Short Communication
How you Should Comment on a Mistake with a Comrade. Must it always be Troublesome?
Full Professor, Department of Clinical and Experimental Cardiology, Boston University, USA
*Corresponding author: Breijo-Marquez FR, Full Professor, Department of Clinical and Experimental Cardiology, Boston University, USA, Ph: +02.673.517.585, E-mail: frbreijo@gmail.com
Received: April 10, 2018 Accepted: April 19, 2018 Published: April 26, 2018
Citation: Breijo-Marquez FR. How you Should Comment on a Mistake with a Comrade. Must it always be Troublesome? Madridge J Intern Emerg Med. 2018; 2(1): 54-55. doi: 10.18689/mjiem-1000111
Copyright: © 2018 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Keywords: Cardiac arrhythmias; Short PR interval; Wolff-Parkinson-White pattern. Interdisciplinary Discrepancies; Medical Ethics.
Document
This possibility, far from being unusual, can be quite frequent. Sometimes and depending on the type of hospital, it can be very widespread. It is a difficult task when it comes to deciding what to do with the comrade. On the one hand, our ethical sense obliges us to give him a comment on the mistake. On the other hand, we don’t want to hurt the professional esteem of the comrade in question.
What to do then?
The most sensible thing would be to comment on the error and discuss it amicably. Although on more occasions than we wished, hostility or resentment emerges in our comrade, and we can do nothing to get him out of his own mistake.
Taking advantage of such an error to obtain a more considerable prestige of one’s own is not very ethical, but on many occasions, it is the most appropriate for the patient, since such an error can have undesirable effects, or condemn the patient to erroneous treatment triggered by a misdiagnosis.
Hence, the first thing we must do is to discuss it with the comrade. And if the latter does not heed our suggestions, we must communicate it to the head of the service and act accordingly.
By way of example, an adult 45-year-old Caucasian woman went to our hospital with a night-time heart palpitations crisis. She had had these crises more than four times in the last two years. Tachycardia had nothing whatsoever to do with exertion, unleashing itself at night, at rest. She denies taking any medication that would make us suspect the one causing such tachycardia.
She was diagnosed with supraventricular paroxysmal tachycardia generically.
In the emergency department, she has been treated with Adenosine: 6 mg in direct bolus. Tachycardia increased, and this fact was classified as Paradoxical effect to Adenosine.
As much in our experience as in that of many other authors, in Wolff-Parkinson-White syndrome [1,2], the administration of Adenosine is not indicated, since the result may be worsening tachycardia.
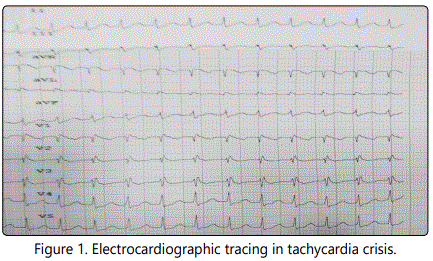
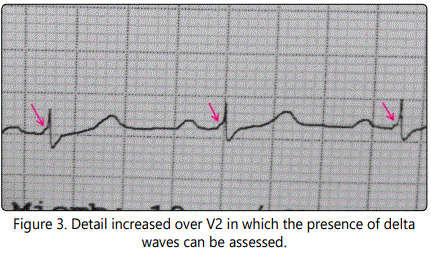
In the following illustration, electrocardiographic tracing allows us to assess the presence of a delta wave. [Figures 1,2,3]
The PR interval is displayed with an acceptable length. But the delta wave is well manifested.
This electrocardiographic feature could represent a new variety of Wolff-Parkinson-White not described so far.
We told the comrade who diagnosed “supraventricular paroxysmal tachycardia” with “a paradoxical effect on the administration of Adenosine”.
The outcome of the dialogue was terrible.
In every branch of medicine, the patient must be the most important. This fact is logical and unquestionable.
But then what about the comrade? An eternal hostility?
Perhaps because the PR interval was of average length, the electrophysiological study was anodyne.
But the genetic study was positive for the PRKAG2 gene.
So we were in front of a variation of the WPW.
Now we have to study it in depth:
A WPW electrocardiographic pattern with normal PR interval and delta wave presence, positive for the PRKAG2 gene.

Another very significant example in which the same conditions of disagreement, multiple interdisciplinary conflicts, occurred was the following:
An 18-year-old young man. He lives on his own and denies taking any drugs. He went to the hospital emergency room for a specific syncope event that was witnessed by his girlfriend. The recovery was full spontaneously. The young man said that this type of events was frequent in him, especially in childhood. He was assessed in the emergency room by a cardiologist, giving as normal all the parameters that were assessed, including an electrocardiographic study. The young man was sent home without further precautions.
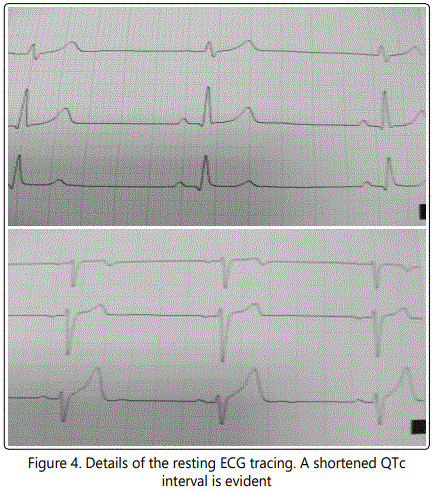
However, a short QT interval [3,4] can be observed in your electrocardiographic tracing, as we can see in the image below.
They are just two examples. How much more will have happened?
So then
What should we be doing when we know that a comrade is making a mistake?
We can all be wrong, but recognizing our own mistakes is one more step towards the goodness of our diagnoses and, therefore, of our treatments and the lives of our patients.
References