Research Article
Perceptions of Perinatal Anxiety, Depression, and Mental Health treatment in a Low-Income, Latina Population
1
Department of Psychiatry, University of Southern California, USA
2
Department of Psychiatry and Biobehavioral Sciences, Semel Institute, University of California, Los Angeles, USA
3
Department of Obstetrics and Gynecology, University of Southern California, USA
*Corresponding author: Jamie Lim Lacsina, Department of Psychiatry, University of Southern California, 2250 Alcazar St. #2200, Los Angeles, CA 90033, USA, Tel: 323-226-5555, E-mail: jllacsina@gmail.com
Received: September 01, 2017 Accepted: September 18, 2017 Published: September 22, 2017
Citation: Lacsina JL, Tang VK, Wolitzky-Taylor K, Brueggmann D, Jaque J, Dossett EC. Perceptions of Perinatal Anxiety, Depression, and Mental Health treatment in a Low-Income, Latina Population. Madridge J Womens Health Emancipation. 2017; 1(1): 22-28. doi: 10.18689/mjwh-1000106
Copyright: © 2017 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
This study examined the perceptions of Latina women regarding perinatal mental health and its treatment. Ninety-five women completed a 60-item Perinatal Mental Health Questionnaire (PMHQ). Responses to items were compared between women who completed the questionnaire in English versus Spanish. In regards to the effects of anxiety or depression on the fetus or breastfeeding infant, both English and Spanish participants expressed concern over potential high levels of harm. Despite this, both groups viewed psychotropic medication during the perinatal period to be unsafe. There was a significant difference when it came to therapy (p<0.001), with those completing Spanish questionnaires finding therapy during pregnancy to be less acceptable. A clear gap existed between the perceived high risks of untreated perinatal depression or anxiety and the low acceptability of mental health services. Understanding these results may lead to increased treatment rates and improve long-term health outcomes for both Latina mothers and their infants.
Keywords: Perinatal anxiety; Depression; Latina; Low income; Postpartum depression.
Introduction
Perinatal depression and anxiety disorders are associated with adverse long-term
health effects for both mothers and infants [19, 30]. As a result, improving mental health
interventions during this critical time period may have important consequences for
women and their children. A systematic review of studies predominantly performed in
high-income countries estimated the prevalence of major depressive disorder to be
between 3.1% and 4.9% during pregnancy and 4.7% in the first three months postpartum.
When minor depression was included, prevalence was estimated to be up to
11% in pregnancy and 13% in the first three months post-partum [13]. In terms of
anxiety, a study done in the U.S. found a prevalence of 13% of anxiety disorder in
pregnant women or post-partum women in the past year [35]. In addition, up to onethird
of women experiencing postpartum depression also meet criteria for postpartum
anxiety disorder, suggesting significant comorbidity rates [28]. According to a 2010 U.S.
Census report, more than half of the growth in the total population of the United States
between 2000 and 2010 was due to the increase in the Latino population [9]. Although
research has been limited, studies of perinatal Latinas have reported prevalence of high
depressive symptoms to be between 15-31% [6, 17].
Evidence-based treatments exist for postpartum
depression [19]. A Cochrane review showed that psychosocial
and psychological interventions were effective for reducing
depression symptoms within the first year postpartum [7].
Antidepressants have been shown to be especially effective in
severe cases of perinatal depression, and a meta-analysis
found that the efficacy of antidepressants increased with the
severity of depression [12, 19]. Good evidence exists for the
effectiveness of non-pharmacological treatment during the
antenatal period, including cognitive-behavioral therapy and
interpersonal psychotherapy [19]. Despite the existence of
these treatments, studies have shown that a low percentage
of women with depression actually receive any interventions
during pregnancy or the postpartum period [14, 18].
