Research Article
Food Choking Hazards in Toddlers: An Interventional Study
Department of Pediatrics, University of Nebraska Medical Center and Childrenʼs Hospital & Medical Center in Omaha, Nebraska, USA
*Corresponding author: Aisha Baig, Department of Pediatrics, University of Nebraska Medical Center and Childrenʼs Hospital & Medical Center in Omaha, Nebraska, USA, E-mail: baiga@upstate.edu
Received: February 2, 2019 Accepted: March 25, 2019 Published: April 2, 2019
Citation: Baig A, Thomas HM, Britigan DH, Colombo JL. Food Choking Hazards in Toddlers: An Interventional Study. Int J Pediatr Neonatal Prim Care. 2019; 1(1): 11-16. doi: 10.18689/ijpn-1000104
Copyright: © 2019 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Background: Choking on food and subsequent foreign body aspiration is a common event in young children. This study suggests that parental knowledge of choking hazards in children is lacking. The purpose of this study was to assess changes in knowledge level and measure retention after an educational intervention on choking and risky food items.
Methods: We prospectively enrolled 103 parents with children ages 1-4 years due to the high risk for choking in that age group. A questionnaire was designed to assess knowledge of food choking hazards in children. We asked when it was safe to give all high risk choking foods, recognition of foods that were safe to give for less than 2 years of age, 2-4 years of age, best setting for their child to eat, whether they should be supervised and the course of action in the event of choking episode. Parental knowledge was assessed at baseline. Following the completion of the form, an educational module with active teaching was presented to the parents during their clinic visit. Following the education, same questionnaire was presented immediately (post–intervention P-1) and after a period of 3 months (long-term post-intervention P-2).
Results: There were 77 pairs that were assessed at baseline and P1, and 49 pairs assessed at baseline, P-1 and P-2. Most parents did not recall receiving any food avoidance anticipatory guidance from their childʼs medical doctor. Baseline knowledge of avoidance of some of the risky food items was present for <2 years age group such as popcorn, nuts and hard candies. However, most parents thought it was acceptable to give other risky food items. Baseline knowledge for age group 2-4 years was poor with most parents allowing access to all the risky food items in this age range. Significant improvement post-educational intervention (P1 and P2) was seen for the appropriate food choking items for age range less than 2 years and for 2-4 years. An analysis between P-1 and P-2 showed good retention of knowledge of most food items. Most parents watched their children during feeding, seated them in an age appropriate chair, and better informed in choosing the appropriate food items for their children.
Conclusions: Parental understanding of food choking hazards for infants and toddlers is insufficient. There is inadequate anticipatory guidance at the primary care provider level. Appropriate education helps provide long term retention of food choking hazards.
Keywords: Choking; Food Advice; Cough; Anticipatory Guidance; Foreign Body.
Abbreviations: P-1: Immediate post-intervention knowledge questionnaire following the educational presentation; Post 2 (P-2): Long-term post-intervention knowledge questionnaire.
Introduction
Food related choking in young children is a major ongoing problem [1]. Food is one of the most common reasons for choking. The number one choking hazard as per the AAP guidelines is hot dog followed by hard candy, peanuts/nuts, seeds, whole grapes, raw carrots, apples, popcorn, chunks of peanut butter, marshmallows, chewing gum and sausages N2.
There are several epidemiological and retrospective studies done to shed light on the seriousness of this issue. The majority of food choking occurrences are in age range of 1-4 [2-4]. A database extraction from the National Electronic Injury Surveillance System-All Injury Program found that an average of 12,435 children present to emergency rooms annually for food related choking events.
Incidents of choking still occur despite updated recommendations in February 2010 by the American Academy of Pediatrics (AAP) which included better labeling of risky food items, modification of food to non-choking form, better surveillance mechanisms for reporting such events, and emphasis to primary care providers to provide choking related anticipatory guidance. AAP also recommends better collaboration of efforts with United States Department of Agriculture and Food and Drug Administration on increasing awareness, product recalls, better inspection of foods considered to be choking hazards, appealing to manufacturers for warning labels, and engineering in a safer format [5].
