Ontario Shores Centre for Mental Health Sciences, Canada
Psychiatric illness and its medical management carry significant risks for oral disease. Although mental illness is common, in many cases it is misunderstood, remains unrecognized, or is undertreated. Mental illness and the resulting disabilities create difficulties not only for the patient but also for oneʼs family and friends, not the least of which remains the highly stigmatized nature of the disease itself.
Understanding the type, severity, stage of mental illness, along with a patientʼs own mood, motivation and personal perceptions of oral disease and lifestyle can enhance the knowledge of dental professionals concerning this critical aspect of a patientʼs medical history and further illustrates how closely mental health and oral health are intertwined.
Mental illness must be viewed from a similar perspective as are other major diseases. Dental professionals should be aware of factors such as the reduced rates of compliance with dental treatment, reduced ability to access oral health care, the effects of various psychotropic medications on oral health including xerostomia, caries and periodontal disease and the potential interactions with drugs used in dental practice.
Patients with psychiatric illness often bring unique needs and differing priorities to a dental practice, and the dental health practitioner must in turn demonstrate patience, flexibility, empathy, and a non-stigmatizing attitude in caring for these individuals. Enhancing self-esteem and feelings of self-worth for those coping with a psychiatric illness can be a very fulfilling experience that can only serve to continue to break down the stigma surrounding this group of diseases.
Biography:
David Clark is Clinic Director of Dental Services at Ontario Shores Centre for Mental Health Sciences in Whitby, Ontario, and is also an Associate, Clinical Dentistry, Department of Oral Medicine, Faculty of Dentistry, University of Toronto. He obtained his MSc. in Oral Pathology at the University of Western Ontario in 1986 and is a Fellow of the Royal College of Dentists of Canada, the Pierre Fauchard Academy and Academy of Dentistry International. His hospital-based practice is devoted to the general dental care of individuals undergoing primary care for various forms of psychiatric illness co-existing with other medically compromising conditions.
1Department of Dental Medicine, Karolinska Institutet, Sweden
2Department of Laboratory Medicine, Karolinska Institutet, Sweden
3Rudbecklaboratory, Uppsala University, Sweden
4Department of Biosciences and Nutrition, Bioinformatics and Expression Analysis Sci Life Lab, Karolinska Institutet, Sweden
5Department of Oncology and Pathology, Karolinska Institutet, Sweden
6Radiumhemmet, Karolinska University Hospital, Sweden
7The Clinic of Oral and Maxillofacial Surgery, Karolinska University Hospital, Sweden
Ameloblastoma of the jaws remains the top difficult to treat odontogenic tumour and has a high recurrence rate. New evidence suggests that non-coding RNAs (ncRNAs) play a critical role in tumourgenesis and prognosis of cancer. However, ameloblastoma ncRNA expression data is lacking. Here we present the first report of ameloblastoma ncRNA signatures. A total of 95 ameloblastoma cases and a global array transcriptome technology covering >285.000 full-length transcripts were used in this two-step analysis. The analysis first identified in a test cohort 31 upregulated ameloblastoma-associated ncRNAs accompanied by signalling pathways of cancer, spliceosome, mRNA surveillance and Wnt. Further validation in an independent cohort points out the long non-coding (lncRNAs) and small nucleolar RNA (snoRNAs): LINC340, SNORD116-25, SNORA11, SNORA21, and SNORA65 as a distinct ncRNA signature of ameloblastoma. Importantly, the presence of these ncRNAs was independent of BRAF-V600E and SMO-L412F mutations, histology type or tumour location, but was positively correlated with the tumour size. Taken together, this study shows a systematic investigation of ncRNA expression of ameloblastoma, and illuminates new diagnostic and therapeutic targets for this invasive odontogenic tumour.
Biography:
Haleh Davanian completed undergraduate studies and major was Biomedicine. She continued with research in the field of Odontology, with major in Periodontitis. In early 2015 I received my PhD in Medicine, with the title Gene expression profile in Periodontitis. Today She work 50% as a postdoctoral researcher and 50% as a lecturer at the Department of Dental Medicine, Karolinska Institutet in Stockholm Sweden. The research topics She work with today is mainly in the field of cancer biology, microbiology as well as immunology are related to oral diseases.