Matching patients with their preferred treatment for
depression is associated with a more rapid improvement in
depression symptomatology [26]. Several studies have looked
at preferences and attitudes regarding treatment for
depression and demonstrated that women with depression
prefer non-pharmacological intervention over antidepressants
[8, 14, 33]. Research shows that minority women have less
preference for SSRIs than U.S.-born Caucasian women [1, 5,
27] and group therapy endorsement is high among immigrant
Latinas [27]. A qualitative study by Lara-Cinisomo et al.
specifically looked at perinatal depression treatment
preferences among Latina mothers. Results showed that
preferences consisted of a pathway approach. This began with
the use of oneʼs own resources followed by the use of formal
support systems and supplemented by the use of behavioral
therapy. Antidepressant use was seen to be acceptable only in
severe cases [24].
Because there have been few studies on the preferences
of women, especially Latinas, regarding treatment for perinatal
anxiety or depression, more research is needed. This study
seeks to add to existing literature by examining perceptions
of perinatal anxiety, depression, and mental health treatment
in a low-income, Latina population at Los Angeles County +
USC Medical Center (LAC+USC). LAC+USC Medical Center is
one of the largest public hospitals in the United States, and it
provides healthcare services for the regionʼs medically
underserved. The majority of patients at LAC+USC are Latino,
many of whom are Mexican or from Central America. A
significant proportion of patients at LAC+USC, of all ethnic
and racial backgrounds, are facing stressors of poverty,
trauma, and fractured social support systems. As a result,
these individuals are at an increased risk of developing mental
health concerns.
Methods
Sample
Participants were recruited from an outpatient OB-GYN/
prenatal clinic at Los Angeles County + USC Medical Center.
They included women seeking obstetric and gynecological
care who were both pregnant and not pregnant. Detainees as
well as minors were excluded. As the study is regarding
perinatal mental illness, male participants were also excluded. Finally, because the questionnaire was only provided in
English and Spanish, those who could not read or understand
either of these languages were excluded. University of
Southern California Health Science Campus Institutional
Review Board approval was received, and informed consent
was obtained from all participants.
Perinatal Mental Health Questionnaire
Participants were asked to complete a 60-item
questionnaire to assess their knowledge and understanding
of perinatal depression and anxiety. The questionnaire also
contained items that addressed personal psychiatric history
and past medical history as well as basic demographics such
as age and ethnicity. After the researchers developed the
items, they were further refined using two focus groups.
Recruitment of focus groups, consisting of a minimum of ten
participants, aimed to represent diversity in age and
educational backgrounds. The first focus group was asked to
give feedback on the clarity of items. The revised questionnaire
was then sent to a second focus group for final feedback. The
questionnaire was then translated into Spanish.
Questionnaires were distributed by a medical student
who was uninvolved in patient care. Patients waiting in the
prenatal care clinic waiting room were asked if they wanted to
participate in the study. If they indicated that they did, they
were given a study information sheet explaining the purpose
of the study and that their choice to participate would not
affect their care (these were in English and Spanish). The
medical student was available to answer any questions
regarding the questionnaire. After completing the survey,
patients returned it to the medical student who placed
completed surveys in a secure box.
Screening for Anxiety and Depression
In addition to the 60-item Perinatal Mental Health Study
Questionnaire, participants were also asked to complete the
Patient Health Questionnaire 9-item (PHQ-9) and Generalized
Anxiety Disorder 7-item (GAD-7), which are validated
screening tools for depression and anxiety, respectively. Based
on a well-known systematic review published by Kroenke et
al., cut points of 5, 10, and 15 were used to represent mild,
moderate, and severe symptom levels on the PHQ-9 and
GAD-7 [22]. We used a cut point of 5 to include women with
mild symptoms of depression or anxiety in our analyses. Upon
completion of the PHQ-9, the medical student evaluated each
survey for signs of suicide risk. If there was any concern for
suicidality, a mental health professional was immediately
notified and the patient evaluated. Of note, all women who
receive care at the LAC+USC outpatient OB-GYN clinic where
this study took place are screened for anxiety and depression.
This screening did not impact the selection of women to
participate in the study. Mental healthcare services and social
support are provided to all those who demonstrate need.
