Research Article
A Clinical Diagnosis of Laryngopharyngeal Reflux in Patients with Voice related Problems via Correlation between Reflux Symptoms and Laryngoscopic Findings
Department of Otolaryngology, College of Medicine, Mustansiriyah University, Baghdad, Iraq
*Corresponding author: Mohammed Radef Dawood, Department of Otolaryngology, College of Medicine, Mustansiriyah University, Baghdad, Iraq, Tel. 7902186858, E-mail: mohmadradef@yahoo.com
Received: June 26, 2018 Accepted: August 6, 2018 Published: August 12, 2018
Citation: Dawood MR. A Clinical Diagnosis of Laryngopharyngeal Reflux in Patients with Voice related Problems via Correlation between Reflux Symptoms and Laryngoscopic Findings. Madridge J Otorhinolaryngol. 2018; 3(1): 55-59. doi: 10.18689/mjol-1000111
Copyright: © 2018 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Background
Laryngopharyngeal reflux (LPR) is not uncommon problem facing an otolaryngologist,
and considered one of the discomfited diagnosing condition due to lack of its definitive diagnostic guidelines, so researches concerned for its potential diagnosis for initiation a proper treatment to improve the patient's quality of life.
Objectives
This study was aimed to access the clinical diagnosis of LPR in patients presenting with voice related problems through assessment the agreement in correlation between main reflux symptoms and reflux physical laryngoscopical findings.
Patients and Methods
Seventy-eight consecutive patients with voice-related problems were recruited in this prospective study where they were asked to fill a self-administrated reflex symptom index (RSI) questionnaire, had a clinical consultation, and then subjected to fibre-optic laryngoscopic examination rated their laryngeal reflex finding score (RFS). Clinical diagnosis of LPR was accessed through analysis the correlation between sum and individual variables of RSI and RFS.
Results
The RSI was ranged (13-30), with mean score (18.625), and RFS was ranged [7-19],
with mean score (9.738). Most common symptom and sign was hoarseness (89.74%)
and posterior commissure hypertrophy (87.17%). There was a positive significant correlation between sum of RSI with RFS (P value =0.001), and mean intra-class correlation coefficient (ICC) score for sum of RFS was (0.894), while those of the individual variables were ranged from (0.881-0.920).
Conclusions
The hoarseness and posterior commisure hypertrophy were the most common findings detected, with highest positive significant correlation between them, also positive correlation was observed between sum of RSI with both sum and some individual sign of RFS.
Keywords: Laryngopharyngeal reflux; reflux symptoms index; reflux findings scale; laryngoscopy.
Introduction
The term laryngoesophageal reflux (LPR) or reflux laryngitis was certified in 2002 by the American Academy of Otolaryngology and Head and Neck surgery that described the clinical manifestation of the gastric reflux on the upper airway [1], and it considered as an extra or supra oesophageal variant of gastroesophageal reflux disease (GERD), was first denominated by Koufman and Cummin in 1994 [2]. As not intent to indicate the origin of the reflux but to draw the awareness to the predominance of symptoms and the tissue changes in this laryngopharyngeal segment, this resulted from the effects of the backflow of the gastric contents to those areas [3]. This etiological relationship had been enriched by the creation of technological devices that were capable of measure the acidity in both proximal and distal laryngopharyngeal segment [4,5], and also on the optical fibres laryngoscopic tools that extensively used in clinical practice that had valuable aid the visualization its effect in the larynx [6].
Although LRP (reflux laryngitis) is not infrequently encountered in ENT practice, but it's one of the challenging diagnosing condition because there are no set guidelines for definitive diagnosis, as well as its symptoms lack sufficient specificity to rule out other causative agents that cause laryngitis, and also it had a numerous non-specific physical laryngeal findings which concentrate on Erythema and Edema.
Although the 24-hour dual-probe ambulatory PH monitoring is considered to be the gold standard method for diagnosis of LPR, but some studies reported to be partially invasive, expensive, has a limited use in an outpatient department, and also it not available in several centres [7].
Also some innovative diagnostic techniques: such as triple-probe PH monitoring, pepsin immunoassay detection, and combined PH and impedance measurement have been recently introduced, however none of these methods are currently suitable for routine clinical practice [8].
