Research Article
The Nature of Changes in the Main Quality-of-Life Parameters after Treatment in Teenagers with Dental Caries
Department of Pediatric Dentistry, A.I. Evdokimov Moscow State University of Medicine & Dentistry, Moscow, Russia (In cooperation with the UNESCO “Healthy Way of Life is a Key to Successful Development” initiative.)
*Corresponding author: Larisa Kiselnikova, Department of Pediatric Dentistry, Moscow State University, Moscow, Russia, E-mail: lpkiselnikova@mail.ru
Received: September 28, 2016 Accepted: May 26, 2017 Published: June 3, 2017
Citation: Kiselnikova LP, Zueva TE, Gurevich KG, Alibekova AA, Popova NS. The Nature of Changes in the Main Quality-of-Life Parameters after Treatment in Teenagers with Dental Caries. Madridge J Dent Oral Surg. 2017; 2(2): 65-70. doi: 10.18689/mjdl-1000116
Copyright: © 2017 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
The aim of this study has been to evaluate the nature of changes in the quality of life in a population of teenagers with dental caries and their complications after oral caries elimination.
The authors have examined and treated 112 teenagers, ages 12 to 17, with dental caries and complications, in the city of Moscow, Russia. A validated Child Perception Questionnaire (CPQ) was used to assess their quality of life. The teenagers were surveyed three times: 1) once when first referred to the dental clinic before dental treatment, 2) just after the initial dental treatment, and 3) three months after the end of the dental treatment.
Additionally, we have conducted a comparative analysis of the quality-of-life parameters of the teenagers with dental caries compared with a control group of teenagers with healthy teeth. We found no improvement in parameters of the teenagersʼ quality of life just after the end of the initial dental treatment. Three months later, however, an improvement was noticed in the quality of life as a whole, as well as in all domains of the CPQ; namely, improvements in the areas of oral symptoms, functional limitations, emotional well-being, and social well-being. Our research has shown that three months after the end of dental restorative treatment, perception of the quality of life by teenagers with a history of dental caries and complications had improved so much that their perception of quality of life was even more favorable than the control group of teenagers without caries.
Keywords: Quality of Life; Teenagers; Dental Caries; CPQ; DMF.
Introduction
Presently, dental caries is the most wide-spread human disease and is an acute problem in modern dentistry.
The prevalence of the main dental diseases in children in various cities and towns of Russia continues to remain high. Analysis of the data of the second National Epidemiologic Examination performed in Russia in 2009, found that the prevalence of permanent-tooth caries in 12-year-old Moscow children amounted to 71%, with the intensity according to the dmf index equal to 2.45. In 15-year-old children, caries prevalence reached 81% and its intensity was 3.72 [1].
In some countries of the world, researchers have investigated the quality of life in pediatric dental patients in order to study the influence of the carious process upon young childrenʼs quality of life as well as the influence of dental health on teenagersʼ quality of life [2-4].
Today in Russia, practically no measuring instruments exist to assess teenagersʼ dental quality of life. Although these assessment tools have not yet been developed in Russian, examples of validation tools for the study of the quality of life already do exist in other world languages [5-8]. Internationally, investigators have conducted studies regarding the correlation between dental status and the quality of life for young children of pre-school age as well as other young school children [9-10].
One of the most widely used indices for evaluation of the quality of life of teenagers is OHRQoL (Oral Health-Related Quality of Life) [11]. Canadian researchers have worked out questionnaires for the evaluation of the quality of life connected with the condition of the oral cavity (Child Perceptions Questionnaires – CPQ) in children of various ages [12,13]. Each of these indexes is intended to measure the frequency, intensity, and the extent of dental problems and their influence on a personʼs functional, social and psychological wellbeing, as well as for expert assessment of the need for and efficacy of dental care.
Prior to our research, no investigations devoted to the study of a correlation between the quality of life and dental disease had been conducted in Russia. Nor did any studies exist which monitored changes in teenagersʼ perception of the quality of life subsequent to dental treatment.
