Mini-Review Article
An Overview on Inflammatory Biomarkers for Diabetes Mellitus
1Department of Biotechnology, MIET Meerut, Uttar Pradesh, India
2Department of Botany, SILB Solan, Himachal Pradesh, India
*Corresponding author: Ritika Gupta, Department of Biotechnology, MIET Meerut, Uttar Pradesh, India, E-mail: guptaritika.27@rediffmail.com
Received: December 17, 2018 Accepted: January 2, 2019 Published: January 9, 2019
Citation: Gupta R, Soni S. An Overview on Inflammatory Biomarkers for Diabetes Mellitus. Madridge J Diabetes. 2019; 3(1): 63-65.doi: 10.18689/mjd-1000112
Copyright: © 2019 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Diabetes mellitus is a very complex disease affecting almost every tissue and organ system, with heterogeneous etiology characterized by insulin resistance. Obesity, sedentary lifestyle and unhealthy diet are well-known risk factors for development of type 2 diabetes mellitus (T2DM). Understanding pathological mechanisms is imperative to prevent and treat the disease. Therefore, identification of specific biomarkers for T2DM is of great interest. Biomarkers are the biological molecules which play a vital role in conducting clinical trials, for screening and risk assessment before diagnosis and are helpful for monitoring recurrent diseases. Developing and characterizing an effective biomarker is arduous. To know the root cause and the effect in the pathogenesis of disease are some of the major challenges in the field of biomarkers. Several approaches including proteomics, genomics, metabolomics and transcriptomics are being applied for early detection of T2DM and further devising new therapies to treat it. The emphasis of the present review is to identify non-genetic and genetic biomarkers through the application of novel methodologies that would predict hyperglycemia and incident T2DM.
Keywords: Diabetes Mellitus; Biomarkers; Hyperglycemia; T2DM; Obesity; Insulin.
Introduction
Diabetes mellitus
Diabetes Mellitus (DM) is a complex multi factorial metabolic disorder with disordered
metabolism and hyperglycemia prevailing world wide. Some risk factors contributing to
DM are smoking, alcohol, obesity, diet, overweight, vascular or cardiovascular disease,
level of physical activity, hormones and some medical treatments. Exercise and diet can
improve the health habits further reducing the risk of developing diabetes. Type 1 and
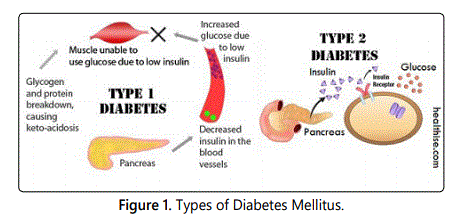
type 2 are the two most important types of DM (figure 1). Type 1 DM commonly referred
as juvenile diabetes and known as insulin dependent diabetes mellitus (IDDM) in which
pancreas is unable to produce insulin due to autoimmune β-cell destruction. Type 2 DM,
an adult-onset diabetes is known as non insulin dependent diabetes mellitus (NIDDM) in
which body tissues and cells are unable to respond properly to the action of insulin [1].
Genetic and metabolic abnormalities are some other abnormalities produced in response
to insulin action and secretion. Type 2 DM usually occurs in adulthood and develops
more with the age and sometimes it is also observed in children and some adolescents
having obesity [2]. Over the past two decades, worldwide prevalence of diabetes mellitus
has risen and is considered as one of the most widely occurring human ailments.
According to survey led by some health agencies like World Health Organization (WHO)
and International Diabetes Federation (IDF), diabetes becomes an epidemic which is not
controlled and is sixth leading cause of human mortality and morbidity globally.
Biomarkers
Biomarker is a substance which is used as an indicator for
pathological state of disease and a characteristic that is estimated
and evaluated for normal, pathological, and pharmacologic
responses to a therapeutic intervention. In 21st century, they
have gained tremendous scientific momentum. They are the
biological molecule found in blood, other bodily fluids, or tissue
which may have any clinical value and can be the component of
interest in the practice of medicine and represents a sign of a
normal or abnormal process or of a condition or disease. A
biomarker may be used to see how well the body responds to a
treatment for a disease or condition. Moreover, it provides high-throughput platforms, adequate analytic performance, carries
therapeutic implications and assesses progression thus
improving the treatment strategy. Biomarkers may reflect the
presence and severity of hyperglycemia (i.e. diabetes itself), or
the presence and severity of the vascular complications of
diabetes. Biomarkers can play an imperative role in laboratory
for drug discovery, diagnosing, classification, and grading the
severity of disease in both laboratory and clinical settings. They
have a potential for understanding the relationship between
disease and health. Some of the diseases are as of protein
biomarkers are, for example, cancer, diabetes, and cardiovascular
and neurological diseases. The protein biomarkers are very
useful for diagnosis and prognosis of the asymptomatic phase
before the development of acute and chronic diseases such as
diabetes, various forms of cancer, and other syndromes.
Inflammatory biomarkers for diabetes
Biomarkers for monitoring diabetes and associated micro and macro vascular complications can be broadly classified as
follows: genomic (single-nucleotide polymorphisms), transcriptomic
(mRNA), proteomic (proteins and glycoproteins), metabolites
(lipids, sugars, amino acids), markers of subclinical disease
(arterial function, aortic plaque burden) and metabolic end-products (urinary proteins). Further research is needed to
identify novel biomarkers for progression monitoring and for
incremental improvement in T2DM diagnosis. In each stage
of T2DM management, biomarkers play an imperative role.