Measuring Perceptions
To measure perceptions regarding medication use during
pregnancy, we calculated a composite score based on
responses to Questions 1M-3M (Table 1). Similarly, we derived composite scores for perceptions regarding therapy during
pregnancy (Table 2) as well as understandings of the effects of
anxiety or depression on the developing fetus and infant
(Table 3).

For each participant, a medication perceptions score was calculated by taking the sum of responses to Questions 1M-3M.For example, if a participant answered “Very Likely” to 1M, “Somewhat Safe” to 2M, and “A Little Safe” to 3M, her composite score would be 1 + 2 + 3 = 6

For each participant, a therapy perceptions score was calculated by taking the sum of responses to Questions 1T-3T.For example, if a participant answered “Very Likely” to 1T, “Definitely Acceptable” to 2T, and “Maybe Acceptable” to 3T, her composite score would be 1 + 1 + 3 = 5

For each participant, a fetal/infant harm perceptions score was calculated
by taking the sum of responses to Questions 1F and 2F.For example, if a
participant answered “Very Much” to 1F and “A Little Bit” to 2F, her
composite score would be 1 + 3 = 4
The internal consistencies of the created composite scores
representing “medication perceptions, “therapy perceptions,”
and “fetal/infant harm” ranged from acceptable to excellent,
with Cronbachʼs α = 0.71, 0.63, and 0.84, respectively.
Analyses
Analyses were performed using SPSS version 22. T-tests
and ANCOVAs were used to examine between-group (i.e.,
survey language) differences on continuous variables.
Specifically, t-tests were conducted with language of the survey (English v. Spanish) as the independent variable and
the medication perceptions score, therapy perceptions score,
and fetal/infant harm perceptions score as the dependent
variables. Next, a series of ANCOVAs were performed with
survey language as the independent variable and the
aforementioned composite scores as the dependent variables.
Age, pregnancy status (yes v. no), and current anxiety or
depression status (yes v. no) were covariates. This follow-up
ANCOVA was conducted to determine whether survey
language had a significant effect on the composite scores
after accounting for variance explained by these potential
confounding variables (age, pregnancy status, current anxiety/
depression status).
Results
A total of 100 women consented to participate in our study, with 95 completing the Perinatal Mental Health Study Questionnaire. The majority of our sample was Latina (75.8%). Of those born outside of the U.S. (60.1%), the majority was born in Mexico (57.9%) followed by El Salvador (12.3%). Of the 51 participants who completed the questionnaire in English, 3.9% screened positive for severe depression (PHQ-9 ≥ 15). Of the 44 participants who completed the questionnaire in Spanish, 4.5% screened positive for severe depression (PHQ-9 ≥ 15). Sample descriptive statistics are summarized in Table4.
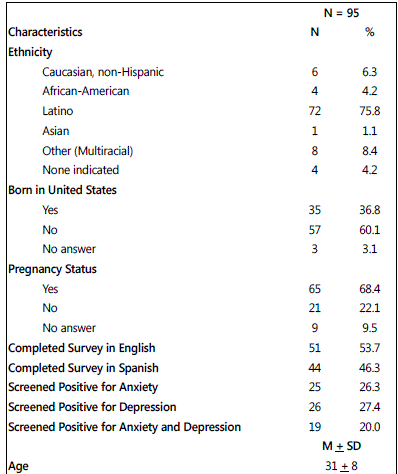
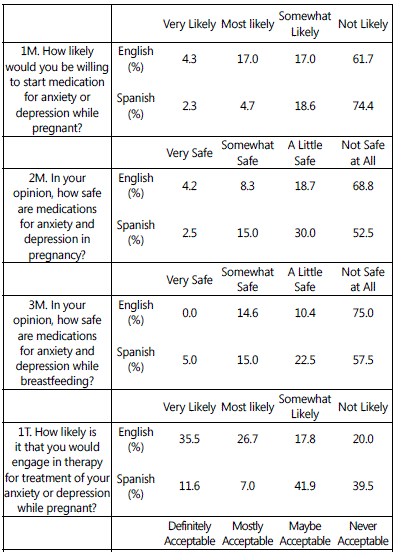
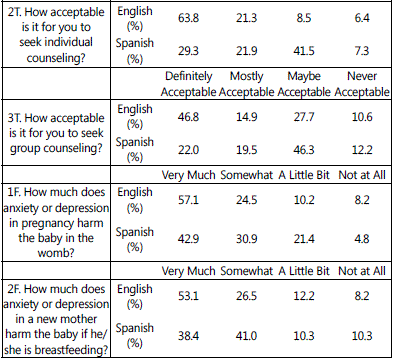
Table 5 shows the percentage distributions of responses to questionnaire items used to derive the medication perceptions score (Table 1), therapy perceptions score (Table 2), and fetal/infant harm perceptions score (Table 3).
