Research Article
HIV Stigma, Perceived Social Support, Coping Style and Mental Health of Women Living with HIV in the Philippines
AIDS Society of the Philippines, Quezon City, Philippines
*Corresponding author: Maria Isabel E. Melgar, AIDS Society of the Philippines, Quezon City, Philippines, E-mail: imelgar@ateneo.edu
Received: March 04, 2022 Accepted: March 26, 2022 Published: March 30, 2022
Citation: Melgar M I E, Alejandro C B, Chia E A. HIV Stigma, Perceived Social Support, Coping Style and Mental Health of Women Living with HIV in the Philippines. Madridge J Behav Soc Sci. 2022: 5(1): 79-85. doi: 10.18689/mjbss-1000114
Copyright: © 2022 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
The women who were infected with HIV represent approximately 6% of the total recorded HIV cases in the Philippines. Very little information is publicly known about their mental health and well-being. This survey study was designed to identify the mental health status and psychological well-being of women living with HIV. A total of 50 women with HIV from different parts of the country participated in the study in 2021.
The survey instrument was composed of different measures such as PHQ9, GAD2, Brief COPE, Perceived Social Support and HIV stigma scales. It was in paper and pencil form and were self-administered. A site research coordinator supervised the administration. Virtual administration was not used because of problems in internet connection.
The results of the survey showed a prevalence of 25% in depression and 23% in anxiety among women with HIV. Suicide ideation was reported by 28% of total respondents. Moderate levels on all types of HIV-related stigma were reported. The predominant coping styles varied from emotional coping to avoidant coping mechanisms. Receiving social support from oneʼs family and significant other was identified as an important source of strength. The association of the variables such as depression, anxiety, stigma, and social support were further analyzed using the multiple regression analysis.
The health sector involved in HIV treatment is challenged to examine feasible models of care that address the mental health unique needs of women amidst limited care giving resources.
Keywords: HIV; Mental Health; Depression; Anxiety; Women with HIV; Stigma; Social Support
Abbreviations Used:
HIV/AIDS – Human Immunodeficiency Virus/Acquired Immunodeficiency Syndrome
PLHIV – Person Living with HIV
WHO – World Health Organization
UNAIDS – Joint United Nations Programme on HIV/AIDS
WHIV – Women Living with HIV
Introduction
The Philippines, based on the most recent estimate of UNAIDS [1], reportedly have 110-120,000 people living with HIV (human immunodeficiency virus) with an incidence of 0.15 per 1000 Filipinos. Currently, the Philippines has the fastest growing HIV epidemic in Asia and the Pacific Region with a 273% increase in annual new HIV infections from 2010- 2020 [2]. Those who are predominantly infected are males with a huge share of 94% (85,578) of total cases. Women reported a small proportion with 6 % (5,371) mostly coming from the young adult population ages 25-34.
Less than 10 years ago, we have seen positive developments in national policies to address the public concern on HIV and to upgrade the quality of care accessed by people infected by the virus. The first is the passage of the Philippine HIV and AIDS Policy Act (RA11166), a policy primarily anchored on the principles of human rights aimed at strengthening treatment, care and support among PLHIV. The second is the Philippine Mental Health Act (RA 11036) which affirms the rights of Filipinos to mental health and supports the primary mental health services across the country. The third is the Universal Health Care (RA11223), a policy which promotes the right to health of all Filipinos and instill health consciousness among them.
The World Health Organizationʼs (WHO) 2016-2021 strategy for health sectors towards ending HIV/AIDS, is not only to reduce HIV transmission and HIV-related deaths but also to improve the health and well-being of all people living with HIV (PLHIV) [3]. This means inclusion of antiretroviral therapy and comprehensive long-term care for all living with HIV and reducing social issues such as stigmatization and discrimination. WHO has moved from a strictly clinical approach to a people-centered approach grounded on human rights and health equity. This implies a broader coverage of PLHIVʼs health needs particularly noncommunicable diseases, mental health and substance use disorders.
Women with HIV as a vulnerable population
In spite of the small percentage of registered women living with HIV (WLHIV), their number has been consistently growing since the first recorded case of infection in 1984. The number of diagnosed females from 2021 was 409 which was three times higher than the numbers a decade ago. In addition, 96% of the registered WLHIV are within the reproductive age-group of 15-49 when they were tested and diagnosed putting them at-risk for transmitting the virus to their offspring. In fact, from January to September 2021 alone, 53 HIV positive women reported that they are pregnant [2]. Moreover, women living with HIV have distinct health concerns such as pregnancy and vertical transmission [4].