Despite all this, cross sectional study from Nichols et al. [4] found that parents of children less than 4 years of age did not receive instructions from their childrenʼs providers on avoiding fruit chunks, raw vegetables and chunks of peanut butter. However, most were aware of choking hazards from nuts, candy and gum avoiding giving them to their children. The researchers found that parental knowledge on choking food items is incomplete and this contributes to food related aspiration in children less than 4 year of age [4]. Another large retrospective study by Sidell et al. concluded that food was the major cause of aspiration, especially nuts and seeds. They found the most common age was children less than 5 years of age [6].
There are several complications from a foreign body aspiration. Airway foreign bodies are easily missed on chest imaging and fluoroscopy. Interestingly, food related aspiration presentation is often misdiagnosed as asthma. It requires a high index of suspicion in the setting of appropriate age, history and physical findings to allow timely evaluation to prevent the associated complications. Some of the complications associated with foreign body aspiration in the trachea bronchial tree are respiratory distress, obstructive emphysema, bronchopneumonia, bronchi ectasis and recurrent pneumonia [7-10].
We did not find any studies that evaluated parental knowledge of food related choking and effect of an educational intervention. By doing so, we hope that improved parental knowledge might be a solution to this issue.
The aim of this study is to assess parental knowledge of different foods and investigate the effect of an interventional education on knowledge retention.
Materials and Methods
Subjects
A sample pilot survey using open-ended questions was conducted in a pulmonary clinic with parents of children aged 1-4 years. The 10-item survey included the following topics: the age solid food was started; food items to be avoided in children less than 2 years; food items to be avoided in children 2-4 years of age; and the age of the child when parents thought all foods were safe to be given. The results revealed variable responses with some parents correctly identifying risky food items due to their link to choking. However, there were other responses only highlighting allergy concerns.
Based on this pilot, we enrolled 103 parents and caregivers of children aged 1-4 years seen in our clinics. The sample was chosen mainly due to convenience based on the recommendation of our statistician. The pilot study helped in framing the questionnaire and addressing areas of deficiency in knowledge of safe vs risky foods.
Study design and methods
The study was approved by University of Nebraska Medical Centerʼs (UNMC) Institutional Review Board (IRB) under the behavioral category: IRB # 652-14-EX.
This study was conducted from November, 2014 to January, 2016 in the ENT, Pulmonary and Pediatrics Clinics at a free standing Childrenʼs Hospital and Medical Center and at the Pediatric Clinic at Nebraska Medicine. The inclusion criterion was parent, grandparent and caregiver of a child age within the age range of 1-4 years. Those with history of choking, dysphasia, oral aversion, severe gastro esophageal reflux, gastric tube feedings (present or past) or aspiration were excluded. The eligible parents/caregivers were older than 19 years of age per the IRB age inclusion criteria. A five dollar gift card was given if the study was completed by the parent/caregiver.
Patients within the recommended age group were selected from the general Pediatric, Pulmonary, and ENT clinics during their routine scheduled follow-up visits. The primary investigator approached the families for their permission to participate after providing them with brief synopsis and procedural information about the research. Some of the parents who were not approached were those with sick visits, language barriers, and difficult follow-ups. Written informed consent was obtained from parents of children who agreed to participate in the study.
The survey questionnaires were developed with the help of a biostatistician from the College of Public Health, Department of Biostatics at UNMC.
The baseline questionnaire contained twelve questions with ten multiple choice questions and two open-ended questions. There were two post-intervention questionnaires with similar questions administered immediately following the presentation (P-1) and after several months (P-2) [11]. The questionnaires were adjusted for 6th grade reading level as determined by electronic health literacy software [12].