There were no significant differences between women
completing the English v. Spanish language surveys on
medication perceptions, p =0.57. This finding remained nonsignificant
after covarying for age, pregnancy status, and
anxiety/depression status in an ANCOVA (p = 0.68). Notably,
none of the covariates were significantly associated with the
medication perceptions score (all ps > 0.15).
In contrast, there was a significant difference between
English and Spanish language participants on therapy
perceptions, t(83) = -3.75, p < 0.001. Those completing
Spanish language surveys had higher mean composite scores
than those completing English language surveys, indicating
that those who completed Spanish language surveys found
therapy during pregnancy to be less acceptable than those
who completed English language surveys. There continued to
be a significant difference in therapy perceptions scores
(English vs. Spanish) after including the covariates in an
ANCOVA, F (4, 77) = 8.09, p < 0.01. With all ps = 0.08, none of
the covariates were significantly associated with therapy
perceptions score.
Finally, there were no significant differences between
women completing surveys in English v. Spanish in regards to
the fetal/infant harm perceptions score, p =0.94. In terms of
the question, “How much does anxiety or depression in
pregnancy harm the baby in the womb?” 81.6% of those
completing English surveys and 73.8% of those completing
Spanish surveys responded “Very Much” or “Somewhat”
(Table 5). Again, no significant difference remained when
covarying for age, pregnancy status, and anxiety/depression
status in an ANCOVA (p = 0.68). In addition, none of the
covariates were significantly associated with the fetal/infant
harm perceptions score (all ps > 0.11).
Discussion
In summary, there was a significant difference between
English versus Spanish language groups regarding therapy
perceptions, with those who completed Spanish language
surveys finding therapy during pregnancy to be less acceptable
than those who completed English language surveys. In
contrast, there was no difference in language groups regarding
medication perceptions. Similarly, there was no significant
difference in the perception of the effects of anxiety or
depression on the fetus or breastfeeding infant. Both English
and Spanish participants endorsed concern about potential
high levels of harm.
In our study, 3.9% of the English questionnaire group and
4.5 % of the Spanish questionnaire group screened positive
for severe depressive symptoms (PHQ-9 > 15). These rates
were much lower than the range of 15-31% of high depressive
symptoms that have been reported in other studies focusing
on Latinas [6, 17]. One reason for these differences could be
the use of different depression scales. The Beck Depression
Inventory and Center for Epidemiologic Studies Depression
(CES-D) have been used in addition to the PHQ-9 to assess
perinatal depression. When looking at these three measures,
the number of items as well as cut-off scores corresponding
to mild, moderate, or severe depression differ [6, 17, 23].
Another explanation for our findings might be that
depression rates vary depending on pregnancy status or stage
of pregnancy. In our study, 68.4% of the women were
pregnant, while in a perinatal depression study done by
Heilemann et al., only 45.7% of the sample was pregnant versus 54.3% post-partum [17]. Heilemann et al. found higher
rates of severe depression, which could be a reflection of the
higher ratio of post-partum to pregnant women in their
sample [17]. In our questionnaire, we did not ask pregnant
women how many weeks gestation they were; future studies
looking at depression across different stages of pregnancy are
needed. Overall, because there were so few women who
screened positive for severe depressive symptoms in our
study, the perceptions regarding medication, therapy, and the
effects of anxiety or depression on the fetus/infant reflect
those of women who denied depression or who were mildly
to moderately depressed. This was confirmed statistically with
an ANCOVA that showed that none of our perception scores
were significantly associated with the anxiety/depression
status of participants.
