Case Report
Haemangioma of the Masseter Muscle: A rare vascular Malformation miming a Parotid Tumor
Department of ENT, Hospital of 20 Aou, Casablanca, Morocco
*Corresponding author: Lahcen Elharti, Department of ENT, Hospital of 20 Aou, Casablanca, Morocco, E-mail: lahcen.elharti@gmail.com
Received: May 19, 2017 Accepted: June 14, 2017 Published: June 20, 2017
Citation: ElHariti L, Tatari MM, Anjar S, Beghdad M, Mahtar M, Abada R. Haemangioma of The Masseter Muscle: A Rare Vascular Malformation Miming a Parotid Tumor. Madridge J Otorhinolaryngol. 2017; 2(1): 23-25. doi: 10.18689/mjol-1000104
Copyright: © 2017 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Introduction: Intramuscular haemangioma of Masseter Muscle is a rare benign neoplasm developing from abnormally differentiated blood vessels.
Case report: We report in this article a case of an Haemangioma involving masseter muscle in a 16-year-old girl referred for progressive and unsightly swelling of the right cheek present since 2-years. Clinical examination showed a painless, well circumscribed, and firm swelling in the right cheek. Facial CT Scan with contrast injection revealed a highdensity region in the right masseteric muscle without bone lysis. MRI showed voluminous encapsulated tissue mass in isosignal T1 and T2 in the right masseter muscle. The patient was operated externally by performing an exo-facial parotidectomy with tumorectomy. Discussion: The masseter muscle localization of intramuscular hemangioma represents the most common site (36%), followed by trapezius. Excessive muscle contractions and trauma seem to be important factors in the development of this type of malformation. It is a mass of variable size, unique, mobile and firm. CT and MRI have significantly increased the accuracy of preoperative diagnosis for this lesion. They allow to define precisely its limits and its relations with the neighboring tissues. The treatment of choice is surgical excision of whole lesion with adjacent muscle.