Introduction: Endodontic therapy aims at eliminating the existing infection and also inhibiting re-infection. In spite of the standard treatment protocol followed, persistence of microorganism attributes to almost 30% of endodontic failure. Enterococcus faecalis is a commonly detected microorganism (range of 2.4 to 17.7%) in asymptomatic endodontic infections. For effective treatment strategies and outcome, identification and characterization of pathogens is imperative. The objectives were (i) to identify Enterococci genusfrom root canal infections in Bangalore Urban population (ii) to isolate E. faecalis by DNA isolation and gel electrophoresis (iii) to evaluate the antibiotic sensitivity of E. faecalis isolates to routine nine antibiotics.
Methodology: 50 patients with primary endodontic infection were randomly selected for the study. Following ethical clearance and patient consent, isolation and standard disinfection of concerned tooth. After gaining access, root canal was filed to disrupt the biofilm using 15k file. The samples were collected with charcoaled paper point and transferred to Amieʼs transport medium for microbial analysis. To identify Enterococci, the samples along with two standards (ATCC 29212 and MTCC 3159) were subjected to series of standard biochemical (gram staining, salt tolerance and bile esculin hydrolysis) and fermentation tests. The isolates were then subjected to DNA isolation and gel electrophoresis to identify E. faecalis. The antibiotic sensitivity of isolates were assessed against nine antibiotics by Zone of inhibition using a Hi Media scale. The transformed values by Fischerʼs method were statistically analyzed using AGRISTAT (version 6) software.
Results: 16 out of 51 samples (31 %) was identified as Enterococci. Only two samples belong to Enterococcus faecalis registering 3.97 % incidence. The gel electrophoresis of isolated DNA indicated genetical variance of one isolate.
All strains of E. faecalis exhibited identical sensitivity to the antibiotics evaluated revealing their similar genetic makeup. Samples showed intermediate sensitivity to Doxycycline hydrochloride except one. Gentamycin was effective in inhibiting the growth of all cultures. Linezolid exhibited resistance to the isolates.
Conclusion: With the limited literature on E. faecalis in Indian population using molecular technique, the present research findings was one of the earliest of its kind. E. faecalis was found in 3.97% of primary endodontic infections whereas enterococci showed incidence of 31%. The identification and characterization of pathogens is significant as they can cause failure of endodontic therapy as well severe systemic implications. Future line of research envisages for Nucleic Acid-based Research and Metagenomic studies of pathogens for effective treatment strategies.
Biography:
Madhu K S is an Assistant Professor in the Department of Conservative Dentistry & Endodontics, Faculty of Dental Sciences, Ramaiah University of Applied Sciences, Bangalore with more than 5 years of academic experience. She is currently pursuing her PhD on her area of interest “Molecular analysis of Endodontic Microflora “ at Ramaiah University of Applied Sciences, Bangalore. She has obtained her Bachelor of Dental Surgery degree from JSS Dental College and Hospital, Mysore, Karnataka in 2005 and Master of Dental Surgery from M R Ambedkar Dental College and Hospital, Bangalore in 2011. She has several national and international publications to her credit. She has presented several papers and poster in various national conferences. She has chaired a scientific session at a national conference-Indian Dental Conference, 2015, Bangalore, India. She is a Life member of Indian Academy of Conservative Dentistry & Endodontics (IACDE) and Indian Dental Association (IDA). She is Ex-Executive Committee member of IDA, Bangalore. She has attended numerous conferences, CDE programs and workshops. She has been resource person for several programs held at the university.
