Case Report
Edentulous Ridges treatment with a CAD/CAM-Milled Screw-Retained Framework and possibility of Individually aligned Screw Channels: A Clinical Case Report and Review
1Division of Prosthodontics, İstanbul Okan University, Turkey
2Dental plus Implant Clinics, Bakırkoy, Istanbul, Turkey
*Corresponding author: Simge Taşın, Division of Prosthodontics, Istanbul Okan University, Faculty of Dentistry, Gülbahar Mahallesi, Istanbul, Turkey, Tel: +902166771630, Fax: +902122726347, E-mail: simgetasin@gmail.com
Received: April 4, 2019 Accepted: May 3, 2019 Published: May 13, 2019
Citation: Taşın S, Üşümez A. Edentulous Ridges treatment with a CAD/CAM-Milled Screw-Retained Framework and possibility of Individually aligned Screw Channels: A Clinical Case Report and Review. Madridge J Dent Oral Surg. 2018; 4(1): 91-95. doi: 10.18689/mjdl-1000121
Copyright: © 2019 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Aim and background: To describe the treatment of a 55-year-old edentulous female patient using computer-aided design and computer-aided manufacturing (CAD/CAM)-milled cobalt chromium (Co-Cr) frameworks infixed complete dentures (FCDs) with a recently introduced possibility of angling the screw channels up to 20 degrees.
Case report: Six months after implants placement, implant level impressions were taken from the mandibula and maxilla with individual trays using the open custom tray technique. The verification indexes for fixed complete dentures (FCDs) were fabricated with resin patterns. The master casts were scanned with an extraoral laser scanner and the frameworks were computerized and designed with reference to the verification indexes. The frameworks were fabricated from a Co-Cr alloy using the CAD/CAM-milled fabrication method and the tooth set-up was performed over each framework using prefabricated resin teeth. The FCDs were checked clinically and the prosthetic screws were tightened at the implant level without the interposition of an abutment.
Results: Screw-retained FCDs have been successfully utilized to rehabilitate completely edentulous ridges.
Conclusion: Connecting the superstructure to the implant using a screw, without the interposition of an abutment, may reduce inaccuracy in laboratory procedures and increase the aesthetic outcome.
Keywords: Edentulism; Dental implants; Fixed complete dentures; Dental implant-superstructure connection.
Introduction
The use of fixed complete dentures (FCDs) in rehabilitation is gaining popularity among oral care professionals [1,2]. The concept of FCDs can be produced in different type designs. Normally made from various kinds of noble materials, FCDs can be generally defined as a denture, comprised of a substructure of metal covered with artificial teeth and gingiva-colored acrylic resin, screwed onto diverse implants. In other words, it is a fixed denture from the patientʼs point of view, but it can be removed by a professional if necessary. FCDs can include a variable number of implants, although ideally the largest possible number should be used [3].
FCDs have helped achieve a high quality of life among edentulous patients. They provide functional, esthetic, and psychological advantages, especially compared to conventional complete dentures [1,2]. Additionally, FCDs compensate for lost tissue in cases and ensure acceptable esthetics and occlusal morphology [4,5]. However, the use of FCD has also been associated with a number of mechanical, phonetic, and infectious–inflammatory complications.
One of the most critical goals in the prosthetic phase of implant treatment is the fabrication of passively fitting superstructures [6]. At present, superstructure fabrication techniques have inherent flaws that lead to geometric and/or dimensional misfit, such as prosthetic complications associated with screw-retained prostheses [7-9]. New manufacturing techniques are being developed to address superstructure compatibility issues. Computer-aided design and computer-aided manufacturing (CAD/CAM)-milled systems have become the mainstream manufacturing technique of FCD frameworks or superstructures for dental implants [10].
FCDs can be connected to implant fixtures in two ways: 1) by placing a screw-retained abutment onto the dental implant and fixing it with the FCD retaining screw; and 2) by directly screwing the superstructure to the implant [11]. Angled screw-retained abutment options can compensate for misaligned implants to a certain degree; however, in complex situations, angled abutments do not produce a natural-looking emergence and can thus adversely affect esthetics [11].