So to facilitate the diagnosis, a useful, available, and validated self-measurement tool was developed by Belafsky et al [9,10]. "Reflux Symptoms Index" (RSI) for assessment of the subjective degree of LRP symptoms, and a clinical scale "Reflux Finding Scale"(RFS) which assess the severity of the mucosal injury that were found by endoscopic examination of the larynx, and both RSI and RFS scales were appeared to be useful for both initial clinical evaluation and also for followup.
Despite of the fact that these tools (RFI and RFS) are widely applied in the clinical practice, but there are a small number of researches that analysing the correlation between them [11].
So this study was aimed to access the clinical diagnosis of LPR through evaluation the correlation between the main symptoms experienced by the patients according to the RSI measurement tool with the main physical laryngeal finding detected by fibre-optic laryngscopic examination according to RFS, in voice-related complaint patients.
Patients and Methods
After study approval and the informed patient's consent was obtained, a prospective observational study of 78 patients with main complaint of 4 weeks voice-related problems attending ENT clinic from May 1st 2017 to May 1st 2018. The access to clinical diagnosis of LPR was attained by a clinical consultation (medical history and proper ENT examination) after the following exclusion criteria were evaluated; organic laryngeal pathologies, asthma and chronic obstructive pulmonary disease, evidence of voice abusers, previous radiotherapy or head and neck surgery, previous or on treatment with proton pump or H1 inhibitors, antacid, or other drugs that alter the oesophageal motor function or gastric acid secretion, smokers, alcohol abusers, psychiatric or sub mental patients whom confirmed by patient's medical record, as well as those who refused to participated in the study. Then the common symptoms were assessed, as each of participated patient was asked to fill the validated 9-items self-administrated questionnaire that developed by Belafsky et al [9]. Through the application of the Reflux symptoms Index (RSI) score sheet from 0 (no problem) to 5 (most severe) of nine symptoms, encompassing score above [13] (see table 1). Along with clinical laryngeal evidence that detected by fibre-optic laryngoscopic examination blindly from their RSI score sheet, by single examiner (using the standardized protocol) in two separated sessions.
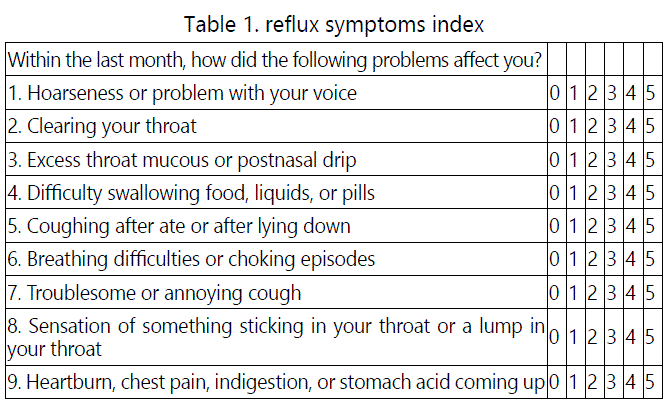
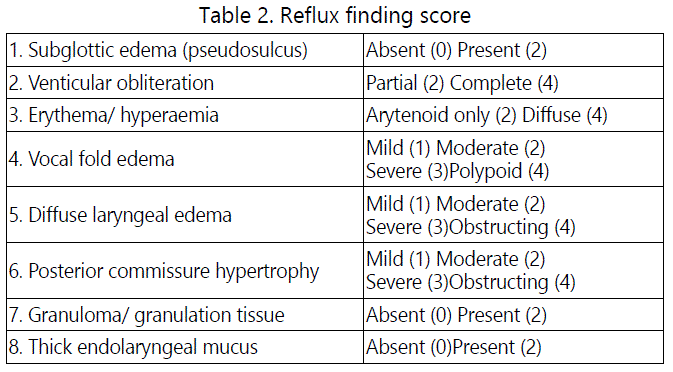
As controls, 78 non LRP patients who agreed to participate in this study were consecutively selected, matched for gender, sex, and other aforementioned criteria presented to our ENT clinic for non-laryngopharyngeal reflux problems. All the controls were completed the Belafsky et al. Questionnaire and subjected to the same above-mentioned fibre-optic laryngoscopic examination.
