Research Article
Correlation Between Ages and the Success Rates of Patients with Permanent Dentition in Restorative Dentistry - Retrospective Method
School of Medicine and Dentistry, Barts and The London, New Road, London, UK
*Corresponding author: Ali Nankali, Clinical Lecturer, School of Medicine and Dentistry, Barts and The London, New Road, London, UK, Tel: +44 (0) 20 7882 6353, E-mail: a.nankali@qmul.ac.uk
Received: March 2, 2017 Accepted: March 17, 2017 Published: March 30, 2017
Citation: Ali N, Doxuan C. Correlation Between Ages and the Success Rates of Patients with Permanent Dentition in Restorative Dentistry - Retrospective Method. Madridge J Dent Oral Surg. 2017; 2(1): 51-54. doi: 10.18689/mjdl-1000113
Copyright: © 2017 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Background: The UK population has undergone a significant increase in the median age during last 40 years. Ageing could cause detrimental effects on oral and medical function; and thus, it has been suggested that Oral Health Care System may to adjust its services due to the changes in age structures.
Aim: An audit was set up to assess the success rates and determine the deficiencies in treatment procedures between seven age groups, which may impact the quality of treatment.
Method: The study was conducted as an audit, and 110 notes from patients who attended as the first visit between 2013 and 2014 in the restorative department at the Royal London Dental Hospital were selected randomly. Measurements included demographic (age, gender, income and educational level) and clinical factors (treatment selection, periodontal charts, high priority, smoking cessation, oral hygiene instruction, radiographs). The audit standards follow from the Royal London Dental Hospital and Central Manchester University Hospitals referral guidelines for the restorative department.
Results: More than half of monitored patients were the cohort of 36 to 65 years old. The presence of priorities, periodontal charts, smoking cessation and oral hygiene instruction was recorded at just below 85 percent in the majority of age groups, and there was a decreasing trend of success rate from 26 to 75s.
Conclusion: The high disproportion in demand between age groups needs to be considered by dental practitioners and required further investigations. A raised number of concerns in primary care service should be investigated. Some clinical steps illustrate the need for continuing professional development courses and further research.
Keywords: Ageing, Restorative Dentistry; Referral Guidelines; UK Population; Survey; Oral Health.
Introduction and Background
Over 40 years since the establishment of restorative dentistry, the UK population has undergone a significant raise in both the median age and proportion of elderly; and it is expected to keep this ageing trend for the followed period of 20 years [1,2]. The average age of the UK population at mid-2014 was at its highest ever at 40 which is much greater compared to 33.9 years in 1974. Similarly, the age of over 65s has increased by 47 percent since 1974 to make up about 18 percent of the total population in mid-2014. Meanwhile, the number of the population aged 75 and higher has grown by 89 percent during the period and now accounts for 8 percent of the UK residents.
Also, the Adult Dental Health Survey (ADHS) from its first publication in 1968 to the most recent survey in 2009 has noticed the high need for oral health services for the present elderly [3]. In the first investigation, 37 percent of the England and Wales population lost all of their natural teeth, and it was not uncommon for people to have no teeth at a relatively young age. This survey, for example, shows that 7 percent of adults in these two regions at the age of 25 to 34 and 22 percent of adults aged 35 to 44 were edentate. They are now getting to be part of an older generation whose overall levels of tooth retention plays an important role in assessing the dental health of the population from 2009.
In addition to the life expectancy changes, Murray (2015) claimed that ageing could lead to detrimental effects on organsʼ function in the human body. The conditions could be general risk factors such as the prevalence of diabetes, cardiovascular disease, arthritis, cancer, chronic obstructive airways disease as well as the simultaneous use of many medications [4-9]. Furthermore, oral risks including xerostomia, lack of manual dexterity, cariogenic diets may contribute to the patientʼs issues [7].
