Research Article
Is Nuchal Cord a cause of concern?
1
Department of Obstetrics and Gynecology, Mahatma Gandhi Institute of Medical Sciences, Sewagram, India
2
Department of Radiodiagnosis, Mahatma Gandhi Institute of Medical Sciences, Sewagram, India
*Corresponding author: Surekha Tayade, Professor, Department of Obstetrics and Gynecology, Mahatma Gandhi Institute of Medical Sciences, Sewagram, 442102, India, Tel: +917887519832, E-mail: stayade@mgims.ac.in
Received: May 15, 2018 Accepted: June 19, 2018 Published: June 23, 2018
Citation: Tayade S, Kore J, Tayade A, Gangane N, Thool K, Borkar J. Is Nuchal cord a cause of concern? Madridge J Womens Health Emancipation. 2018; 2(1): 46-50. doi: 10.18689/mjwh-1000110
Copyright: © 2018 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Context: The controversy about whether nuchal cord is a cause of concern and its adverse effect on perinatal outcome still persists. Authors express varying views and hence managing pregnancy with cord around the neck has its own concerns. Thus study was carried out to find out the incidence of nuchal cord and its implications.
Method: This was a prospective, cross sectional, comparative study carried out in the Kasturba Hospital of MGIMS, Sewagram a rural medical tertiary care institute. All deliveries over a period of one year, were enrollled and studied for nuchal cord, tight or loose cord, number of turns, fetal heart rate irregulaties, pregnancy and perinatal outcome.
Results: Total women with nuchal cord in labour room were 1116 (2.56%) of which 85.21 percent had single turn around the babies neck. Most of the babies ( 77.96 %) had a loose nuchal cord, however 22.04 percent had a tight cord. Cesarean section was twice as common with nuchal cord. There was two times more risk of meconium stained liquor in nuchal cord labours and 3 times risk of abnormal fetal heart rate patterns. Apgar scores below 7 was more common in neonates with cord (33.42 %) as compared to non nuchal cord (6.69%). Admissions in neonatal intensive care unit (33.42 %) and neonatal mortality(4.39 %) were higher compared to their counterparts.
Conclusion: Nuchal cord is associated with varying degrees of intrapartum complications such as fetal heart rate irregularities, meconium staining, low Apgar scores, increased cesarean sections and increased incidence of neonatal admissions in intensive care unit. Antenatal and intrapartum vigilance is imperative for positive pregnancy outcomes.
Keywords: Nuchal Cord; Cord around neck; Neonatal morbidity; Pregnancy outcomes.
Introduction
The umbilical cord, which is the principal connection between the fetus and the placenta serves as a critical lifeline to the developing fetus, providing nutrients and oxygen. However, cord problems occur when sometimes the cord may get wrapped around the fetal neck in360 degrees and is called a nuchal cord [1]. Nuchal cords are common, with a prevalence rate of 6% to 37% and the incidence increases with advancing gestation age [2]. It appears to be a random event, with increased risk among fetuses with excessive movement and/or a long umbilical cord [3]. Nuchal cord can be single or multiple and tight or loose.”Type A” cord wraps around the neck in 360 degrees, wherein, the placental end crosses over the umbilical end, entangling the neck in an unlocked pattern whereas in “Type B” pattern the cord cannot be undone and ends up as a true knot. Here, the placental end crosses under the umbilical end, entangling the neck in a locked pattern [4].
The assumption that nuchal cord entanglement could cause cord compression and thus intra-partum complication is not recent. About 20%–60% of all foetal deaths are attributed to foetal asphyxia. Nuchal cord accident comprises 5%–18% of all foetal asphyxia cases, and 10% of stillbirth may be due to umbilical cord complications [5]. Umbilical cord compression due to tight nuchal cord may cause obstruction of blood flow in the thin walled umbilical vein, while blood continues to be pumped out of the fetus through the thicker walled umbilical arteries causing hypovolemia, acidosis and anemia [1]. An entangled cord around the neck may prevent progression of the fetal head towards the pelvic outlet and may be associated with a non reassuring fetal heart rate pattern thus contributing to fetal distress and failure of induction [6].
