Research Article
Cord Blood Haptoglobin as an Indicator for Early diagnosis of Neonatal Jaundice
Faculty of Medicine for Girls, Al-Azhar University, Cairo, Egypt
*Corresponding author: Safaa EL Meneza, Professor, Faculty of Medicine for Girls, Al-Azhar University, Cairo, Egypt, E-mail: safaa5@hotmail.com
Received: February 13, 2019 Accepted: February 25, 2019 Published: March 12, 2019
Citation: Ismail KA, Gharib AF, Farghly AH, et al. Detection of Plasmodium Antigen in Feverish Patients. Int J Hematol Blood Res. 2019; 1(1): 5-9. doi: 10.18689/ijhbr-1000102
Copyright: © 2019 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Early identification of newborns at risk of developing severe hyperbilirubinemia, continue to be a problem in neonatology.
Objective: Study the role of cord blood haptoglobin in prediction of hyperbilirubinemia in healthy full term newborn infants.
Patient and Methods: This prospective study conducted in the delivery room and neonatal intensive care unit (NICU) of Alzahraa University hospital and Hurghada general hospital. 75 healthy full term newborn infants were included. Complete blood count (CBC), serum bilirubin (total and direct), maternal & neonatal blood group and cord blood haptoglobin was estimated at birth and on fifth day postnatal age. The studied neonates distributed into 3 zones (low, intermediate and high risk zones) according to their TSB at first and fifth day.
Results: 28% of cases needed treatment for hyperbilirubinemia. Highly statistically significant difference between neonates who needed treatment with a phototherapy and those didnʼt need regarding to first day haptoglobin; P value=0.00. Haptoglobin increased significantly on the fifth day of life. Significant negative correlation was found between haptoglobin and TSB in cord blood, and on fifth day of life. Also between cord blood haptoglobin and fifth day TSB with p-value=0.00.
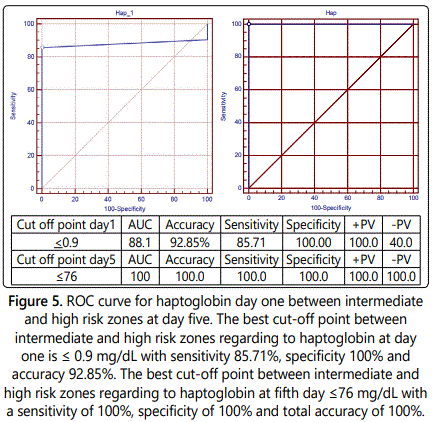
Haptoglobin was significantly different between low risk, intermediate and high risk zones with p-value=0.00. The best cut-off point between low and intermediate risk zones at first day was ≤ 1 mg/dL with sensitivity of 100%, specificity of 86.54% and accuracy of 78.27% and between intermediate and high risk zones was ≤ 0.9 mg/dL with sensitivity of 85.71%, specificity 100% and accuracy of 92.85%.
Conclusion: We conclude that the haptoglobin value from the blood of umbilical cord can be used as predictor indicator for future occurrence of jaundice in full term newborns.
Keywords: Newborn infants; Haptoglobin; Neonatal jaundice; Hyperbilirubinemia.
Abbreviations: TSB: Total serum bilirubin; NICU: Neonatal intensive care unit; CBC: Complete blood count; Hb-Hp: Haemoglobin-Haptoglobin; SGA & LGA: Small for gestational age and Large for gestational age; UC: Umbilical Cored.
Introduction
Neonatal jaundice is widespread problem in newborn infants and is often the cause for a parent to consult a health visitor or physicians. It is recognized that up to 40 percent of breastfed infants have jaundiced at 14 days of age and need investigations [1]. Serum bilirubin levels may extremely elevated and lead to death or lifelong neurologic sequelae in infants who survive [2]. Therefore, an early recognition of newborns at hazard of developing severe hyperbilirubinemia, persist to be a dilemma in neonatology.
Hyperbilirubinemia in the first days of life can be induced due to increased heme catabolism. Haemoglobin attaches instantly with haptoglobin, a serum glycoprotein, and forms a stable haemoglobin-haptoglobin (Hb-Hp) molecule. Haptoglobin has been suggested to be more beneficial than the other protein markers to measure acuteness of hemolysis [3].
Hypothesis
Can we use cord blood haptoglobin as an early marker for hyperbilirubinemia in health full term newborn infants?
Objectives
Study the role of cord blood haptoglobin in prediction of hyperbilirubinemia in healthy full term newborn infants
The Aim of our Work
1. To measure haptoglobin and bilirubin in the cord blood.
2. To measure haptoglobin and bilirubin in the fifth day of life.
3. To correlate the need for treatment of hyperbilirubinemia with the mean values of haptoglobin in cord blood and on the fifth day of life.