Accordingly, it has been suggested that Oral Health Care System has to adjust its services to adapt to changes in age structures in the UK population [10]. A treatment plan should be considered more thoroughly of the older population. The dental staffs are acquired to comprehend the correlation between oral health and aged - related factors combined with being patient in taking history and performing the examination for these individuals in order that no factors would be discounted.
Aims and Objectives
The audit to some age–related factors in restorative dentistry is still unknown, and it seems that not all of the general dental practitioners comprehend their treatments, communications, examinations and referrals for each age group [11]. Thus, in the audit, it is more focused on the evaluation of the treatment plans as well as the appreciation of referrals.
Aim
The purpose of the audit was to assess the success rates with by age-groups (16-25, 26-35; 36-45, 46-55, 56-65, 66-75 and above 75) at the restorative department in RLDH. It was also aimed to determine the deficiencies in the procedures of making treatment plan and its performance for permanent dentition between the age groups.
Objective
To finding the factors that may be used to improve the National Health Service quality of service and increase the success rates of patients in restorative dentistry.
Materials and Method
Study design
The study was conducted as an audit to evaluate treatment planningʼs considering patientsʼ age in restorative dentistry, which was with the intention of reassessing current dental care. The audit was carried out retrospectively for several months in 2016 using the records of the restorative department at the Royal London Dental Hospital. This audit was approved by Barts Health NHS – Trust via Clinical Effectiveness team on the 22nd of February in 2016 before starting data collection.
110 notes by random were collected and analysed. The audit included adult patients who were16 years old and above in order to have appropriate ages groups according to Adult dental health survey 2009. Following up permanent dentition was also corresponded to the goal of this audit. In order to assess the process more objectively, we selected the patients were from those who were recorded as first visited to the restorative department between 2013 and 2014.
Measurement
In terms of demographic, patientsʼ age are based on their closest birthday and the first date of the clinic. Patientʼs locations (Loc) were recorded according to their postcodes. From those, socioeconomic were identified via free and publicly available website.
In addition, periodontal charts, smoker, oral hygiene state (OH), oral hygiene instruction (OHI) and reassessments of OH contributing to the favourable results, was assessed.
Criteria and standards
As the audit was placed in the Royal London Dental Hospital (RLDH), it was tried to use the RLDH referral guidelines in congestion with Central Manchester University Hospitals (CMUH) guidelines would support the missing points [12-13].
Results
Demographics
In the audit, the largest random selected seen sample (23.4%) was the age between 36 to 45 years old, followed by 16 to 25 (18%) and 46 to 55 (16.3%). The cohort of 26 to 35 and 56 to 65 together made up 30.6 percent of the total sample size. It was noticed that the majority of cases were under impact by income and education level.
Clinical
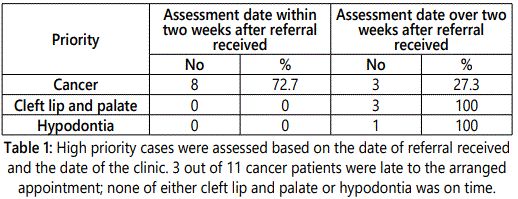
The information guided us to recognise 3 groups of patients: Cancer, cleft lip and palate, and hypodontia. The vast majority of cancer patients (72.7%) were assessed less than two weeks after the referral letter was received.
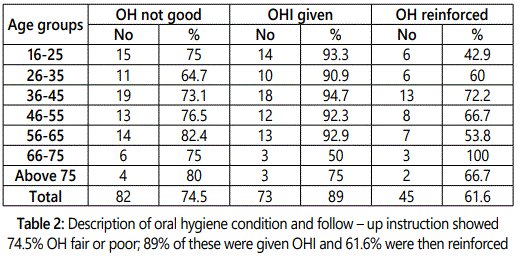
The analysed data which reflected into Table 2, illustrates that 65 to 80 percent of each categorised group did not have a good oral hygiene condition. Of those, approximately 90 percent of groups below 66 years old were given oral hygiene instruction, whilst only half and three-quarter respectively of the other two groups were shown how to take care of their teeth properly. Furthermore, the rate of oral hygiene reinforcement was far lower compared to the first instruction, excluding patients from 66 to 75 years old.