With the advent of ultrasound, there is an increase in the diagnosis of nuchal cord in fetuses and pregnant women regularly request antenatal ultrasound scans to look for nuchal cord in routine obstetric scans. However, the implications of nuchal cords are controversial. Several studies have noted an association between nuchal cords and adverse perinatal outcome. In contrast, others find that umbilical cord compression due to tight nuchal cords could be an incidental finding that is seldom associated with perinatal morbidity. Henry et al in his large series of 219,337 births with 6.6 percent nuchal cords found no association with adverse neonatal outcome [7]. On the other hand, in case reports and some small case series, nuchal cords have been associated with fetal demise, impaired fetal growth, meconium-stained amniotic fluid, and an increased frequency of intrapartum fetal heart rate abnormalities, operative delivery, low five-minute Apgar scores, and umbilical artery acidemia. Hippocrates talked about nuchal cord as one of the dangers of eighth gestational month, stating that a nuchal cord persisting until term, will cause suffering to the mother and either perish or bear difficulties to the fetus [8]. There are instances in which fetuses with 3 to 4 loops of cord around the neck have delivered uneventfully, vaginally, while some women have to be delivered by caesarean section for foetal distress caused by a single loop of cord around the neck. Many women have requested elective caesarean sections because nuchal cord has been detected on ultrasound scan. As the effect of a nuchal cord on the outcome of delivery is controversial, this study was planned to investigate the frequency of nuchal cords and determine its effect on perinatal outcomes.
Methods
This was a prospective, cross-sectional, comparative study done at Kasturba Hospital of Mahatma Gandhi Institue of Medical Sciences, Sewagram between January to December 2017. All women admitted to the labour and delivery unit were enrolled in the study and were studied for presence of cord around neck on ultrasound scans and at the time of delivery. Number of coils whether loose or tight, intrapartum complications, fetal heart rate patternsand perinatal outcome were noted. The cases with nuchal cord at the time of delivery were taken as study group and the cases without nuchal cord served as control group. Outcome variables between the two groups were compared. Outcome variables used were meconium staining of liquor, rate of instrumental and caesarean delivery and intrapartum fetal heart rate (FHR) irregularities. As a measure of perinatal outcome Apgar scorec<7 at 1 minute and 5 minutes and incidence of admission in neonatal intensive care unit was also observed. Relevant data was collected, cleaned, compiled, analysed and interpreted as per study objectives. Data was analysed using SPSS version 21.
Results
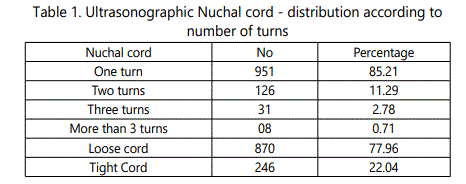
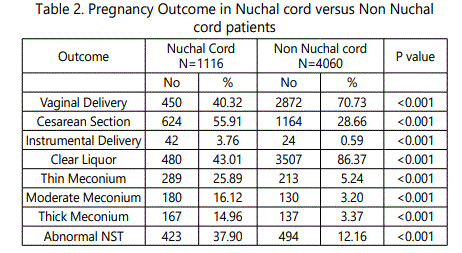
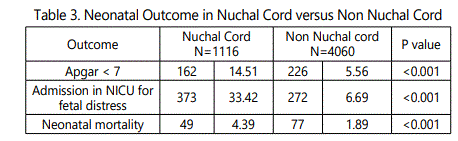
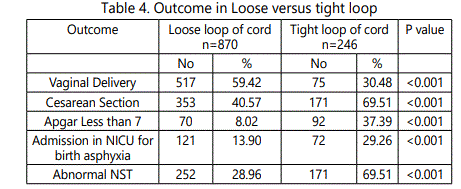
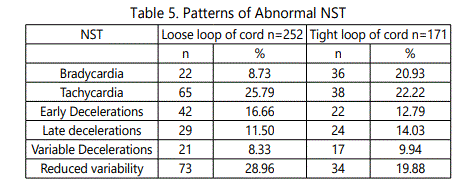
