Case Report
Syncope caused by Transient High Grade Atrioventricular Block in a Teenager
Department of Internal Medicine, Division of Cardiology, Texas Tech University Health Science Center, Lubbock, Texas, USA
*Corresponding author: Saranapoom Klomjit, Department of Internal Medicine, Division of Cardiology, Texas Tech University Health Science Center, Lubbock, Texas, USA, Tel: +1806-7433155, Fax: +1806-7433148, E-mail: saranapoom.klomjit@ttuhsc.edu
Received: October 10, 2016 Accepted: December 14, 2016 Published: December 19, 2016
Citation: Klomjit S, Argueta E, Singh A. Syncope caused by Transient High Grade Atrioventricular Block in a Teenager. Madridge J Cardiol. 2016: 1(1): 12-13. doi: 10.18689/mjc-1000104
Copyright: © 2016 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Syncope Caused by Transient High Grade Atrioventricular Block in a Teenager.
Introduction: Syncope due to heart conduction anomalies is life threatening. High grade atrioventricular (AV) conduction defect in teenagers is uncommon. History, physical examination and use of different testing modalities can guide us to identify a plausible cause for syncope.
Case: A 19 year old woman with no known medical history presented to clinic after having multiple episodes of syncope. The first episode occurred 6 months ago while walking. She quickly regained consciousness with no confusion and denied other symptoms or seizure like activity. She then had two more episodes associated with minimal exertion. Her mother and grandmother had a diagnosis of systemic lupus erythematosus. There was no family history of heart disease. Physical exam was unremarkable, including no orthostatic hypotension or murmur.
Initial ECG showed normal sinus rhythm. Transthoracic echocardiogram was normal. A treadmill stress test showed an appropriate heart rate response and good exercise capacity. Blood analysis including serum Lyme titters and auto-antibodies were negative. Tilt table testing showed a high grade AV block during which the patient lost consciousness. She spontaneously regained consciousness and her ECG returned to normal. We discussed the benefit of implanting a permanent pacemaker for which she agreed.
In conclusion: Our case reinforces the importance of obtaining a good history and using diagnostic modalities to reach a diagnosis. Although a cause for the AV block was not found, an appropriate treatment option was pursued.
Keywords: Syncope; High Grade AV block; Teenager; Maternal Lupus Erythematosus.
Introduction
Syncope due to heart conduction abnormalities is life-threatening. High grade atrioventricular (AV) conduction abnormalities in teenagers are uncommon. Careful history taking, physical examination and thorough investigation guide us to better care for the patients.
Case
19 years old white female with no known past medical history presented to the clinic with multiple episodes of syncope. The first episode was 6 months ago while she was walking to the school. She regained her consciousness within minutes and there was no head injury, confusion, headache, convulsion, chest pain or palpitation before or after the episode. She subsequently had two more similar episodes associated with minimal exertion. Her mother was diagnosed with systematic lupus erythematosus (SLE) four years prior to clinic visit but not at the time of her pregnancy. Her maternal grandmother was also diagnosed with SLE. She denied any heart disease in the family. On examination, she was afebrile, her blood pressure was 105/70 mmHg without orthostatic hypotension, and her heart rate was 62 bpm. Cardiac examination revealed normal heart sounds without murmurs/gallops/rubs. No central or peripheral cyanosis. The rest of the examination was unremarkable. Transthoracic echocardiogram (TTE) showed normal ejection fraction and no valvular abnormalities. Treadmill stress test revealed appropriate heart rate response, achieving maximal heart rate of 169 bpm and a maximal workload of 13.7 METs (metabolic equivalents of tasks). Patient was able to run on BRUCE protocol for 12 minutes.Tilt table test was then recommended. During the test, her ECG showed sinus tachycardia (Figure 1) followed by high grade AV block associated with passing out (Figure 2). She spontaneously regained her consciousness and herECG returned to normal sinus rhythm.