A systematic review has also identified some major problems with the FCDs [12]. Technical complications have been reported around 60–80% due to implant components and prosthetic superstructures, but fixture failure was reported in less than 1% of in vivo cases [12]. According to this review, the presence of additional components between the implant and the superstructure can complicate the system and thus increase the rate of medical complications.
One example of an FCD was introduced—namely, a CAD/CAM-milled framework made of titanium or cobalt chromium (Co–Cr) alloy, with screw channels that can be individually aligned up to 20 degrees. The angulation allows the screw channels to be angled into the lingual side, making it possible to create multi-unit FCDs and achieve satisfactory esthetics at the same time. Additionally, this technology is compatible with various implant systems [11].
Few case reports or clinical studies have included milled Co-Cr screw-retained frameworks. This report describes the management of an edentulous patient using a milled Co-Cr FCD built on an implant system.
Case Report
A 55-year-old woman whose remaining teeth were deemed hopeless due to severe chronic periodontal disease agreed to undergo maxilla mandibular rehabilitation (Figures 1 and 2). The patient chose to be treated with FCDs on four to six dental implants. Other treatment options were offered to her included maxillary and mandibular complete dentures and implant-supported over dentures.
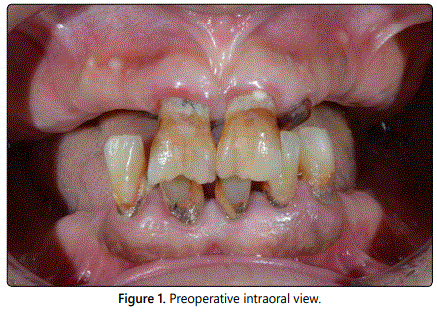
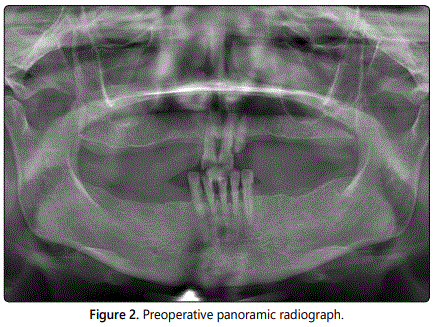
Following extraction of the remaining teeth, four implants (Bio Horizons Implant Systems Inc, Birmingham, AL, USA) were placed in the maxilla and six implants (Bio Horizons Implant Systems Inc, Birmingham, AL, USA) were placed in the mandibula following the extraction of teeth at the same appointment (Figure 3) under general anesthesia. No graft application or other advanced surgical procedures were performed during surgery. After an osseointegration period of 6 months without functional loading and with the implants submerged at the sub gingival level, the second stage of the surgery was performed under local anesthesia; the closure screws were removed and healing abutments were placed.
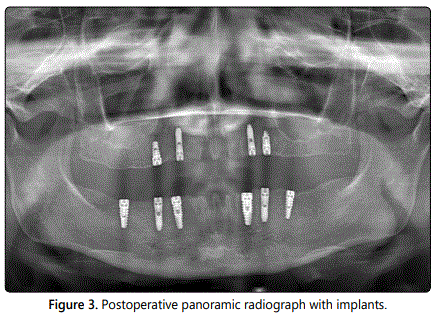
The prosthodontic treatment protocol was initiated two weeks later, after the soft tissue had healed. The healing abutments were removed and impression copings were placed. The transfer copings were splinted with pattern resin before the impressions were taken. Implant-level impressions were then made using the open custom tray technique, with individual trays and A-silicone (Variotime, Kulzer GmbH, Hanau, Germany), and implant analogs were connected to the copings in the polymerized impressions. Soft tissue moulage gingival replication material (Soft tissue Moulage TM, Kerr Orange, CA, USA) was placed into the impression to mimic the maxilla and mandibula. Soft tissue working models were fabricated with type-III dental stone (Moldano, Kulzer GmbH, Hanau, Germany).
The centric relation records were generated with record bases, occlusal rims, and inter occlusal bite registration material; the occlusal vertical dimension was fixed. Esthetic and phonetic factors were considered when establishing the position of the maxilla mandibular anterior teeth. The verification indexes for FCDs were fabricated with resin patterns, which had in turn been made using a diagnostic denture wax-up as a guide. The indexes were tried intra orally to confirm the integrity of the master cast (Figure 4).