Furthermore, compared to their male counterparts, WLHIV experience significantly more somatization, obsessivecompulsiveness, depression and anxiety [5]; report poorer health and functional status, and have an increased risk for chronic diseases [6]. Their mental health conditions are of particular importance since they are all related to treatment adherence and health outcomes [7].
In many ways, WLHIVs are more vulnerable to mental health conditions and emotional well-being that can affect their quality of life and prognosis as individuals living with HIV. This is of special concern since the Philippineʼs progress in terms of providing integrated services to PLHIVs including mental health interventions remains a challenge [8].
Mental Health and HIV
The mental health burden among PLHIV is characterized by a high prevalence of psychological distress, depression, anxiety, and suicidality. This is particularly evident in Asia. For instance, in a systematic review conducted in China, it was found that the prevalence of depressive symptoms among PLHIV was 60%, anxiety symptoms, 43% and suicidal ideation, 30-34% [9]. In Vietnam, 36.5% symptoms of depression was reported warranting further evaluation [10]. In a study conducted in Thailand, 12% had psychiatrist-confirmed mental health disorders where ten attempted suicide and three had suicidal ideation [11]. In the Philippines, 3.1% reported symptoms of depression while 10% reported anxiety [12]. In the 2021 qualitative study among Filipino women with HIV, traumatic feelings after diagnosis and strong feelings of rejection and depression were disclosed as the most difficult phase of HIV [13].
In a recent cross-sectional study in 2019-2020 in selected Asian countries including the Philippines [14], the estimated prevalence of depression was 47% (mild to severe) while 6% warranted psychiatric treatment. Some 19% had thoughts of suicide or self-hurting. Another study confirmed that depression was a strong predictor of poor ART adherence [15]. In a related study, mental disorders significantly associated with higher levels of community and family, and internal stigma [16]. Those experiencing severe personalized stigma have 3.4 times risk of depression while internalized stigma doubles the risk [17].
The response to a regional problem mirrors that of the global dilemma where merely 1% of the health workforce works in mental health (WHO, 2015). Access and linkage to mental health care and treatment remains to be a challenge. For example, only 32% of PLHIV participants in Malaysia with severe or extremely severe mental health symptoms received psychiatric referrals [18]. More than 80% with prevalent symptoms were not previously recognized clinically because of lack of routine screening.
With these developments, we chose to focus more attention to mental health concerns among women with HIV where little is known about this condition in this special group. It is imperative that we monitor their mental health status and psychological well-being if we wish to provide appropriate services to help them with these issues. The data that we aim to generate from this study can inform the development of relevant policies and programs for positive women in the future.
The goal of this study are to explore the mental health and psychological well-being of Filipino women living with HIV/AIDS specifically to: (1) identify their mental health status (depression and anxiety), (2) describe the HIV-related stigma they experience, (3) describe their coping styles, (4) describe their perceived social support, and (4) describe the relationship of the HIV-related stigma, coping styles, and perceived social support with depression and anxiety.
Methods
Research Design
The study used an observational design focused on describing the mental health and psychological well-being of WLHIV by using a quantitative survey method. The protocol of the study was reviewed and approved by the Ateneo School of Medicine and Public Health Ethics Committee.
Study Population and Criteria
Participants in the survey were cis-females diagnosed with HIV and with ages 18 years and above. They were being treated in four selected HIV treatment hubs in the Philippines. Their CD4 cell count is 300 and above as determined by their routine CD4 monitoring in the past 6 months.
Recruitment Method
For this study, convenience sampling from a cohort was used with the assistance of AIDS Society of the Philippines. Participants were recruited by coordinating with government accredited HIV/AIDS treatment hubs in Cebu, Davao, Angeles, and NCR. Site coordinators gave flyers to potential participants and posted invitations in their respective Facebook groups.
The target sample size was at least 139 participants using Open epi sample size calculator for survey sampling. The parameter used was the prevalence of females living with HIV in the Philippines in 2019 (0.01) published by UNAIDS [8]. A total of 150 participants consented to join the study.
In the pilot phase, four participants participated in the validation of the Filipino versions of the questionnaire by answering the survey and going through the cognitive interview process.