Research Aim
The aim of our research was to evaluate the nature of changes in the quality of life of teenagers with dental caries and complications after restorative treatment of the oral cavity.
Materials and Methods
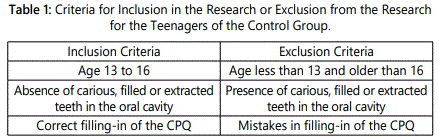
An epidemiologic dental examination and survey were conducted of 205 teenagers, aged 13 to 16, studying at Moscow secondary educational institutions. On the basis of the dental examination, a group of 35 teenagers without any dental carious lesions were selected to serve as a control group for comparative analysis (Table 1).
Additionally, 112 teenagers, who came to the Dental Clinic of the Department of Pediatric Dentistry of Moscow State University of Medicine and Dentistry (MSUMD) for dental treatment, were examined. Dental caries and complications were diagnosed in all the examined teenagers (Table 2).
After the examination, all of the teenagers were referred to dentists for treatment in the Dental Clinic of MSUMD Department of Pediatric Dentistry.
The treatment of caries and complications offered to the teenagers from the subject group was performed in accordance with the standard systems of dental care. Only dental materials recommended in the list of standards for providing dental care to children were used.

Dental examination was carried out inside a dentistʼs office with artificial lighting and with the use of a standard kit of dental instruments.
The following parameters of the dental status were assessed:
- Caries intensity according to the dmf index
- Hygienic condition of the oral cavity, hygiene index OHI – S.
To assess the quality of life we used the validated CPQ questionnaire. This questionnaire was developed in accord with the WHO recommendations on the basis of the Child Perceptions Questionnaire (CPQ) [12,13].
An adapted version of the CPQ questionnaire for teenagers was drafted by a group of specialists with participation of a dentist, a psychologist, translators and 13- to 16-year-old teenagers [14,15].
Linguistic and cultural adaptation of the questionnaire was carried out involving the following stages:
- 1st stage—a direct translation from the questionnaireʼs original language. At this stage, we received two independent Russian translations from the original English version.
- 2nd stage—a preliminary version of the questionnaire. At this stage, a preliminary Russian version of the questionnaire was created on the basis of the two direct translations from English.
- 3rd stage—back translation. At this stage, two back translations of the preliminary version from Russian into English were completed.
- 4th stage—expert examination. This was the stage during which an independent expert provided an assessment, and any necessary orthographical or grammatical editing was completed. As a result, a test version of the questionnaire was produced.
- 5th stage—pilot testing or pre-testing. At this stage, teenagers were surveyed in order to reveal their opinions about the questions contained in the questionnaire and to discover their wishes for a more correct and exact formulation of questions.
The questionnaire consists of 16 questions which assess the teenagerʼs quality of life according to four main domains: 1) oral symptoms, 2) functional limitations, 3) emotional wellbeing, and 4) social wellbeing.
To register any oral symptoms in the mouth cavity, it was necessary to record information about difficulties in food mastication, the presence of bad breath, dental or any other pain in the mouth, bleeding, as well as any information about lesions and wounds.
The functional limitations domain focuses on possible sleep disturbances due to problems with teeth, difficulties when eating hot, cold or hard food, as well as difficulties in pronouncing words.
The domain dealing with emotional wellbeing contains questions dealing with feelings of being upset or irritated due to problems with oneʼs teeth. This domain also includes questions aimed at finding out if teenagers are ashamed of their teeth or worried about other peopleʼs opinion about the condition of their teeth.
Social wellbeing is evaluated by including questions dealing with teenagerʼs social relationships, asking, for example, if teenagers are being teased, if they are shy when answering a teacher in a classroom setting or when they are reading aloud in class, or if, when they are smiling, others notice their teeth problems and discuss them.
In answering questions in all four domains, teenagers are asked to choose one of four possible responses. These responses are coded with the assessment points for further analysis: a response of “never” receives 1 point, a response of “seldom” receives 2 points, a response of “often” receives 3 points, a response of “always” receives 4 points. In other words, the larger the number of points respondents receive as a result of answering the questionnaire, the more seriously they feel about their condition.