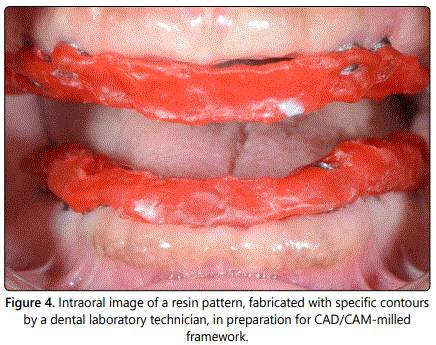
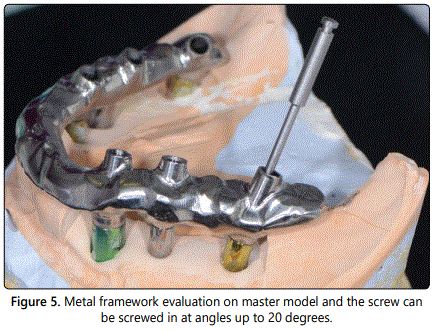
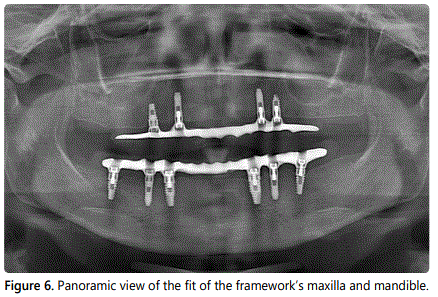
The master casts were scanned with an extra oral laser scanner (3Shape, Kulzer GmbH, Hanau, Germany) and the FCD frame works were computerized and designed with reference to the verification indexes. The frameworks were fabricated in the dental laboratory from a Co-Cr alloy using the CAD/CAM-milled fabrication method. They were checked intra orally, as well as on the master model, to confirm that they were passively seated over the implants (Figure 5). The clinician checked the adjustment of the frameworks by means of selective pressure, the single-screw test, and panoramic radiograph (Figure 6). The tooth set-up was performed over each FCD framework using prefabricated resin teeth (Vitapan, H Rauter GmbH & Co, Bad Sackingen, Germany). The centric relation, occlusal plane, vertical dimension of occlusion, and phonetics were evaluated clinically; and the midline was verified. The patientʼs acceptance of the esthetics was obtained at the trial insertion appointments.
The FCDs were constructed in the dental laboratory using heat-curing acrylic resin, and adjusted to maintain occlusal point contacts in centric relation, canine guidance for lateral excursions, and anterior guidance for protrusion. Before finalizing the process, the FCDs were checked clinically for final fit between the denture base and mucosa, as well as esthetics, phonetics, occlusal relation, and stability. The prosthetic screws were tightened according to the manufacturerʼs recommendations, and access holes were sealed with a Teflon band and a composite resin (Filtek Z250, 3M ESPE, St Paul, MN, USA) (Figure 7). The patient received verbal and visual explanations on how to use, clean, and maintain her dentures, as well as essential instructions in a written form.
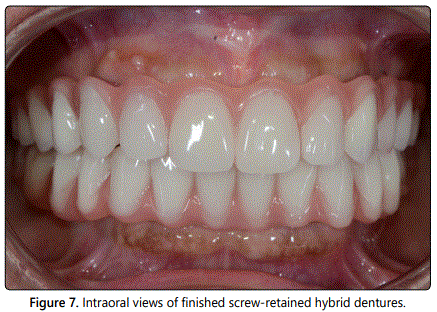
At the 6th and 12th monthʼs follow-up, the patient reported that her denture looked good and her speech was improved. During this period, the oral hygiene of patient remained satisfactory and the ability to chew of patient had improved. Radiographically, crestal bone level around the implants exhibited bone loss within normal limits.