Instrument
The Mental Health Questionnaire (MHQ) is a battery of tests in Filipino aimed at looking into the different domains of mental health and psychological well-being. The questionnaire is composed of six parts with the first part being composed of HIV-related health questions and the rest are culturally adapted versions of common assessment tools that look into different aspects of psychological well-being of PLHIVs namely: HIV Stigma Scale, Patient Health Questionnaire- 9 (PHQ-9), Generalized Anxiety Disorder 2-item (GAD-2), Brief Coping Orientation to Problems Experienced Inventory (COPE), and Multidimensional Scale of Perceived Social Support (MSPSS). The Filipino translation of the mentioned assessment tools underwent a cultural adaptation protocol wherein tests were translated and administered to pre-study participants for cognitive interviewing. The results further improved the test items in terms of comprehensibility and appropriateness of terms or phrasing to Filipino culture.
Statistical Analysis
Data was analyzed using IBM SPSS version 20. Descriptive statistics was used for demographic variables, general health and well-being items, and all culturally adapted assessment tools. For the relationships between different variables, multiple linear regression was used with all parameters set to default with confidence interval set to 95% and significance level at 0.05.
Results
Demographic profile
The survey was administered to a total of 150 WLHIV residing in four major cities in the Philippines. They were recruited through the help of Department of Health accredited HIV treatment hubs and Social Hygiene Clinics in the cities of Manila, Angeles, Cebu, Davao. Some 89% of the women surveyed fell on the reproductive age of 18-50 years-old with an average of 5.9 years of being diagnosed with HIV. The HIV status of those surveyed were 83% asymptomatic, 15% symptomatic, and 2% AIDS converted. Most of the women (97%) got infected with HIV through sex with males, 3% from injecting drugs, and 1% from blood transfusion. Seventy-nine of 150 respondents were single while 28 were married. Fifty-four were living with their parents while 52 have their own house or are renting. Thirty-eight have no children.
Mental Health and Well-being
Pandemic-related response
Questions were asked on general coping of the WLHIV respondents in dealing with the Covid-19, how the pandemic affected their livelihood and the accessibility of their medicine using a 5-point Likert-scale with 1 referring to highly affected by the pandemic to 5 referring to not affected by the pandemic. This survey showed an average rating or a not so overwhelming response with regards to the pandemic. Among the three pandemic-related questions, the aspect that the pandemic impacted the most was their livelihood with mean score of 2.85, while coping and access to medicine were 3.09 and 3.56 respectively. This means that the treatment regiments they need were not disrupted and they were able to cope well with the pandemic situation. However, access to work and livelihood was moderately disrupted.
Depression
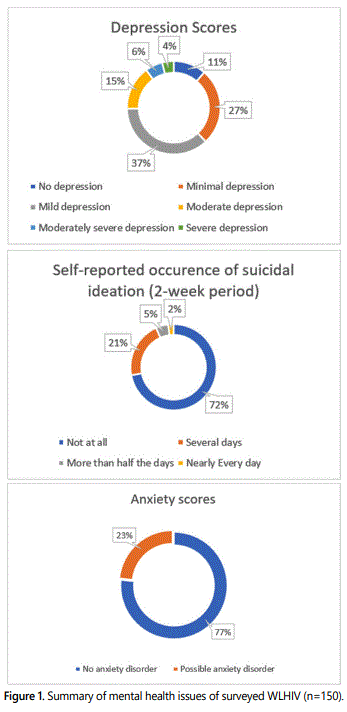
Results of PHQ-9, a measure of depression, showed a mean score of 7.01± 5.50. This means that WLHIV reported average experience or mild levels of depression where 11% of participants had no depression, 27% showed minimal depression and 37% had mild depression. However, some 15% reported moderate depression; 6% had moderately severe depression while 4% reported severe depression. Although a large percentage experienced non-clinical levels of depression, moderate to severe depression was experienced by 25% of the total respondents (see Figure 1).
Anxiety
Some 115 out of a total of 150 or 77% of the respondents met the criteria of no anxiety disorder. However, 23% of the respondents reached the cut off of 3 points on GAD-2, the measure for anxiety, for possible anxiety disorder (see Figure 1).
Suicide Ideation
One hundred eight out of 150 WLHIVs (72%) who answered the survey did not report any suicide ideation. However, there were 42 women (28%) who disclosed suicide thoughts from several days (21%) to nearly every day (2%) (see Figure 1).
