Research Article
Prevalence of Pseudoexfoliation Syndrome in Erbil population: A hospital based study
Department of Ophthalmology, Erbil Teaching Hospital, Erbil, Iraq
*Corresponding author: Adeeb M Ubeid, Department of Ophthalmology, Erbil Teaching Hospital, Erbil, Khanzad St, Iraq, Tel: +9647504462654, Fax: +9647506462654, E-mail: akrawiadeeb@gmail.com
Received: January 5, 2018 Accepted: January 29, 2018 Published: February 3, 2018
Citation: Ubeid AM. Prevalence of pseudoexfoliation syndrome in Erbil population: A hospital based study. Madridge J Ophthalmol. 2018; 3(1): 33-35. doi: 10.18689/mjop-1000110
Copyright: © 2018 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Purpose: To study the prevalence of pseudoexfoliation syndrome in Erbil population.
Materials and Methods: A hospital based study carried out at the department of ophthalmology, Erbil Teaching hospitals, Erbil, Iraq (Sept. 2007- Nov. 2009). A total 620 patients of 50 years and above were examined for evidence of and pseudoexfoliation those with the disease were subjected to further examinations including intraocular pressure measurement, gonioscopy and dilated fundus examination. Pseudoexfoliation was diagnosed clinically by the presence of typical pseudoexfoliative material at the pupillary border before dilatation or anterior lens capsule after pupil dilatation.
Results: Out of 620 patients, 100 (16.1%) were found to be having pseudoexfoliation syndrome. The disease was unilateral in 42 cases and bilateral in 58. There were 67 males and 43 females with male to female ratio of 1.3:1. 23% of the subjects had high intraocular pressure. of the 100 patients with pseudoexfoliation syndrome, 94 patients had cataract.
Conclusion: To the best of our knowledge, this is the 1st study conducted in Kurdistan/ North of Iraq region to determine the prevalence of pseudoexfoliation syndrome. It is a common disease in our population. A prevalence of 16.1% was identified in this hospital based study. The prevalence increased with advancing age. A high percentage of patients had high intraocular pressure.
Keywords: Pseudoexfoliation syndrome; Prevalence; Erbil
Introduction
Pseudoexfoliation (PEX) syndrome is a common ocular disorder of the elderly in many part of the world [1]. It is characterized by the deposition of a distinctive fibrillary material in the anterior segment of the eye. Histologically, this material has been found in and on the lens epithelium and capsule, pupillary margin, ciliary epithelium, iris pigment epithelium, iris stroma and blood vessels, and subconjunctival tissue. Although the origin of this material is not known precisely, it probably arises from multiple sources as a part of generalized basement disorder [2]. Clinical diagnosis is made by the presence of typical pseudoexfoliative material (PXM) on the anterior capsule surface and/or the pupillary margin. In addition to PXM, other features include endothelial pigmentation, loss of pupillary ruff, iris transillumination, sampaolesi's line and pigment deposition in the trabecular meshwork [3]. Pseudoexfoliation syndrome is associated with various ocular complications including elevated intraocular pressure, glaucoma, poor mydriasis, zonular weakness, corneal endotheliopathy, higher rate of vitreous loss during cataract surgery, postoperative complications such as capsular phimosis, and opacification. However, in many cases PEX remains asymptomatic. PEX syndrome is rarely seen before the age 50 and its prevalence increases markedly with age [4]. Although it occurs in virtually every area of the world, it prevalence varies depending on race, sex, age, and geography; for example, it is least prevalent in Eskimos (0%), where is the highest prevalence is in Najavo Indians (38%) [5,6]. The primary aim of our epidemiological study is to assess the prevalence of pseudoexfoliation syndrome in Erbil population, provide a descriptive analysis and report several clinical and ocular associations.
Materials and Methods
This study was approved by the Ethics Committee of Hawler Medical University and performed in adherence to the tenets of the Declaration of Helsinki. A total of 620 patients who aged 50 years or older attending the ophthalmic outpatient units of Erbil and Rizgary Teaching hospitals, Erbil, Iraq were recruited in this study. Written informed consent was obtained from all patients enrolled in this cross-sectional non-interventional study and ethics committee approval was granted.
Relevant details in medical and ocular history were obtained from each patient including history of diabetes mellitus and systemic arterial hypertension. A complete ocular examination is conducted in all patients including slit lampbiomicroscopy before and after mydriasis, intraocular pressure (IOP) measurement with Goldman tonometer and dilated fundus examination. Gonioscopy was performed in all PEX patients using Goldman triple mirror. Following the examination, the patients were classified into two groups: the PEX group and the non-PEX group. PEX syndrome was diagnosed clinically the presence of typical fluffy, white granular material at the pupillary margin before mydriasis or anterior lens capsule after mydriasis. The consequent analyses were conducted on the basis of a person, not per eye. Grading of the angle was done with Schaffer system of gonioscopic classification. Angle width was classified as narrow for those with Schaffer grade 0–2 and open for those with grade 3–4. Cataracts were assessed and classified morphologically as follows: nuclear sclerosis (NS), cortical (C), and posterior subcapsular (PSC). An average of three intraocular pressure (IOP) readings was computed for each eye and any IOP of more than 21 was considered as high. Systemic hypertension was diagnosed if the systolic blood pressure was 140 and/or diastolic blood pressure 90 mmHg or higher or the patient has history of hypertension with current use of systemic antihypertensive medications. Diabetes was determined from history with current use of antidiabetic medications or a postprandial blood sugar of 180mg/dl or greater.
All statistical analyses were conducted using Statistical Package for Social Studies (SPSS version 15.0), and Chi square and t tests were applied. A P value < 0.05 was considered as statistically significant.
