To the best of our knowledge the literature does not include any reports of granulomatous rosacea in welders. The presented patient's complaints were most likely not the result of welding fumes, but was exacerbated by the high temperature of his work environment.
Determining that the presented patient had not been exposed to M. tuberculosis helped differentiate his lesions from skin tuberculosis and tuberculids, and the absence of both scarring from lupus miliaris disseminatus faciei and Demodex parasites, based on histopathologic examination, helped differentiate his lesions from demodicidosis. Here in we described a patient with granulomatous rosacea that was initially diagnosed as papulonecrotic tuberculid, so as to highlight the importance of re-evaluation of clinical findings and analysis of newly-prepared histopathological sections for a definitive differential diagnosis of facial granulomatous lesions.
References