When therapy perception scores (Table 2) were compared
between participants who completed the questionnaire in
Spanish versus English, there was a significant difference. Those
completing the survey in Spanish found engaging in therapy as
well as individual and group therapy less acceptable overall. A
study looking at mental health utilization by Latino immigrants
reported that one-third of the participants cited the combination
of their lack of ability to speak English and service providersʼ
lack of ability to translate into Spanish significantly prevented
their help-seeking [3]. In the clinic where this study took place,
there were few healthcare providers, let alone mental healthcare
providers, who spoke Spanish fluently. In addition, translation
for patients is often performed using a phone service. As a
result, participants who were not as proficient in English might
view therapy as less effective and/or more time-consuming
given the lack of Spanish-speaking providers and reliance on
phone translation services.
Another possible explanation for our findings is a greater
fear of negative consequences as a result of therapy by
participants who preferred Spanish versus English. A qualitative
study looking at depression care in obstetric settings found
that participants were less likely to disclose symptoms of
depression and/or intrusive thoughts due to the threat of
child protective services and involuntary psychiatric
hospitalization [4]. Although we did not ask about immigration
status, for our participants who preferred Spanish, deportation
might also be a feared consequence of disclosing information,
perhaps more so than participants who preferred English. To
better understand and interpret our results, we plan to do a
follow-up study involving in-depth focus groups with women
from the same county outpatient clinic.
When calculated medication perception scores (Table 1)
were compared between participants who took the survey in
Spanish vs. English, there was no significant difference. This
implied that being more fluent in English, and perhaps living
in United States longer, did not affect a womanʼs perception
of how safe medications were while pregnant or breastfeeding.
This is consistent with studies done in the general
population that report pregnant and post-partum women
generally find psychotropic medication to be unacceptable [2,
29, 36]. Potential reasons for this include mixed messages from the media and care providers regarding the safety of
medications in pregnancy. Women might also be concerned
about becoming addicted to medication or potential side
effects. Finally, the stigma of having a mental illness and
having to take medications to control it could also account for
the unacceptability of antidepressants.
The greatest proportion of women in both English and
Spanish language groups selected “Very Much” when asked
how much they believed anxiety or depression harm a
developing fetus or baby (Table 5). When fetal/infant harm
perception scores (Table 3) were compared between these
two groups of participants, there was no significant difference.
Both groupsʼ preferences were consistent with current
research linking both maternal antenatal and postnatal
depression to adverse effects in fetal and childhood
development [30]. Symptoms of antenatal depression are
associated with an increased risk for premature delivery [15,
16], child emotional problems [25, 34] as well as low levels of
general cognitive development, including IQ scores [10, 21].
Postpartum depression has been associated with increased
problems with emotional regulation and social behavior in
infants [11, 28] and adverse development in social, emotional,
and cognitive domains in children [20, 30, 31].
Despite the majority of women in both English and
Spanish groups believing that anxiety or depression is harmful
to the baby in the womb and during breastfeeding, most of
our sample expressed how it would not be likely that they
would start medication. There was also reluctance by the
Spanish group to engage in therapy as treatment. These
findings suggest that women in our study perceived the
unacceptability of psychotropic medication or psychotherapy
to be greater than the risks of being anxious or depressed
while pregnant. This is significant because it implies that
women need mental health services that fall outside those
traditionally offered in medical settings to address the real
dangers they sense from untreated perinatal mood disorders.
