Research Article
Like a Modern Day, Sherlock Holmes: Diagnosing and Differentiating the Etiology of Altered Mental Status
1Assistant Professor, Section of Emergency Medicine, Baylor College of Medicine Ben Taub General Hospital 1504 Taub Loop Houston, Texas USA
2Menninger Departments of Psychiatry and Behavioral Sciences, Baylor College of Medicine Houston, Texas, USA
3Section of Emergency Medicine, Baylor College of Medicine, Ben Taub General Hospital 1504 Taub Loop Houston, Texas USA
*Corresponding author: Veronica Tucci, Section of Emergency Medicine, Baylor College of Medicine, Ben Taub General Hospital, 1504 Taub Loop, Houston, Texas, USA, E-mail: vtuccimd@gmail.com
Received: June 19, 2017 Accepted: October 12, 2017 Published: October 20, 2017
Citation: Sekhon N, Moukaddam N, Tucci V. Like a Modern Day, Sherlock Holmes: Diagnosing and Differentiating the Etiology of Altered Mental Status. Madridge J Intern Emerg Med. 2017; 1(1): 14-24. doi: 10.18689/mjiem-1000104
Copyright: © 2017 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Altered mental status is a challenging clinical syndrome that often confronts the emergency physician and represents up to 10% of all Emergency Department visits. Like a modern day Sherlock Holmes, the emergency provider is tasked with ascertaining whether the change in mental status is secondary to delirium, dementia, or psychosis. Failure to properly investigate and diagnose delirium results in worse outcomes. A good history, including obtaining collateral information, is essential in patients who present with altered mental status. Initial evaluation should include an assessment of the patient’s airway, breathing and circulatory status, in addition to a blood glucose measurement. Hypoglycemia is one of the most easily recognized and reversible cause of delirium. Additional laboratory testing and imaging should be tailored by the history and physical examination.
Keywords: Altered mental status; Delirium; Dementia; Abnormal mentation; Altered level of consciousness; Altered mentation; Acute confusional state; Confusion; Change in cognitive function; Madness mimickers.
Case Presentations
My name is Sherlock Holmes. It is my business to know what other people don’t know. The Adventure of the Blue Carbuncle, Arthur Conan Doyle
Case #1: It is a busy Friday overnight shift at your friendly, inner city county hospital. You just put your coffee down when a nurse walks up to you and states: “We have a schizophrenic patient for you in Room 2. He’s starting to act up, can we give him something.” You walk into the room and see a disheveled 43 year old male who is tremulous, alert only to self and picking at the spiders that only he can see. You decide to check his pulse and note that it is in the 15’s. You look at the triage vitals and note that his initial blood pressure was 170/110.
Case #2: Next, you sign up for a 30 year old patient who comes in for a medication refill of his lactulose. Thinking to yourself that this might be an easy disposition, you are surprised that when you evaluate him he only alert to self. On exam, you also note that the patient has no stigmata of liver disease. You are intrigued. You call his mother who tells you that he was recently admitted to an outside Intensive Care Unit a month ago for altered mental status, and they figured out that he had an elevated ammonia level but a normal liver panel. You examine the patient, and he has profound asterixis.
Case #3: 25 year old female who presents to the Emergency Department for a new-onset of bizarre behavior. She is alert to person and place, and she is paranoid that the C.I.A. is out to get her. You talk to her parents who states that she had been sick with a flu-like illness a month ago, and has since become more violent and paranoid. The family notes that she had a seizure yesterday, which she never had before. You begin to wonder if this is something more than new-onset psychosis.
Introduction
Altered mental status is a common, but challenging chief complaint for patients that visit the Emergency Department, with studies suggesting that it accounts for up to 10% of all visits [1] [2]. Altered mental status is a vague term that encompasses a wide variety of brain dysfunctions, ranging from coma to stupor to delirium.
Of these dysfunctions, the diagnosis of delirium is often the most challenging as made evident by fact that Emergency Department physicians miss the diagnosis in between 57-83% in elderly patients [3-6]. Also, if the diagnosis is missed in the Emergency Department, a study showed that 93.8% of the time the inpatient physicians missed the diagnosis as well [6]. Also, if a patient with delirium is sent home, those patients have increased morbidity and mortality as compared to those who are appropriately diagnosed and admitted to the hospital [5] [6]. Even when patients with delirium are admitted to the hospital, they have increased mortality, as high as 10% in some studies [1]. This demonstrates the importance of making the diagnosis of delirium in the Emergency Department and finding the underlying cause, which will be the focus of this article.
The Emergency Medicine physician often takes care of patients with acute changes in their mental status, and the rapid recognition and treatment of delirium improves outcomes. This review article discusses how to diagnose delirium and how to differentiate between the myriad of different causes of delirium.
Methods
There is actually a dearth of information on altered mental status in the Emergency Department setting. A literature search was performed using PubMed online with the following search terms: altered mental status, altered mental status emergency, delirium, delirium emergency and altered mental status delirium. Approximately 2000 articles from 1965 to present were reviewed. The National Guideline Clearing house and the Cochrane Database of Systematic Reviews were searched with the terms altered mental status and delirium and 2 and 5 review articles were reviewed, respectively. To find additional primary literature, a search for altered mental status and delirium was performed in the following emergency medicine journals: Annals of Emergency Medicine, the American Journal of Emergency Medicine, Academic Emergency Medicine, Emergency Medicine Clinics of North America and Western Journal of Emergency Medicine. The bibliographies of these articles were examined to verify accurate representation of the literature.