Bapuji Dental College and Hospital, India
This prospective single cohort study was conducted to evaluate the efficacy of a composite graft containing rhPDGF-BB+β-TCP (β-tricalcium phosphate) admixed with Xenograft, in the minimally invasive direct sinus augmentation of localised atrophic maxillary posterior ridges. Radiographic (CBCT scan) examinations were done at baseline, immediate post-operative and 6 months post-operatively and histomorphometry was performed 6 months post-operatively. A total of 17 patients (20 maxillary sinuses) with atrophic maxillary posterior residual ridges willing for the implant supported restorations were selected for this study, using consecutive sampling technique, from the out-patient Department of Periodontics, Bapuji Dental College & Hospital, Davangere (India). Surgical procedure was carried under strict asepsis incorporating stress reduction protocol. Direct sinus augmentation procedure was done under local anaesthesia where the lateral window was separated from underlying schneiderian membrane using the wall-off technique. A composite graft containing rhPDGF-BB+β-TCP admixed with deproteinzed bovine bone was used to augment the sub-antral compartment and the bony window was replaced back followed by a resorbable collagen membrane placement. Primary flap closure was achieved using polyamide sutures. An immediate post-operative CBCT was taken to ensure the intactness of schneiderian membrane. After 6-month healing period, a CBCT scan was taken and radiographic evaluation of healed grafted sinus. During the implant placement, a bone core was harvested one per treated sinus from the previous access window and histomorphometric analysis was done. On radiographic evaluation, the mean pre-operative bone height (H0) was 3.02±1.35mm, Post-graft bone height (H1) immediately after the augmentation was 15.18±2.52mm and post-operative bone height (H2) after 6 months observation period was 14.79±2.30mm. The immediate post-graft volume (V1) was 1106.10±398.84 mm3 and post-operative volume (V2) was 1086.95±396.86 mm3. There was significant gain in the residual ridge height over 6 months from the baseline, while there was no significant change in the gained height or volume of the grafted sinus during this period. Histological evaluation revealed the bone bridging and bone regenerative efficacy of the graft material with vital new bone formation, residual graft and non-mineralized tissue of 19.17±2.63%, 33.02±7.01% and 47.38±6.72% respectively and the implants placed in the augmented showed 100% survival rates. The preliminary data obtained from this study, with in its limitations, indicates that this minimally invasive sinus augmentation with the composite graft could be efficiently used for the implant site preparation of posterior maxillary atrophic ridges. A predictable and promising bone gain and integration of the implant was observed with this procedure.
Biography:
Sai Divya Gayatri Pamidimarri, is a resident pursuing Periodontics from Bapuji Dental College and Hospital, Davangere. With themotto of spreading smiles and a ray of interest in exploring dentistry abroad she attended an international student exchange programme during September 2011 in University of Medicine and Dentistry New Jersey (Now Rutgerʼs University), Newark, USA. She was one of the winner (second prize) of the national essay competition conducted by Elsevierpublications in 2016 for the inaugural of 12th edition Carranzaʼs Clinical Periodontology textbook in India. She has two national papers published under specialty of Periodontics. Besides these, she has a couple of clinical studies one of which is to be presented in Dental-2017 Conference, UAE.
King Saud University, Saudi Arabia
Introduction: The adhesion between the reline material and the denture base to form durable bond is needed for the comfort and function of the patientsʼ prosthesis. Some authors recommend denture surface treatment prior to applying the reline material to overcome the problem of separation of relining materials.
Objectives: The aim of the study was to evaluate the effect two different surface treatments on the tensile bond strength of three different resilient relining materials bonded to urethane dimethacrylate (UDMA) light activated resin denture base and to detect the mode of debonding between the resilient lining materials and the UDMA.
Materials and Methods: A total of 108 dumbbell-shaped specimens UDMA resin specimens were prepared. Specimens were divided into three group. The first group was the control with untreated surface. The second group was treated with Al2O3 size 50μm while the third group was treated with acetone for 30 seconds. Furthermore, these group were divided to three subgroup according to relining materials used, heat-polymerized acrylic (Vertex Soft), self-polymerized acrylic (Perma Soft) and self-polymerized silicone (Bosworth-Dentusil). All specimens were subjected to thermo cycling (1500) cycles for 24 hours, the temperature ranging from5_55°. Then specimens were attachedto instron by a custom jig and subjected to a tensile force at a crosshead speed of 5 mm/ min until debonding occurred. The data was analyzed statistically by Two-way ANOVA and one way ANOVA test for detection of the difference within the group and between the groups.