One of the biggest limitations of this study was its crosssectional
design. As a result, only perceptions at one point of
time could be examined and analyzed. To make sure time-related
factors such as a participantʼs age or pregnancy status
were not associated with perception scores, we used ANCOVA
analysis to determine if our results still remained significant or
non-significant when taking these factors into account. In
each case, age and pregnancy status were not associated with
composite scores. In addition, formal reliability and validity
testing of our questionnaire items was not conducted.
Participants were screened for anxiety or depression, however,
using well-validated instruments such as the PHQ-9 and GAD-
7. To make composite scores better estimates of overall
perceptions, more questionnaire items could have been
developed and used to calculate composite scores. Despite
this, measures of internal consistency for the medication
perceptions score, therapy perceptions score, and fetal/infant
harm perceptions scores were found to be acceptable or
excellent in each case. Finally, only ninety-five women, all of
whom were volunteers, were included in our study. Because of the small sample size and the fact that strict random
sampling was not employed, there could be biases in the data
set that limit extrapolation to larger populations.
Conclusions
Perinatal depression and anxiety can have lifelong
consequences for mothers and their infants. In our study,
most women in both language groups believed that anxiety
or depression is harmful to the developing fetus or infant, but
also expressed reluctance to engage in allopathic or
psychological mental health services, even when located in a
prenatal care clinic. The majority expressed how unlikely they
would be to take psychotropic medication while pregnant or
breastfeeding. A significant difference between participants
who completed our survey in Spanish versus English was
found in regards to perceptions of therapy as an intervention
for perinatal anxiety or depression. To address this gap
between knowledge of illness and treatment acceptability, we
plan to do a qualitative study where in-depth focus groups
can provide better insight into our findings. It is our hope that
this research will help improve perinatal mental health services
for Latinas and encourage future collaborations between the
fields of psychiatry and obstetrics.
Conflicts of interest, Ethical Approval, Certification of
Responsibility
The authors declare that they have no conflicts of
interest. All procedures performed in this study involving
human participants were in accordance with the ethical
standards of the University of Southern California Health
Science Campus Institutional Review Board as well as the 1964
Helsinki declaration and its later amendments. Informed
consent was obtained from all individual participants included
in this study. All authors certify their responsibility for this
manuscript.
References
- Alvidrez J, Azocar F. Distressed womenʼs clinic patients: preferences for mental health treatments and perceived obstacles. Gen Hosp Psychiatry. 1999; 21(5): 340-347.
- Bonari L, Koren G, Einarson TR, Jasper JD, TaddioA , Einarson A. Use of antidepressants by pregnant women: evaluation of perception of risk, efficacy of evidence based counseling and determinants of decision making. Arch Womens Ment Health. 2005; 8(4): 214-220. doi: 10.1007/ s00737-005-0094-8
- Bridges AJ, Andrews AR 3rd, Deen TL. Mental health needs and service utilization by Hispanic immigrants residing in mid-southern United States. J Transcult Nurs. 2012; 23(4), 359-368. doi: 10.1177/1043659612451259
- Byatt N, Biebel K, Friedman L, Debordes-Jackson G, Ziedonis D, Pbert L. Patientʼs views on depression care in obstetric settings: how do they compare to the views of perinatal health care professionals?. Gen Hosp Psychiatry. 2013; 35(6): 598-604. doi: 10.1016/j.genhosppsych.2013.07.011
- Cooper LA, Gonzales JJ, Gallo JJ, Rost KM, Meredith LS, Rubenstein LV, et al. The acceptability of treatment for depression among African-American, Hispanic, and white primary care patients. Med Care. 2003; 41(4): 479-489. doi: 10.1097/01.MLR.0000053228.58042.E4
- Davila M, McFall SL, Cheng D. Acculturation and depressive symptoms among pregnant and postpartum Latinas. Matern Child Health J. 2009; 13(3): 318-325. doi: 10.1007/s10995-008-0385-6
- Dennis CL, Dowswell T. Psychosocial and psychological interventions for preventing postpartum depression. Cochrane Database Syst Rev. 2013; (2):CD001134. doi: 10.1002/14651858.CD001134.pub3
- Dwight-Johnson M, Sherbourne CD, Liao D, Wells KB. Treatment preferences among depressed primary care patients. J Gen Intern Med. 2000; 15(8): 527-534.