Relevant Practice Guidelines
Altered mental status is a vague term that can apply both to the comatose patient as well as the patient with excited delirium. It is difficult to define, but Posner in his landmark paper defined it as a change in cognitive function or level of consciousness. Consciousness consists of two parts:
Delirium
In the Emergency Department, the physician is often tasked with finding the etiology of an acute change in mental status. Most often, the cause is delirium. Delirium is a syndrome, or a group of symptoms [12], and the DSM-V’s definition is listed in Box 1 below.

According to the DSM-V, delirium involves a change in attention, awareness and cognition that developed over a short period of time that is caused by a medical condition. Delirium itself can be broken down into three different types, summarized in table 1.

Hyperactive delirium is characterized by psychomotor agitation and is the least common subtype of delirium [6]. Hyperactive delirium is most often caused by ingestion of illegal drugs or alcohol withdrawal/intoxication, but can also be infectious.
Hypoactive and mixed delirium are more common, and more commonly found in the elderly. The diagnosis of hypoactive delirium can be especially challenging, as the psychomotor slowing can often be attributed to fatigue or depression [15] [16]. A study by Farrell, et. al. showed that among elderly admitted patients to a hospital that had psychiatric consultations for Major Depressive Disorder, 28 out of 67 patients were actually found to be delirious, which illustrates the challenge in diagnosing the patient with hypoactive delirium. In addition to being difficult to diagnose, Kiely and colleagues showed that in 457 patients who were admitted with delirium, it was the patients who had hypoactive delirium that had worse one year mortality [18].
Delirium can be caused by a variety of medical conditions, including toxicologic, infectious, endocrine, neurologic, traumatic and psychiatric insults. However, the degree of insult that it takes to induce delirium varies from patient to patient. Risk factors for delirium include those who have a decreased cognitive reserve. These include: old age, dementia, Parkinson’s disease, stroke, sensory impairment and poly pharmacy [19-21]. Also, a single episode of delirium also may more than double the risk of dementia in a patient [22].
It is also important to note that delirium is generally reversible if the underlying cause is discovered [23], which highlight the importance of finding that cause in delirious patients.
Patho physiology of Delirium
The pathophysiology of delirium remains incompletely understood, likely due to the fact that delirium is multifactorial and there are likely many different mechanisms that induce delirium. Fong et al, used single photon emission computed tomography to suggest that delirium may be secondary to cerebral hypo perfusion [24]. Other studies have showed that delirium is associated with imbalances in neurotransmitters; most notably serotonin, dopamine and increased anticholinergic activity have all been implicated [25-28]. However, despite these advances, no unifying theory has been established to define delirium.
Dementia versus Delirium
As compared to delirium, dementia is a more chronic, indolent process. For patients that present to the Emergency Department, establishing a time course can be very helpful in distinguishing between the two. Delirium usually begins acutely, while the changes in dementia begin slowly over months to years. Also, patients with delirium tend to have fluctuations in awareness while dementia tends to have a more stable decline. Other changes that tend to lend towards delirium are increased level of inattention and decreased levels of arousal. In patients who have dementia, the attention span and level of arousal tend to be relatively preserved.

Psychosis versus Delirium
It is important to distinguish patients who are psychotic from those who are delirious. These patients are especially challenging given the underlying cognitive dysfunction in patients which make obtaining an accurate history difficulty, in addition to causing clinicians to erroneously attribute changes in consciousness to psychosis.
Fortunately, there are clinical indicators that can help differentiate psychosis from delirium. One key point is that patients who are psychotic tend to keep their orientation, while those who are delirious do not. Also, patients who are delirious tend to have visual hallucinations, while those who are psychotic tend to have auditory hallucinations. In some cases, psychotic patients display thought blocking and inability to respond quickly enough, which can be confused for disorientation. The table below highlights some of the differences between psychosis and delirium.
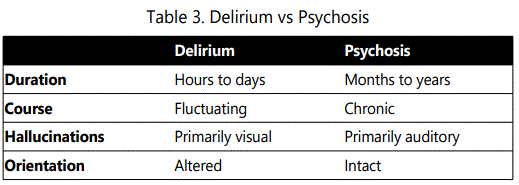
Causes of Altered Mental Status
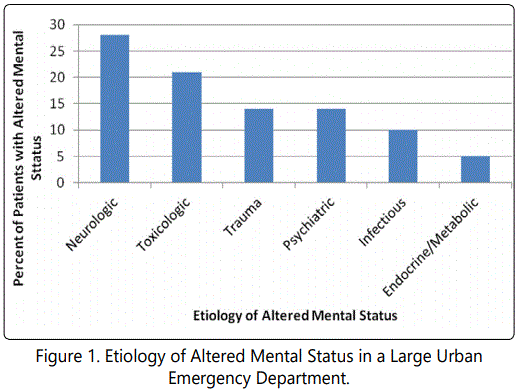
The differential diagnosis for the etiology of altered mental status can be broken up into three main groups: delirium, psychosis, and dementia. We will talk in detail about delirium as it is the focus of this article as it is usually reversible if the underlying cause is treated.