Statistical analysis
Spearman's rank coefficient was used to assess the correlation between RSI and RFS, as well as the individual correlation between the main symptoms according to RSI and the main laryngeal signs according to RFS. The results with P value <0.05 was considered to be statistically significant. The intra-class correlation coefficient (ICC) was applied for the confirmation the intra-rater reliability, through evaluation the agreement of the physical findings detected by the same examiner between two separated laryngoscopic examination sessions. ICC score ranged from 0.0 to 1.0, if there was very close agreement between the two scores, it would be close to 1.0.
Results
There were 50 females' patients (64.1%) and 28 males patients (35.9%), with the mean age of 41.8 years.
The RSI was ranged from 13-30, with mean score 18.6, and the RFS was ranged from 7-19, with mean score 9.7.
The most common symptom from RSI detected was hoarseness (89.7%), followed by the frequent throat clearing (76.9%), and the distribution of the frequencies of the reflux symptoms among the patients sample was shown in table 3.

The most common physical finding from RFS encountered with fibre-optic laryngoscopic examination was posterior commissure hypertrophy (87.2%), followed by vocal fold edema (79.5%), and the distribution of the patient's laryngoscopic finding among the patients sample was shown in table 4.
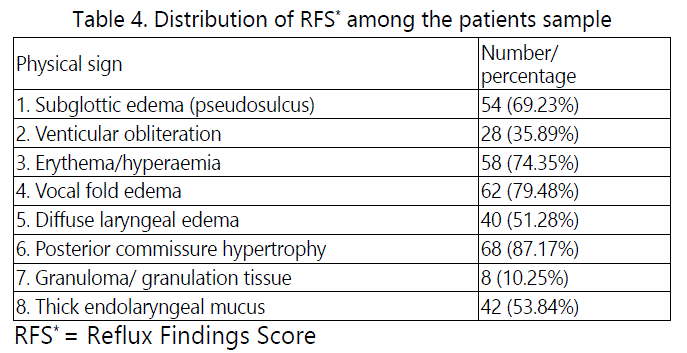
RSI-RFS correlation
A simple and multivariate regression analysis revealed a significant statistical association between sum of the patient's symptoms of RSI and laryngoscopic findings of RFS with P=0.001, while the association between individual variables of RSI and physical findings of RFS revealed the following observations; A significant statistical association was detected between symptom of hoarseness and the following physical signs; posterior commissure hypertrophy, vocal fold edema, and laryngeal erythema and subglottic edema with P< 0.05, also between throat clearing and posterior commissure hypertrophy, diffuse laryngeal edema, thick endolaryngeal mucous with P<0.05, and throat foreign body sensation or lump was statically significant associatedwith diffuse laryngeal edema, laryngeal erythema and thick endolaryngeal mucous with P<0.05, finally the symptom of excess throat mucus or postnasal drip was statically significant associated with the following laryngoscopic finding; posterior commissure hypertrophy, subglottic edema, thick endolaryngeal mucus as well as diffuse laryngeal edema with P< 0.05.
RFS intra-rater reliability results
The study revealed a remarkable consistent intra-rater reliability of ICC scores, as determined by a very close agreement in the evaluation of fibre-optic laryngoscopic physical signs and mean ICCs score of (0.894) for sum RFS, while that of individual variables ICC scores were ranged from (0.881 to 0.920), as shown in table 5.
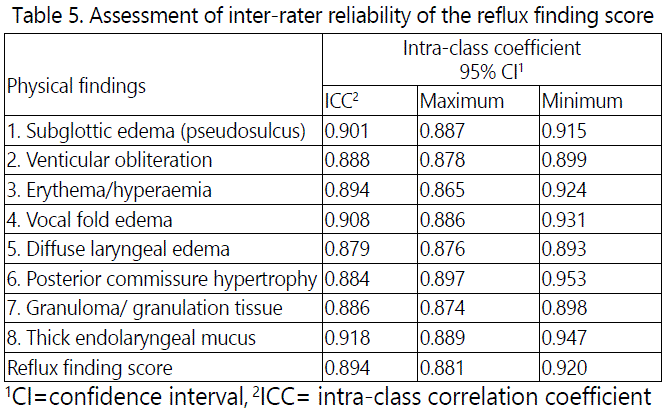
The study reported that none of the control group were found to had reflux symptoms assessed by RFI Belafsky et al questionnaire, as well as none of them had physical laryngeal findings based upon RFS Belafsky et al fibre-optic laryngoscopy.