Conclusion: Intra masseter hemangiomas are rare tumors often mistakenly considered as parotid tumors. The essential radiological exam before treatment are CT with injection or MRI. Surgery is the reference treatment.
Keywords: Masseter Muscle; haemangioma; head and neck.
Introduction
Intramuscular haemangioma is a rare benign congenital neoplasm developing from abnormally differentiated blood vessels. Skeletal muscle localization account for less than 1% of cases. The masseter muscle accounts for 5% of all intramuscularhaemangioma of headand neck region.
The present article describe the clinical presentation, diagnostic and treatment modalities of an Haemangioma involving masseter muscle in a 16-year-old girl in whom a surgical excision of whole lesion was done.
Case Report
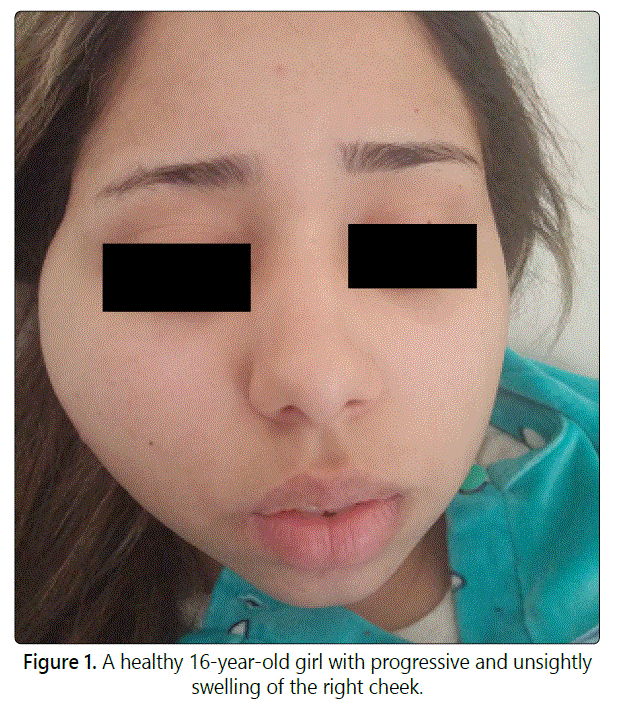
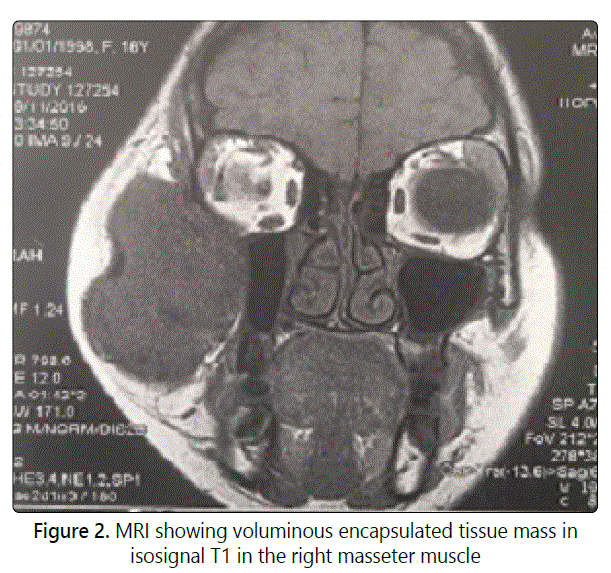
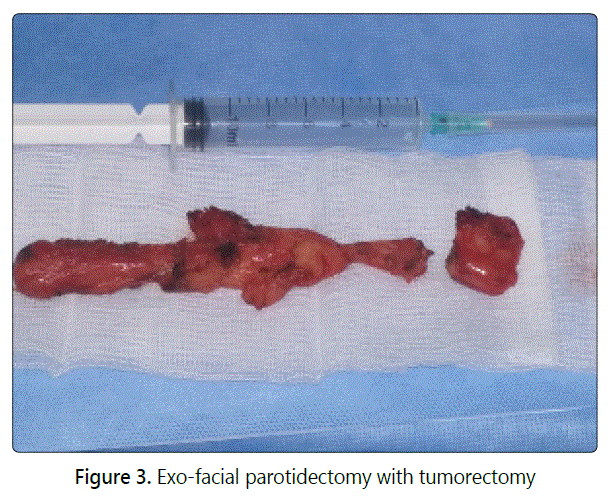
A healthy 16-year-old girl was referred for evaluation and management of progressive, unsightly swelling of the right cheek. The swelling had been present since 2-years and had gradually increased in size. No prior history of trauma, dental problems, trismus or other medical problems was noted. Clinical examination showed a big swelling in the right cheek, measuring 9 cm x 4 cm, painless, well circumscribed, and firm (Fig 1). The overlying skin was freely moveable and not discolored. No pulsation or collateral venous circulations were noted. There was no lymphadenopathy. The patient was otherwise asymptomatic. Facial CT Scan with contrast injection revealed a high-density region in the right masseteric muscle measuring 31 x 47 x 83 mm without bonelysis. MRI showed voluminous encapsulated tissue mass in isosignal T1 and T2 in the right masseter muscle (Fig 2). The arteriography showed a vascularised mass by a branch of the maxillary artery. Preoperative diagnosis was hemangioma of the masseter muscle and surgery was scheduled after arterialembolization. The patient was operated externally by performing an exo-facial parotidectomy with tumorectomy by taking a little part of the masseter muscle (Fig 3). The operative sequences were simple, with facial paresis.