HIV Stigma
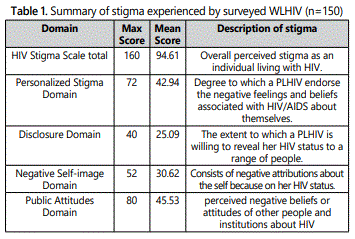
The mean score for HIV Stigma Scale is 94.61 from a maximum score of 160 which denotes a higher-than-average level of felt stigma. As Table 1 shows, the women respondents still experienced a moderate level of stigma and various forms of stigma such as personalized stigma, disclosure stigma, negative self-image and public stigma.
Coping Styles
Three different coping styles were assessed through this survey. First is the problem focused coping style which is composed of strategies that describe active coping, seeking instrumental support, and planning. The mean score obtained by WLHIVs on problem focused coping is 23.35 from a maximum score of 32. Second is the emotion focused coping style composed of strategies that describe acceptance, emotional social support, use of humor, positive reframing, and spirituality. The mean score for this coping style is 29.82 from a maximum score of 42. Third is the avoidant coping style composed of strategies that describe behavioral disengagement, selfdistraction, self-blame, use of substances to cope, and venting out. Coping scores of WLHIVs surveyed showed a mean of 15.61 for avoidant coping from a maximum score of 32. This means that WLHIV surveyed primarily employedemotion-focused coping, followed by problem-focused coping, and avoidant coping in dealing with stressors or personal problems.
Perceived Social Support
Results showed a mean social support of 60.91 from the total score of 84 on the Multidimensional Scale of Perceived Social Support (MSPSS).Based on the results of MSPSS, 2% of the sample perceived low levels of social support, 45% perceived moderate levels of social support, and 53% perceived high levels of social support. Overall, women in this survey were getting good social support.
In terms of social support, significant others showed a mean of 21.67, the family domain showed a mean of 21.06, and friends domain showed a mean of 18.17. This means that WLHIV surveyed primarily obtained social support from significant others, family members and friends. In the MSPSS, significant others did not identify specific people who are considered a significant other.
Relationship of Stigma with Depression and Anxiety
Results showed that stigma experienced by WLHIV significantly predicts depression, R2 = .07, F(1, 148) = 10.73, p = .001 and anxiety, R2 = .09, F(1, 148) = 13.73, p = .000.
With regards to specific stigma domains, the public attitude domain significantly predicts depression, R2 = .09, F(4, 145) = 3.78, p = .014, and that for every increase of .608 in the public attitude domain score, there is 1 point increase in depression score. This means that the higher perceived stigma from the public resulted to higher levels of depression.
There was no relationship found between stigma domains and anxiety scores.
Relationship of Coping Styles with Depression and Anxiety
Among the coping styles, avoidant coping significantly predicts depression, R2 = .16, F(3, 146) = 8.91, p = .003, and that for every increase of .282 in the avoidant coping score, there is 1 point increase in depression score. As mentioned, avoidant coping means disengaging oneself or escaping from a problem through distraction. This means that the use of a coping style such as avoidant coping has a negative impact on the individual by its contribution to oneʼs depression level. There is a significant relationship between one of the coping domains, avoidant coping, and anxiety. Avoidant coping was found to be a significant predictor R2 = .15, F(3, 146) = 8.58, p = .000and that for every increase of .340 in the avoidant coping score, there is 1 point increase in anxiety score. This means that the use of a certain coping style can affect the level of anxiety felt by an individual. In this case, using avoidant strategies for coping results to a greater probability of having anxiety disorder.
Relationship of Perceived Social Support with Depression and Anxiety
Perceived support from significant other is a significant predictor of depression, R2 = .11, F(3, 146) = 5.71, p = .000, and that for every decrease of .353 in the support from significant other score, there is 1 point increase in depression score. This means that the less support respondents feel from their significant other, the more depressed they feel. In the scale used by this survey, however, significant other was unspecified. Anxiety, on the other hand, is significantly predicted by perceived support from significant other, R2 = .08, F(3, 146) = 4.34, p = .001, and family support R2 = .08, F(3, 146) = 4.34, p = .010.For every decrease of .319 in the support from significant other score or increase of .283 in family support score, there is 1 point increase in anxiety score. This means that the less support from their significant other lead to higher anxiety and the more support they feel from their family results to greater probability of having anxiety disorder.