- Ennis SR, Rios-Vargas M, Albert NG. The Hispanic Population: 2010. 2011; Census Briefs: U.S. Census Bureau.
- Evans J, Melotti R, Heron J, Ramchandani P, Wiles N, Murray L, et al. The timing of maternal depressive symptoms and child cognitive development: a longitudinal study. J Child Psychol Psychiatry. 2012; 53(6): 632-640. doi: 10.1111/j.1469-7610.2011.02513.x
- Field T. Postpartum Depression Effects on Early Interactions, Parenting, and Safety Practices: A Review. Infant Behav Dev. 2010; 33(1): 1-6. doi: 10.1016/j.infbeh.2009.10.005
- Fournier JC, DeRubeis RJ, Hollon SD, Dimidjian S, Amsterdam JD, Shelton RC, et al. Antidepressant drug effects and depression severity: a patientlevel meta-analysis. JAMA. 2010; 303(1): 47-53. doi: 10.1001/ jama.2009.1943
- Gavin NI, Gaynes BN, Lohr KN, Meltzer-Brody S, Gartlehner G, Swinson T. Perinatal depression: a systematic review of prevalence and incidence. Obstet Gynecol. 2005; 106(5 Pt 1): 1071-1083. doi: 10.1097/01. AOG.0000183597.31630.db
- Goodman JH. Womenʼs attitudes, preferences, and perceived barriers to treatment for perinatal depression. Birth. 2009; 36(1): 60-69. doi: 10.1111/j.1523-536X.2008.00296.
- Grigoriadis S, Vonder Porten EH, Mamisash vili L, Tomlinson G, Dennis CL., Koren G, et al. The impact of maternal depression during pregnancy on perinatal outcomes: a systematic review and meta-analysis. J Clin Psychiatry. 2013; 74(4): e321-341. doi: 10.4088/JCP.12r07968
- Grote NK, Bridge JA, Gavin AR, Melville JL, Iyengar S, Katon WJ. A metaanalysis of depression during pregnancy and the risk of preterm birth, low birth weight, and intrauterine growth restriction. Arch Gen Psychiatry. 2010; 67(10): 1012-1024. doi: 10.1001/archgenpsychiatry.2010.111
- Heilemann M, Frutos L, Lee K, Kury FS. Protective strength factors, resources, and risks in relation to depressive symptoms among childbearing women of Mexican descent. Health Care Women Int. 2004; 25(1): 88-106. doi: 10.1080/07399330490253265
- Horowitz JA, Cousins A. Postpartum depression treatment rates for at-risk women. Nurs Res. 2006; 55(2 Suppl): S23-27.
- Howard LM, Molyneaux E, Dennis CL, Rochat T, Stein A, Milgrom J. Nonpsychotic mental disorders in the perinatal period. Lancet. 2014; 384(9956): 1775-1788. doi: 10.1016/S0140-6736(14)61276-
- Kersten-Alvarez LE, Hosman CMH, Riksen-Walraven JM, van Doesum KTM, Smeekens S, Hoefnagels C. Early School Outcomes for Children of Postpartum Depressed Mothers: Comparison with a Community Sample. Child Psychiatry Hum Dev. 2012; 43(2): 201-218. doi: 10.1007/s10578- 011-0257-y
- Koutra K, Chatzi L, Bagkeris M, Vassilaki M, Bitsios P, Kogevinas M. Antenatal and postnatal maternal mental health as determinants of infant neurodevelopment at 18 months of age in a mother-child cohort (Rhea Study) in Crete, Greece. Soc Psychiatry Psychiatr Epidemiol. 2013; 48(8): 1335-1345. doi: 10.1007/s00127-012-0636-0
- Kroenke K, Spitzer RL, Williams JB, Lowe B. The Patient Health Questionnaire Somatic, Anxiety, and Depressive Symptom Scales: a systematic review. Gen Hosp Psychiatry. 2010; 32(4): 345-359. doi: 10.1016/j. genhosppsych.2010.03.006