The CPQ questionnaire validation was discussed and approved by both the Ethical Committee (Protocol No. 6, dated February 22, 2011) and the Scientific Board (protocol No. 6, dated March 15, 2011) of A.I. Evdokimov Moscow State University of Medicine and Dentistry.
Surveying of teenagers in the comparison group using the CPQ questionnaire was conducted only once, during dental epidemiologic investigation. The teenagers answered the questions in the questionnaire independently.
Teenagers in the study group were surveyed three times: 1) initially, when coming to the clinic but before dental treatment began, 2) then just after the oral cavity curative treatment was completed, and 3) finally, three months after the end of treatment to the clinic.
For purposes of mathematical data processing, we used the software package Statistica 6.0 of StatSoft, Inc.
The following calculations were used at every stage of the research: mean values, extensive and intensive indices, standard errors, the reliability of the mean and relative values.
Results
The data of the analysis of dental caries intensity and of hygienic condition of the oral cavity of the teenagers who took part in the research are given in table 3.
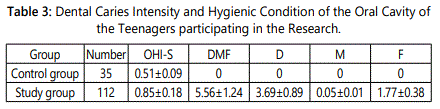
The control group included 35 teenagers without any dental carious lesions (DMF is 0). The analysis of the oral cavity hygienic condition in this group of teenagers revealed a good level of hygiene with the mean value on the OHI-S index being 0.51±0.09.
Dental caries and its complications were diagnosed in all the teenagers in the study group. Caries intensity in this group was equal to 5.56±1.24. During the assessment of individual components of the DMF index, it was found out that the “D” component (teeth with caries) was equal to 3.69±0.89 and the “F” component (filled teeth) was 1.77 ±0.38. The number of extracted teeth (component “M”) in the study group was also insignificant and was as little as 0.05±0.01.
The assessment of the hygienic condition of the oral cavity according to the OHI-S index in this group of teenagers showed a satisfactory level of hygiene with its main value being 0.85±0.18.
To assess the nature of changes in the main quality-of-life parameters of the teenagers who came to the MSUMD Department of Pediatric Dentistry clinic for treatment (the study group), we performed a comparative analysis of the CPQ survey data. We compared the data recorded at three different times: 1) during the initial survey on the day of the teenagersʼ first arrival to the clinic, 2) during the survey immediately after the oral cavity restorative treatment, and 3) three months after the restorative treatment. These data were then also compared with the results received when surveying the teenagers from the control group (Table 4).
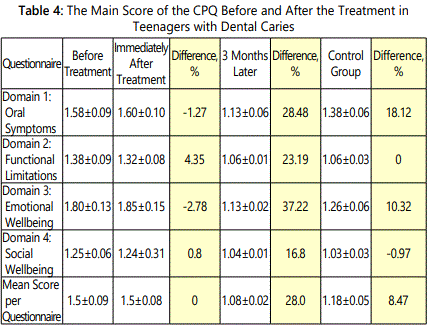
In the course of the comparative analysis of the CPQ parameters in teenagers with dental caries before and after treatment, we found that immediately after curative treatment the mean score of the questionnaire had not changed (the difference is 0%). Three months after the restorative treatment, this parameter improved by 28.48% (from 1.5 to 1.08 points). The perceived changes suggest an improvement of the quality of life of the surveyed teenagers only three months after completion of the restorative treatment.
We also compared the mean score of the CPQ for teenagers from the study group (the teenagers who had come to the clinic for treatment of dental caries and its complications) after the treatment with the scores of teenagers from the control group (the teenagers with intact teeth). Three months after the oral cavity restorative treatment, the questionnaire mean score for teenagers from the study group improved by 8.47% less when compared with the scores of the teenagers in the control group. In the study group, the score was 1.08; in the control group, it was 1.18.
Thus, the comparative analysis has shown that after dental restorative treatment in teenagers with dental caries, the quality-of-life parameters not only improve, but actually exceed the quality-of-life parameters in the control group of teenagers whose teeth were without any carious lesions.
