Mini-Review Article
Therapies for Pediatric Sialorrhea: A Review of the literature
Department of Otolaryngology - Head and Neck Surgery, University of Tennessee Health Science Center, 62 S Dunlap St #300, Memphis, TN 38103, USA
*Corresponding author: Anthony Sheyn, Assistant Professor, Department of Otolaryngology - Head and Neck Surgery, University of Tennessee Health Science Center; LeBonheur Children's Hospital, Department of Pediatric Otolaryngology, 62 S Dunlap St #300, Memphis, TN 38103, USA, Tel. 513-225-2288, E-mail: asheyn@uthsc.edu
Received: February 29, 2016 Accepted: April 20, 2016 Published: April 25, 2016
Citation: Sheyn A, Thompson J. Therapies for Pediatric Sialorrhea: A Review of the literature. Madridge J Otorhinolaryngol. 2016; 1(1): 12-14. doi: 10.18689/mjol-1000102
Copyright: © 2016 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Sialorrhea in the pediatric population usually affects patients with neuromuscular disorders such as cerebral palsy, muscular dystrophies, and children with anoxic brain injuries in utero and post-partum. These patients have significant neuromuscular incoordination which leads to dysphagia, difficulty handling salivary secretions, and recurrent aspiration pneumonia. In addition to medical complications, pediatric sialorrhea can lead to significant stressors on the patient's family due to constant clothing changes and fears of recurrent illness. Treatments that have been described with varying degrees of success include medical management, Botulinum toxin injection, and surgical management. The articles that were reviewed are listed in Table 1.
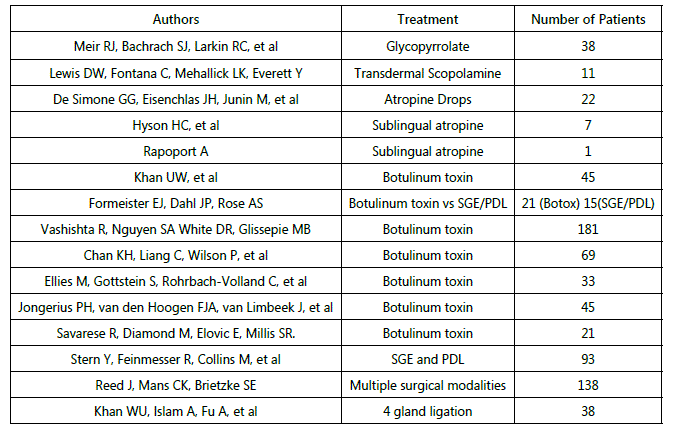
Figure 1: List of Review Articles.
Keywords: Pediatric Sialorrhea; Botulinum toxin injection; Scopalamine; Robinul and Surgical Therapies.
Literature Review
Pediatric patients who suffer from sialorrhea are initially treated with medical therapy. Anticholinergic medications such as Scopalamine and robinul are commonly employed. The main goal is to decrease the volume of salivary secretions. This treatment does not address the associated swallowing disorders that are commonly found in this patient population. In one study 39 children were started on glycopyrrolate (Robinul). Twenty seven completed the study with improvement from severe drooling to dry or mild drooling [1]. Twelve patients dropped out due to side effects of the medication. Other studies, although small, have shown similar efficacies of transdermal scopolamine [2]. Although there seem to be improvements in drooling, particularly in severe cases, a significant portion of the treatment population discontinue systemic anticholinergic therapy due to unacceptable side effects such as xerostomia, pupillary dilation, mouth breathing, and restlessness. Additional research has focused on local therapy in hopes of treating sialorrhea and avoidance of more invasive procedures.
Sublingual atropine has been described in the adult population with some success in patients with neurologic disorders such as Parkinson's disease and less success in patients with sialorrhea following treatment for head and neck cancer [3,4]. Sublingual atropine has been described with some success in the pediatric population in a case report,
but further study is needed to determine if this is a safe and effective treatment strategy [5]. When medical management is ineffective or not tolerated, surgical therapy is usually the next step. These therapies are usually limited to Botulinum toxin injection and surgical excision of glands.
Reported rates of decreased sialorrhea following Botox injection range from 51% to 79% [6]. The wide range of success is likely due to the subjective nature of defining decreased saliva production and the lack of a widely used objective system to determine success rate of medical and surgical therapies. Formeister, et al. utilized the Teacher Drooling Scale
(TDS) to assess the pre- and post-operative saliva production in children with chronic sialorrhea [7]. Other methods of evaluating severity of sialorrhea is inquiring about the number of bib changes per day, Likert scale, the Thomas-Stonell and Greenberg scale, and the drooling impact scale [8].