Patients and Methods
A prospective study was conducted in the delivery room of gynecology and obstetrics as well as neonatal intensive care unit (NICU) of Alzahraa University Hospital and Hurghada General Hospital.
The study included100 healthy full term newborn infant with gestational age between 37-42 weeks and exclude the preterm <37 weeksʼ gestational age, SGA & LGA, cases with congenital malformations, suspected or diagnosed neonatal sepsis, respiratory distress, inborn error of metabolism, and newborn infants who were unable to initiate or maintain oral feedings within 3 hr after birth. Only 75 newborn infants completed the study as 25 newborn infants did not show up after discharge.
The infants were categorized according to their further need for treatment and total serum bilirubin levels into 3 group zones (low risk zone, intermediate risk zone, and high risk zone), we used age specific total serum bilirubin level centile [4,5].
All patients included in the study were subjected to adequate history taking including antenatal –natal–postnatal history, family history of jaundice in the siblings, family history of G6P deficiency and type of feeding as well as thorough clinical examination. Estimation of haptoglobin at birth from cord blood and on fifth day post-natalage from the serum using radial immune diffusion technique and, also we measured serum bilirubin (total and direct), as well as complete CBC, maternal and neonatal blood group were done.
The study was approved by the ethical committee of pediatrics department and faculty of medicine for girls at Al-Azhar University. An informed consent was taken from all parents of the studied infant before inclusion in the study.
Statistical methods
The data were collected, revised, coded and entered to the Statistical Package for Social Sciences (SPSS) version 17.
Results
The results are shown in tables 1 to 5 and figures 1 to 5.
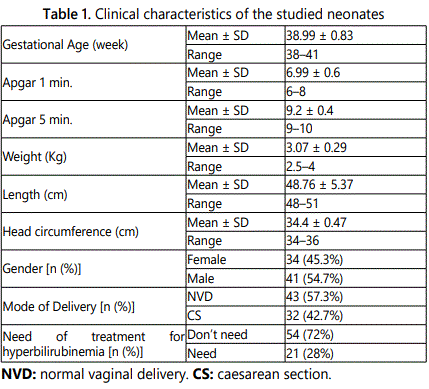
Table 1 shows that 41 of the studied neonates were males with a percent of 54.7% and 34 (45.3%) were females. 43 (57.3%). They were delivered with NVD and 32 (42.7%) with CS. (28%) of the studied neonates needed admission to NICU to be treated with a phototherapy and 54 (72%) didnʼt need a treatment.
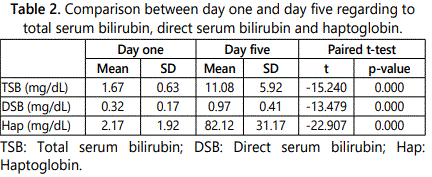
Table 2 shows that there was a highly statistically significant increase in the value of TSB, DSB and haptoglobin in day five than day one.
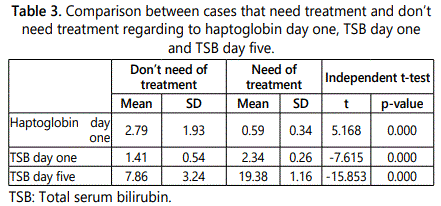
Table 3 shows that there was a highly statistically significant difference between a group of the studied neonates needed admission to NICU to be treated with a phototherapy and a group of the studied neonates didnʼt need of treatment regarding to haptoglobin at day one, TSB at day one and TSB at day five with p-value = 0.00.
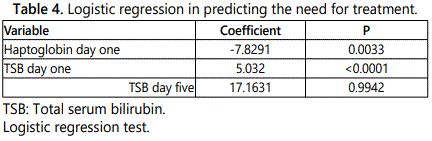
Table 4 shows that there was significant association between haptoglobin at day one and need for treatment at day five, highly significant association between TSB at day one and need for treatment at day five, while there was no significant association between TSB at day five and need for treatment at day five.
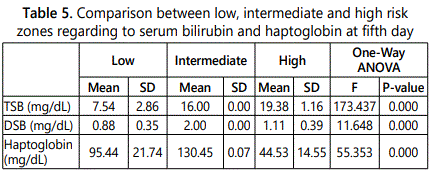
Table 5 shows that there was a highly statistically significant difference between the three groups regarding to TSB, DSB and haptoglobin at the fifth day with p-value=0.00.
Discussions
Our study included 75 healthy full term neonates, their gestational ages ranged between 38 and 42 completed weeks with mean ± SD of 38.99 ± 0.83. They were further classified according to development of hyperbilirubinemia and to risk [4,5]. During the first day all our cases was in low risk zone as their TSB values were less than 5 mg/dL. On the fifth day 69.3%, of the studied neonates were in low risk zone, while 2.7% were in intermediate risk zone and 28% were in the high risk zone and needed admission to treat their jaundice by phototherapy.