Discussion
This study explored and identified the mental health status and psychological well-being among women with HIV in the Philippines. Foremost in our findings is the current rate of depression and anxiety in this special group of infected women. We found through our screening, that 1 out of 4 experienced depression and a little less than this figure has probable anxiety disorder. Another alarming finding is the suicide ideation disclosed by the third of our respondents. However, it is difficult to make a direct attribution of this mental health crisis to HIV alone because the survey was conducted during the height of the COVID-19 pandemic in 2021. Loss of income, isolation and bereavement over deaths of people they knew who perished due to COVID-19 may have affected their mental status.
In a technical paper issued by Australasian Society for HIV, Viral Hepatitis and Sexual Health Medicine [19], the authors asserted that prior to COVID 19 many people will have met their emotional needs through family, friends, peer networks or support groups and/or personal self-management strategies. Further to this, those that are already experiencing isolation, disconnection and having mental health issues may feel lonelier and more distressed and may have exacerbation in mental health conditions. In this light, we recognize the possible effect of the COVID-19 pandemic in this study.
Depression and anxiety were both associated with HIV-related stigma [20-23]. The link between depression and suicide ideation; and stigma has clinical significance that must receive more attention from health professionals. We found in our study that there are a number of stressful factors that can trigger depression. These are HIV-related stigma, coping styles and perceived social support. The close relationship between stigma and depression is consistent with other studies [20-22,24-26]. Upon further analysis, HIV-related stigma and the negative public attitude towards people with HIV are most predictive of depression. The avoidant coping style among the respondents and weak support from significant others were identified significant predictors of depression. This finding reflects a typical behavior among Filipinos in avoiding to confront negative realities by not talking about sensitive issues and hiding oneʼs unfortunate condition; or experiencing shame in soliciting help from others. Likewise, the negative attitude of the public may also reflect ignorance of the dreaded disease leading to unfair judgement of people with HIV.
In the case of anxiety, however, our analysis showed no significant relationship between anxiety and specific HIVrelated stigma domains. Our study showed that higher anxiety can be attributed to avoidant coping style and perceived low support from significant others. In this study, we identified avoidant coping as a unique type of coping response and it turned out to be an important variable to consider in monitoring a womanʼs ways of coping. Mental health professionals must be aware about helping patients recognize the dangers of avoidant coping and teach them how to use more adaptive coping styles.
This finding contrasts with Seffren and colleaguesʼ study [27] where emotion-focused coping, problem-focused coping, and higher community support were related to more anxiety symptoms. An important finding to note in our study is the unlikely relationship of family support and anxiety where increased perceived support from family members results to higher levels of anxiety. It is probable that the kind of anxiety that is strongly related to family had something to do with disclosure dilemma or death anxiety depending on the womanʼs situation. This is an area that needs further exploration through qualitative research.
These findings have strong implications in terms of challenging the local health sector to effectively respond to the psychological and emotional needs of a proportion of women with HIV. Whether we have a lockdown situation or an improved health situation, health providers should be ready to assess telehealth communications through telephone or video triaging and counseling. As of this writing, internet connectivity remains to be a problem around the country which makes telehealth not a feasible solution in some regions with poor infrastructure. Nevertheless, treatment hubs should readily link WLHIV with external resources and peer-based organizations that understand their lived experience [9]. In the Philippines, mental health services are not fully integrated in HIV treatment hubs nor in community-based health centers. The collaborative model for instituting mental health is likewise non-existent or a weakly implemented service.
Conclusions and Recommendations
Collective findings about depression, anxiety and suicide ideation call for attention and intense efforts to deal with the mental health needs of WLHIVs in the Philippines. Although majority can be considered physically healthy with few comorbid conditions, a large percentage of them are reporting high depressive symptoms while a minority are already experiencing less moderate symptoms. It is important to note that all the participants in this study are females which by their very nature have higher propensity towards experiencing mental health issues. The multiple roles of adult women as mothers, sisters, caregivers, breadwinners and as patients are all potential sources of negative stress which translate to negative emotions.