Botulinum toxin A is the most common type employed in the treatment of sialorrhea. Botulinum toxin B has also been used in the past with some studies revealing equivalent results to type A [9]. Type B has been found to have some systemic anticholinergic effects which are not seen with use of type A.
A third formulation, Botulinum toxin type C is currently being evaluated for use in sialorrhea.
Although less invasive than open surgical procedures,
Botox injection can lead to significant complications. Minor complications include neck pain, nausea and speech problems;
while major complications may include aspiration pneumonia,
prolonged dysphagia, and need for gastrostomy tube placement due to prolonged dysphagia [6,10]. The complication rate leading to hospitalization has been reported to be approximately 7-8% in two studies, while Khan et al reported that 26% of the patients enrolled had minor complications [6,11].
Decreased salivary production may not be noted in patients until 2-3 weeks post-injection, with a gradual return to baseline sialorrhea in 2-3 months [12-14]. Repeated injections are necessary for adequate control.
Due to the wide range of success in utilizing Botox injection for control of sialorrhea and the need for repeated procedures, some patients and families choose to undergo a more permanent open surgical procedure. Formeister, et al.
noted that one third of their patients who underwent Botox injection eventually underwent open surgical procedures [7].
The most common utilized procedure is bilateral submandibular gland excision (SGE) and bilateral parotid duct ligation (PDL). Stern et al looked at 93 patients with chronic sialorrhea who underwent SGE and PDL over a period of 9
years [15]. 87% reported no further drooling over a period of
1-10 years. Additionally, the procedure was found to be quite safe with only 3 post-operative complications, 7 patients reporting xerostomia, and 2 reporting increased dental caries.
A meta-analysis by Reed et al reviewed 47 studies that focused on surgical management of sialorrhea identified a success rate of 81.6% for all surgical procedures [16]. Bilateral SGE and PDL were identified as the most effective procedures with a success rate of 87.8%. Ligation of all 4 ducts was found to be the least effective procedure with a success rate of only
64.1%. Another study evaluated intra oral duct ligation procedures. Procedures included submandibular duct ligation,
3-duct ligation, and 4-duct ligation. All procedures had a recurrence rate of 58% or higher, and the time to recurrence was at the most 6 months [17].
Four duct ligation is another option for treatment of pediatric sialorrhea that offers the advantage of being less invasive compared to gland excision. Khan et al identified 38
patients with sialorrhea who underwent four duct ligation
[18]. There was subjective improvement in sialorrhea at 1
month in 80% of patients and at 1 year in 69% of patients.
Decreased sialorrhea was noted to last up to 20.4 months,
significantly longer than botulinum toxin effects but not as good as excision of submandibular glands and ligation of parotid ducts.
A multi-disciplinary approach for the treatment of sialorrhea has gained attention over the past several years. A
2 year experience at Nationwide Children's Hospital was recently published describing the effectiveness of their multidisciplinary clinic [19]. The clinic included specialists from pediatric otolaryngology, speech language pathology,
physical medicine and rehabilitation, and pulmonology. The authors felt that due to the complex nature of pediatric sialorrhea a more comprehensive evaluation and treatment strategy should be employed for patients with this disorder.
Conclusion
Pediatric sialorrhea is a complex disorder that may be difficult to control. Various treatment strategies have been employed over the years with varying efficacies. While effective medical management is available it carries a higher risk of systemic side effects relative to surgical therapy. The most effective surgical treatments include Botulinum toxin injection and bilateral submandibular gland excision and parotid duct ligation. While still in its early stages, a multidisciplinary approach may prove to be the most effective method of approaching pediatric sialorrhea.
Conflicts of Interest: The author(s) report(s) no conflicts of interest.