Adapted from data from i. Kanich W, Brady WJ, Huff JS, et al. altered mental status: evaluation and etiology in the ED. Am J Emerg Med. 2002; 20(7): 613-17.
The causes of delirium are far too numerous to list here, but the more common and life-threatening diagnoses are listed on the table below.
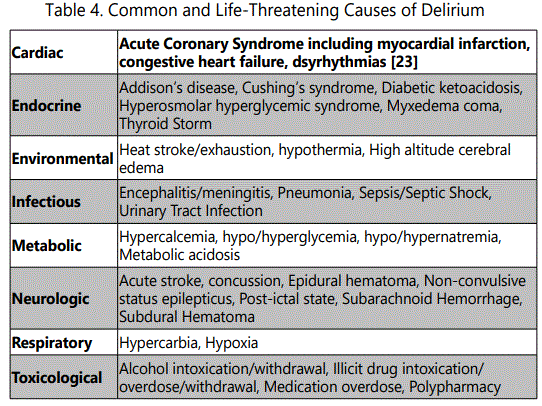
When confronted with a patient with delirium, it is important to first assess for life-threatening, yet easily reversible, causes of delirium. These include hypoglycemia, opioid overdose, hypoxia and hypotension.
Selected Causes of Delirium
Hypoglycemia
Hypoglycemia is a very common and easily reversible cause of altered mental status. Studies suggest that up to 10% of altered Emergency Department patients are hypoglycemic [29]. As the number of patients with Diabetes continues to increase, the number of patients with hypoglycemia is only going to increase as well. Patients who are hypoglycemic have a variety of presentations, from the mildly confused to the comatose.
It is also important to find the underlying cause of why the patient became hypoglycemic. The causes of hypoglycemic include infection, cirrhosis, acute myocardial infection, change in meal pattern and overuse of insulin and sulfonylureas. Interestingly, one study of 228 patients found that 5.70% were hypoglycemic secondary to sepsis, underlying the point that the etiology for the hypoglycemic episode should be searched for by the Emergency Physician.
Sinert et al did a study of 291 patients who presented to the Emergency Department with hypoglycemia and 23% of them were diagnosed with new renal failure, 11% with hyperkalemia, 8% with hypokalemia and 19% with pyuria [30]. This suggests that routine laboratory testing may be indicated in hypoglycemic patients.
Opioid Overdose
Opioid overdose is becoming a more common presentation of delirium, causing over 15,000 deaths per year [31]. Patients with opioid overdoses classically present with respiratory depression, decreased mental status and pinpoint pupils. Opioids have also been shown to decrease the respiratory response to hypoxia [32], which makes the respiratory depression all the more concerning. Fortunately, opioid overdoses are easily treated with naloxone. Care should be used to not precipitate acute withdrawal in these patients with excessive doses of naloxone.
Hypoxia
Hypoxia is a life threatening but usually reversible cause of altered mental status. This changes mental status by reduced oxygen supply to the brain, which negatively affects cerebral processes. These patients usually respond to the administration of oxygen, but the key is to find the underlying cause of the decreased oxygenation. Common causes include: pneumonia, pulmonary embolism, pneumothorax, congestive heart failure exacerbation, exacerbations of reactive airway diseases.
Bacterial Meningitis
Altered mental when caused by meningitis is a lifethreatening emergency, with mortality rates in the literature ranging from 18.4% [33] to 25% [34]. The classic triad for the diagnosis of meningitis is: fever, nuchal rigidity and altered mental status/headache. Unfortunately, meningitis is also common in patients without the triad, with retrospective case reviews showing that in bacterial meningitis the number of patients that presented with the triad varied from as low as 21.2% to as high as 67% [33-35]. Also, it is classically taught in medical school that nuchal rigidity, Kernig’s and Brudzinsky’s signs can be used to assess for bacterial meningitis. However, studies show that the sensitivities of these tests are very low, from 5% to 64% a newer test, the jolt accentuation test has been thought to be used to rule out bacterial meningitis. Unfortunately, recent studies do not bear this out. Thus, a high level suspicious is needed to diagnose meningitis. Diagnosis is confirmed with a lumbar puncture.
Alcohol and Drug Toxicity/Withdrawal
Alcohol related visits are a common occurrence in the Emergency Department. Alcohol intoxications often present smelling like alcohol, with presentations varying from decreased mental status requiring intubation to belligerence. Alcohol levels can be done to confirm the diagnosis, but the history and physical is usually sufficient.
Alcohol/Benzodiazepine withdrawal is a spectrum of disease (ranging from mild withdrawal symptoms to severe delirium tremens) that can be a life threatening cause of altered mental status. Symptoms can include autonomic and psychomotor hyperactivity, tremor, insomnia, nausea, hallucinations, anxiety and seizures. Diagnosis is primary clinical, and the mainstay of treatment are benzodiazepines. Of note, a recent randomized controlled of 101 patients by Rosenson et al showed that a single dose of phenobarbital when used in conjunction with benzodiazepines reduced ICU admissions from 25% to 8% and had no difference in adverse events.