The questionnaire asked any specific food avoidance instructions provided by doctor or nurse and foods parents thought were appropriate to give for age <2 years and 2-4 years of age, meal seating environment [13], appropriate course of action during food related choking event [14] and if parents behavior has changed in choosing the safe food choices for their children post-presentation. Attached is the sample of pre and post knowledge questionnaires. (Supplementary section: Appendix A)
Educational intervention was in-person narration using PowerPoint presentation on an iPad. The time of presentation averaged 7-10 minutes. Each new concept was introduced with images. For example, the size of an airway of a child was depicted with an image of a drinking straw in a cup. Colorful graphic drawings were used to relate upper airway anatomy. Bronchoscopy pictures and chest radiographic images were also included to show how an aspirated item would appear in the trachea bronchial tree. Photographic images of avoidable food choices were added to the slides (including size, shape and texture. Safe feeding practices and the necessary steps in the event of a choking incident were also discussed. The source of information was from AAP, American Academy of Family Physicians and the feedback received in the pilot study. Attached is a copy of the power point presentation. (Supplementary section: Appendix B).
The post-questionnaires P-1 and P-2 were identical. The time interval between the two questionnaires on average was a period of 2-4 months. This time period was chosen to find out if they can remember the knowledge on a long term basis [15].
Each caregiver was used as his/her own comparison. Every effort was made to ensure it was the same person who filled out the baseline, P-1 and P-2. The follow-up information on P-2 was collected in several ways. The questionnaire was answered over the phone, via email, or in person during a follow-up clinic visit.
Statistical analysis
The changes are measured in terms of mean score and the subjects are paired (in this case, same person for pre- and postintervention), so the sample size assumes a paired t-test analysis. A minimum power of 80% was considered due to a possible 30% loss to follow up. A continuous response variable from matched pairs of study subjects was planned. Prior pilot data indicated that the difference in the response of matched pairs is normally distributed with standard deviation 5. If the true difference in the mean response of matched pairs is 2 points, then a sample size of 51 pairs of subjects is required to be able to reject the null hypothesis. The Type I error probability associated with this test of this null hypothesis is 0.05.
Only subjects who completed the baseline, P-1and P-2 were included in the final analysis. Given the paired data, McNemarʼs test was used to assess the knowledge changes between baseline and P-1 and P-1 and P-2. A p-value<0.05 was considered statistically significant. All analyses were conducted using the software SAS version 9.3 (SAS Institute; Cary, NC).
Results
Demographics
Among the 103 parents/care givers who were enrolled in the study, there were 77 pairs evaluated at baseline and P-1 to assess knowledge improvement and 49 pairs at baseline, P-1 and P-2 to assess for knowledge retention.
Limited demographics are available for people who completed the study to P-2. Most of them resided between two midtown clinics, a Nebraska Medicine Pediatric Clinic and a free-standing clinic at Childrenʼs Hospital and Medical Center: urban setting. Of the 49 (47%) of the caregivers (majority were parents) who completed the study, nearly half of them (59%) were covered by Medicaid and the remaining 41% had either private insurance or unknown status. There was no gender difference between the patients. All patients were 1-4 years of age group.
MD anticipatory guidance
Of the total 77 parents who answered this question, 67 parents (87%) were not able to recall any guidance related to food avoidance provided by the medical team. Out of the 10 parents (12%) who answered this question affirmatively, 6 (7%) recalled being told to avoid high risk food items due to choking and 4 (5%) recalled it as to avoid due to allergy concerns.