There were total 7982 admissions in maternity ward and 5176 deliveries during the study period of one year. Total women with nuchal cord in labour room were 1116(21.56 %) of which 85.21 percent had single turn around the babies neck. Most of the babies ( 77.96 %) had a loose nuchal cord, however 22.04 percent had a tight cord (table 1). Women with nuchal cord had vaginal delivery in 50.32 % as compared to 70.73 % in non nuchal cord women, and cesarean section was twice as common with nuchal cord. There was two times more risk of having meconium stained liquor in nuchal cord labours and 3 times risk of abnormal fetal heart rate patterns as compared to non nuchal nuchal cord labours (table 2). Apgar scores below 7 was more common in neonates with cord (33.42 %) as compared to non nuchal cord (6.69%), 3 times more risk ( table 3). Admissions in neonatal intensive care unit were much more common in neonates with cord around the neck (33.42 %) as compared to their counterparts (6.69 %) and neonatal mortality was high (4.39 %) with approximately 2 times more risk (table 4). Tight nuchal cord fared worse with a cesarean rate of 69.51 %, Apgar score less than 7 in 37.39 %, admissions in neonatal ICU in 29.26 % and abnormal NST in 69.51 %, all of these were significantly higher compared to loose nuchal cord. Reduced variability (28.96%) and Tachycardia (25.79 %) were more commonly seen as abnormal fetal heart rate patterns in fetuses with loose nuchal cord, and Tachycardia (22.22 %), Bradycardia (20.93%) and reduced variability were more common with tight cord (19.88 % ) (table 5).
Discussion
Nuchal cords are notorious in the way that the outcome of such preganncies is disputable. Many a times 3-4 loops of cord around neck may deliver vaginally, however sometimes a single turn of nuchal cord may prove hazardous and we may have a still birth on our hands. It is thus, very important to understand the implications of nuchal cord and devise a strategy for safe childbirth and excellent outcome.
The present study reports an incidence of 21.56 % for nuchal cord among women admitted in labour delivery unit. Various authors have reported an incidence of 6-37 percent [2]. The incidence of nuchal cords increases with increasing gestational age. At term, reported incidence ranges from 15 to 34 percent in a large series [9]. Larson et al [10] reported an incidence of 6% at 20 wks gestation and 29% at 42 weeks of gestation. Henry et al found an incidence of 14.7 % in 166,318 deliveries [7]. Incidence of nuchal cord at the time of delivery was 22.85% in Shrestha”s series [11]. Of 1254 neonates, Tamrakar et al found that nuchal cord was present in 6.85% of deliveries (n = 289). Of these, the incidence was 6.57% at preterm, 49.13% at term, 39.79% at postdated and 4.50% at postterm. Incidence of nuchal cord reported by Spellacy et al [12] was between 15.8 and 30% and by Singh et al was 18.57% [13]. Single nuchal cords are more common than multiple nuchal cords (11 to 28 percent versus 2 to 7 percent) [14,15] in most studies. Tamrakar found 151 had one loop (52.24%) and 138 had two or more loops(47.75%) [16]. Incidence of single nuchal cord was 18.95% in Shresthas series. In one study, the incidence of single, double, triple, and quadruple nuchal cords at delivery was reported to be 10.6, 2.5, 0.5 and 0.1 percent, respectively [17]. Present study reports single nuchal cord in 85.21 %of all nuchal cord cases (18.37 % of deliveries). Loose loop of cord is more commonly found and fairs better than tight cord for obvious reasons. Henry, et al [7] observed tight nuchal cord in 6.6% and 21.6% loose nuchal cord.Present study found loose nuchal cord in 16.80% and a tight cord in 4.76 %.