Synthetic cannabinoids are rapidly becoming a more common drug of abuse due to its cheap price and ready availability. Synthetic cannabinoids go by a variety of names including K2, spice, Kush and Cloud 9. Due to the wide variety of chemicals and production processes involved, the presentations can be quite varied. According to 418 cases reported to the Texas Poison Control, the following clinical effects were noted: tachycardia 36.6%, agitation 19.1%, drowsiness 17.5%, and 11.2% had hallucinations and delusions. Notably, synthetic cannabinoids have also been associated with increased rates of acute kidney injury, making evaluation with basic metabolic panels more necessary. There are no routine drug screens to help with diagnosis, so diagnosis is primary clinical. Treatment is primary supportive with fluid hydration and benzodiazepines.
Medication Side Effects
A variety of medications have been associated with precipitating delirium, especially those in high risk populations like the elderly and those with reduced cognitive reserve. Benzodiazepines and opioids are a well-known culprit and must be used with caution in high-risk populations. Medications with ant cholinergic properties have been thought to increase the risk of delirium in patients; however recent studies do put these thoughts into question.
A recent observational cohort study of 147 elderly patients with cognitive impairment did not show that the use of anticholinergic medications increased the risk of delirium. Another prospective study of 1,112 patients did not show any increase in delirium in critically ill patients with increasing anticholinergic activity of the medications prescribed. Other medication classes that have been thought to induce delirium include tricyclic antidepressants, anti-Parkinsonism medications, and steroids. These mediations should be used with caution in high risk patients.
Cereberovascular accidents
With the current pressure to improving door to needle times for patients that are have an acute stroke, the challenge in diagnosing a stroke in a patient with altered mental status is quite challenging. It is helpful to know what kinds of stroke subtypes are associated with particular changes in mental status, so that a focused neurologic exam can be performed. Basilar artery occlusion can be associated with decreased mental status and even coma. Left middle cerebral artery occlusion can cause Wernicke’s aphasia (the inability to understand language in its written or spoke form), which can be confused for psychosis. In addition, agitation has been described in patients that have right middle cerebral artery infarctions, non-dominant parietal lobe infarcts and posterior cerebral artery infarcts.
Given the wide variety of different kinds of altered mental status that can be witnesses in patients have an acute cereberovascular accident, a thorough neurologic examination is both prudent and necessary in patients with altered mental status. We would define thorough neurologic examination to encompass not only cranial nerve examinations and alert and oriented status but motor strength, sensation to pin prick, proprioception, dysdiadokinesis, deep tendon reflexes, evaluation for limb ataxia and asterixis as well as gait abnormalities. The patient’s baseline National Institute of Health’s Stroke Scale should also be documented.
Prehospital Care
Prehospital care is an essential aspect in the care of the patient with altered mental status. A primary survey should be performed on all these patients, and the patients should be rapidly screened for life threatening and easily reversible causes of altered mental status. In addition to the ABC’s, hypoglycemia should be assessed for with finger stick blood glucose in all patients with altered mental status. Also, patients with an exam concerning for opioid overdose (miotic pupils, respiratory depression) should be given naloxone if there is concern regarding their airway.
A good history is often the key to diagnosing the etiology of a patient’s altered mental status (has the greatest diagnostic value of tests done in the EC according to a study done by Kanich, et al), and pre hospital providers are in a special position to provide this useful information as the patients often cannot. By talking to witnesses at the scene, prehospital providers can often discover useful facts like whether the patient has been abusing illicit substances, whether the patient had a seizure, and a general history of what happened. Also, the scene of where the patient was found is often helpful as well, like whether there was evidence of violence at the scene, empty pill bottles to an overdose or drug paraphernalia that may suggest drug use.
A special concern to the prehospital provider is the violent or agitated patient. Two studies showed that the percentage of prehospital providers who had sustained an injury from a violent patient ranged from 25% to 67%. Thus, physical and chemical restraints are often needed to protect the patient and the providers. Special care must be used with physical restraints, as positional asphyxia has occurred in the prehospital setting.
Chemical Sedation in the Prehospital Setting Chemical sedation is often used in the prehospital setting to both protect the patient and pre hospital providers. A variety of medications have been used in this regard, and we will briefly discuss each.
Benzodiazepines
Benzodiazepines have a long history of use given their relatively good safety profile and efficacy. The two primary drugs that are used are midazolam and diazepam, with lorazepam being used less often in the prehospital setting because it is heat labile. Midazolam has a more rapid onset than rectal valium and is usually preferred, with intranasal midazolam gaining popularity.
Ketamine
The use of ketamine is becoming more common in the prehospital setting for the agitated patient. It does provide reliable sedation; one study followed 52 patients who received ketamine in the prehospital setting and 49 received adequate sedation. However, 5.7% did have significant respiratory depression. Two out of these 52 patients required endotracheal intubation. Another study of 49 patients who were given ketamine prehospital, 29% required intubation in the Emergency Department. Ketamine is used in the prehospital setting, but does come at a significant risk of intubation. Interestingly, these two studies did not demonstrate any increased rate of agitation once the sedation wore off. Ketamine is not indicated in patients with pre-existing psychosis because of the possibility of exacerbating psychosis, but it sometimes difficult for the care providers to determine the etiology of altered mental state at hand, and this contraindication is considered relative, not absolute.
