Case Report
Perianal Well Differentiated Liposarcoma
Hospital Universitario Virgen Macarena de Sevilla, Unidad de Coloproctología, Facultad de Medicina, Universidad de Sevilla
*Corresponding author: Luis C Capitán Morales, Hospital Universitario Virgen Macarena de Sevilla, Unidad de Coloproctología, Facultad de Medicina, Universidad de Sevilla, Spain, E-mail: lcapitan@us.es
Received: October 30, 2017 Accepted: December 2, 2017 Published: January 1, 2018
Citation: Jurado F, Cintas J, Ramirez A, et al. Perianal Well Differentiated Liposarcoma. Madridge J Surg. 2018; 1(1): 6-8. doi: 10.18689/mjs-1000102
Copyright: © 2018 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Perineal liposarcoma is a very rare entity, with slow growth and more prevalent in middle aged males. The perineal localization is extremly weird on our environment. We describe the management of a man who consults with the complaint of an asymtomatic gluteal lump. RMN suggest a big mass compatible with Liposarcoma of 17x7x6cm. A needle core biopsy was performed and the tissue was histologically consistent with fibrofatty tissue with vascular ectasia that requires surgical treatment with exeresis in wich "edges of surgical section" can not be obtained. Histology confirms the diagnosis of well differentiated Liposarcoma that not requires adjuvant therapy. Patient stays without recurrence.
Keywords: Perianal; Well differentiated; Liposarcoma; Perianal region.
Purpose
Presentation of a very rare case of well differentiated liposarcoma located in the perianal region.
Method
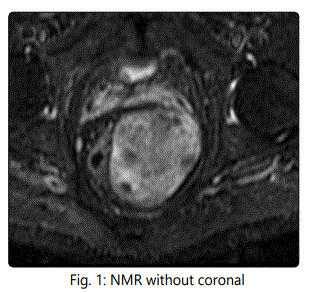
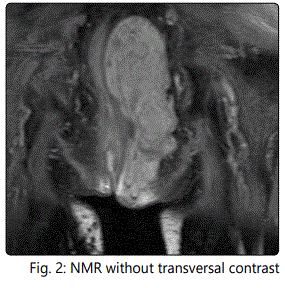
56-year-old man seen in consultation because of an injury on the left gluteus that causes discomfort. Magnetic resonance imaging of non-contrasting pelvis is performed for the diagnosis, which describes a large tumor with dimensions of 16 x 7 x 6 cm with well defined contours, lobed, located at the level of the ischiorectal fossa, displacing the elevator ani muscle and extending caudally towards the subcutaneous cellular tissue of the left gluteal region, without involvement of prostate, seminal vesicles and bladder. PAAF is guided by ultrasound and the pathological study shows fibroadipose tissue with vascular ectasia.
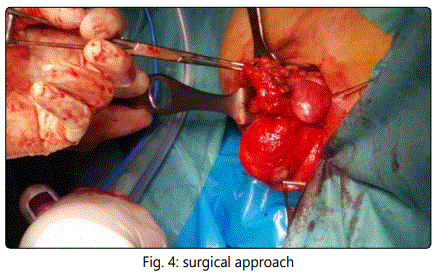
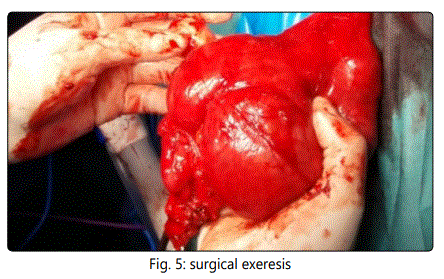
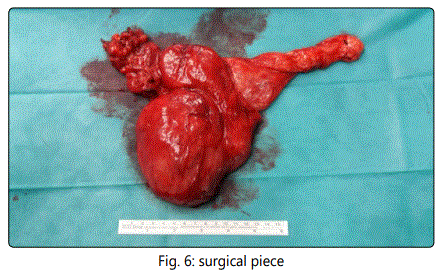
Surgical treatment was proposed in June of 2016, with complete excision of the lesion. The anatomopathological result of the piece shows contact with the resection edges of an atypical sclerosing lipomatous tumor. The molecular study (HIS) shows amplification of the MDM2 gene, confirming the diagnosis.