Results: Two-way ANOVA showed that the surface treatment and the different relining material had significant effect on the tensile bond strength. Perma Soft had the higher tensile bond strength than the other groups (2.465 ±0.261 Mpa) and it was increased 30% more with acetone surface treatment. Sand blasting surface treatment increased the tensile bond strength for Bosworth-Dentusil and vertex soft but not statistically significant. Bosworth-Dentusildebonded in adhesive, cohesive and mixed failure mode. The other two materials debonded adhesively only.
Conclusion: this study showed that Perma Soft relining material is best option for relining UDMA denture resin, and its tensile bond strength was increased 30% more with acetone surface treatment. Each relining material react in different manner than the other for each surface treatment.
Biography:
Kareimh Hadhiah is from Kingdom of Saudi Arabia graduated from King Saud University with bachelor degree and continue her postgrade study in prosthodontics in the same university, she work in the ministry of health in the eastern region, Dammam medical complex.
1Zayed University, UAE
2University of Bergen, Norway
3University of Science and Technology, Sudan
Background and Objectives: The microbial profile of aggressive periodontitis patients is considered to be complex with variations among populations in different geographical areas. The aim of this study was to determine the prevalence of four putative periodontopathic bacteria (Aggregatibacteractinomycetemcomitans, Porphyromonasgingivalis, Tannerella forsythia, Treponemadenticola) and two periodontal herpes viruses [Epstein-Barr virus-1 (EBV), human cytomegalovirus (HMCV)] in subgingival plaque and whole saliva of Sudanese subjects with aggressive periodontitis and their family members and to compare the results with those of healthy controls.
Material and Methods: The study group consisted of 122 subjects, 17 aggressive periodontitis patients, 17 periodontally healthy controls (14-19 years of age), 54 family members of the cases and 34 family members of the controls. Whole stimulated saliva and pooled subgingival plaque were collected and analyzed for detection of bacteria and viruses using loop mediated isothermal amplification (LAMP).
Results: Prevalence of subgingival A. actinomycetemcomitans, HCMVand P. gingivalis were significantly higher among aggressive periodontitis patients than periodontally healthy controls. Co-infection with A. actinomycetemcomitans, HCMV and/or EBV-1 was restricted to the cases and their family members. Pooled subgingival plaque showed significant higher prevalence of A. actinomycetemcomitans and P. gingivalisthan whole stimulated saliva in this population (p=0.0001, p=0.04). Increased risk of aggressive peritonitis was the highest when A. actinomycetemcomitans& was detected together with EBV-1(OD 49.0, 95% CI2.5-948.7, p= 0.01) and HCMV(OD 39.1, 95% CI 2.0 - 754.6, p= 0.02).
Conclusions: In Sudanese patients, A. actinomycetemcomitansand HCMV were the most associated test pathogens with aggressive periodontitis. Saliva may be useful as an alternative sampling tool for selected pathogens. However, parallel subgingival sampling is recommended for A. actinomycetemcomitansand P. gingivalis.
Biography:
Elamin is an assistant professor at Zayed University, United Arab Emirates. She earned her Bachelor of Dental Surgery (BDS) from Khartoum University, Sudan. Dr. Elamin obtained her PhD from Section for Microbiology and Immunology, The Gade Institute, University of Bergen, Norway. Dr. Elaminʼs research mainly focuses on the microbial etiology of aggressive periodontitis, specificallyintra-species phylogenetic differences and virulent clones of Aggregatibacteractinomycetemcomitans associated with the aggressive periodontitis. In addition she is interested in bacterial-viral interactions in oral cavity.
Her main research interest is childrenʼs and adolescents oral health. Mainly examining the etiology of aggressive periodontitis and intra-species phylogenetic differences and identify virulent pathogenic clones of Aggregatibacteractinomycetemcomitans associated with the disease. Dr. Elamin is also interested in pre-school oral health and associating it to dietry habits and parenting styles.
Kathmandu University School of Medical Sciences, Nepal
Complete regeneration of the periodontium remains an elusive goal with current treatment modalities. A number of emerging technologies are being examined that can improve the outcome of periodontal regeneration. These include the application of protein and peptide therapy, cell-based therapy, genetic therapy, application of scaffolds, bone anabolics, and lasers. As emerging technologies, by definition, most of these therapies lack high levels of evidence. Currently, there are numerous human clinical trials in varying stages of completion that are attempting to delineate the best applications of the emerging therapies.