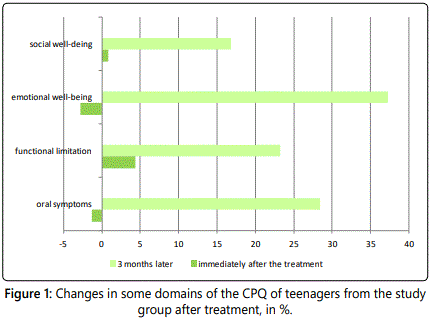
When analyzing the nature of changes in some domains of the questionnaire devoted to the quality of life, the following data were received before and after treatment in relation to the teenagers with dental caries (Figure 1).
When analyzing the changes in the “oral symptoms” domain, we noticed that immediately after dental treatment, there was an insignificant increase (1.27%) in the mean score in this domain of the questionnaire. This fact suggests a worsening of the quality of life. The change in the “Oral symptoms” domain saw an increase of the mean score from 1.58 to 1.60%.
An absolutely different pattern of changes was revealed three months after the dental restorative treatment. We can see an improvement in the mean score of the answers to the questions in this domain from 1.58 to 1.13 points and, as a consequence, an improvement in the quality of life (the difference is 28.48%).
Comparison of the data received after restorative treatment in the control group revealed that for the teenagers in the study group three months after treatment, the mean score in the questionnaire domain dealing with “physical discomfort” was less than in the control group. In the study group, the score was equal to 1.13, while in the control group it was 1.38. The difference between the groups was 18.12% which was the maximal difference in the CPQ among all the domains.
In the domain dealing with “functional limitations”, we could see an improvement in the quality of life both immediately after the treatment and three months later. Yet, the changes were noticed to be even more pronounced after three months. So, the initial mean score value in the questionnaire for this domain was 1.38 in the study group of teenagers, though immediately after the treatment the mean score dropped slightly to 1.32 (the difference is 1.06%). Three months later the change became more pronounced; the mean score parameter dropped to 1.6, which resulted in a difference of 23.19%.
Comparison of the results recorded for the study group three months after restorative treatment with the data for the control group, showed that the mean score of points for the “functional limitations” domain in the teenagers of both the study group and the control group was exactly the same—1.06.
In the “emotional well-being” domain, the teenagers from the study group showed an increase of the mean score by 2.78% from the initial value (from 1.80 up to 1.85 points) immediately after dental treatment, which suggests worsening of the above quality-of-life parameter. Three months later, the teenagerʼs perception of their condition changed; the mean score for this domain improved by 37.22% (from 1.8 to 1.13 points). This fact indicates betterment in the quality of life for these teenagers.
When comparing the obtained results with the control group, we found that after oral cavity restorative treatment the mean score for the domain dealing with “emotional wellbeing” was better than in the control group by 10.32%. The mean score parameters for the teenagers in the study group and for those in the control group were 1.13 and 1.26, respectively.
In the domain dealing with “social well-being”, minimal mean score values were received for all the time points of observation. The difference in the values before and after treatment was less pronounced.
Immediately after dental treatment, the mean score in this part of the questionnaire dropped insignificantly from 1.25 to 1.24 points (the difference is 0.8%). Three months after oral cavity curative treatment, the improvement was more marked (16.8%), and the parameter reached a value of 1.4. This fact also suggests an improvement in the quality of life in this domain.
Comparison of “social well-being” with the control group, revealed that three months after oral cavity curative treatment, the teenagers in the study group had a mean score in this domain very closely resembling that in the control group—1.04 and 1.03, respectively. As a result, the difference between the mean scores of the study group and the control group was not significantly different, differing by only 0.97%.
Thus, the analysis showed that immediately after oral cavity curative treatment, teenagers with dental carious lesions do not notice any positive changes in the quality of life initially, but, on the contrary, they notice a little worsening according to questionnaire domains “physical discomfort” and “emotional well-being”.
An improvement in the quality of life in all the parameters, however, was observed three months after oral cavity restorative treatment. The most pronounced changes were revealed in “emotional well-being” domain, while the least were noticed in “social well-being” domain.