Haloperidol
Intramuscular haloperidol has had longstanding use in the prehospital setting in the treatment of agitated patients, especially those whose agitation is thought to be secondary to psychiatric reasons. Special care should be taken in those who cardiac issues, as haloperidol does prolong the QTc and can provoke torsade de pointes.
Droperidol
Droperidol used to be used prolifically in the use of acute agitation. However, in 2001, the FDA placed a black box warning on droperidol due to its QTC prolongation that can provoke torsades de pointes. This caused its use to be severely diminished with many hospitals no longer carrying it on formulary. However, recent studies bring the black box warning into question. A randomized-controlled double blind trial of 144 patients showed that a single dose of droperidol was more effective than a single dose of midazolam in controlling agitation with no increase in adverse outcomes. Another study of 532 patients in the prehospital setting showed that use of droperidol as compared to haloperidol had no statistically increase in QTc, adverse events or use of adjunct sedating agents. Given this data, droperidol may be used more frequently in the prehospital setting.
Emergency Department Evaluation
The main purpose of the Emergency Department evaluation of altered mental status is to identify and treat the underlying cause. Like most ED patient’s, the evaluation begins with a primary survey and addressing the issues with Airway, Breathing and Circulation. The initial Emergency Department evaluation should focus on identifying life-threatening but easily treatable causes of altered mental status. Hence, all patients with altered mental status should get a finger stick blood sugar. Also, patients with respiratory depression and meiotic pupils should be treated with naloxone.
A common conundrum that faces Emergency Medicine clinicians is distinguishing the etiology of altered mental status from between delirium, psychiatric and dementia. For key clinical features that helps one distinguish between the three, please read the section on Epidemiology and Pathophysiology. However, as mentioned before, this can be quite challenging, especially when it comes to delirium in the elderly with miss rates between 57 to 83%. Another study showed that the sensitivity of the standard Emergency Department physician exam has a sensitivity of 35.3%.
To help make the diagnosis, a thorough ED evaluation is required. The results from a study by Kanich et al shows which part of the ED evaluation had the most diagnostic value in the chart below.
Data from Kanich W, Brady WJ, Huff JS, et al. Altered mental status: evaluation and etiology in the ED. Am J Emerg Med. 2002; 20(7): 613-17.
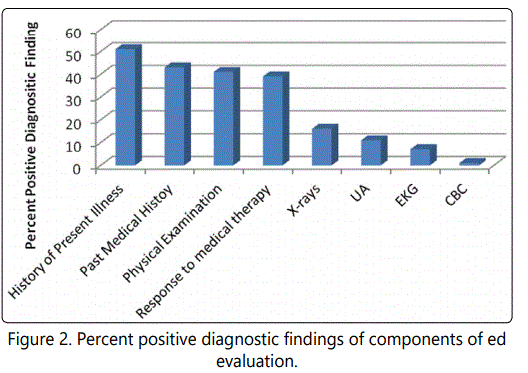
History
As Figure 2 shows, the history is by far the most important part in the evaluation of the ED patient with altered mental status. What makes obtaining a history particularly challenging in these patients is that the patient is often altered, and often cannot provide a coherent history themselves. This makes it extremely important to get collateral information from sources that include: EMS, family, friends and bystanders.
An important element history of all patients with altered mental status is a patient’s baseline mental status, especially in those patients with baseline cognitive dysfunction. This can help you distinguish if the patient’s current mental status is dementia or delerium. In addition, establishing a time course of the change in mentation is important. A slow, gradual decline suggests dementia while a more acute and fluctuating change in mental status suggest delirium as an etiology. It is also important to search for a history of substance abuse or diabetes can also help suggest a diagnosis. Also, a recent change/addition in medications can be a cause of altered mental status, particularly in the elderly.
Physical Examination
Before doing a physical examination, it is important to ensure that both the patient and providers will be safe during this process. In the agitated patient, this can be done by verbal de-escalation, assuming a non-aggressive posture, reducing stimuli int the room, and if needed medication and restraints. A complete physical examination can help the ED physician discover the underlying cause of altered mental status.
It is important to expeditedly obtain vital signs in all patients with altered mental status. Obtaining an accurate temperature is vital, and rectal temperatures will often provide useful information that will guide therapy. Mouth breathing in a non-cooperative patient can give falsesly low temperatures. A core temperature is essential and may lead the practitioner to uncover an infectious or toxic-metabolic causes of the patient’s symptoms. Unexplained abnormal vital sign are red flags and MUST be investigated.
Clinical Scoring Systems
Glasgow Coma Scale
The Glasgow Coma Scale (GCS) has long been used to assess the conscious state of an individual after trauma. For non-traumatic patients, it has been shown to correlate well with outcomes. A GCS [3-5]. has been shown to a 2-week rate of being awake of 14.8% as compared to GCS [6-8] that had an awake rate of 53.1%.