Discussion
Liposarcoma is a very rare tumor, derived from primitive cells capable of differentiating into adipose tissue presenting on 50 different types at the histological level. It is a neoplasm typical of adult patients, whose peak incidence is between 40 and 60 years. It shows a slight prevalence for the male sex and the most frequent location is in the extremities. They are usually asymptomatic and have slow growth. Majority of the patients go to consult referring to the appearance of a mass.
They are currently classified into three biological types: amplification of the 12q13-15 gene (well differentiated liposarcoma / dedifferentiated liposarcoma), translocation of FUS-DDIT3 (myxoid liposarcoma / round cell liposarcoma) and pleomorphic liposarcoma with complex genome changes [1]. The well differentiated liposarcoma and the myxoid are of low degree of malignancy. The term atypical lipomatous tumor is used by some pathologists to define the histologically pure types of well differentiated liposarcomas that do not metastasize and with the possibility of performing a curative resection with free margins, usually located in the lower limbs and trunk. 90% of well-differentiated and dedifferentiated liposarcomas have the expression of MDC2, HMGA2 and CDK4 oncogenes on chromosome 12q13-15 that may be related to the genesis of liposarcomas [2]. There is a malignant potential of well differentiated tumors, estimated in 20% of the first recurrences and 44% of the second recurrences in the retroperitoneal localization [3]. Malignancy traits are larger than 5 cm in size that affect deep planes and fixation to adjacent tissues. Imaging techniques are of choice for the diagnosis of liposarcomas, with some types of radiological characteristics that facilitate diagnosis. It is preferable to perform magnetic resonance imaging at pelvic and lower limb locations. Computed axial tomography may be useful to complete the study in abdominal localization liposarcomas. The biopsy is not used in a systematic way. In retroperitoneal localization liposarcoma, surgical resection is preferred without prior biopsy because of the poor benefit of neoadjuvant treatment with radiotherapy and chemotherapy. In cases of not being resectable, a biopsy can be performed to determine the histological subtype [4].
The treatment of choice is surgical resection with the aim of completely removing the tumor and preventing relapses, performing a broad or radical resection. The resection margin should be 1 cm if possible [5]. In the case of infiltrated neurovascular structures, it must be exhaustively dissected including the surrounding tissue. Studies have shown an increase in the rate of local and distal recurrences when the resection of an organ attached to the tumor is added in the surgical treatment [6].
The local recurrence rate at five years is estimated between 22% -41% according to published series [7, 8].
Local recurrence depends to a large extent on the state of the margins in the surgical specimen, the margins affected by the tumor are associated with a high rate of relapse. Patients with distant metastases have a worse prognosis with a 50% survival rate at 18 months [9].
There are currently no data demonstrating the benefit of neoadjuvant / adjuvant chemotherapy in liposarcomas.
Well-differentiated and undifferentiated liposarcomas often have resistance to chemotherapy, with CDK4 inhibitors being the most effective [1].
In the lower limb localization, adjuvant therapy can be performed with radiotherapy in dedifferentiated liposarcomas. Well differentiated liposarcomas have a 1% risk of metastasis and are not radiosensitive [10].
In the case of incomplete resections with positive margins, sizes greater than 5 cm, adjuvant radiotherapy can be performed in dedifferentiated liposarcomas.
In patients with local recurrence, it is necessary to observe the evolution of the tumor. If there is a possibility of resecting with free margins, surgical treatment should be performed. In the case of not being resectable or being symptomatic with progressive growth, experimental treatments may be considered. The growth of 0.9cm per month has been related to worse long-term results after surgery, with no difference in patients with this same growth rate who did not undergo surgical treatment, thus, in relapses local with a growth rate of 1 cm per month is not indicated the surgical resection of the recurrence [11]. In the case that after treatment with chemotherapy / radiotherapy the tumor can be resected surgical treatment may be an option.