In the course of comparison with the group of teenagers of similar age without carious lesions (the control group), we observed better quality-of-life parameters in the “oral symptoms” and “emotional well-being” domains for teenagers of the study group three months after oral cavity restorative treatment. However, in the “functional limitations” and “social well-being” domains, the mean score of the CPQ was identical in the both groups. In summary, three months after dental restorative treatment, the study group teenagers with dental caries and complications perceived their quality of life as not only having improved, but so much so, that their perception of quality of life even exceeded that of teenagers with intact teeth (control group).
Discussion
Research aimed at the study of correlation between diseases of the oral cavity and perception of the quality of life by children of school age has been carried out in different countries of the world [16-19]. According to Palache J, et al. [20], dental problems such as dental caries, discolorations, traumatic lesions have a negative influence on all domains of the quality of life in children 12–14 years old. The effect of the extent of dental caries lesions upon the childrenʼs quality of life is mentioned in the research of many other authors [21,22,32].
When in the course of this research we made an assessment of the quality-of-life parameters (according to CPQ) in children aged 11–14, we discovered carious lesions had a negative influence on oral symptoms, functional limitations, emotional and social well-being. CPQ index values and those of all its domains were higher in teenagers with dental caries than the values of a control group comprised of healthy teenagers.
The worst parameters in the quality of life in teenagers with dental caries were discovered in the “Emotional wellbeing” domain which correlates with the results presented by Foster Page LA et al. [23,24]. Foster-Page LA et al. showed that emotional and social characteristics of the quality of life (OHRQoL) are more important for teenagers than clinical ones, and thus are more susceptible to the influence of dental problems.
The analysis has revealed that immediately after the restorative dental treatment, the teenagers with carious lesions do not notice any positive changes in the quality of life. On the contrary, according to the data in the “oral symptoms” and “emotional well-being” domains, we noticed an insignificant worsening.
Such results may be connected with a feeling of discomfort just after the treatment of caries and its complications. Such discomfort may be attributed to such causes as infiltration/conduction in the place where an anesthetic needle was inserted or irritation of the gingival papilla after the use of matrix systems in the treatment of dental caries on contact surfaces of the teeth. In addition, during long-term dental treatment, teenagersʼ emotional condition often adversely affected.
Improvement of the quality of life in all the parameters was observed three months after treatment, with the most pronounced changes being in the “Emotional well-being” domain and the least pronounced changes being in the “Social well-being” domain.
The data of this study agree well with the results given by other investigators [25-27].
An investigation which studied changes in the quality of life after dental treatment involving the use of general anesthesia in children aged 6–14 was conducted in Australia by Yawary R, et al [28]. For the assessment of the quality of life, the authors used the CPQ and surveyed children on the basis of this questionnaire three times: 1) once before treatment, 2) again two weeks after treatment, and 3) finally three months after the treatment. All children had received treatment under general anesthesia. Improvement in the quality of life as a whole and per individual questionnaire domains (Oral symptoms, Functional limitations, Emotional and Social wellbeing) was observed. There was an improvement in the questionnaire mean score by 65% two weeks later and by 76.5% three months after treatment.
In our study, the mean improvement was not as dramatic. This differing score reduction may be due to worse initial oral cavity parameters of children in R. Yawaryʼs investigation. The childrenʼs dmf was equal to 8.2, whereas in our research, the dmf was only 5.56. The difference may also be connected with the psycho-emotional condition of the children who require general anesthesia for an adequate treatment, as well as the age deferential between the two studies.
Researchers in various countries observe improvement in teenagersʼ quality of life after treatment of dental caries and its complications [29-31].
In addition, belated treatment in younger children may give rise to more pronounced limitations in their quality of life [32,33].
The authors of this current study were the first in Russia to validate the CPQ for the evaluation of teenagersʼ quality of life and to establish a correlation between caries with complications and its impact on teenagersʼ quality of life. The data we discovered in our research determine that it is justifiable to use the validated CPQ when planning the volume and scope of dental treatment, as well as when assessing the efficacy of treatment for caries and its complications in teenagers.