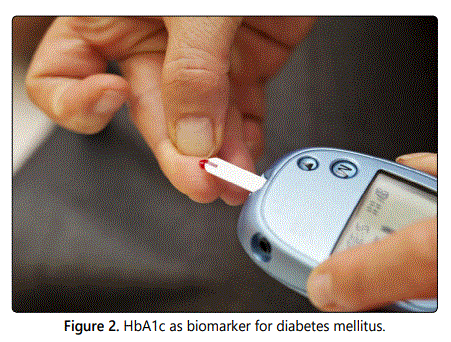
Plasma glucose (A1C) is one of the most common biochemical
parameters or biomarkers based on which T2DM diagnosis is
done (figure 2). Type 1 diabetes (T1D) is caused by T-cell
abnormalities further leading to the destruction of pancreatic
islets while in type 2 diabetes, activation of monocytes and
inflammation are responsible for insulin resistance resulting
in the loss of insulin secretory function by islet cells. Various
studies have suggested the co-relation between inflammation
and diabetes demonstrating that inflammatory markers can be used to refine T2DM risk prediction. Cytokines are those
groups of proteins which act as immune mediators and
regulators and are expressed by several cell types. Insulin
resistance has been associated with decreased production of
anti-inflammatory mediators (IL-4 and IL-10) and abnormal
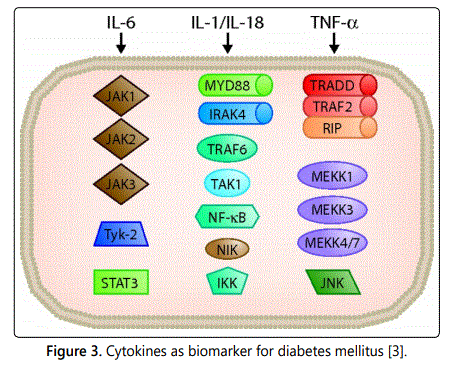
secretion of pro inflammatory cytokines (tumor necrosis
factor-α (TNF-α) and Interleukin-6 (IL-6)) (figure 3). IL-1 could
promote beta-cell destruction and alter insulin sensitivity.
Interleukin-6 (IL-6) is a pleiotropic pro inflammatory cytokine,
induces the development of insulin resistance by inducing the
expression of SOCS-3 leading to the impairment of
phosphorylation of insulin receptor and insulin receptor
substrate-1. CRP (C-reactive protein) is sensitive and systemic
biomarker for inflammation and is synthesized by liver. Recent
reports have suggested that IL-6 and CRP are associated with
T2DM.
Literature Review
Leinonen et al. [4] reported urinary 8-hydroxy-2'- deoxyguanosine (8-OHdG) as a sensitive biomarker in NIDDM patients. They investigated oxidative DNA damage and oxidative stress by urinary 8-OHdG assessments in the urine samples. They further determined increased level of 8-OHdG in NIDDM patients when compared to non-diabetic control subjects by screening 24 hr urinary excretion [4]. Tso et al. [5] investigated serum adipocyte fatty acid-binding protein (A-FABP) levels to predict the development of T2DM. They reported that serum A-FABP levels were higher in glucose intolerant patients. Lui et al. 2013 systemically reviewed the association of IL-6 and CRP in diabetes mellitus by conducting meta-analysis. They explored numerous electronic databases and a systematic literature search was performed. They further demonstrated that chronic inflammation is a predictor of type 2 diabetes development. Ghosh P et al. [6] established an enzyme linked immune sorbent assay (ELISA) to measure serum/plasma glycated human CD59 and evaluated its potential as a diabetes biomarker. They conducted a clinical trial and found that GCD59 was significantly higher in individuals with than in individual without diabetes [6]. Takada T et al. [7] reported increased level of an up regulated protein known as monomeric α2-macroglobulin in diabetic patients. They purified the protein through highly efficient strategy from diabetic and control (non-diabetic) serum samples. SDSPAGE was used to fractionate the extracted sera and further the isolated protein bands were analyzed by mass spectrometry. They concluded that monomeric α2-macroglobulin can be used as a potential biomarker in many diabetic subjects [7]. Molnos et al. [8] showed pair wise metabolite (valine to phosphatidylcholine acyl-alkyl C32:2) ratio to be associated with an increased risk of type 2 diabetes. They conducted a clinical trial on 130 healthy members and examined the association of metabolite levels on those patients. They observed dynamic changes in metabolite levels after arginine, glucose and glucagon-like peptide-1 (GLP-1) stimulation [8].
Conclusion
Diabetes is a global endemic with rapidly increasing prevalence in both developing and developed countries.T2DM is a chronic, progressive disease that traditionally is characterized by insulin resistance. Currently, the diagnosis and progression of diabetes rely predominately on glycemic indices. Biomarkers play an integral part in conducting clinical trials and treating patients. However, much research, prospectively planned and with clear treatment implications, is needed before wear rive at truly "personalized" diabetes care.
References