Studies aimed at the knowledge of therapeutic targets for the treatment of liposarcoma are currently under development. The major advances are directed to the chemotherapeutics that act by inhibiting the CDK4 and on competitive inhibitors of the complex MDM2-p53 (nutlina).
Treatments are being tested in the case of patients with metastases with Eribulin synergistically improving the effectiveness of other antitumor agents [12].
Likewise, monoclonal treatment such as regorafenib is being used in randomized, double-blind studies for the treatment of some types of liposarcomas, with promising results [13].
In our case the patient presents the tumor in perianal location. After the radiological study and biopsy, surgical treatment by means of a complete resection of Ligasure Impact tumor was chosen, observing a large tumor to the upper edge of the prostate. The preoperative anatomopathological results of fibroadiposal tissue with vascular ectasia differ from those analyzed by the surgical specimen resulting in atypical sclerosing lipomatous lesion with MDM2 expression in histology. This low-grade tumor is currently classified as a well-differentiated liposarcoma with poor metastasis and relapse after RO excision. The surgical treatment carried out does not manage to obtain free margins. After the patient's agreement with the treatment, he stated that he did not want to undergo surgical techniques, so no other resection was performed to expand the margins. Long-term observation of the patient is decided. After 12 months of follow-up he has not shown recurrence of the disease at present.
Conclusion
The term "liposarcoma" refers to a set of neoplasms whose behavior depends on the histological subtype. Welldifferentiated liposarcomas have a 1% risk of metastasis and are not radiosensitive. Studies aimed at the knowledge of therapeutic targets for the treatment of liposarcoma are currently under development. The major advances are directed to the chemotherapeutics that act by inhibiting the CDK4 and on competitive inhibitors of the complex MDM2-p53.
References
- Crago AM, Dickson MA. Liposarcoma, multimodality management and future targeted therapies. Surg Oncol Clin N Am. 2016; 25(4): 761-773. doi: 10.1016/j.soc.2016.05.007
- Dalal KM, Kattan MW, Antonescu CR, et al. Subtype specific prognostic nomogram for patients with primary liposarcoma of the retroperitoneum, extremity, or trunk. Ann Surg. 2006; 244(3): 381-391. doi: 10.1097/01. sla.0000234795.98607.00
- Murphey MD, Arcara LK, Fanburg-Smith J. From the archives of the AFIP: imaging of musculoskeletal liposarcoma with radiologic-pathologic correlation. Radiographics. 2005; 25(5): 1371-1395. doi: 10.1148/rg.255055106
- Singer S, Antonescu CR, Riedel E, Brennan MF. Histologic subtype and margin of resection predict pattern of recurrence and survival for retroperitoneal liposarcoma. Ann Surg. 2003; 238(3): 358-370. doi: 10.1097/01.sla.0000086542.11899.38
- Bonvalot S, Miceli R, Berselli M, et al. Aggressive surgery in retroperitoneal soft tissue sarcoma carried out at high-volume centers is safe and is associated with improved local control. Ann Surg Oncol. 2010; 17(6): 1507-1514. doi: 10.1245/s10434-010-1057-5
- Italiano A, Mathoulin-Pelissier S, Cesne AL, et al. Trends in survival for patients with metastatic soft-tissue sarcoma. Cancer. 2011; 117(5): 1049- 1054. doi: 10.1002/cncr.25538
- Pawlik TM, Pisters PW, Mikula L, et al. Long-term results of two prospective trials of preoperative external beam radiotherapy for localized intermediate- or high-grade retroperitoneal soft tissue sarcoma. Ann Surg Oncol. 2006; 13(4): 508-517. doi: 10.1245/ASO.2006.05.035
- Thomas C, Movva S. Eribulin in the management of inoperable soft-tissue sarcoma: patient selection and survival. Onco Targets Ther. 2016; 9: 5619- 5627. doi: 10.2147/OTT.S93517
- Olivier M, Thomas B, Antoine I, et al. Safety and efficacy of regorafenib in patients with advanced soft tissue sarcoma (REGOSARC): a randomised, double-blind, placebo-controlled, phase 2 trial. Lancet Oncol. 2016; 17(12): 1732-1742. doi: 10.1016/S1470-2045(16)30507-1