Discussion and Clinical Significance
The selection of a connection method for the final restoration to the implant is a critical decision for using FCDs [13,14]. The current consensus is that screw-retained and cement-retained fixations are both clinically acceptable methods, and neither is more advantageous than the other [15-17]. The main advantage of screw retention is retrievability; however, off-axial implant positioning may result in the labial or buccal emergence of unsightly screw access holes. Additionally, depending on implant placement, especially in the anterior regions, the neck of the angled abutment may be visible under the superstructure. This affects esthetics and precludes the correct formation of the FCD emergence profile.
Implant location and implant-abutment connection are key factors to prevent screw-related failures [18,19]. Errors in the multiple steps during the fabricating an implant-supported fixed dentures [20-22], the type of the materials used in production [23,24], and surface irregularities of the part of implants [19,23,25], are some of the reasons of the screw loosening. In efforts to overcome the limitations of conventional methods, CAD/CAM systems that feature various ways of producing a dental prosthesis have been introduced.
The mechanical characteristics of FCDs have not been sufficiently explored, especially when restorations are connected directly to dental implants without any abutment. However, researchers expect large stresses in the screw and connection area to cause deformation, which may affect the mechanical properties of these restorations. Dittmer et al. [11] evaluated the effects of artificial aging on the load-bearing capacity of three implants-supported titanium frameworks using a cyclic mechanical loading test. No screw loosening or structure failure was reported during the cyclic mechanical loading; they suggest that this may be due to the passivity of the CAD/CAM-milled system. In contrast, Eliasson et al. [26] reports that this system is clinically acceptable without passive fit.
A clinical significance of the presented case is that the concept involves direct screw retention at the implant level without the interposition of an abutment, in addition to a milled or sintered implant bar with screw channels angled up to 20 degrees. This concept makes use of a straightforward technology that can reduce inaccuracy in laboratory procedures; and the type of denture makes it possible to realize FCDs on four or six implants with little effort and without using expensive abutments or precious alloys.
Conclusion
This clinical report documents the esthetic and functional rehabilitation of a patient through the use of implant-supported FCDs. The main limitation of this case report is that it presents the treatment of only one patient; therefore, the results herein may not be generalizable to other cases. However, this denture type does make it possible to realize FCDs on four or six implants, with little effort and without using expensive abutments or costly precious alloys.
References
- Meijer HJ, Raghoebar GM, Van't Hof MA. Comparison of implant-retained mandibular overdentures and conventional complete dentures: a 10-year prospective study of clinical aspects and patient satisfaction. Int J Oral Maxillofac Implants. 2003; 18(6): 879–885.
- Ekelund JA, Lindquist LW, Carlsson GE, Jemt T. Implant treatment in the edentulous mandible: a prospective study on Branemark system implants over more than 20 years. Int J Prosthodont. 2003; 16(6): 602–608.
- Attard NJ, Zarb GA. Long-term treatment outcomes in edentulous patients with implant-fixed prostheses: the Toronto study. Int J Prosthodont. 2004; 17(4): 417–424.
- Balshi TJ. Preventing and resolving complications with osseointegrated implants. Dent Clin North Am. 1989; 33(4): 821–868.
- Golden WG, Wee AG, Danos TL, Cheng AC. Fabrication of a two-piece superstructure for a fixed detachable implant-supported mandibular complete denture. J Prosthet Dent. 2000; 84(2): 205–209. doi: 10.1067/mpr.2000.108454
- Tan KB. The clinical significance of distortion in implant prosthodontics: is there such a thing as passive fit? Ann Acad Med Singapore. 1995; 24(1): 138–157.
- Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY. Clinical complications with implants and implant prostheses. J Prosthet Dent. 2003; 90(2): 121–132. doi: 10.1016/S0022-3913(03)00212-9
- Heckmann SM, Karl M, Wichmann MG, Winter W, Graef F, Taylor TD. Cement fixation and screw retention: parameters of passive fit—an in vitro study of three-unit implantsupported fixed partial dentures. Clin Oral Implants Res. 2004; 15(4): 466–473.
- Katsoulis J, Takeichi T, Sol Gaviria A, Peter L, Katsoulis K. Misfit of implant prostheses and its impact on clinical outcomes. Definition, assessment and a systematic review of the literature. Eur J Oral Implantol. 2017; 10: 121–138.