Grmec et al followed 286 patients who were admitted with nontraumatic coma and checked their initial Glasgow Coma Scale, Acute Physiology and Chronic Health Evaluation II (APACHE II) and the Mainz Emergency Evaluation System. Interestingly, they found that in terms of outcomes, all three were equally accurate at predicting the outcome of the coma and that the GCS was easiest to use.
Richmond Agitation-Sedation Score (RASS)
The RASS score is another scoring system that is used to assess the level of consciousness of a patient, which can be helpful in screening for delirium.

There was a study of ED physician’s using the RASS score to assess for delirium in 406 elderly patients. Delirium was defined as patients having a RASS score of other than zero. Using the RASS was 84.0% sensitive and 87.6% specific for delirium when compared to the evaluation by a psychiatrist. However, having a RASS of greater than one or less than negative one had a likelihood ratio of 19.4 for delirium.
Confusion Assessment Method (CAM)
The confusion assessment method is a standardized way to screen patients for delirium. A validation study by Inouye et al showed that at two independent sites, the sensitivities were 100% and 94% while the specificities were 95% and 90%. Other studies validate its accuracy in a variety of settings. A validation study performed with Emergency Department patients showed a sensitivity of 86%.The primary features of CAM is in the table below, and there are a variety of tools to assess these elements.
Adapted from Inouye SK, van Dyck CH, Alessi CA, Balkin S, Siegal AP, Horwitz RI. Clarifying confusion: the confusion assessment method. A new method for detection of delirium. Ann Intern Med. 1990; 113(12): 941-48.

Diagnosis of delirium using this tool requires presence of both features 1 and 2 and either 3 or 4. Despite its accuracy in diagnosing delirium, its practice has not gained popularity. This is primarily due to the fact that completing the CAM assessment can take up 10 minutes, which can be difficult to perform in a busy Emergency Department.
Mini-Mental State Examination (MMSE)
The MMSE is a widely used screening test that is used to screen for dementia, and has been taught to medical students for decades. As is well known, false positives can be found in patients who have low education or are physical infirm. False negatives can be found in patients who have high educational attainment. Multiple studies show that the MMSE is not useful in making the diagnosis of delirium, but that can be used as a screening tool using a cutoff of 24.
The main barrier to the routine use of the MMSE in the Emergency Department, that like the CAM, it can be time-consuming and take up to [7-10] minutes to complete.
Diagnostic Studies
Altered mental status is a clinical syndrome, thus the focus of the diagnostic studies should be used to diagnose the underlying cause of the altered mental status. In particular, patients with delirium require a more thorough work-up to tease out the etiology. The work-up should be tailored by the patients history, as Kanich et al showed that blood testing only resulted in a diagnosis of the etiology in 6% of pateints.1
All patients with altered mental status should get a finger stick blood sugar done as soon as possible. This is a cheap test that can rapidly identify a readily-reversible form of delirium. Patients with an unspecified etiology of their alteration of mental status should receive a more thorough evaluation including: Cell Blood Count, Basic Metabolic Panel, Urine Drug Screen, and Urinalysis (which can be helpful in 11% of patients). Other tests like Ammonia should be based on the history and physical. We will go into more detail on a few of the diagnostic studies.
Urine Drug Screen
The urine drug screen is a test that is probably over-ordered and rarely changes the course of a patient in the Emergency Department. Emergency Psychiatrists value urine drug screens as it allows insight into the etiology of the cognitive disturbance at hand, but is has little place in the main non-psychiatric algorithm for management. Eisen et al followed 133 patients in the Emergency Department and found that the results of the urine drug screen changed management in one of 133 patients. Another study of 392 patients in a psychiatric Emergency Department found that routine urine drug screens did not change disposition or affect length of stay. Interesting, only 20.8% of patients who denied drug use had positive screens Another study of 196 patients with acute psychosis showed that urine drug screens only The American College of Emergency Physicians has a Level III recommendation against the routine use of urine drug screens in the Emergency Department for the medical clearance of psychiatric patients. For the overdose patient, in a study of patients with a history of a drug overdose, the urine drug screen changed management in zero patients.
The utility of the urine drug screen is also limited by the many false negative and positives that complicate interpretation of the results. A list of the false positive and negatives are listed below in the table.
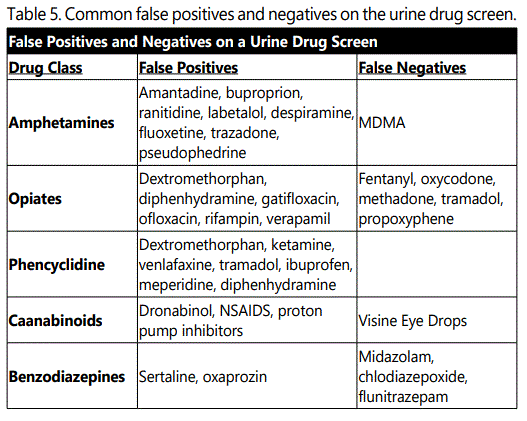
Computed Tomography of the Head (CT Head)
A CT of the head is key to the investigation of the cause of undifferentiated altered mental status. When CT scans were ordered in patients with altered mental status, an abnormal finding was found in 5% to 45%. In the study by Leong, the abnormal findings were: ischemic stroke (55%), 43% hemorrhagic stroke and 2% were intracranial masses. Patients with alcohol intoxication also commonly receive CT scans of the head because they have the perceived increased risk of intracranial hemorrhage. A recent study of 2,671 patients who were intoxicated and received CT scans of their heads showed that 1.9% had a positive scan which was identified as evidence of intracranial hemorrhage. Another study of 43 patients with overdose who received head CT’s, none had any relevant findings.