Discussion
Intramuscular Haemangioma are believed to be benign, hamartomatous, congenital neoplasm developing from abnormally differentiated blood vessels and proliferating endothelial cell network [1]. Skeletal muscle localization account for less than 1% of cases [2]. Lessthan 20% of these are found in head and neck region. The masseter muscle represents the most common site (36%), followed by trapezius, sternocleidomastoid, temporalis, mylohyoid, mentalis, buccinator, lip, tongue and salivary glands [1,3]. In 90% of cases, the diagnosisis made before the age of 30 years. There is no racial factor. Excessive muscle contractions and trauma seem to be important factors in the development of this type of malformation. Hormonal factors also play a role. There is indeed a marked increase in volume during menarche, pregnancy and menstrual cycles, whichexplains a slight female predominance for this type of tumor, although for the masseterian sites, the majority of cases are diagnosed in men [4]. Diagnosis of intramuscular hemangioma of the head and neck region can be difficult [5]. Only 8% of all cases of intramuscular hemangiomas are diagnosed pre-operatively [6]. It is a mass of variable size, unique, mobile and firm. In more than half of the cases, intermittent pain is present. This pain is due to muscle compression. Exceptionally, the skin may have a bluish tint, with increased local heat related to hyper vascularization. The beating character and the auscultatorythrill are exceptional because they are often masked by the thickness of the superficial muscular layer. Similarly, it is very rare to observe an increase in the size of the tumefaction, head leaning forward, or "sign of Wattle" which orientates strongly towards the diagnosis. Thesesemiological signs are present in the masseterian sites only in the case of superficial and bulkytumors [4,7]. The differential diagnosis of intramuscular hemangioma of the masseter muscle includes: congenitalcyst, lymphadenopathy, parotid canal sialocele, parotid cancer, lymphangioma, benign or malignant muscle tumor, masseter muscle hypertrophy and schwannoma [7]. Ultrasonography is an inexpensive and noninvasive method, however the information obtained slimited [8]. CT and MRI have significantly increased the accuracy of preoperative diagnosis for this lesion. They allow to define precisely it slimits and its relations with the neighboring tissues. Phlebolith formation and calcification have been reported as a characteristic feature of hemangiomas [4,9]. Arteriography is indicated only in voluminous tumors. It makes it possible to identify the arterial pedicles that feed the tumor and the preoperativeembolization, thus reducing the risk of intra operative bleeding [10]. Manyforms of therapy have been advocated to cure or control intramuscular hemangioma: sclerotherapy, cryotherapy, steroids, radiation and embolization are reported in the literature depending up on its location, size, its growth rate, age of the patient, cosmetic and functional considerations. But the treatment of choice is surgical excision of whole lesion with adjacent muscle [1,3,4,9]. Several surgical approaches have been described. The most used is the external temporoauricular or temporo-auriculo-cervical. The intra-oral approach is possible and does not seem to give more complications than extra-oral approach. A post operative physiotherapy avoids or limits the muscular contractions responsible for a limitation of the mouth opening [2]. Minor feedingvessels and residual tumor are responsible for are currence rate of approximately 18%, with 7% recurring more than once [9].
Conclusion
Intra masseter hemangiomas are rare tumors often mistakenly considered as parotid tumors. The essential radiological exam before treatment are CT with injection or MRI. Surgery is the reference treatment with different possible approaches.
Conflicts of Interest: The authors declare no conflicts of interest with this submission.
References
- Altug HA, et al. Hemangiomas of the head and neck withphleboliths: Clinicalfeatures, diagnostic imaging, and treatment of 3 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007; 103(3): 60-64. doi : 10.1016/j.tripleo.2006.09.006
- Meziane M, et al. Hémangiome du masséter opéré par voie intra-orale Intramasseteric hemangioma operated by intraoral approach. Rev Stomato Chir Maxillo fac. 2010; 111: 168-171. doi: 10.1016/j.stomax.2010.04.004
- Satnam SJ, et al. Intramuscular Cavernous Haemangioma of Masseter Muscle - A Case Report of Surgical Excision. J Clin Diagn Res. 2015; 9(4): 01-02. doi: 10.7860/JCDR/2015/11305.5770
- Allen PW, Enzinger FM. Hemangioma of skeletal muscle. Ananalysis of 89 cases. Cancer. 1972; 29: 8-22. doi: 10.1002/1097-0142
- Demir Z, Oktem F, Celebioglu S. Rare case of intra masseteric cavernous hemangioma in a three-year-old boy: a diagnostic dilemma. Ann Oto Rhinol Laryngol. 2004; 113: 455-8. doi: 10.1177/000348940411300607
- Avci G, Yim S, Misirliogolu A, Akoz T, Kartal LK. Intra masseteric hemangioma. Plast Reconst Surg. 2002; 109: 1748-9.
- Koltsidopoulos P, Skoulakis C. Hémangiome intramusculaire faisant saillie (turkey wattle sign). CMAJ. 2015. doi: 10.1503/cmaj.140364
- Gampper TJ, Morgan RF. Vascular anomalies: hemangiomas. Plast Reconstr Surg. 2002 ; 110 : 572-85.
- Kanaya H, et al. Intramuscular hemangioma of masseter muscle with prominent formation of phleboliths: A case report. Auris Nasus Larynx. 2008 ; 35 : 587-591. doi: 10.1016/j.anl.2007.11.003
- Capote A, Acero J, Garcia-Recuero I, et al. Infratemporal-preauricularcervicalapproach for resection of a cavernousintramasseterichemangioma: a casereport. J Oral Maxillofac Surg. 2008; 66: 2393-7. doi: 10.1016/j. joms.2007.06.650