Discussion
The diagnosis of laryngopharyngeal reflux is not a simple and a straightforward task; however, it is usually based upon clinical consultation through detailed medical history taken with their main complaint of voice related symptoms, and associated with other reflux symptoms, together with the endoscopic identification of the suggestive non-specific physical findings of the laryngeal irritation and inflammation.
Although there is no concrete method that confirm the unambiguously causal relationship between reflux and laryngitis, yet there are 2 approaches that may be applied to verify it diagnosis: first the clinical response of the reflux symptoms with the improvement of the endoscopic reflux laryngeal irritation signs in response to medical and behavioural management, and second the identification of the reflux events by ambulatory multi-channel impedance and 24-hour PH-oesophageal monitoring studies, but unfortunately both these aforementioned approaches were not used in this study, either because of the nature of the study that excluded those patients whom had received or on reflux treatment, and second because of unavailability of PH monitoring tool in our medical centre.
So the main limitation of this study was the lack of the 24-hour PH monitoring test, which considered a gold standard diagnostic tool, so the confirmation of LPR diagnosis was potentially questionable task, however some studies [1,7]. Stated that 24-hour PH monitoring is relatively invasive technique, and did not have a wide acceptance usage in an outpatient setting.
The most frequent symptom detected in this study was hoarseness, followed by the frequent throat clearing, and usually at morning, and this observation was supported by some studies that found dysphonia being a major symptom of LPR, and is more common in morning was due to vocal cords edema that resultant from reflux of gastric acid at supine position night sleep and thus improving during the day time [12], and the most common laryngoscopic physical findings were posterior commissure hypertrophy and vocal cords edema and diffuse laryngeal edema, and these observations were agreed by other studies [13,14].
Belafsky et al types of the measurement tools was used in this study as these tools were validated, easy, non-invasive and can be used as outpatient setting [7]. To reach the diagnosis of LPR, as well as to determine the correlation between the presenting symptoms with voice-related disorders and their physical laryngoscopic findings in order to assess the reliability of RFS.
This study revealed a positive correlation between RSI and RFS, which was confirmed with both significant statistical analysis (p=0.001) and high scores of ICC reliability test, these values were detected above the acceptance level of 0.70. These findings confirm the previous studies observations that support these 2 scales could be very useful for predictable LPR patients [11,13,15]. However some studies found that RFS and RSI have limited value, especially in symptomatic patients if used independently or in isolation [16,17], while Keichner LN et al [18]. In their study detect a notable lack of agreement in reviewing videolaryngoscopic examinations and implementing RFS scores on them.
In analysing the individual symptoms from RSI versus laryngeal finding from RFS with both statistical method and ICC reliability, this study revealed the symptom hoarseness and frequent throat clearing was positively correlated with posterior commissure hypertrophy, and vocal folds and diffuse laryngeal edema, and these results were almost comparable with the findings of other studies [13,14], karakaya NE et al [15]. Whom used a rigid laryngoscope in their study, they found the posterior commissure hypertrophy was most frequent finding in voice related complaints patients, and RFS was with relatively high intra-rater and inter-rater agreement for evaluation of LPR, while RSI was considerably correlated with both sum RFS and all individual variables from RFS, except posterior commissure hypertrophy. The explanation there is some degree of keratinisation and epithelial hyperplasia resultant from chronic exposure of posterior part of the larynx "interarytenoid area" to gastric acid [19]. And this histopathological transformation could represent an irreversible change.
Flexible and rigid laryngoscopes, they concluded that the posterior part of the larynx was difficult to view and assessed properly by rigid laryngoscope, therefore, the arytenoid area and pseudosulcus were more likely to be detected by a flexible rather than rigid laryngoscope. So reliability of RFS should be better assessed with flexible laryngoscopy as "in this study".