The type of support needed by WLHIV who feel stigmatized and distressed can be deduced from the relationships of different relevant mental health variables. This could mean developing a creative menu of different forms of support which can range from personal show of compassion to promoting positive attitudes. Depression and anxiety could be reduced if clinical efforts are focused either to reducing negative emotions or to reducing HIV-related stigma. Stigma reduction should begin within the four walls of the clinic. Doctors, nurses and peer counselors could be more conscious and sensitive of how their attitudes could affect perceptions of stigma and rejection among clients. Stigma reduction programs should be incorporated in interventions with family members, caregivers, and the immediate community. HIV issues could be discussed in family counseling or group sessions with peers.Lastly, demystifying myths and misconceptions about HIV through strong media and public education campaign will help reduce negative mindset about the dreaded disease. Reaching out to key populations or those at-risk population is no exemption.
Psychosocial interventions are found to reduce depressive and anxiety symptoms for PLHIVs (see van Leunen et al., [28] for a review) even if stigma reduction is not among its goals. Online mental or psychological First Aid should be considered as a readily available intervention to help with the clientsʼ traumatic reactions to HIV and the stigma associated with it. Group interventions that revolve around the common issues of mental health could be initiated among peer groups in clinics but facilitated experienced by counselors or social workers. An intervention that could be explored is family counseling and couples therapy since perceived support from these groups were found to affect mental health. Lastly, because of high prevalence of depression and suicidal thoughts found in the study, routine screening for mental health issues should be part of the clinical protocol in any regional treatment hub. A strong referral system should be established in the absence of professional help in clinics and treatment hubs.
Acknowledgments
The researchers would like to thank the Canadian Fund for Local Initiatives, the AIDS Society of the Philippines (ASP), the HIV Treatment Hubs, and Social Hygiene Clinics for supporting this survey research.
Conflicts of Interest Statement
The authors whose names are listed immediately below certify that they have NO affiliations with or involvement in any organization or entity with any financial interest ( such as honoraria; educational grants; participation in speakersʼ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Maria Isabel E. Melgar, PhD
Chester B. Alejandro, OTRP, MA Psy
Elsa A. Chia
References
- Joint United Nations Programme on HIV/AIDS (UNAIDS). UNAIDS Data. 2021.
- Department of Health Philippines (DOH). Department of Health Epidemiology Bureau: HIV/AIDS & ART Registry of the Philippines. September 2021.
- World Health Organization. Global Health Sector Strategy on HIV 2016-2021: Towards Ending AIDS. 2016
- Arias-Colmenero T, Pérez-Morente MÁ, Ramos-Morcillo AJ, Capilla-Díaz C, Ruzafa-Martínez M, Hueso-Montoro C. Experiences and Attitudes of People with HIV/AIDS: A Systematic Review of Qualitative Studies. Int J Environ Res Public Health. 2020; 17(2): 639. doi:10.3390/ijerph17020639
- Kennedy CA, Skurnick JH, Foley M, Louria DB. Gender differences in HIV-related psychological distress in heterosexual couples. AIDS Care. 1995; 7(1): 33-38. doi:10.1080/09540129550126803
- Scholten F, Mugisha J, Seeley J et al. Health and functional status among older people with HIV/AIDS in Uganda. BMC Public Health. 2011; 11 (1). 886. doi:10.1186/1471-2458-11-886
- Mayston R, Kinyanda E, Chishinga N, Prince M, Patel V. Mental disorder and the outcome of HIV/AIDS in low-income and middle-income countries: a systematic review. AIDS. 2012; 26(2): 117-135. doi:10.1097/QAD.0b013e32835bde0f
- Performance Monitoring Report: Regional and Country Report. UNAIDS. 2020.
- Niu L, Luo D, Liu Y, Silenzio VMB, Xiao S. The Mental Health of People Living with HIV in China, 1998-2014: A Systematic Review. PLoS One. 2016; 11(4): p.e0153489. doi:10.1371/journal.pone.0153489
- Thai TT, Jones MK, Harris LM, Heard RC, Hills NK, Lindan CP. Symptoms of Depression in People Living with HIV in Ho Chi Minh City, Vietnam: Prevalence and Associated Factors. AIDS Behavior. 2018; 22 (1): 76-84. doi:10.1007/s10461-017-1946-8
- Songtaweesin WN, et al. Mental health management integration into adolescent HIV treatment services in Bangkok, Thailand. International Workshop on HIV Pediatrics. 2020.
- Gauiran DT, Samala KG, Lim JA, De Guzman MLRE. Measurement of anxiety and depression among HIV patients seen in the Philippine General Hospital using the Hospital Anxiety and Depression ScalePilipino version (HADS-P). Acta Medica Philippina. 2018; 52(1): 40-52. doi:10.47895/amp.v52i1.466
- Jareno P. Living with HIV: A Womanʼs Journey of Resiliency. AIDS Society of the Philippines Webinar. 2021.