Clinically, nuchal cords prior to delivery can be assessed by transabdominal manual compression of the fetal neck. If fetal heart rate deceleration is observed, the test is positive. This indicates impending risk of cord compression and suggests close FHR monitoring. Mendez-Bauer, et alfound a sensitivity of 82.3% and specificity 89.1%for this test. These results were statistically significant in both late pregnancy and labor [18]. Routine use of this test can contribute to decreasing perinatal morbidity and diminishing the impact of cord problems by early recognition and appropriate decisions. Ultrasonography with color doppler imaging is considered the gold standard for diagnosing nuchal cord and requires some expertise to categorise the event [19]. Ultrasound correctly identifies 72% of single and 94% of multiple nuchal cords, with greatest sensitivity after 36 weeks (93% vs. 67%). “Divot” sign, a circular indentation of the fetal nuchal skin is charecteristic, however, posterior cystic masses, folds of skin, or amniotic fluid pockets have to be ruled out [20]. Both longitudinal and transverse views of the fetal neck should be obtained. Color Doppler imaging or Doppler flow velocimetry enhances sensitivity. Nuchal cords are easier to detect when there are multiple loops. Subjective assessment of the ease of visualization of nuchal cord was best with three-dimensional sonography [21].
One can also diagnose presence of nuchal cords noninvasively prior to delivery, by using vibroacoustic stimulation which elicits fetal heart rate decelerations. The incidence of nuchal cord was significantly higher for the group with a response pattern of fetal heart rate acceleration followed by deceleration than for the acceleration or noresponse groups (39.2% versus 10.5% versus 11.1%; P<.05) [22]. During labour, the only indication of a nuchal cord or a cord being around the babies body may be variable foetal heart decelerations more likely seen with uterine contractions as this is the time the cord gets stretched more tightly. Intrapartum complications like FHR irregularities and meconium staining of liquor are thus increased in nuchal cord group [11]. One of the causes of variable decelerations in antenatal fetal heart rate monitoring is nuchal cord. Higher rates of labor induction and non-reassuring fetal heart rate patterns were noted among pregnancies with nuchal cord as compared with the control group (30.1% vs. 24.2%; OR=1.3, 95% CI 1.3-1.4, P<0.001 and 4.5% vs. 2.6%; OR=1.8, 95% CI 1.6-1.9, P<0.001; respectively) [9]. The present study found 3 times more risk of abnormal fetal heart rate patterns as compared to non nuchal nuchal cord labours, tachycardia and reduced variability being the commonest patterns. Other studies too found that fetal bradycardia and variable decelerations in fetal heart rate occurred almost twice as often in the nuchal cord group (18.6% as compared with 9.6%, (P less than .01) [23]. Two large retrospective studies including approximately 38,000 fetuses with a nuchal cord at birth reported a 60 to 80 percent increase in abnormal fetal heart rate tracings compared with pregnancies with no nuchal cord, although the cesarean delivery rate was not increased [9]. Multiple nuchal cords appear to increase the risk of an abnormal FHR trace [15]. Some prospective studies on the other hand of newborn outcomes after antenatal identification of nuchal cords have generally not described increased rates of nonreassuring FHR patterns or operative delivery [21]. However, these studies included less than 400 subjects.
Nuchal cord may be considered worse than strangulation, since in nuchal cord, umbilical cord itself acts as a noose while carrying blood supply with oxygen and umbilical vein being more vulnerable to collapse. Many of infants with nuchal cord pass meconium, which is probably an indication of vagal collapse. Present study found twice as risk of meconium staining in nuchal cord.