Another reason for non-significant correlation of posterior commissure hypertrophy with RSF as some studies demonstrated there were no changes in degree of posterior commissure hypertrophy with LPR in patients whom on long treatment with acid suppressive drugs [21]. However it is worth to mention that any patient receiving LPR treatment was excluded from this study.
The concept of sensitivity and specificity issue of refluxrelated laryngeal physical signs also continued to be a matter of debate [22]. Since no evident physical laryngeal sign could solidify make a diagnosis of laryngeal reflux and appear to be disagreement regarding any degree of LPR is considered normal [23].
The solution of the problem of unreliability of the endoscopic physical laryngeal finding, Branski RC et al [24]. Recommended a training program for otolaryngologist including a set of standard video laryngoscopic examination for identification the individual variable of RFS with rating the degree of its severity.
After many years of researches, both diagnosis and treatment of LPR disease had been subjected for numerous studies due to controversial issue, and even the gold standard PH monitoring method for its diagnosis have been questioned by several authors whom concluded had no 100% sensitivity, so this would impacts on its results and consequently the diagnosis of LPR disease, so continuing studies is required that concerned consensus for diagnosis of LPR disease in order for establishment a proper management of this problem in order to improve patients quality of life [25].
Conclusions
The study revealed hoarseness and posterior commisure hypertrophy were the most common findings detected, with highest positive significant correlation between them, also positive significant correlation between the voice related symptoms based on RSI with both sum and individual variables of physical laryngeal signs based on RFS. Therefore both these scales were considered to be very useful, and complementary to each other for the clinical diagnosis of LPR disease
Conflicts of interests: None declared
References
- Koufman JA, Aviv JE, Casiano RR, Shaw GY. Laryngopharyngeal reflux: position statement of the committee on speech, voice, and swallowing disorders of the American Academy of Otolaryngology-Head and Neck Surgery. Otolaryngol Head Neck Surg. 2002; 127: 32-35. doi: 10.1067/ mhn.2002.125760
- Koufman JA, Cummins MM. The prevalence and spectrum of reflux in laryngology: a prospective study of 132 consecutive patients with laryngeal and voice disorders. Available at: http://legacy.library.ucsf.edu/ tid/trj60d00. Accessed 8 September 2016. 1994.
- Eckley CA, Rios L, Rizzo LV. Salivary EGF concentration in adults with reflux chronic laryngitis before and after treatment: preliminary results. Braz J Otorhinolaryngol. 2007; 73: 156-160.
- Katz PO. Ambulatory esophageal and hypopharyngeal PH monitoring in patients with hoarseness. Am J Gastroenterol. 1990; 85(1): 38-40.
- Uluap SO, Toohill RJ, Hoffmann R, Shaker R. Pharyngeal PH monitoring in patients with posterior laryngitis. Otolaryngol Head Neck Surg. 1999; 120: 672-677. doi: 10.1053/hn.1999.v120.a91774
- Shaw GY, Searl JP. Laryngeal manifestations of gastroesophageal reflux before and after treatment with omeprazole. South Med J. 1997; 90: 1115- 1122.
- Issing WJ, Karkos PD, Perreas K, Folwaczny C, Reichel O. Dual-probe 24- hour ambulatory pH monitoring for diagnosis of laryngopharyngeal reflux. J LaryngolOto. 2004; 118: 845-848. doi: 10.1258/0022215042703660
- Maldonado A, Diecerich L, Castell DO, Gideon RM, Katz PO. Laryngopharyngeal reflux identified using a new catheter design: defining normal values and excluding artefacts. Laryngoscope. 2003; 113: 349-355. doi: 10.1097/00005537-200302000-00027
- Belafsky PC, Postma GN, Koufman JA. Validity and reliability of the reflux symptom index (RSI). J Voice. 2002; 16: 274-277. doi: 10.1097/00005537- 200108000-00001
- Belafsky PC, Postma G.N, Koufman JA. The validity and reliability of the reflux finding score (RFS). Laryngoscope. 2001; 111: 1313-1317. doi: 10.1097/00005537-200108000-00001
- Habermann W, Schmid C, Neumann K, Devaney T, Hammer HF. Reflux symptom index and reflux finding score in otolaryngologic practice. J Voice. 2012; 26: 123-127. doi: 10.1016/j.jvoice.2011.02.004
- Wendl B, Pfeiffer A, Pehl C, Schmidt T, Kaess H. Effect of decaffeination of coffee or tea on gastroesophageal reflux. Aliment Pharmacol Ther. 1994; 8: 283-287.