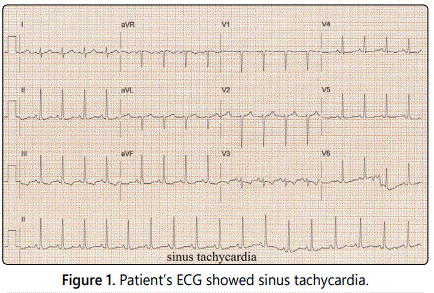
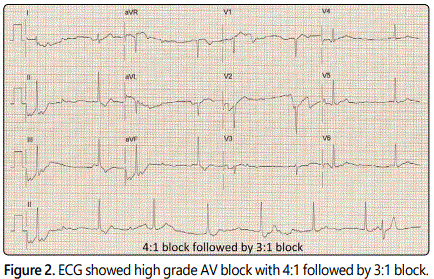
Laboratory values showed normal complete blood count and complete metabolic panels Serum Lyme titers were negative. The ANA test was negative. Anti-dsDNA was negative. Anti-Ro/SSA and anti-La/SSB were negative. We discussed about benefit of permanent pacemaker for which she agreed. Patient had no episodes of syncope on follow up visit to the clinic 2 months after pacemaker implantation.
Discussion
Our case report demonstrates high grade AV block during tilt table test and she did not demonstrate conduction abnormalities during treadmill stress test. We hypothesized that AV block could be due to 1) first episode of isolated AV block secondary to maternal SLE, 2) AV block as an early sign of SLE, 3) early sign of idiopathic fibrosis like Lenegre-Lev disease, which is less likely in this case due to patientʼs age and 4) ischemic heart disease which we ruled out by normal treadmill stress test.
With history of maternal systemic lupus erythematosus (SLE), the delayed onset of atrioventricular block may occur later in adult life [1]. We however could not retrieve patientʼs maternal history during the time of pregnancy and anti-Ro/SSA and anti-La/SSB of the mother were not obtainable. The antibodies in SLE mother and strong family history of SLE showed significant association with congenital atrioventricular block (CAVB) [1] but only 2% of mothers who acquired such antibodies had CAVB children [2]. It was difficult at this point to definitely determine if maternal SLE played role in her condition. We looked further at the second hypothesis and found no cardiac involvement of SLEwhich could have rare manifestation as conduction abnormalities [3]. There was a case report where complete heart block preceded the definitive diagnosis of SLE [4]. ANA and anti-dsDNA as well as anti –Ro and anti-La were negative on this patient. The diagnosis of SLE was not yet established. We have to follow the patient closely and see if she developed SLE or other autoimmune disease.
Idiopathic fibrosis is a rare condition in young adult which this patient could have acquired. MRI of the heart could possibly help us locate the pathology in this case but it would not yield difference in treatment approach. We ruled out other possibilities such as Lyme disease as the patient did not have any history of traveling to endemic area and the Lyme titers were negative. It is still challenging to have definite explanation for her conduction abnormalities. However the treatment which has shown to improve outcome on symptomatic syncope patient with high grade AV block is a permanent pacemaker which was pursued [5].
References
- Bergman G, Skog A, Tingstrom J, et al. Late development of complete atrioventricular block may be immune mediated and congenital in origin. Acta paediatrica. 2014; 103(3): 275-281. doi: 10.1111/apa.12483
- Miner JJ, Kim AH. Cardiac manifestations of systemic lupus erythematosus. Rheumatic diseases clinics of North America. 2014; 40(1): 51-60. doi: http://dx.doi.org/10.1016/j.rdc.2013.10.003
- Epstein AE, DiMarco JP, Ellenbogen KA, Estes NA, 3rd, Freedman RA, Gettes LS, et al. ACC/AHA/HRS 2008 Guidelines for Device-Based Therapy of Cardiac Rhythm Abnormalities: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the ACC/AHA/NASPE 2002 Guideline Update for Implantation of Cardiac Pacemakers and Antiarrhythmia Devices): developed in collaboration with the American Association for Thoracic Surgery and Society of Thoracic Surgeons. Circulation. 2008; 117(21): e350-e408. doi: https://doi.org/10.1161/CIRCUALTIONAHA.108.189742