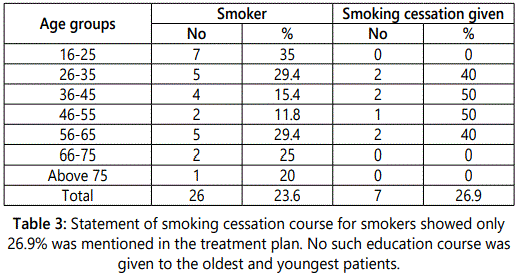
Concerning smoking cessation, neither the youngest nor the two oldest individuals were given any such course of therapy. Also, no more than half of the remaining age ranges were recommended professionally to quit smoking (Table 3).
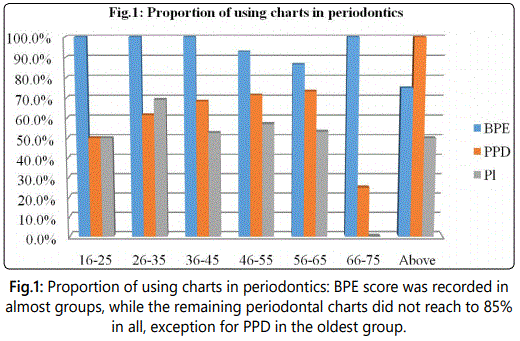
As shown in the Fig.1, the basic periodontal examination (BPE) was used absolutely in groups under 46 years old and group 66 to 75. It was used around 90 percent in the bands between 46 to 65 and 75 percent in the most elderly periodontal patients. The use of the periodontal pocket depth (PPD) was just around 70 percent in middle age ranges and just over 60 percent in 26 to 35. In addition to the presence of PPD in the periodontal younger groups, half of 16 to 25 did not use this. In the older groups, PPD was used all patients 76 and older; however, only one out of four (25%) of 66 to 75 – year – old patients having periodontal diseases was presented in this chart. Finally, the plaque distribution chart (Pl) was used 50 to 70 percent, with the highest rate of use being by the group 26 to 35.
A total of 842 appointments represented 842 treatment attempts to construct patient teeth and of those only 153 attempts (18.2%) resulted in a successful outcome.
There was a decreasing trend of successful outcomes when the age increased from 25 to 75 years old. In addition, the two patients over 75 with 100 percent success were discharged back at the first visit (table 4).

Discussion
The demographic results demonstrate valuable information which may be helpful for improving dental care.
The high disproportion findings in demand for 36 to 65 year - old patients and older groups which align with the results of the survey of the Office for National Statistics, may highlight that a number of issues are closely related to certain ages [1-2]. Are the issues related to the limitation of transport or general health for the elderly declared by Jablonski and Barber in 2015 [10]? Answering this question may play an important role in these cases which could help to improve the quality of dental health.
In addition, it was observed that there is a link between recording patients, educational level and financial abilities in relation to selecting treatments and changes in outcomes. Difficulties in payment for advanced treatment such as implants and complex treatments may also be considered as another factor that affect decided - upon treatment plans.
For clinical practice, providing equal services for priority patients that meet the requirement of the Barts Health can be an additional criterion. The late appointments recorded (Table 3.2), particularly in the cleft lip and palate and hypodontia circumstances, are raised by the audit, while in fact, they are available in the guidelines as the similar urgent scenarios.
It is also noted that the other disregards were of oral hygiene instruction and smoking cessation (see Table 2 and 3). The lack of such education courses as can be seen in the results could be the barriers to achieving successful outcomes, especially for the elderly when the literature claimed that their manual dexterity is not flexible [10].
Regarding periodontal cases (see Fig. 1), the basic periodontal examination (BPE) score shows that it mitigates the risk of non - compliance in the majority of groups, in accordance with the guidelines. In contrast, use of six – point periodontal charts and plaque distribution charts was still below the reasonable assurance level of Barts Health. Those important assessments being not available in the notes may lead to an incomplete mission. Hence, another study is necessary to find out why the deficiency occurs.