Emerging technologies are presenting options to hopefully improve the outcomes of regeneration in challenging clinical scenarios. Cellular allografts represent a current technology in which cells and scaffolds are being delivered directly to the periodontal lesion. Recombinant human fibroblast growth factor 2 and teriparatide (parathyroid 1-34) have each been tested in controlled prospective human randomized clinical trials, and both have been shown to have potential for periodontal regeneration. These examples, as well as other emerging technologies, show promise for continued advancement in the field of periodontal regenerative therapy.
At present, there are indications that emerging technologies can be used successfully for periodontal regeneration. Case reports and clinical trials are being conducted with a variety of emerging technologies. However, many are yet to be approved by a regulatory agency, or there is a lack of evidence-based literature to validate their expanded use. This presentation will review the existing modalities of the periodontal regeneration and its future perspective.
Biography:
Manoj Humagain completed his MDS, at Kathmandu University, 2008 and BDS, Gauhati University, India 2003. Presently he was associate professor in Kathmandu University School of Medical Sciences.
Institute of Medicine, Nepal
Objective: The aim was to determine and compare the shear bond strength of bracket-bonding system cured with Light emitting diode and Halogen based light curing unit at various polymerization times.
Methods: Ninety six human maxillary premolar teeth extracted for orthodontic purpose were divided into four groups, according to the light-curing unit and exposure times used. In the Halogen group, the specimens were light cured for 20 and 40 seconds. In the LED group, the specimens were light cured for 5 and 10 seconds. Stainless steel brackets were bonded and stored in distilled water at 37°C for 24 hours and then submitted to SBS testing.
Results: The highest mean SBS was obtained with the Halogen 40 seconds (18.27MPa) followed by Halogen 20 seconds (15.36 MPa), LED 10 seconds (14.60 MPa) and least with LED 5 seconds (12.49 MPa) group. According to analysis of variance and Tukey multiple comparison test, Shear bond strength of Halogen 20 seconds group was not significantly different from other groups. LED 5 seconds group was not significantly different from LED 10 seconds group. Whereas Halogen 40 seconds group was significantly different from LED 5 seconds & LED 10 seconds group.
Conclusion: Polymerization with both Halogen and LED resulted in shear bond strength values which were clinically acceptable for orthodontic treatment in all groups. Hence, for bonding orthodontic brackets, photoactivation with Halogen for 20 seconds and LED for 5 seconds is suggested.
Keywords: Shear bond strength, Halogen curing light, LED curing light, Polymerization time
Biography:
Sanjay Prasad Gupta completed his BDS (Bachelor of Dental surgery) from Universal College of Medical Science, Bhairahawa, Nepal in 2009 (2003-2009). Post graduation: MDS (Master of Dental surgery) in Orthodontics from Maharajgunj Medical Campus, Institute of Medicine, Kathmandu, Nepal in 2013 as a first batch of Tribhuvan University (2010-2013). First rank holder in Post graduate entrance examinations for MDS in Institute Of Medicine-Government Institute in 2010. Present Position was Assistant Professor in Orthodontics & Dentofacial Orthopedics unit, Faculty of post graduate MDS programme, Department of Dentistry, Institute of Medicine-Tribhuvan University teaching Hospital, Maharajgunj, Kathmandu, Nepal.
University of Alberta, Canada
A toothache of non-odontogenic origin is pain felt in a tooth with no clinical indication of pulpal or periodontal involvement. From the total dental visits with a chief complaint of a toothache, 3% are of a non-odontogenic origin and 9% are a mix of odontogenic and non-odontogenic origin (Yatani et al 2014).