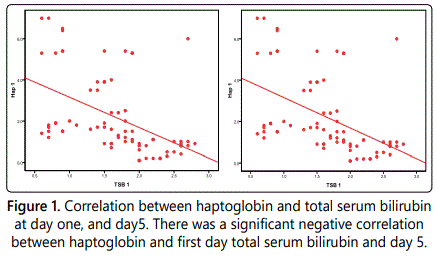
In our study there was a highly statistically significant association between total serum bilirubin and haptoglobin in the umbilical cord blood at day one and at day five. Also there was significant association between haptoglobin at day one and need for treatment at day five. The mean values of serum haptoglobin was significantly lower at the first day among studied neonates who needed treatment with a phototherapy and there was significant association between haptoglobin mean values at day one and need for treatment at day five. Also there was significant association between TSB at day one and need for treatment at day 5.
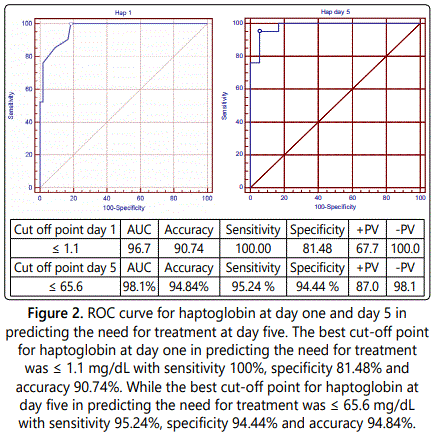
The best cut-off point for haptoglobin at day one in predicting the need for treatment at day five is ≤ 1.1 mg/dL with sensitivity of 95.24%, specificity of 94.44% and accuracy of 94.84%, and the best cut-off point for haptoglobin at day five in predicting the need for treatment is ≤ 65.6 mg/dL with sensitivity of 95.24%, specificity of 94.44% and accuracy of 94.84%.
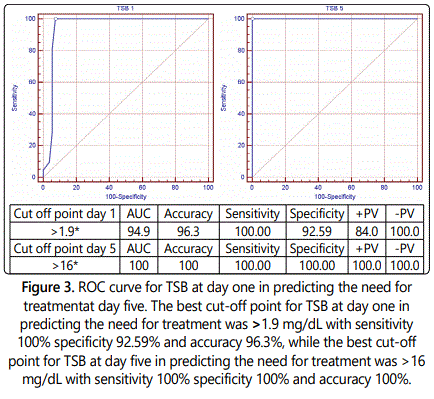
There was a highly statistically significant increase in the value of TSB and direct serum bilirubin (DSB) in day five than day one. Our study showed that the best cut-off point for umbilical cord TSB at day one in predicting the need for treatment was >1.9 mg/dL with sensitivity 100%, specificity 92.59% and accuracy 96.3%, and the best cut-off point for TSB at day five in predicting the need for treatment was >16 mg/dL with sensitivity 100%, specificity 100% and accuracy 100%. Significant associations to the study done by Nahar Z et al. and Ipek IO et al. [6,7]. Knowledge of low risk of hyperbilirubinemia in a newborn could encourage the physicians in the decision of early postnatal discharge.
Mean value ± SD of UC haptoglobin level measured by radial immunodiffusion was (2.17± 1.92), while fifth day mean value ± SD was (82.12 ± 31.17). Our results are more or less similar to the study done by Cakmak et al. and those of Chavez-Bueno et al. [8,9]. Haptoglobin was found to be more useful than the other protein markers to evaluate seriousness of hemolysis as manifested hypo or an haptoglobin is associated of hemolysis [8].
In our study there was significant increase in the value of haptoglobin in day five than day one. This may be explained by immaturity of neonatal liver as haptoglobin is synthesized predominately by the hepatocyte [10]. Moreover, there is normal physiological increase in the haptoglobin with increase of postnatal age as seen in the study of Chavez-Bueno et al. [9], they concluded that both gestational and postnatal age should be considered when interpreting concentrations of haptoglobin.
In our study there was highly statistically significant negative correlation between cord blood haptoglobin day one and day five TSB (p=0.000). The same results were reported by Cakmak et al. [8], so this inverse relationship can help us in detecting the neonates at risk of developing hyperbilirubinemia by detecting the level of serum haptoglobin at day one. These findings indicate that it may be possible to predict neonatal jaundice with the cord blood haptoglobin and it is a useful tool to predict hyperbilirubinemia in healthy term newborns.
Also haptoglobin mean values was not statistically different in relation to newborn infants blood groups, on the contrary infants of B negative mothers showed elevation of mean values of haptoglobin on the fifth day of life.