Results
Out of the 620 patients examined, 100 were found to have PEX with an overall prevalence of 16.1% in those aged ≥ 50 years.
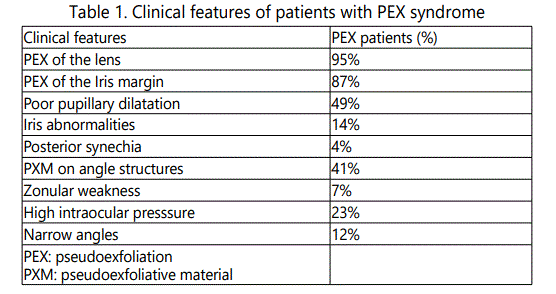
PEX deposits were found on anterior lens capsule in 95% of patients with PEX and on the pupillary border in 87%. The salient clinical features of patients with PEX are shown in table 1.
The mean age of subjects with PEX was 67.86 year (SD8.06) while the mean age of subjects was without PEX was 61.15(SD 7.84), the difference being significant (p<0.001). The median age for participants with PEX was 69 years (age range 50-90 years).The prevalence of PEX syndrome was found to increase with age, from 2.58 % in the50-59 age group to 8.05 % in patients 70 years and older age group (p <0.001).
Among subjects without PEX, 55.4% were men and 44.6% were women. There was no significant difference in sex distribution between both groups, this remained after adjusting for age ('z' test, p=0.953).
of the 100 patients with PEX, 57(21.5%) were males and 43(12.1%) were females, and the difference was significant (p=0.016).
The disease was unilateral in 42% of the subjects and bilateral in 58%, the proportion of patients with bilateral PEX was not significantly older than those with unilateral disease (p=0.341).
The mean intraocular pressure (IOP) in people with PEX was 18.51±3.2 mmHg compared to 15.7±2.7 in those without PEX (p=0.001).Twenty-three (23%) cases with PEX has IOP higher than 21 mmHg at presentation.
The most common type of cataract in PEX subjects was mixed cataract (46%), while nuclear sclerosis was the second common morphology type (39%), cortical and posterior subcapsular opacities were observed in 5% and 4% of subjects respectively.
Thirty one percent of patients with PEX had hypertension while sixteen had diabetes mellitus, with a prevalence of 30 and 20 percent respectively. We found no statistically significant association between PEX and diabetes mellitus (p=0.18) or systemic hypertension (p=0.25).
Discussion
The reported prevalence rate of pesudoexfoliation syndrome in different populations shows extensive variation, a 0% prevalence were reported in Eskimos [5], 1.8% in the United States [7], 5-25% in the Scandanavian countries [5], and 38% in Navajo Indians [6].
This study is a first study of its kind in Kurdistan region north of Iraq. Our examined population was sampled from a general hospital and we found the prevalence PEX to be 16.1%. This finding is higher than the prevalence data reported from neighboring countries like Iran (13.1%) [8], Saudi Arabia (13%) [9] and Turkey (7.2%) [10]. It is quite possible that this higher prevalence rate in our study may be due to the design of our study which was hospital study, whereas most of the above statistics are the result of population based surveys.
The mean age of subjects with PEX in our study was 67.86. This was significantly higher compared to 61.15 in whole examined population. The reported mean age of PEX ranges from 69-75 years in different populations [11].
We found a higher prevalence of PEX among men than in women (21.5% and 12.1% respectively). The difference was statistically significant. A higher prevalence of PEX in men has been reported in Turkey [10], although some studies have reported a female preponderance [7,11] whereas others demonstrated equal gender distribution [9,12].
The distribution of bilateral vs. unilateral cases is highly variable in reported series. In our survey, the bilateral cases outnumbered unilateral cases representing 58% and 42% of cases respectively. Thomas et al, [13] reported ultrastructural alterations in anterior segment tissues of all apparently non involved eyes in clinically unilateral PEX supporting the concept that PEX is basically bilateral disorder with clinically marked asymmetric manifestation.
High IOP was recorded in 23% of subjects with PEX. Most studies have shown prevalence of high IOP with or without glaucoma to be in between 22 to 30% or about 6-10 times the rate in eyes without PEX [14,15,16]. Chronic pressure elevation in eyes with PEX is caused by an increased outflow resistance in the trabecular meshwork as a result of a blockage of the outflow channels by pseudoexfoliative material. The mean IOP in people with PEX was 18.51mmHg compared to 15.7mmHg in those without PEX.
Increasing evidence suggest an etiological association between PEX and cataract formation. Over 90% of the phakic eyes with PEX in our study had some lens opacity. A quite similar result reported by Yalaz [10] who showed a prevalence of 88.1% in his PEX patients. Nuclear opacity was the commonest type of lens opacity observed followed cortical and posterior subcapsular opacities. This finding is in accordance with similar results reported in the Beaver Dam Eye Study [11] and Framingham Eye Study [17]. In contrast, cortical opacities were most prevalent in African [18] and Indian population [19].
We found no statistically significant association between PEX and diabetes mellitus or systemic hypertension. Similar reports have been shown in Croatia [20]. McCarthy [21] also didn't find an association between PEX and history of hypertension or use of antihypertensive medications. However, Mitchell [22] found PEX to be significantly associated with hypertension and Sollosy [23] recorded a high incidence of PEX in diabetic patients. An association of PEX with systemic diseases has so far only been established by rather small-scale retrospective studies in single centers. A carefully planned prospective, randomized multicenter study is warranted to finally asses a cause and effect relation of systemic diseases.
Conclusion
To the best of our knowledge, this is the 1st study conducted in Kurdistan region/North of Iraq to determine the prevalence of PEX syndrome. It is a common disease in our population. A prevalence of 16.1% was identified in this hospital based study. The prevalence increased with advancing age. A high percentage of patients had high IOP.
References