Knowledge improvement between baseline and P-1 between two groups: <2years of age and 2-4 years of age
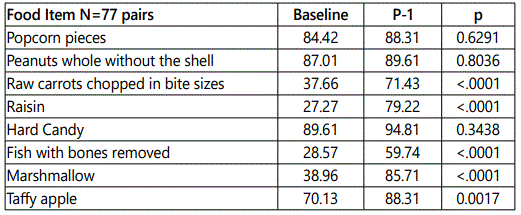
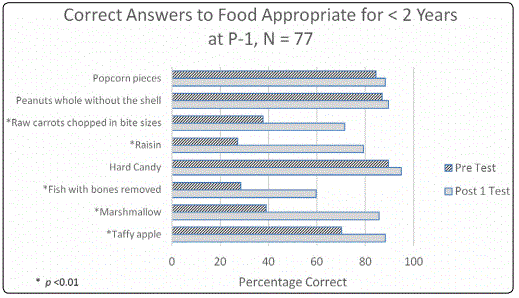
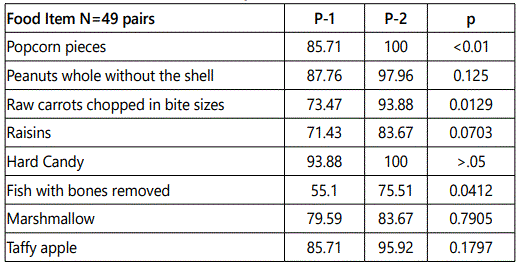
Group<2 years of age: Most parents knew to avoid popcorn, peanuts, hard candy and taffy apple (Table 1, figure 1). Significant improvement was reached immediately post-presentation, P-1 for raw carrots, raisins, fish, marshmallow and taffy apple (p<0.001).
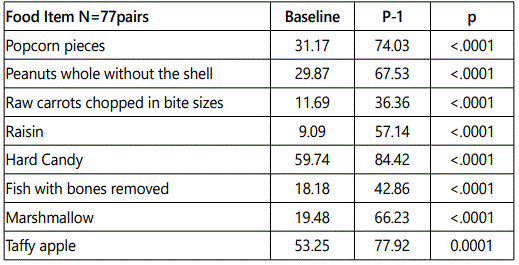
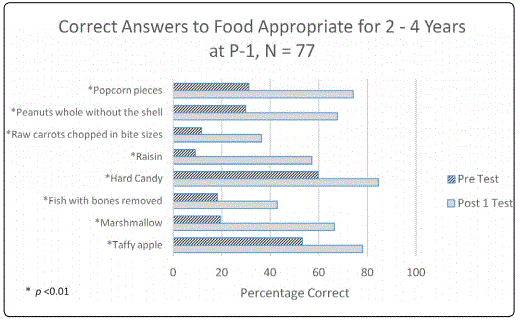
Group 2-4 years of age: At baseline most parents thought the avoidable food items for <2 years of age were allowable at 2-4 years of age (Table 2, figure 2). Significant improvement was obtained in recognition of all the risky food items immediately post-education P-2 (p<0.001).
Knowledge retention between P-1 and P-2 between two groups: <2 years of age and 2-4 years of age
For age< 2years: Parents remembered to avoid all the risky food items several months later when they filled out the P-2 questionnaire and some had improvement in knowledge from P-1 to P-2 (Table 3, figure 3). However, significance was reached for remembering to avoid popcorn and raw carrots both at (p<0.01). Near significance was reached for recalling to avoid raisins (p<0.07), fish (p<0.04) and hard candy (p<0.05).
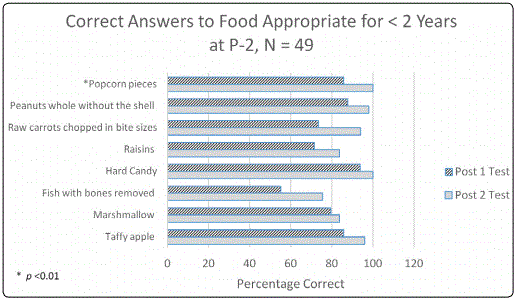
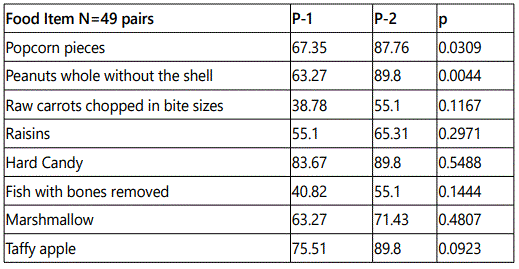
For age range 2-4 years: Parents remembered to avoid all risky food items for this age group as shown by the increased P-2 percentage, but significance was reached for popcorn and peanuts (p<0.01) (Table 4, figure 4).

Setting during eating
Statistically significant improvement in knowledge was appreciated during meal seating and observation during feeding.