From analysing the deficiency of clinical steps, the major duty of further treatment should be minimising the number of failures in attending appointments in cohorts of elderly patients in order to encourage them to pursue procedures. In addition to this, GDPs must keep in mind that discharge at the first visit may be related to time concerns, disturbance for patients and misunderstanding of referral requirements in primary care.
Limitations of the Study
Data collection from a hospital involves a sample of patients from secondary care, and this cannot provide full information of the primary care. More severe status could be worked out in the first step; and hence, the population in this audit is not likely to be representative of all ratios between therapy types. The results may also be distorted as data collected retrospectively relies on the accuracy of the records. Additionally, the short period of study does not allow the authors to conduct a larger investigation from other sources such as data from other hospitals.
Suggestions and Future of the Project
Because of early described issues as well as unequal distribution of age groups, we would suggest that for 36 to 65, the primary care practitioners should give provisional aid to simplex cases in order to reduce the great proportion. A further study into the difficulties related to the limitation of transport impacting general health should be announced. Meanwhile, we suggest that the cost of treatments should not change the quality of health care, either by financially helping patients directly or having some funds to be able to be used for persons unable to pay.
Furthermore, a continuing professional development (CPD) programme targeting the regularly omitted factors such as high priority conditions, OHI, periodontal charts and smoking cessation could be established.
Conclusion
The process of treatment in restorative department audited retrospectively shows several issues in relation to patientʼs age, in response to which we suggest some points to enhance the quality of service. A decreasing overall trend of success rate in the cohorts of 26 to 75 probably illustrates the difficulties dental practitioners face with patientsʼ ageing. Another concern is related to the absences of clinical stages including high priorities, oral hygiene instruction, smoking cessation and periodontal charts in clinical practice. Therefore, the need for continuing professional development courses for GDPs and post - graduate students may be the key objective of the finding. Also, the clinical considerations that came up in this audit could act as a part of further studies. In the meantime, more research focusing on age - related factors is required, particularly for 35 to 65 as they make up the largest part. Further to this, the fact of collecting data from the hospital cannot mirror the initial oral condition when patients came to the GDPs prior to being referred to consultants.
Therefore, advance audit cycles may need to be carried out from the primary care phase with a number of subjects from various areas. This will more accurate identify issues and can be used to diminish the mistakes and number of attempts for both on – going and up - coming treatments while those patients age.
References
- Office for National Statistics. Population Estimates for UK, England and Wales, Scotland and Northern Ireland, Mid-2014. Office for National Statistics. 2015b.
- Office for National Statistics. National population projections, 2014-based Statistical Bulletin. Office for National statistics. 2015a.
- Muray CG. Advanced restorative dentistry – a problem for the elderly? An ethical dilemma. Australian Dental Journal. 2015; 60: 106–113. doi: 10.1111/adj.12289
- Mannino DM and Buist AS. Global burden of COPD: risk factors, prevalence, and future trends. Lancet. 2007; 370: 765–773. doi: 10.1016/S0140-6736(07)61380-4
- Petersen PE. The World Oral Health Report 2003: continuous improvement of oral health in the 21st century--the approach of the WHO Global Oral Health Programme. Community Dental Oral Epidemiology. 2003; 31 Suppl 1, 3–23. doi: 10.1046/j..2003.com122.x .
- Reginster J Y. The prevalence and burden of arthritis. Rheumatology (Oxford). 2002; 41 Supp 1: 3–6. doi: 10.1093/rheumatology/41.S1.3
- Blain H, Rambourg P, Le Quellec A, et al. Appropriate medication prescribing in older people. Rev Med Interne. 2015; 36: 677–89. doi: 10.1016/j.revmed.2015.03.016
- Jablonski RY and Barber MW. Restorative dentistry for the older patient cohort. British Dental Journal. 2015; 218(6): 337-342. doi: 10.1038/sj.bdj.2015.197


