Case Report
Acute Periodontal Abscess in an Adolescent Patient: Case Report
Department of Periodontology, Faculty of Dentistry, Atatürk University, Erzurum, Turkey
*Corresponding author: Alparslan Dilsiz, Professor, Department of Periodontology, Faculty of Dentistry, Atatürk University, Turkey, Fax: +90 442 2361375, Tel: +90 442 2360940, E-mail: aydilsiz@yahoo.com
Received: August 16, 2017 Accepted: September 3, 2017 Published: September 8, 2017
Citation: Dilsiz A. Acute Periodontal Abscess in an Adolescent Patient: Case Report. Madridge J Dent Oral Surg. 2017; 2(2): 77-79. doi: 10.18689/mjdl-1000118
Copyright: © 2017 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Periodontal abscess has been defined as a suppurative lesion that is associated with periodontal breakdown and pus collection in the gingival wall of the periodontal pocket. The prevalence of periodontal abscess is relatively high and it affects the prognosis of the tooth. In this article, a patient with acute periodontal abscess due to poor oral hygiene was treated periodontically 10 days after the start of antibiotic therapy. The clinical features and likely healing results of the lesion were discussed and related literatures were reviewed.
Keywords: Periodontal Abscess; Periodontal Pocket; Alveolar Bone Resorption; Suppuration; Anti-Bacterial Agents; Periodontal Atrophy and Periodontal Debridement.
Introduction
Periodontal abscess, which is a localized purulent infection of the periodontal tissues adjacent to a periodontal pocket, is a frequent periodontal condition in which periodontal tissues may be rapidly destroyed [1,2]. Major symptoms of a periodontal abscess are known as the spontaneous or evoked pain, gingival or mucosal swelling, Red or reddish blue discoloration of affected tissue [1-4]. Affected teeth typically experience rapid periodontal tissue destruction with deep pocket formation, frequently become hypermobile, and may sometimes extrude from the alveolar socket [4]. Suppuration may appear spontaneously or after incision of the abscess [3,4]. The diagnosis of a periodontal abscess is based on information from patient history and clinical and radiographic examinations. The lesions may be acute or chronic [5]. Differential diagnosis between abscesses of periodontal and endodontic origin can be made on the basis of pulp vitality, the presence of deep periodontal pockets versus dental caries, the location of the abscess, radiographic examination, and the response to periodontal therapeutic intervention [5]. This infection occurs in the walls of periodontal pockets as a result of the invasion of bacteria into the periodontal tissues.
Different etiologies have been proposed and two main groups can be distinguished depending on its relation with periodontal pockets [5-9]. In the case of a periodontitis-related abscess, the condition may appear as an exacerbation of a non-treated periodontitis or during the course of periodontal therapy [10]. In non-periodontitis-related abscesses, impactation of foreign objects, and radicular abnormalities are the two main causes [10-11]. The abscess microflora seems to be similar to that of adult periodontitis, and it is dominated by gram-negative anaerobic rods, including well-known periodontal pathogens [12]. Periodontal abscesses are termed ‘mixed anaerobic infections’, based on microbiological findings [2,3]. Herpesvirus and Candida species can also be recovered from periodontal abscesses [6,7]. The periodontal abscess is the third most prevalent emergency infection (%6-7), after acute dento-alveoler abscess (%14-25), and pericoronitis (%10-11) [9,10].
Complications and consequences include tooth loss and the spread of the infection to other body sites [5-8]. In fact, abscess formation in the periodontium is a relatively rare occurrence [3].
Case Report
A 17-year-old girl with severe pain, swelling, excessive gingival bleeding, refractory gingival reddish, tenderness to even slight palpation on the lower anterior region, which was interfering with normal eating, brushing and speaking, was admitted to the Department of Periodontology, Faculty of Dentistry at Atatürk University.
She claimed to be in relatively good health and had not a history of drug and food allergies. She did not smoke and did not take alcoholic beverages. The patient reported that he had a severe toothache of lower right incisors teeth the night before.
During physical examination, the extraoral examination showed mouth breathing. General health status was fair but, a few enlarged and tender lymph nodes were present bilaterally in the submandibular areas.
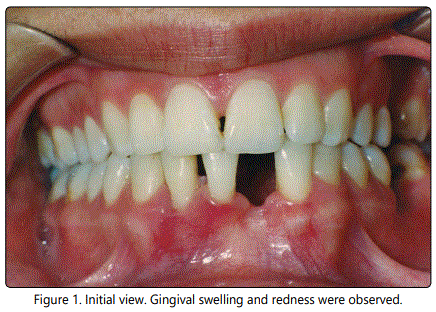
The intra-oral examination revealed that she was suffering from severe pain, swelling, gingival bleeding and disfunction. There was a heavy accumulation of dental plaque and calculus, the gingival tissues were swollen (Figure 1). Periodontal pocket was measured as 7mm in facial of mandibulary right central and lateral incisors. Baseline periodontal parameters are listed in table 1.