Traditionally, a cord entanglement around the fetal neck during the labor is regarded as a cause of fetal distress. However, whether or not nuchal cords are associated with significantly increased adverse perinatal outcome is debated [23]. Some Authors [24] reported that the nuchal cord is associated with an increased risk of fetal distress, meconiumstained amniotic fluid and lower Apgar score whereas others [25] did not find an increased frequency of nonreassuring FHR patterns, operative vaginal delivery and low Apgar score. In a very large study including more than twenty thousand pregnancies with nuchal cord documented at birth, Sheiner et al reported a higher rate of labour induction and not reassuring fetal heart pattern, but no significant association with perinatal mortality or caesarean section [9]. The present study however reports a significantly higher ceasarean rate ( twice as common, (55.91 % versus 28.66%). Another study found that Instrumental delivery rate was high in nuchal cord group but statistically not significant (0.108). However, caesarean section rate was high in the group with nuchal cord (p=0.029) [11].
A correlation between nuchal cord and induction of labour has been noted, being still uncertain if nuchal cord incidence is increased by labour induction or if pregnancies with nuchal cord more frequently undergo labour induction. In a population-based case-control study, induction of labour has been shown to be significantly associated with a higher prevalence of nuchal cord at delivery [24]. This association may be related to increased uterine activity, which may be caused by agents used for induction of labour and may affect the umbilical cord position. Ogueh et al in 2006 confirmed a higher prevalence of umbilical cord around the neonatal neck in pregnancies having undergone induction of labour and reported an association between nuchal cord and increased second stage of labour [26]. However, the presence of nuchal cord did not seem to be more likely also when caesarean section was performed due to suspected fetal distress. However, other studies have reported no correlation between nuchal cord and cesarean section rates. In our study, percentage of caesarean and forceps delivery was more common in test as compared to control group although difference was not statistically significant. Miser et al [23] observed that there was no significant difference in number of operative deliveries between nuchal cord and non-nuchal cord group. Larson et al also reported that caesarean delivery was not more common in multiple entanglement that the control group [15].
Shrestha found that Apgar score<7 at 1 minute was significantly low in nuchal cord group (p=0.010) but apgar score at 5 minutes and admission to neonatal unit was not more common [11]. Similarly one minute Apgar scores were lower in nuchal cord group in present study (14.51% vs 5.56 %). A significant umbilical arterial acidosis can occur in nuchal cord infants even in the setting of normal or near normal Apgar scores with intrapartum period as the necessary key factor. The established terminology ‘Compression Asphyxiaʼ in forensic medicine could be applied to these infants with tight nuchal cords because of the similarities in their pathophysiological mechanisms and clinical findings [27]. This may help in distinguishing birth asphyxia from infant with the effects of a tight nuchal cord. In a large retrospective study, term neonates with a tight nuchal cord were slightly more likely to be admitted to a neonatal intensive care unit similar to the present study [1].
Baergen, et al [28] found that as many as 20% of stillbirths at autopsy are due to fatal compromise of umbilical circulation. Parast et al, for the first time established evidence of placental histologic criteria for umbilical blood flow restriction (cord accident) in unexplained stillborns [29]. Present study found that neonatal mortality was 4 times higher in nuchal cord. A nuchal cord at the onset of labor is very unlikely to correct itself. It hardly matters whether the cord is wrapped around the neck, or the shoulder or the leg, the outcome can be the same. Everything may be fine throughout the entire pregnancy; however, at the time of delivery, as the foetus moves into the birth canal, the cord can become stretched or compressed. All of these problems are rare and unfortunate but natural processes. It is the task of the obstetrician to recognise the signs of foetal distress and to act swiftly before the reduction in oxygenation causes permanent injury [30]. Tight cord have poorer neonatal outcome as compared to loose cord and need more vigilance.