Conclusions
1. There is no improvement in the parameters of teenagersʼ quality of life immediately after treatment; on the contrary, there is a little worsening in such domains as “oral symptoms” and “emotional well-being”.
2. Three months after dental treatment there was an improvement in the quality of life as a whole as well as per all the domains of the CPQ, namely, in oral symptoms, functional limitations, emotional well-being and social well-being.
3. The validated CPQ is recommended to be used as an objective criterion for the assessment of the efficacy of treatment of caries and its complications in teenagers.
Conflict of Interest
The authors declare no conflict of interest with this submission.
References
- Foster Page LA, Thomson WM, Jokovic A, Locker D. Validation of the Child Perceptions Questionnaire (CPQ 11–14). J Dent Res. 2005; 84: 649–652. doi: 10.1177/154405910508400713
- Tsacos G, Bernabe E, OʼBrien K, Sheiham A. Comparison of the selfadministered and interviewer-administered models of the child-OIDP. Health and Quality of Life Outcomes. 2008; 6: 40. doi: 10.1186/1477-7525-6-40
- Marshman Z, Rodd H, Stern M, et al. An evaluation of the Child Perceptions Questionnaire in the UK. Community Dent Health. 2005; 22: 151–155.
- Yusuf H, Ghrunpong S, Sheiham A, Tsakos G. Validation of an English version of the Child-OIDP index, an oral health-related quality of life measure for children. Health and Quality of life Outcomes. 2006; 4: 38. doi: 10.1186/1477-7525-4-38
- Easton JA, Landgraf JM, Casamassimo PS, et al. Evaluation of a generic quality of life instrument for early childhood caries-related pain. Community Dent Oral Epidemiol. 2008; 36: 434–440. doi: 10.1111/j.1600-0528.2007.00417.x
- de Castro RA, Portela MC, Leao AT, de Vasconcellos MT. Oral healthrelated quality of life of 11- and 12-year-old public school children in Rio de Janeiro. Community Dent Oral Epidemiol. 2011; 39(4): 336–344. doi: 10.1111/j.1600-0528.2010.00601.x
- Hugoson A, Koch G, Helkimo AN, Lundi SA. Caries prevalence and distribution in individuals aged 3-20 years in Jonkoping, Sweden, over a 30-year period (1973–2003). Int J Paediatr Dent. 2008; 18(l): 18–26. doi: 10.1111/j.1365-263X.2007.00874.x
- Robinson PG, Nalweyiso N, Busingye J, Whitworth J. Subjective impacts of dental caries and fluorosis in rural Ugandan children. Community Dent Health. 2005; 22: 231–236.
- Jokovic A, Locker D, Stephens M, Kenny D, Tompson B, Guyatt G. Validity and reliability of a questionnaire for measuring child oral-health-related quality of life. J Dent Res. 2002; 81: 459–463. doi: 10.1177/154405910208100705
- Jokovic A, Locker D, Tompson B, Guyatt G. Questionnaire for measuring oral health-related quality of life in eight- to ten-year-old children. Pediatr Dent. 2004; 26: 512–518.
- Brown A, Al-Khayal Z. Validity and reliability of the Arabic translation of the child oral-health-related quality of life questionnaire (CPQ 11–14) in Saudi Arabia. Int J Paediatr Dent. 2006; 16: 405–411. doi: 10.1111/j.1365-263X.2006.00775.x
- Leal SC, Bronkhorst EM, Fan M, Frencken JE. Untreated cavitated dentine lesions: impact on childrenʼs quality of life. Caries Res. 2012; 46: 102–106. doi: 10.1159/000336387
- Schuch HS, Costa FS, Torriani DD, Demarco FF, Goettems ML. Oral-healthrelated quality of life of schoolchildren: impact of clinical and psychosocial variables. Int J Paediatr Dent. 2015; 25: 358-65. doi: 10.1111/ ipd.12118.