- Ross J. Integrating mental health services into HIV clinical settings in Asia. The AIDS Society of the Philippines Mental Health in HIV Webinar. 2020.
- Uthman OA, Magidson JF, Safren SA, Nachega JB. Depression and Adherence to Antiretroviral Therapy in Low-, Middle- and High- Income Countries: A Systematic Review and Meta-Analysis. Curr HIV/AIDS Rep. 2014; 11(3): 291-307. doi:10.1007/s11904-014-0220-1
- Yi S, Chhoun P, Suong S, Thin K, Brody C, Tuot S. AIDS-Related Stigma and Mental Disorders among PLiving with HIV: A Cross-Sectional Study in Cambodia. PLos One. 2015; 10(3): eO121461. doi:10.1371/journal.pone.0121461
- Charles, B., et al. Association between stigma, depression and quality of life of people living with HIV/AIDS (PLHA) in South India-a community based cross sectional study. BMC Public Health. 2012. 12: 463. doi:10.1186/1471-2458-12-463
- Li CM, Ying FJ, Raj D, Li WP, Kudreja A, Omar SF, Kamarulzaman A, Rajasuriar R. A retrospective analysis of the care cascades for noncommunicable disease and mental health among people living with HIV at a tertiary-care center in Malaysia: Opportunities to identify gaps and optimize care. J Int AIDS Soc. 2020; 23(11): e25638. doi:10.1002/jia2.25638
- Supporting mental health and wellbeing through COVID-19: A mental health first aid approach for the busy provider. ASHM & Taskforceʼs Mental Health Cluster Group. 2020.
- Logie C, Gadalla TM. Meta-analysis of health and demographic correlates of stigma towards people living with HIV. AIDS Care. 2009; 21(6): 742-753. doi:10.1080/09540120802511877
- Kamen C, Arganbright J, Kienitz E, et al. HIV-related stigma: implications for symptoms of anxiety and depression among Malawian women. Afr J AIDS Res. 2015; 14(1): 67-73. doi:10.2989/16085906.2015.1016987
- Rueda S, Mitra S, Chen S, et al. Examining the associations between HIVrelated stigma and health outcomes in people living with HIV/AIDS: a series of meta-analyses. BMJ Open. 2016; 6(7): e011453. doi:10.1136/bmjopen-2016-011453
- Durteste M, Kyselyova G, Volokha A, et al. Anxiety symptoms and felt stigma among young people living with perinatally or behaviourallyacquired HIV in Ukraine: A cross-sectional survey. PLoS One. 2019; 14(1): e0210412. doi:10.1371/journal.pone.0210412
- Vanable PA, Carey MP, Blair DC, Littlewood RA. Impact of HIV-related stigma on health behaviors and psychological adjustment among HIVpositive men and women. AIDS Behav. 2006; 10(5): 473-482. doi:10.1007/s10461-006-9099-1
- Simbayi LC, Kalichman S, Strebel A, Cloete A, Henda N, Mqeketo A. Internalized stigma, discrimination, and depression among men and women living with HIV/AIDS in Cape Town, South Africa. Soc Sci Med. 2007; 64(9):1823-1831. doi:10.1016/j.socscimed.2007.01.006
- Turan B, Budhwani H, Fazeli PL, et al. How Does Stigma Affect People Living with HIV? The Mediating Roles of Internalized and Anticipated HIV Stigma in the Effects of Perceived Community Stigma on Health and Psychosocial Outcomes. AIDS Behav. 2017; 21(1): 283-291. doi:10.1007/s10461-016-1451-5
- Seffren V, Familiar I, Murray SM, et al. Association between coping strategies, social support, and depression and anxiety symptoms among rural Ugandan women living with HIV/AIDS. AIDS Care. 2018; 30(7): 888-895. doi:10.1080/09540121.2018.1441969
- van Luenen S, Garnefski N, Spinhoven P, Spaan P, Dusseldorp E, Kraaij V. The Benefits of Psychosocial Interventions for Mental Health in People Living with HIV: A Systematic Review and Meta-analysis. AIDS Behav. 2018; 22(1): 9-42. doi:10.1007/s10461-017-1757-y