Conclusion
Encirclement of umbilical cord around foetal neck (nuchal cord) is not an uncommon occurrence and can be detected very well on ultrasonography when combined with Colour Doppler. The incidence of nuchal cords increases with increasing gestational age with single loop of nuchal cords being more common than multiple and many a times they are loose. Pregancy outcomes are negatively affected with abnormal fetal heart rate patterns, meconium staining of amniotic fluid and increased cesarean section rates. Nuchal cord is also related to increased foetal morbidity and mortality, low APGAR score and increased NICU admissions. Tight cord is associated with poorer neonatal outcome as compared to loose cord, with higher FHR abnormalities, more cesarean section rates, lower Apgar scores and increase NICU admissions. The obstetrical challenge of the clinical management of nuchal cords depends upon number of involved nuchal loops, the amniotic fluid index, the gestational age, and the fetal growth. A prolonged persistent nuchal cord with poor fetal growth deserves close monitoring and delivery as appropriate. Some obstetricians opt to deliver early when multiple nuchal cord loops are noted on fetal scans. Presence of variable decelerations during fetal heart rate monitoring is indicative of possible presence of nuchal cord. Antenatal nuchal cord particularly in later gestational age and in prelabor warrents close monitoring of fetus and appropriate intervention is desired.
Acknowledgement
We are grateful to the department of Obstetrics and Gynaecology and Department of Radiodiagnosis, MGIMS, Sevagram and Hospital Information System, for helping us in conducting this study.
Conflict of Interest
The authors confirm that there is no conflict of interest regarding this manuscript.
References
- Peesay M. Nuchal cord and its implications. Matern Health Neonatol Perinatol. 2017; 3: 28. doi: 10.1186/s40748-017-0068-7
- Jouppila P, Kirkinen P. Ultrasonic diagnosis of nuchal encirclement by the umbilical cord: A case and methodological report. J Clin Ultrasound. 1982; 10(2): 59-62. doi: 10.1002/jcu.1870100205
- Sherer DM, Abramowicz JS, Hearn-Stebbins B, Woods JR Jr. Sonographic verification of a nuchal cord following a vibratory acoustic stimulationinduced severe variable fetal heart rate deceleration with expedient abdominal delivery. Am J Perinatol. 1991; 8(5): 345-346. doi: 10.1055/s-2007-999411
- Collins JH. Umbilical cord accidents: human studies. Semin Perinatol. 2002; 26(1): 79-82.
- Singer D, Macpherson T. Fetal death and the macerated stillborn fetus. Textbook of fetal and perinatal pathology. 1991;1:266-267.
- Ghi T, DʼEmidio L, Morandi R, Casadio P, Pilu G, Pelusi G. Nuchal cord entanglement and outcome of labour induction. J Prenat Med. 2007;1(4):57-60.
- Henry E, Andres RL, Christensen RD. Neonatal outcomes following a tight nuchal cord. J Perinatol. 2013; 33(3): 231-234. doi: 10.1038/jp.2012.79
- Phadol VA, Naik AS, Naik SA. Nuchal cord and perinatal outcome in a rural hospital: a case control study. J Evolution Med. Dent Sci. 2016; 5(53): 3531- 3535. doi: 10.14260/jemds/2016/814
- Sheiner E, Abramowicz JS, Levy A, Silberstein T, Mazor M, Hershkovitz R. Nuchal cord is not associated with adverse perinatal outcome. Arch Gynecol Obstet. 2006; 274(2): 81-83. doi: 10.1007/s00404-005-0110-2
- Clapp JF 3rd, Stepanchak W, Hashimoto K, Ehrenberg H, Lopez B. The natural history of antenatal nuchal cords. Am J Obstet Gynecol. 2003; 189(2): 488-493.
- Shrestha NS, Singh N. Nuchal cord and perinatal outcome. Kathmandu Univ Med J (KUMJ). 2007; 5(3): 360-363. doi: 10.1016/S0029-7844(02)02931-9
- Spellacy WN, Gravem H, Fisch RO. The umbilical cord complications of true knots, nuchal coils, and cords around the body: Report from the collaborative study of cerebral palsy. Am J Obstet Gynecol. 1966; 94(8):1136-1142. doi: 10.1016/0002-9378(66)90777-0
- Singh G, Sidhu K. Nuchal cord: a retrospective analysis. Med J Armed Forces India. 2008; 64(3): 237-240. doi: 10.1016/S0377-1237(08)80102-5
- Schaffer L, Burkhardt T, Zimmermann R, Kurmanavicius J. Nuchal cords in term and postterm deliveries--do we need to know? Obstet Gynecol. 2005; 106(1): 23-28. doi: 10.1097/01.AOG.0000165322.42051.0f
- Larson JD, Rayburn WF, Crosby S,Thurnau GR. Multiple nuchal cord entanglements and intrapartum complications. Am J Obstet Gynecol. 1995; 173(4): 1228-1231.