Non-odontogenic toothaches may represent a wide variety of pain types: neuropathic pain such as trigeminal neuralgia, neurovascular conditions like migraine headaches, visceral pain such as sinusitis and/or a musculoskeletal pain such as myofascial pain. Case reports of headaches mimicking toothache have also been published. However, toothache of non-odontogenic origin may also be due to a more life threatening disease like cancer and/or a heart attack. Incorrect diagnosis of these conditions usually leads to unnecessary dental procedures: root canal therapy and/or dental extractions. The end result is a patient experiencing no change or an aggravation of the pre - existent toothache. In some cases, due to the extensive attempts to palliate the pain, the patient ends with complications including pain in a larger area.
At the end of this presentation, the attendee should be able to learn the main clinical features of a toothache of non-odontogenic origin, and how this pain can be mistaken as a true toothache. Clinical cases of mistaken toothache of odontogenic and non-odontogenic origin will be presented. Differential diagnoses for each case will be discussed. Treatment recommendations and the need of referral to other healthcare professionals will also be outlined.
Biography:
Hernández graduated from Dentistry at the University of Concepción, Chile (1992). She completed her TMD/Orofacial Pain Residency (2002), Masters in Medical Sciences (2003) and, Doctor of Dental Surgery Degree (2005) at the University of Alberta, Canada. She became a Diplomate of the American Board of Orofacial Pain, (2004) and a Fellow of the American Academy of Orofacial Pain (2005) in which she is now a council member. She belongs to several other professional pain organizations. Currently, Dr. Hernández maintains a busy private practice; she is also an Assistant Clinical Professor at the Oral Medicine Graduate Program, University of Alberta.
Objectives: The aim of this study is to evaluate the color changes and surface roughness (Ra) of different types of composite after their immersion in different sport drink types for 7days, 1 month, 3 months as well as 6 months.
Materials and Methods: Sixty specimens were made from different composites (Filtek Z250, Vertis Flow and Spectrum). Each specimen was cured for 20 sec. Color measurements of each specimen were performed with Color Eye system at baseline and at 7days, 1, 3 and 6 months of immersion in the sport energy drinks (Code Red, Red Bull and Bison). Another Thirty six disc-shaped specimens for surface roughness (Ra) determination using a noncontact 3D-optical-profilometer. Baseline and after immersion in the sport drinks for 6 months were determined. Surface topography (Ra) and color changes (DE values) of the groups were recorded and statistically analyzed.
Results: Variations in the composition of different sport drinks media did not affect the color changes of composite groups. The effect of time showed that the color changes of all composite tested are directly proportional to the increase in time. Surface roughness (Ra) showed insignificant difference between the groups except for the Spectrum when immersed in code red the Ra increased.
Conclusion:1. All resin composite tested showed color changes when immersed in sport drinks solutions. 2. The color changes is directly proportional to the time of immersion of resin composite. 3. Vertise Flow showed the least color changes by time followed by the Filtek Z250 while the Spectrum showed the highest color changes.
Biography:
Ihab Moussa was graduated from Cairo University with a very good grade, assigned as a demonstrator in 1987. He had his Master`s Degree in Biomaterials by 1992, and his Ph.D. in Biomaterial Sciences by 1999. He was assigned as lecturer in Menia, Suez Canal and 6th October Universities. He was assigned as Head of Biomaterial Division in 6th October University. At 2005, he had his Associate Prof. Degree then affiliated to work at King Saud University till present.
Dubai Health Authority, UAE
The aim of this study was to investigate the caries prevalence of 3-5 year old children, attending private school in Dubai. Caries were recorded according to the clinical criteria set by WHO in 1987. Sample size at the age of 3, 4 and 5 was 273, 1205 and 1479 children where the mean dmft values found were 0.90 (2.18), 1.50 (2.73) and 1.72 (2.85) accordingly. The dmft for the total of the sample was 1.55. This is the first caries prevalence study in Dubai recording caries for 3 and 4 year-old children.
Introduction: Dental caries is a multi-factorial infectious disease, which can affect children and adults at any age. Progress of dental caries is faster in primary dentition, as a result of the thinner dental structures both enamel and dentine, along with deferences in mineralization of the primary teeth. Until now there is no data on caries prevalence in 3 and 4 year old children in Dubai and the last available data for 5 year old children date more than a decade ago. Many countries have showed a decline in the dmft values over the years.