- Tubert-Jeannin S, Pegon-Machat E, Gremeau-Richard C, Lecuyer MM, Tsakos G. Validation of a French version of the Child-OIDP index. Eur J Oral Sci. 2005; 113: 355–362. doi: 10.1111/j.1600-0722.2005.00230.x
- Pulache J, Abanto J, Oliveira LB, Bonecker M, Porras JC. Exploring the association between oral health problems and oral health-related quality of life in Peruvian 11- to 14-year-old children. Int J Paediatr Dent. 2016; 26(2): 81–90. doi: 10.1111/ipd.12160
- Krisdapong S, Prasertsom P, Rattanarangsima K, Sheiham A. Relationships between oral diseases and impacts on Thai school childrenʼs quality of life: evidence from a Thai national oral health survey of 12- and 15-yearolds. Community Dent Oral Epidemiol. 2012; 40(6): 550–559. doi: 10.1111/j.1600-0528.2012.00705.x
- Martins-Junior PA, Oliveira M, Marques LS, Ramos-Jorge ML. Untreated dental caries: impact on the quality of life of children of low socioeconomic status. Paediatr dent. 2012; 34: 49–52.
- Foster-Page LA, Thomson WM, Ukra A, Farella M. Factors influencing adolescentsʼ oral-health-related quality of life (OHRQoL.). Int J Paediatr Dent. 2011; 23: 415–423. doi: 10.1111/ipd.12011
- Foster-Page LA, Thomson WM. Caries prevalence, severity, and 3-year increment, and their impact upon New Zealand adolescentsʼ oralhealth-related quality of life. J Public Health Dent 2012; 72: 287–294. doi: 10.1111/j.1752-7325.2012.00336.x
- Paula JS, Tôrres LH, Ambrosano GM, Mialhe FL. Association between oral health-related quality of life and atraumatic restorative treatment in school children: an exploratory study. Indian J Dent Res. 2012; 23(6): 738– 741. doi: 10.4103/0970-9290.111249
- Alves LS, Dame-Teixeira N, Susin C, Maltz M. Association among quality of life, dental caries treatment and intraoral distribution in 12-year-old South Brazilian schoolchildren. Community Dent Oral Epidemiol. 2012; 11: 22–29. doi: 10.1111/j.1600-0528.2012.00707.x
- Dame-Teixeira N, Alves LS, Ardenghi TM. Traumatic dental injury with treatment needs negatively affects the quality of life of Brazilian school children. Int J Paediatr Dent. 2013; 23(4): 266–273. doi: 10.1111/ipd.12002
- Yawary R, Anthonappa RP, Ekambaram M, McGrath C, King NM. Changes in the oral health-related quality of life in children following comprehensive oral rehabilitation under general anaesthesia. Int J Paediatr Dent. 2016; 26(5): 322–329. doi: 10.1111/ipd.12200
- Mashoto KO, Astrom AN, Skeie MS, Masalu JR. Changes in the quality of life of Tanzanian school children after treatment intervention using the Child-OIDP. Eur J Oral Sci. 2010; 118: 626–634.
- Nurelhuda NM, Ahmed MF, Trovik TA, Astrom AN. Evaluation of oral health related quality of life among Sudanese schoolchildren using ChildOIDP inventory. Health Qual Life Outcomes. 2010; 8: 152–163. doi: 10.1186/1477-7525-8-152
- Chukwumah NM, Folayan MO, Oziegbe EO, Umweni AA. Impact of dental caries and its treatment on the quality of life of 12- to 15-year-old adolescents in Benin, Nigeria. Int J Paediatr Dent. 2016; 26(1): 66–76. doi: 10.1111/ipd.12162
- Bianco A, Fortunato L, Nobile CGA, Pavia M. Prevalence and determinants of oral impacts on daily performance: results from a survey among school children in Italy. Eur J Public Health. 2010; 20: 595–600. doi: 10.1093/eurpub/ckp179
- Biazevic MGH, Rissotto RR, Michel-Crosato E, Mendes LA, Mendes MO. Relationship between oral health and its impact on quality of life among adolescents. Braz Oral Res. 2008; 22: 36–42. doi: 10.1590/S1806-83242008000100007