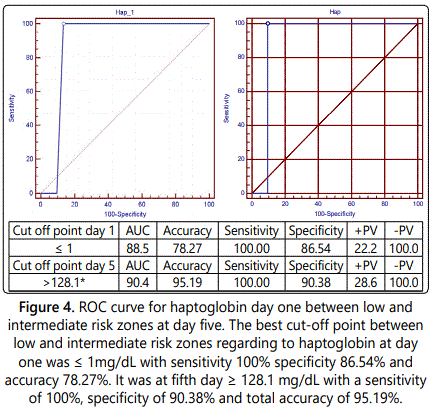
We found highly statistically significant difference between low risk, intermediate and high risk zones regarding to TSB, DSB and haptoglobin. The best cut-off point between low and intermediate risk zones regarding to haptoglobin at fifth day was found >128.1 mg/dL with a sensitivity of 100%, specificity of 90.38% and with accuracy of 95.19% and between intermediate and high risk zones ≤ 76 mg/dL with a sensitivity of 100%, specificity of 100% and with total accuracy of 100%. Therefore, at 5th day of life, readings <128.1 mg/dL can be considered as mild hyperbilirubinemia, >128.1 mg/dL can be considered as moderate hyperbilirubinemia while ≤ 76 mg/dL can be considered as sever hyperbilirubinemia.
The use of UC blood, is safe, easy practical, furthermore, it keeps the baby free from pain and, most importantly, the data are available immediately after birth. So, high-risk newborn infant might be detected with high certainty, even if parents would like to leave the hospital within the first postnatal hours [11,12].
We conclude that the haptoglobin value from the umbilical cord can be used as predictor indicator for future occurrence of jaundice in healthy full term newborns. The use of UC blood, is safe, easy practical, furthermore, it keeps the baby free from pain and, most importantly, the data are available immediately after birth.
Recommendation
Quantification of cord blood haptoglobin can be used as a method to predict in advance the healthy term neonate who will develop hyperbilirubinemia as determine by low cord of haptoglobin
Conflicts of Interest
The authors declare no conflicts of interest.
Ethics Statement
The study was approved by the ethical committee of pediatrics department and Faculty of medicine for girls at Al-Azhar University. An informed consent was taken from all parents of the studied infant before inclusion in the study.
References
- Paul SP, Hall V, Taylor TM. Prolonged jaundice in neonates. Pract Midwife. 2012; 15(6): 14-17.
- Ruud Hansen TW. Phototherapy for neonatal jaundice--therapeutic effects on more than one level? Semin Perinatol. 2010; 34(3): 231-234. doi: 10.1053/j.semperi.2010.02.008
- Delanghe JR, Langlois MR. Hemopoexin: A review of biological aspects and the role in laboratory medicine. Clin Chim Acta. 2001; 312(1-2): 13-23.
- Bhutani VK, Johnson L, Sivieri EM. Predictive ability of a predischarge hourspecific serum bilirubin for sub-sequent significant hyperbilirubinemia inhealthy termand near-term newborns. Pediatrics. 1999; 103(1): 6-14.
- American Academy of Pediatrics Subcommittee on Hyperbilirubinemia. Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics. 2004; 114(1): 297-316.
- Nahar Z, Shahidullah Md, Mannan A, Dey SK, Mitra U, Selimuzzaman SM. The Value of Umbilical Cord Blood Bilirubin Measurement in Predicting the Development of Significant Hyperbilirubinemia in Healthy Newborn. Bangladesh J Child Health. 2009; 33(2): 50-54.
- Ipek IO, Bozaykut A, Cagril SC, Sezer RG. Does cord blood bilirubin level help the physician in the decision of early postnatal discharge? J Matern Fetal Neonatal Med. 2012; 25(8): 1375-1378. doi: 10.3109/14767058.2011.636089
- Cakmak A, Calik M, Atas A, Hirfanoglu I, Erel O. Can Haptoglobin be an Indicator for the Early Diagnosis of Neonatal Jaundice? J Clin Lab Anal. 2008; 22(6): 409-414. doi: 10.1002/jcla.20279
- Chavez-Bueno S, Beasley JA, Goldbeck JM, et al. Haptoglobin concentrations in preterm and term newborns. J Perinatol. 2011; 31(7): 500-503. doi: 10.1038/jp.2010.197
- Wang Y, Kinzie E, Berger FG, Lim SK, Baumann H. Haptoglobin, an inflammation-inducible plasma protein. Redox Rep. 2001; 6(6): 379-385. doi: 10.1179/135100001101536580
- Knupfer M, Pulzer F, Gebauer C, Robel-Tillig E, Vogtmann C. Predictive value of umbilical cord blood bilirubin for postnatal hyper bilirubinaemia. Acta Paediatr. 2005; 94(5): 581-587.
- ELMeneza S. Egyptian Neonatal Safety Standards-2014. 2019.