- Jemt T, Back T, Petersson A. Precision of CNC-milled titanium frameworks for implant treatment in the edentulous jaw. Int J Prosthodont. 1999; 12(3): 209–215.
- Dittmer MP, Nensa M, Stiesch M, Kohorst P. Load-bearing capacity of screw-retained CAD/CAM-produced titanium implant frameworks (I-Bridge® 2) before and after cyclic mechanical loading. J Appl Oral Sci. 2013; 21(4): 307–313. doi: 10.1590/1678-775720130077
- Berglundh T, Persson L, Klinge B. A systematic review of the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. J Clin Periodontol. 2002; 29: 197–212.
- Michalakis KX, Hirayama H, Garefis PD. Cement-retained versus screwretained implant restorations: a critical review. Int J Oral Maxillofac Implants. 2003; 18(5): 719–728.
- Lee A, Okayasu K, Wang HL. Screw-versus cement-retained implant restorations: current concepts. Implant Dent. 2010; 19(1): 8–15. doi: 10.1097/ID.0b013e3181bb9033
- Vigolo P, Mutinelli S, Givani A, Stellini E. Cemented versus screw-retained implant-supported single-tooth crowns: a 10-year randomised controlled trial. Eur J Oral Implantol. 2012; 5(4): 355–364.
- Sherif S, Susarla HK, Kapos T, Munoz D, Chang BM, Wright RF. A Systematic Review of Screw-versus Cement-Retained Implant-Supported Fixed Restorations. J Prosthodont. 2014; 23(1): 1–9. doi: 10.1111/jopr.12128
- Crespi R, Cappare P, Gastaldi G, Gherlone EF. Immediate occlusal loading of full-arch rehabilitations: screw-retained versus cement-retained prosthesis. An 8-year clinical evaluation. Int J Oral Maxillofac Implants. 2014; 29(6): 1406–1411. doi: 10.11607/jomi.3746
- Binon PP. Evaluation of the effectiveness of a technique to prevent screw loosening. J Prosthet Dent. 1998; 79(4): 430–432. doi: 10.1016/S0022-3913(98)70157-X
- Hecker DM, Eckert SE. Cyclic loading of implant-supported prostheses: changes in component fit over time. J Prosthet Dent. 2003; 89(4): 346–351. doi: 10.1067/mpr.2003.71
- Zervas PJ, Papazoglou E, Beck FM, Carr AB. Distortion of Three-Unit Implant Frameworks during Casting, Soldering, and Simulated Porcelain Firings. J Prosthodont. 1999; 8(3): 171–179.
- Nicoll RJ, Sun A, Haney S, Turkyilmaz I. Precision of fit between implant impression coping and implant replica pairs for three implant systems. J Prosthet Dent. 2013; 109(1): 37–43. doi: 10.1016/S0022-3913(13)60008-6
- Barbi FC, Camarini ET, Silva RS, Endo EH, Pereira JR. Comparative analysis of different joining techniques to improve the passive fit of cobaltchromium superstructures. J Prosthet Dent. 2012; 108(6): 377–385. doi: 10.1016/S0022-3913(12)60196-6
- Cibirka RM, Nelson SK, Lang BR, Rueggeberg FA. Examination of the implant—abutment interface after fatigue testing. J Prosthet Dent. 2001; 85(3): 268–275. doi: 10.1067/mpr.2001.114266
- de Torres EM, Rodrigues RC, de Mattos Mda G, Ribeiro RF. The effect of commercially pure titanium and alternative dental alloys on the marginal fit of one-piece cast implant frameworks. J Dent. 2007; 35(10): 800–805.
- Khraisat A, Stegaroiu R, Nomura S, Miyakawa O. Fatigue resistance of two implant/abutment joint designs. J Prosthet Dent. 2002; 88(6): 604–610. doi: 10.1067/mpr.2002.129384
- Eliasson A, Wennerberg A, Johansson A, Örtorp A, Jemt T. The Precision of Fit of Milled Titanium Implant Frameworks (I-Bridge®) in the Edentulous Jaw. Clin Implant Dent Relat Res. 2010; 12(2): 81–90. doi: 10.1111/j.1708-8208.2008.00131.x


