Case Report
Atypical Presentation of Chilblains
Department of Dermatology, Cruces University Hospital, Baracaldo, Spain
*Corresponding author: Olane Guergue-Diaz de Cerio, Department of Dermatology, Cruces University Hospital, Plaza de Cruces, s/n, 48903, Baracaldo, Vizcaya Spain, Tel: +34 946006149/+34 625898855, Fax: 34 94 600 61 38, E-mail: olaneguergue06051988@gmail.com
Received: October 20, 2016 Accepted: November 8, 2016 Published: November 11, 2016
Citation: Guergue Diaz de Cerio O, Vicente-Sanchez I, Mendieta-Eckert M. Atypical Presentation of Chilblains. Madridge J Dermatol Res. 2016; 1(1): 18-19. doi: 10.18689/mjdr-1000104
Copyright: © 2016 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Keywords: Chilblains; Idiopathic Chilblains; Pernio; Perniosis.
Abstract
This case report describes the appearance of some spectacular chilblains in a healthy man.
Chilblains (also known as pernio and perniosis) is a common skin disorder that results from cold exposure. Although the diagnosis is usually based on clinical findings, sometimes both laboratory tests and a skin biopsy are necessary to confirm it.
Report of a case
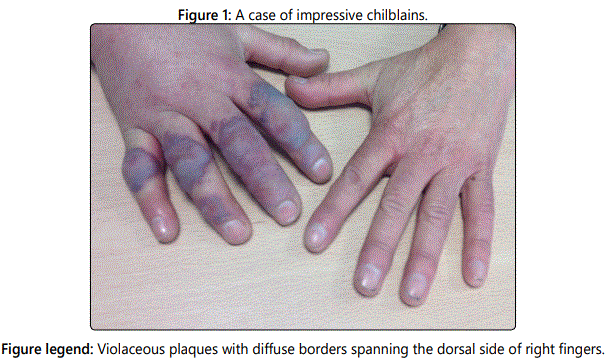
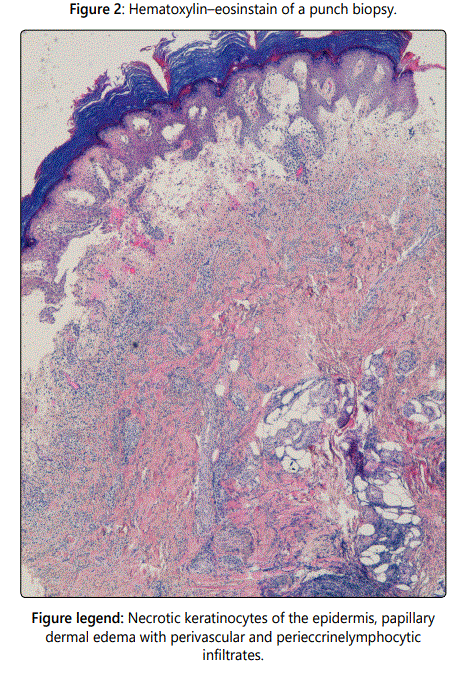
An otherwise healthy man in his 60s was referred for evaluation of one-week history of asymptomatic swelling in his right hand. He reported that it had appeared after removing snow. He did not report any systemic symptoms. The examination of his right hand revealed violaceous plaques with diffuse borders spanning his dorsal side of fingers (Figure 1). Laboratory test results were all within the normal reference range, including complete blood cell count, C-reactive protein, antinuclear antibodies, antiphospholipid antibodies, serum protein electrophoresis, coagulation and cryoglobulins. Hepatitis C antibody test was negative. Histologic findings from a skin biopsy showed necrotic keratinocytes of the epidermis, intense papillary dermal edema and lymphocytic infiltrate with perivascular and perieccrine distribution (Figure 2). Based on the relation of touching snow to his skin lesions, laboratory test values and skin biopsy findings, chilblains were considered for diagnosis. Prednisone was prescribed for 2 weeks. He was advised to avoid exposure to cold by using gloves and socks. At 3-week follow-up after discharge, he had dramatic improvement. No recurrence had been at one-year later follow-up.
Discussion
Chilblains (also known as pernio and perniosis) consist of erythematous or bluish and usually itchy and inflammatory papules, plaques or nodules that appear secondary to contact of the body with cold. Women are more commonly affected [1], and there is some evidence of familial predisposition. Skin lesions typically have a symmetric acral distribution, especially affecting dorsal and lateral aspects of fingers of the hands and feet, ears or thighs. The lesions appear between 12 and 24 hours after cold temperature exposure and they resolve spontaneously in a few weeks without sequela. The patient may have recurrences during the following years and usually resolve definitely. Although most cases occur in healthy people ("primary or idiopathic perniosis"), they may be associated with an underlying systemic disease ("secondary chilblains") such as hematological malignancies (especially chronic myelomonocytic leukemia), systemic lupus erythematosus, cryoglobulinemia, antiphospholipid syndrome and macroglobulinemia [1]. Clinical findings of both types are difficult to distinguish. The pathogenesis is still unknown, but it is thought to be related to alterations in intrinsic microcirculation that cause vasospasm [2]. The diagnosis is clinically made in many cases, though it is important to exclude an underlying disorder that can cause lesions with a similar appearance. The most difficult differential diagnosis is with chilblain lupus [3]. Therefore, a minimal study should include a complete blood count, antiphospholipid antibody, cryoglobulins, cryofibrinogen, cold agglutinins, antinuclear antibodies and serum protein electrophoresis. A skin biopsy can be helpful to exclude other diagnoses in atypical, treatment-resistant or chronic chilblains. The histopathologic findings although nonspecific, usually include necrotic keratinocytes, an intense papillary dermal edema and perivascular inflammatory infiltrate extending to perieccrine region. It has been suggested that in lupus erythematosus lesions vacuolation of basal cells is more commonly seen, while perieccrine inflammation and dermal edema are rare. There is no curative treatment for chilblains. The most important thing is the prevention, which is based on avoidance of cold exposure. The therapeutic management usually consists of symptomatic relief with potent topical steroids. More recently, topical 0.2% nitroglycerine has been proposed as an alternative treatment [4]. Although current advice in general practice considers nifedipine in the winter months as a good treatment option for chronic chilblains [1,3], a recent randomized trial did not show evidence in favor of nifedipine over placebo [5]. It is more; nifedipine was associated with a higher rate of side effects such as a lower systolic blood pressure and edema. In the other side, secondary chilblains may respond to systemic corticosteroids and immunosuppressive therapy, such as mycophenolatemofetil, or anti-malarial medications, such as hydroxychloroquine [1].
Funding source: No funding was secured for this study
Financial Disclosure: The authors have no financial relationships relevant to this article to disclose.
Conflict of Interest: The authors have no conflicts of interest to disclose.
References