After having undergone clinical examinations, she was diagnosed a1s having “Acute periodontal abscess”. Written informed consent was obtained from the patient after all treatment procedures had been fully explained.
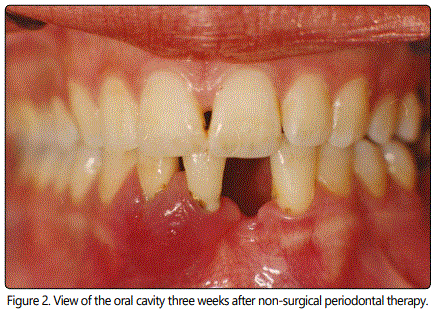
At the conclusion of her periodontal examination, the patient was prescribed antibiotics (amoxicillin 1000 mg, every 8 hours, 3 days), analgesics (Naproxen 550 mg, every 12 hours, 3 days) and instructed to rinse twice daily with 0.12% chlorhexidine (Kloroben®, Drogsan Drug Ltd, İstanbul, Turkey) oral rinse for seven days. Seven days later, the affected regions of gingiva appeared less painless. Thereafter, a thorough supra and subgingival scaling, root planning and crown polishing were performed carefully and pus was careful drained via probing from the pocket. Ten days later deep subgingival curettage was performed. Three weeks following non-surgical periodontal therapy, the affected area had completely healed, there were no gingival redness, bleeding and swelling, and no lymphadenopathy was noted (Figure 2). She was encouraged to practice good oral hygiene with a soft-bristle toothbrush. She has visiting a periodontist regularly for three years since that time.
Discussion
Periodontal abscesses are the most common type of abscesses including the periodontium. Its importance is based on the possible need of urgent care, the affectation of tooth prognosis, and the possibility of infection spreading [1-6].
In the related literature, there is scant information in the scientific literature regarding this condition, and most of it has been published as case reports and text books, where conclusions are not evidence-based, but rather empirical observations made by recognised clinicians [6-9]. In the present case, periodontal abscess was associated with subgingival calculus and periodontal pocket.
Diagnosis of periodontal abscess should be made after on overall evalution and interpretation of the patientʼs chief complaint, medical-dental history, and clinical and radiographic examinations. Periodontal abscess can be treated with draining, scaling-root planing, curettage and giving antibiotics, and routine surgical technics [5,8-12], as was showed in this case.
In conclusion, diagnosis and treatment of periodontal abscess are mainly based an empiricism, since evidence-based data are not available. To maintaine periodontal health and to correct the esthetics, their pathology should be treated.
References
- Corbet EF. Diagnosis of acute periodontal lesions. Periodontol 2000. 2004; 34: 204-216. doi: 10.1046/j.0906-6713.2003.003432.x
- Jaramillo A, Arce RM, Herrera D, et al. Clinical and microbiological characterization of periodontal abscesses. J Clin Periodontol. 2005; 32: 1213-1218. doi: 10.1111/j.1600-051X.2005.00839.x
- Herrera D, Roldan S, Gonzalez I, et al. The periodontal abscess (I). Clinical and microbiological findings. J Clin Periodontol. 2000; 27: 387-394. doi: 10.1034/j.1600-051x.2000.027006387.x
- Carranza FJ. Carranzaʼs Clinical Periodontology, 9th edn. Philadelphia: W.B. Saunders. 2002; 448-451.
- Dahlen G. Microbiology and treatment of dental abscesses and periodontal-endodontic lesions. Periodontol 2000. 2002; 28: 206-239. doi: 10.1034/j.1600-0757.2002.280109.x
- Saygun I, Yapar M, Özdemir A, Kubar A, Slots J. Human cytomegalovirus and Epstein-Barr virus type 1 in periodontal abscesses. Oral Microbiol Immunol. 2004; 19: 83-87. doi: 10.1046/j.0902-0055.2002.00118.x
- DeWitt GV, Cobb CM, Killoy WJ. The acute periodontal abscess: microbial penetration of the soft tissue wall. Int J Periodontics Restorative Dent. 1985; 5: 38-51.
- Herrare D, Rolden S, Sonz M. The periodontal Abscess: A review. J Clin Periodontol. 2000; 27: 377-386. doi:10.1034/j.1600-051x.2000.027006377.x
- Meng HX. Periodontal Abscess. Ann Periodontol. 1999; 4: 79-82. doi: 10.1902/annals.1999.4.1.79
- Mc Leod DE, Lainson PA, Spivey JD. Tooth Loss due to Periodontal Abscess: A retrospective study. J Periodontol. 1997; 68: 963-966. doi: 10.1902/jop.1997.68.10.963
- Palmer RM. Acute lateral periodontal abscess. Br Dent J. 1984; 15: 311-312.