Lumbar Puncture
Lumbar puncture is a bread and butter Emergency Medicine procedure, and a recent study showed that it yields a diagnosis in 13.4% of the time in a community Emergency Department. Lumbar punctures are indicated when there is suspicion of meningitis or subarachnoid hemorrhage. As mentioned earlier, the absence of Kernig’s and Brudzinsky’s does not rule out bacterial meningitis, and neither does the jolt accentuation test. In the elderly, a recent study showed that the absence of a fever does not rule out bacterial meningitis. A high level of suspicion is needed to diagnose bacterial meningitis, and lumbar puncture is a valuable tool.
Treatment
The treatment of altered mental status is the treatment of the underlying cause. What follows is a brief discussion on the use of benzodiazepines and antipsychotics in delirium.
With the exception of the delirium due to stimulant use and alcohol/benzodiazepine withdrawal syndrome, the use of benzodiazepines in delirium is limited. A Cochrane Review of this topic in 2009 could not conclude that there was any benefit to using benzodiazepines in delirious patients that were not secondary to alcohol withdrawal or stimulant use. Benzodiazepines have also been known to worsen and provoke delirium.
The Use of Antipsychotics in Delirium
Antipsychotics are often used in the treatment of delirium. A review of 28 studies showed that ~75% of delirious patients improved with the use of antipsychotics. Another randomized controlled trial showed response rates for haloperidol, olanzapine and nondrug treatment groups being 87.5%, 82% and 31% respectively. This suggests that antipsychotics have a role in the treatment of delirium. Interestingly, a Cochrane review comparing low-dose haloperidol (dose <4.5 mg) to atypical antipsychotics in the treatment of delirium showed equal efficacy and no increase in extra pyramidal side effects. Antipsychotics should be used with caution in patients with Lewy Body Dementia and Parkinson’s disease as they can increase extra pyramidal symptoms.
Special Circumstances/Populations
The Elderly
The elderly are more prone to altered mental status given their decreased cognitive reserve. These patients have increased rates of dementia, which can complicate establishing whether they are at their baseline. Studies show that Emergency Department physicians missed the diagnosis of delirium between 57-83% of the time in this patient population. Often, Emergency Department providers mistakenly attribute a change in mental status for dementia, which in itself is a risk factor for delirium. Table 2 goes over the clinical differences between dementia and delirium. In particular, missing the diagnosis of delirium can be particularly harmful, as it is associated with increased mortality if they are discharged. This makes making the diagnosis extremely important, and getting a thorough history with collateral is often helpful.
The Psychiatric Patient
The psychiatric patient can be a difficult historian, and with possible underlying psychoses making obtaining a history challenging. Because of this and the underlying bias that the changes in mental status are psychiatric in nature, these patients are at increased risk of not being recognized as being delirious. It is especially important to recognize patient with dual diagnosis (mental illness and addiction), as withdrawal symptoms can exacerbate psychiatric symptoms and present as impaired cognition. It is important to not miss a diagnosis of delirium, as these patients have an increased mortality if admitted to a psychiatric facility. A thorough history and physical is needed in these patients with particular importance to obtaining collateral history. Table 2 highlights the key clinical differences between delirium and psychiatric disorder.
Controversies and Cutting Edge
Anti-NMDA receptor encephalitis
Anti-NMDA receptor encephalitis is particularly concerning because it can present with only psychiatric complaints. It is a new type of encephalitis that was first discovered in 1997, and a recent study of all cases of encephalitis over a 13 month period in England in 24 hospitals found that 4% were caused by Anti-NMDA receptor antibodies. The classic clinical history is that it begins with a viral prodrome, followed by primary psychiatric symptoms (psychosis, agitation and confusion) which then progresses to seizures, autonomic instability and hypoventilation. Interestingly, one study of 571 patients showed that 4% of patients with Anti-NMDA receptor encephalitis have purely psychiatric symptoms, which makes this diagnosis challenging. Anti-NMDA receptor encephalitis is associated with a teratoma in 60% of cases. Recent studies suggest that with removal of the tumor and/or immunosuppression, near 80% of patients will have near baseline function, but without treatment is almost always fatal. What makes this diagnosis even more difficult, that the only way to make this diagnosis is to do a lumbar puncture, but the routine lumbar puncture studies are often normal? The only way to diagnose it is to send an anti-NDMA receptor (NR1 and NR2) antibody test of cerebrospinal fluid to a laboratory in Spain. A high level of suspicion is needed to diagnose this entity.