- Tamrakar SR. Incidence of nuchal cord, mode of delivery and perinatal outcome: a notable experience in Dhulikhel Hospital - Kathmandu University Hospital. Nepal Med Coll J: NMCJ. 2013; 15(1): 40-45.
- Kan Pun S, Eastman NJ. Coiling of the umbilical cord around the foetal neck. J Obstet Gynaecol Br Emp. 1957; 64(2): 227-228.
- Mendez-Bauer C, Troxell RM, Roberts JE, Firman SM, Dubois JF, Menendez A, et al. A clinical test for diagnosing nuchal cords. J Reprod Med. 1987; 32(12): 924-927.
- Jauniaux E, Mawissa C, Peellaerts C, Rodesch F. Nuchal cord in normal third-trimester pregnancy: a color Doppler imaging study. Ultrasound Obstet Gynecol. 1992; 2(6): 417-419. doi: 10.1046/j.1469-0705.1992.02060417.x
- Ranzini AC, Walters CA, Vintzileos AM. Ultrasound diagnosis of nuchal cord: the gray-scale divot sign. Obstet Gynecol. 1999; 93(5 Pt 2): 854.
- Peregrine E, OʼBrien P, Jauniaux E. Ultrasound detection of nuchal cord prior to labor induction and the risk of Cesarean section. Ultrasound Obstet Gynecol. 2005; 25(2): 160-164. doi: 10.1002/uog.1767
- Anyaegbunam AM, Ditchik A, Stoessel R, Mikhail MS. Vibroacoustic stimulation of the fetus entering the second stage of labor. Obstet Gynecol. 1994; 83(6): 963-966.
- Miser WF. Outcome of infants born with nuchal cords. J Fam Pract. 1992; 34(4): 441-5.
- Rhoades DA, Latza U, Mueller BA. Risk factors and outcomes associated with nuchal cord. A population-based study. J Reprod Med. 1999; 44(1): 39-45.
- Mastrobattista JM, Hollier LM, Yeomans ER, Ramin SM, Day MC, Sosa A, et al. Effects of nuchal cord on birthweight and immediate neonatal outcomes. Am J Perinatol. 2005; 22(2): 83-85. doi: 10.1055/s-2005-837737
- Ogueh O, Al-Tarkait A, Vallerand D, Rouah F, Morin L, Benjamin A, et al. Obstetrical factors related to nuchal cord. Acta Obstet Gynecol Scand. 2006; 85(7): 810-814. doi: 10.1080/00016340500345428
- Sauvageau A, Boghossian E. Classification of asphyxia: the need for standardization. J Forensic Sci. 2010; 55(5):1259-1267. doi: 10.1111/j.1556-4029.2010.01459.x
- Baergen RN. Cord abnormalities, structural lesions, and cord “accidents”. Semin Diagn Pathol. 2007; 24(1): 23-32. doi: 10.1053/j.semdp.2007.02.004
- Parast MM, Crum CP, Boyd TK. Placental histologic criteria for umbilical blood flow restriction in unexplained stillbirth. Hum Pathol. 2008; 39(6): 948-953. doi: 10.1016/j.humpath.2007.10.032
- Joshi K, Saxena R, Bhat M, Lomrod Y, Verma K. Incidence of cord around the neck and its effects on labour and neonatal outcome. Advances Human Biology. 2017; 7(1): 15-18. doi: 10.4103/2321-8568.199535