References
- Richard J Mier, Steven J Bachrach, Ryan C Lakin, Tara Barker, Judith Childs, Maria Moran. Treatment of sialorrhea with glycopyrrolate: a double-blind dose ranging study. Arch Pediatr Adolesc Med. 2000; 154(12): 1214-1218. doi: 10.1001/archpedi.154.12.1214
- Lewis DW, Fontana C, Mehallick LK, Everett Y. Transdermal scopolamine for reduction of drooling in developmentally delayed children. Development Medicine and Child Neurology. 1994; 36(6): 484-486. doi: 10.1111/j.1469-8749.1994.tb11877.x
- De Simone GG, Eisenchlas JH, Junin M, Pereyra F, Brizuela R. Atropine drops for drooling: A randomized controlled trial. Palliat Med. 2006; 20: 665-671. doi: 10.1177/0269216306071702
- Hyson HC, Johnson AM, Jog MS. Sublingual atropine for sialorrhea secondary to parkinsonism: a pilot study. Mov Disord. 2002; 17: 1318- 1320. doi: 10.1002/mds.10276
- Rapoport A. Sublingual atropine drops for the treatment of pediatric sialorrhea. J Pain Symptom Mangmnt. 2010; 40: 783-788. doi: 10.1016/j. jpainsymman.2010.02.007
- Khan UW, Campisi S, Nadaraja YA, et al. Botulinum toxin A for treatment of sialorrhea in children: an effective, minimally invasive approach. Arch Otolaryngol Head Neck Surg. 2011; 137: 339-344. doi: 10.1001/ archoto.2010.240
- Formeister EJ, Dahl JP, Rose AS. Surgical management of chronic sialorrhea in pediatric patients: 10 year experience from one tertiary care institution. Int J Ped Otorhinolaryngo. 2014; 78: 1387-1392. doi: 10.1016/j. ijporl.2014.06.005
- Daniel SJ. Botulinum toxin injection techniques for pediatric sialorrhea. Operative Technique in Otolaryngol. 2015; 26: 42-49. doi: 10.1016/j. otot.2015.01.004
- Schroeder AS, Kling T, Huss K, et al. Botulinum toxin type A and B for the reduction of hypersalivation in children with neurological disorders: A focus on effectiveness and therapy adherence. Neuropediatrics. 2012; 43(1): 27-36. doi: 10.1055/s-0032-1307457
- Vashishta R, Nguyen SA White DR, Glissepie MB. Botulinum toxin for the treatment of sialorrhea: a meta-analysis. Otolaryngol Head Neck Surg. 2013; 148(2): 191-196. doi: 10.1177/0194599812465059
- Chan KH, Liang C, Wilson P, Higgins D, Allen GC. Long term safety and efficacy data on Botulinum toxin type a: an injection for sialorrhea. JAMA Otolaryngol Head Neck Surg. 2013; 139: 134-138. doi: 10.1001/ jamaoto.2013.1328
- Ellies M, Gottstein U, Rohrbach-Volland S, Arglebe C, Laskawi R. Reduction of salivary flow with Botulinum toxin: extended report on 33 patients with drooling, salivary fistulas and sialadenitis. Laryngoscope. 2004; 114: 1856-1860. doi: 10.1097/00005537-200410000-00033
- Jongerius PH, van den Hoogen FJ, van Limbeek J, Gabreëls FJ, van Hulst K, Rotteveel JJ. Effect of botulinum toxin in the treatment of drooling: a controlled clinical trial. Pediatrics. 2004; 114(3): 620-627.
- Savarese R, Diamond M, Elovic E, Millis SR. Intraparotid injection of Botulinum toxin A as a treatment to control sialorrhea in children with cerebral palsy. Am J Phys Med Rehabil. 2004; 83: 304-311.
- Stern Y, Feinmesser R, Collins M, et al. Bilateral submandibular gland excision and parotid duct ligation for treatment of sialorrhea in children: long-term results. Arch Otolaryngol Head Neck Surg. 2002; 128: 801-803. doi: 10.1001/archotol.128.7.801
- Reed J, Mans CK, Brietzke SE. Surgical management of drooling: a metaanalysis. Arch Otolaryngol Head Neck Surg. 2009; 135: 924-931. doi: 10.1001/archoto.2009.110
- Martin TJ, Conley SF. Long term efficacy of intra-oral surgery for sialorrhea. Otolaryngol Head Neck Surg. 2007; 137: 54-58. doi: 10.1016/j. otohns.2007.01.034
- Khan WU, Islam A, Fu A, et al. Four-duct Ligation for the treatment of sialorrhea in children. JAMA Otolaryngol Head Neck Surg. 2016; 142(3): 278-283. doi: 10.1001/jamaoto.2015.3592
- Ali SA, Haney J, Payne L, Grischkan JM. Initial experience from a multidisciplinary pediatric salivary gland disorder clinic. Int J Ped Otorhinolaryngo. 2015; 79: 1505-1509. doi: 10.1016/j.ijporl.2015.06.038