EEG and micro EEG
The electroencephalogram (EEG) can be helpful in the diagnosis the etiology of altered mental status. A study of 82 patients with altered mental status in the Emergency Department, who received EEGs, showed that it assisted in diagnosis 51% of the time, but changed the management only 4% of the time. A key barrier to routinely having EEG’s available in the Emergency Department is the fact that EEG technicians and neurologists are not usually readily available. To overcome these challenges, the micro EEG has been developed. It is a new, miniaturized, wireless device that can be placed on the scalp by a technician with minimal training and transmits data to the neurologist to review. It has been shown to have the same diagnostic accuracy as a standard EEG. A recent study of 149 Emergency Department patients with altered mental status, the micro EEG had an abnormal finding in 93%, and had a change in diagnostic work up in 42%. However, compared to controls, it did not change length of stay.
New Screening Tools for Delirium
As mentioned earlier in this article, the Emergency Department physician often miss the diagnosis of Delirium, which often results in worse outcomes for patients. The current standard screening tools, like the Confusion Assessment Method (CAM) (the only tool validated in the Emergency Department setting) have challenges to being used routinely in the Emergency Department, namely, the length of the exam. Newer screening tools are in the process of being validated and may help in the future with screening for delirium in high risk patients. Other screening tools have been developed and used in the Emergency Department. This includes the CAM-ICU, CAM-ED, The Organic Brain Syndrome Scale, the Diagnostic and Statistical Manual criteria, the Delirium Rating Scale, and the NEECHAM Confusion Scale.
None of these scales have been validated in the Emergency Department setting. The CAM-ICU is the best studied of these scales in the Emergency Department setting, and was originally an adaptation of the CAM for the ICU setting. It is also a more rapid test than the CAM, making it more likely to be used in the Emergency Department. It is a tool, where at every question, if it is normal, the tool can be terminated and delirium ruled out. However, a validation study of 406 patients by Han et al showed that the sensitivity was only 58.3%. More work needs to be done to find a reliable screening tool in the Emergency Department for delirium.
Time- and Cost-Effective Strategies for diagnosing patients with altered mental status
1. Check oxygen saturation in all altered patients. This is a life-threatening and possible reversible cause of altered mental status that should not be missed. The test for it is simple, pulse oximetry and should be done on altered patients.
2. Obtain a finger stick blood sugar in all altered mental status patients. Hypoglycemia is a common and readily reversible form of altered mental status. Failure to diagnose this early can both cause the patient harm but also expose them to unnecessary testing.
3. Obtain collateral information. Altered patients often cannot provide a good history, and it is of utmost importance to get a good history to both provide a baseline for the patient as well as to give a time course of the altered mental status. This can help focus both your history and your work-up. For collateral, be sure to use family members, friends, primary care and prehospital providers.
4. Examine the pupils and respiratory rate. If the patient has a diminished respiratory rate and meiotic pupils, narcotic overdose should be high on your differential. Naloxone can be both a diagnostic and therapeutic intervention, saving the patient from a possibly expensive work-up.
5. Get a medication history. Medication changes are a common cause of delirium in the elderly, and pay special attention to medications that have anticholinergic properties.
Markers of Quality Care
Disposition
The disposition of a patient is influenced by the cause of the change in mental status.
Dementia- If the change is due to dementia, the patient can generally be discharged from the Emergency Department with any remaining work up completed by the patient’s primary care provider. However, patients with dementia may also have behavioral emergencies that are not well.
Delirium- Most patients with delirium should be admitted to the hospital to discover and treat the underlying cause of the delirium. There is, however, one, notable category of patients who are an exception to this rule: namely, those patients who have abused substances (both acute alcohol intoxication and drug intoxication). Patients should have frequent reassessments to assess clinical sobriety and whether they may safely be discharged from the Emergency Department.
Psychiatric Disorders- The disposition of a patient who is altered due to an exacerbation of their psychiatric issues should be made in consultation with a psychiatrist.
Summary
Altered mental status is a constellation of symptoms, not a disease entity. Its causes can be broken up into three main causes: psychiatric, dementia and delirium. A thorough history and physical is needed to differentiate between the three. Obtaining collateral information is particularly important as these patients often cannot provide a cogent history. Delirium is often missed, and missing it worsens patient’s outcomes. If a patient is found to have delirium, it is important to assess for the underlying precipitant of the delirium. Antipsychotics can be used for the treatment of delirium, but care should be used in those who have Lewy Body Dementia and Parkinsonism.
Eliminate all other factors, and the one which remains must be the truth- Sherlock Holmes, the Sign of Four, and Arthur Conan Doyle.
Case Conclusions
Case #1: The first patient was in florid Delirium Tremens. After 320mg of Valium and 320mg of phenobarbital, he was finally stable enough to go to the Intensive Care Unit.
Case #2: You find that the second patient was on Depakote, and his ammonia was 400! The patient had valproic acid induced hyper ammonemia. With discontinuation of the Depakote, the patient’s mental status improved in a few days and he was discharged.
Case #3: The third patient had a normal lumbar puncture, but you sent the studies to Spain to rule out anti-NMDA receptor encephalitis. It came back positive and the patient was started on immunosuppressant agents and her previously undiscovered teratoma was removed. Three weeks later she was discharged near her baseline.
References