Action in the event of choking episode
Improvement in baseline knowledge of allowing their child to cough and call 911 as needed was observed in 64/77 (83%, p<0.001) at P-1. This knowledge was significantly retained in 48/49 parents (97%, p=0.0078).
Change in behavior
Most parents 45/49 (91%) agree that their behavior changed in selecting the right food choice after an educational intervention.
Discussion
Foreign body aspiration is a major public health issue in the U.S. and worldwide. The most commonly aspirated foreign bodies are food items. There are studies assessing parental knowledge of choking food items [4] but none describing improvement in parental knowledge and retention of such knowledge after food avoidance related educational intervention.
According to our survey, most parents did not recall receiving any food avoidance anticipatory guidance from their childʼs medical provider. Very few recalled receiving food avoidance specific to choking and some thought the reason related to food allergy. Our study revealed many areas of deficiency in choice of risky food items for children <2 years and 2-4 years of age. However, appropriate education resulted in improvement and retention of knowledge especially for the most risky age group (2-4 years of age).
From the limited demographics observed, insurance status and caretakerʼs socio economic status did not appear to play a role in identification and avoidance of food related aspiration.
Most parents were aware of avoiding the common food choking hazards such as nuts/popcorn/candies for <2 years age group. Most parents were unaware of other choking hazards such as raisins, fish, marshmallow and taffy apple. Most parents thought it was acceptable to provide the risky food items at 2-4 years of age but this improved significantly to avoidance post education.
Long-term knowledge of the risky food items was retained and increased significantly for both age groups especially the 2-4 years of age. Based on the previous studies [4], this is the riskiest age group. Some of the likely reasons include increased awareness through social media, discussion with other families having similar age range children and parents self-research and education.
Health care providers should provide education on avoidance of risky food items for <2 year olds and especially 2-4 year old age group based on our findings. Appropriate audiovisual presentation with discussion helps in long term retention of the necessary knowledge [15]. Anticipatory guidance repetition is important.
Food related aspiration has a significant morbidity, mortality and cost burden to the families and society. Very few parents are aware of such consequences.
Based on a large retrospective literature review from KID US inpatient database from various Childrenʼs Hospitals across 36 states, Shah et al. concluded that mean age of foreign body (esophageal/airway)was at 2.5 years and 42% were food related. Of the 52% who underwent bronchoscopy for suspected airway aspiration, positive finding was in 37%. The mortality rate was at 3.7% related to food aspiration with average length of stay being 6 days and a mean total charge per patient being $30,270 [16].
Similarly, Kim et al. looked at large retrospective literature review of the U.S. inpatient sample from 2009-2011 of foreign bodies aspirated. They found that males were more than half and the mean age of the study group was at 3.6 years. The ratio of nonfood to food was 5:3. Similar to Shah, they found that 56% underwent bronchoscopy for removal and 41% had a foreign body. There was 4% mortality and morbidity rate, 1.8% mortality, 3 days of median length, median charge of $20,820 per case (average from $3,628 to $16,723), with a national estimate of $41 million in inpatient healthcare expenses annually [17].
Most studies cite the lack of awareness in parents due to lack of physician awareness and education on food related choking hazards. Our study tries to educate parents and caregivers via language appropriate presentation on the identification, signs/symptoms, appropriate seating and action in the event of choking. Our study was also able to show that with time, parents were able to recall such information and hopefully they will act accordingly with their judgment.
Our study had some limitations. Our sample size was limited due to various logistics such as difficulty with recruiting patients, prolonged time during physician visits for the participants, parents not utilizing appropriate time to fill out forms. It was also difficult to reach some parents for the P-2 questionnaire due to changed addresses, phone numbers, and their decision to not participate. This resulted in a significant drop out rate. The personalized narration was not scripted and it would have been better to prerecord for consistent delivery.
Conclusions
This study adds to a body of research involving food related choking items. It highlights the deficiency in our current anticipatory guidance in food choking risk in infants and especially toddlers. It supports having specific educational intervention at childhood health care visits during these years. This should not only include risky foods, but also actions to be taken in the event of a choking episode and the seating arrangements during feeding.