- Mesallam TA, Stemple JC, Sobeih TM, Elluru RG. Reflux symptom index versus finding score. Ann Otol Rhino Laryngol. 2007; 116: 436-440. doi: 10.1177/000348940711600608
- Silva CED, Niedermeier BT, Portinho F. Reflux laryngitis: correlation between the symptoms findings and indirect laryngoscopy. Int Arch Otorhinolaryngol. 2015; 19: 234-237. doi: 10.1055/s-0034-1399794
- Karakaya NE, Akbulut S, Altintas H, Demir MG, Demir N, et al. The reflux finding score: reliability and correlation to the reflux symptom index. JAREM. 2015; 5: 68-74. dio: 10.5152/jarem.2015.698
- Watson NA, Kwame I, Oakeshott P, Reid F, Rubin JS. Comparing the diagnosis of laryngopharyngeal reflux between the reflux symptom index, clinical consultation and reflux finding score in a group of patients presenting to an ENT clinic with an interest in voice disorders: a pilot study in thirty-five patients. Clin Otolaryngol. 2013; 38(4): 329-333. doi: 10.1111/ coa.12113
- Park KH, Choi SM, Kwon SU, Yoon SW, Kim SU. Diagnosis of laryngopharyngeal reflux among globus patients. Otolaryngol Head Neck Surg. 2006; 134(1): 81-85. doi: 10.1016/j.otohns.2005.08.025
- Keichner LN, Home J, Lee L, Klaben B, Adam S, et al. Reliability of speechlanguage pathologist and otolaryngologist ratings of laryngeal signs of reflux in anasymptomatic population using the reflux finding score. J Voice. 2007; 21: 92-100. doi: 10.1016/j.jvoice.2005.09.004
- Kambic V, Radsel Z. Acid posterior laryngitis: aetiology, histology, diagnosis, and treatment. J LaryngolOtol. 1984; 9: 1237-1240. doi: 10.1017/s0022215100148340
- Milstein CF, Charbel S, Hicks DM, Abelson TI, Richter JE, et al. Prevalence of laryngeal irritation signs associated with reflux in asymptomatic volunteer: impact of endoscopic technique (rigid vs. flexible laryngoscope). Laryngoscope. 2005; 115: 2256-2261. doi: 10.1097/01.mlg.0000184325.44968.b1
- Vaezi MF. Sensitivity and specificity of reflux-attributed laryngeal lesions: experimental and clinical evidence. Am J Med. 2003; 18; 115: 97S-104S.
- Noordzij JP, Khidr A, Evans BA, Desper E, Meek RB, Reibel JF, et al. Correlation of pH probe-measured laryngopharyngeal reflux with symptoms and signs of reflux laryngitis. Laryngoscope. 2002; 112: 2192- 2195. doi: 10.1097/00005537-200212000-00013
- Hil RK, Simpson CB, Velazquez R, Larson N. Pachydermia is not diagnostic of active laryngopharyngeal reflux disease. Laryngoscope. 2004; 114: 1557-1561. doi: 10.1097/00005537-200409000-00010
- Branski RC, Bhattacharyya N, Shapiro J. The reliability of the assessment of endoscopic laryngeal findings associated with laryngopharyngeal reflux disease. Laryngoscope. 2002; 112: 1019-1024. doi: 10.1097/00005537- 200206000-00016
- Vazquez F, Fernandez GS, Gomez MdeL. Laryngopharyngeal reflux: correlation between symptoms and signs by means of clinical assessment questionnaires and fibre endoscopy. Is this sufficient for diagnosis. Acta Otorrinolaringol Esp. 2007; 58: 421-425.