- Lara MA, Navarrete L, Nieto L, Martin JP, Navarro JL, Lara-Tapia H. Prevalence and incidence of perinatal depression and depressive symptoms among Mexican women. J Affect Disord. 2015; 175: 18-24. doi:10.1016/j.jad.2014.12.035
- Lara-Cinisomo S, Wisner K.L, Burns RM, Chaves-Gnecco D. Perinatal depression treatment preferences among Latina mothers. Qual Health Res. 2014; 24(2): 232-241. doi: 10.1177/1049732313519866
- Leis JA, Heron J, Stuart EA, Mendelson T. Associations between maternal mental health and child emotional and behavioral problems: does prenatal mental health matter?. J Abnorm Child Psychol. 2014; 42(1): 161- 171. doi: 10.1007/s10802-013-9766-4
- Lin P, Campbell DG, Chaney EF, Liu CF, Heagerty P, Felker BL, et al. The influence of patient preference on depression treatment in primary care. Ann Behav Med. 2005; 30(2): 164-173. doi: 10.1207/s15324796abm3002_9
- Nadeem E, Lange JM, Miranda J. Mental health care preferences among low-income and minority women. Arch Womens Ment Health. 2008; 11(2): 93-102. doi: 10.1007/s00737-008-0002-0
- Reck C, Struben K, Backenstrass M, Stefenelli U, Reinig K, Fuchs T, et al. Prevalence, onset and comorbidity of postpartum anxiety and depressive disorders. Acta Psychiatr Scand. 2008; 118(6): 459-468. doi: 10.1111/j.1600-0447.2008.01264.x
- Sleath B, West S, Tudor G, Perreira K, King V, Morrissey J. Ethnicity and depression treatment preferences of pregnant women. J Psychosom Obstet Gynaecol. 2005; 26(2): 135-140. doi: 10.1080/01443610400023130A
- Stein A, Pearson RM, Goodman SH, Rapa E, Rahman A, McCallum M, et al. Effects of perinatal mental disorders on the fetus and child. Lancet. 2014; 384(9956): 1800-1819. doi: 10.1016/S0140-6736(14)61277-0
- Sutter-Dallay AL, Murray L, Dequae-Merchadou L, Glatigny-Dallay E, Bourgeois ML, Verdoux H. A prospective longitudinal study of the impact of early postnatal vs. chronic maternal depressive symptoms on child development. Eur Psychiatry. 2011; 26(8): 484-489. doi: 10.1016/j.eurpsy.2010.05.004
- Tronick E, Reck C. Infants of depressed mothers. Harv Rev Psychiatry. 2009; 17(2): 147-156. doi: 10.1080/10673220902899714
- van Schaik DJ, Klijn AF, van Hout HP, van Marwijk HW, Beekman AT, de Haan M, et al. Patientsʼ preferences in the treatment of depressive disorder in primary care. Gen Hosp Psychiatry. 2004; 26(3): 184-189. doi: 10.1016/j. genhosppsych.2003.12.001
- Velders FP, Dieleman G, Henrichs J, Jaddoe VW, Hofman A, Verhulst FC, et al. Prenatal and postnatal psychological symptoms of parents and family functioning: the impact on child emotional and behavioural problems. Eur Child Adolesc Psychiatry. 2011; 20(7): 341-350. doi: 10.1007/s00787-011- 0178-0
- Vesga-Lopez O, Blanco C, Keyes K, Olfson M, Grant BF, Hasin DS. Psychiatric disorders in pregnant and postpartum women in the United States. Arch Gen Psychiatry. 2008; 65(7): 805-815. doi: 10.1001/ archpsyc.65.7.805
- Whitton A, Warner R, & Appleby L. The pathway to care in post-natal depression: womenʼs attitudes to post-natal depression and its treatment. Br J Gen Pract. 1996; 46(408): 427-428.