Funding
This study was supported by the Pediatrics Research Committee, UNMC, Omaha, NE.
Acknowledgements
Statistical assistance provided by Harlan Sayles at the UNMC College of Public Health Center for Collaboration on Research Design and Analysis (CCORDA). Special thanks to Dr. Monirul Islam, Deviany Poppy, Trisari Anggondowati and Timothy Hallberg, Research Technologist, UNMC and Dr. David Finken, Pediatrician.
References
- Smith SA, Norris B. Reducing the risk of choking hazards: mouthing behavior of children aged 1 month to 5 years. Inj Control Saf Promot. 2003; 10(3): 145-154. doi: 10.1076/icsp.10.3.145.14562
- American Academy of Pediatrics. Prevention of Choking Among Children. Committee on Injury, Violence, and Poison Prevention. Pediatrics. 2010; 125(3).
- Centers for Disease Control and Prevention. Nonfatal choking-related episodes among children-US, 2001. MMWR Morb/Mortal weekly Rep. 2002; 51(42): 945-948.
- Nichols BG, Visotcky A, Aberger M, et al. Pediatric exposure to choking hazards is associated with parental knowledge of choking hazards. Int J Pediatr Otorhinolaryngol. 2012; 76(2): 169-173. doi: 10.1016/j.ijporl.2011.10.018
- Chapin MM, Rochette LM, Annest JL, Haileyesus T, Conner KA, Smith GA. Non fatal Choking on Food Among Children 14 Years or Younger in the United States, 2001–2009. Pediatrics. 2013; 132(2): 275-281. doi: 10.1542/peds.2013-0260
- Sidell DR, Kim IA, Coker TR, Moreno C, Shapiro NL. Food Choking hazards in Children. Int J Pediatr Otorhinolaryngol. 2013; 77(12): 1940-1946. doi: 10.1016/j.ijporl.2013.09.005
- Tan HK, Brown K, Mc Gill T, Kenna MA, Lund DP, Healy GB. Airway foreign bodies: a 10 year review. Int J Pediatr Otorhinolaryngol. 2000; 56(2): 91-99.
- Blazer S, Naveh Y, Friedman A. Foreign body in the airway: a review of 200 cases. Am J Dis child. 1980; 134(1): 68-71. doi:10.1001/archpedi.1980.02130130050015
- Midulla F, Guidi R, Barbato A, et al. Foreign body aspiration in children. Pediatr Int. 2005; 47(6): 663-668. doi:10.1111/j.1442-200x.2005.02136.x
- Foltran F, Ballali S, Rodriguez H, et al. Inhaled foreign bodies in Children: A Global Perspective on Their Epidemiological, Clinical and Preventive Aspects. Pediatr Pulmonol. 2013; 48(4): 344-351. doi:10.1002/ppul.22701
- Dillman DA, Smyth JD, Christian LM. Internet, Mail and Mixed-Mode Surveys: The Tailored Design Method. 3rd edition. John Wiley & Sons; 2008.
- Health Literacy Innovations. Improving Health Literacy One Word at a Time. 2019.
- Simpson EM, Moll EK, Kassam-Adams N, Miller GJ, Winston FK. Barriers to Booster Seat use and Strategies to increase their use. Pediatrics. 2002; 110(4): 729-736.
- Furman O, Dorfman N, Hasson U, Davachi L, Dudai Y. They saw a movie. Long term memory for an extended audiovisual narrative. Learn Mem. 2007; 14(6): 457-467. doi:10.1101/lm.550407
- Shah RK, Patel A, Lander L, Choi SS. Management of foreign bodies obstructive the airway in children. Arch Otolaryngol Head Neck Surg. 2010; 136(4): 373-379. doi:10.1001/archoto.2010.38
- Kim IA, Shapiro N, Bhattacharyya N. The national cost burden of foreign body aspiration in children. Laryngoscope. 2015; 125(5): 1221-1224. doi:10.1002/lary.25002