Materials & Methods: The sample consisted of 2957 children, (1527 males and 1430 females), 3-5 year-old, attending private schools in Dubai, participated in this study.
Children were screened for caries by three licensed, calibrated dentists using the WHO 1987, clinical examination criteria.
Results: Mean dmft for 3, 4 and 5 year-old children was 0.90 (2.18), 1.50 (2.73) and 1.72 (2.85) respectively.
Conclusions: 3-5 yo preschoolers of Dubai schools exhibited high prevalence of caries with dmft from 0.90 to 1.72
Biography:
Maitha obtained her DDS from Ajman University of Science and Technology back in 2005, in 2015 she got her Masters Degree in Pediatric Dentistry from the European University College in Dubai. Dr. AlKhayat currently practicing as Pediatric Dental Specialist Registrar in Dubai Health Authority
-Dubai.
Genome & Hi Care Dental & Skin Care Clinics, Saudi Arabia
Dentistry and its Industry, a unique profession that is considered & thought of by many as a negative nightmarish force that they have to deal with someday in life, just like a thorn in every rose waiting to be touched. A mandatory fear they will face one day. The repelling attitude expressed by clients & patients is very well established in almost all communities. In movies we are the jock & in real life we are the devil that they are compelled to befriend yet, after pain subsiding or concluding a Smile Make-Over (SMO) we as Dentists all of a sudden become their savior & their best friend!! WHY is that?
Biography:
A Smile Designer where many trends become one. Created (Digital Tooth-Dental Tattoo) program. Patent applicant of Rubtrix - Cottedge & Quick Paste & Brush. B.D.S. from Bangalore University (India) (2000) PG in Aesthetic & Cosmetic Dentistry (Smile Design) UB-NY (USA) & India (2003/4) PMP from Dar Alruʼa (KSA) (2010) HCM course from IHMF (2016).
Dubai Health Care City, UAE
Orthodontic treatment is a long procedure which requires about 18-24 months of treatment. This long duration of treatment can cause a variety of side effects like alveolar bone resorption, root resorption, caries and decrease in the compliance of the patient.
Therefore finding a method to shorten the treatment period remains one of the big challenges lying ahead of orthodontics. Nowadays, the versatility of low-level laser therapy has been extensively applied in clinical practice. In particular, in the field of orthodontics; it has been used for the alleviation of orthodontic pain and acceleration of orthodontic tooth movement. The purpose of this study was to investigate whether the use of photobiomodulation therapy (using OrthoPulse machine from Biolux) combined with conventional fixed orthodontic appliance will result in reducing overall treatment time by accelerating maxillary and mandibular anterior alignment rates and reducing patient pain perception scores during the treatment.
Biography:
Nour Alokla completed Diploma in dental laboratory technology as Dental technician from Damascus University in 2006, after that She studied Dentistry at Al Kalamoon University in Syria and graduated in 2011. She obtained my Master degree in orthodontic and dentofacial orthopedic from European University college. She am interested in acceleration of the tooth movement during orthodontic treatment researches. Currently working as full time orthodontist in Dubai Health care city.
The Dental Studio, Hollywood Smile Clinic, UAE
In diagnosing patients with possible TMD it is necessary to aknowledge the great variety of causes of orofacial pain and dysfunction. The treatment of the temporomandibular joint disorders can vary from simple self – care techniques to complex multidisciplinary procedures including the splint therapy which is one of the first stops in TMJ disorder treatment. It is very important to have an idea about the functional anatomy of the TMJ, understand the musculo-skeletal stable position of the condyle in the fossa, The understanding of the CPI and the interpretation of the CO/ CR discrepancy after mounting on the articulator, and the map of pain of ROCABADO, in addition to these diagnostic tools we need to understand the radiological diagnosis of the TMJ, the different stages of degenerative joint disease and disc pathology progression. The good understanding of the TMJ and the relations between the seated condyle and the stable occlusion lead us to the right way to treat TMD patients with occlusal interferences. In this lecture weʼll discuss the diagnostic tools that we use in TMD cases, occlusal analysis and treatment options that affect the occlusion and maintain the condyle in a musculo -skeletal stable position with the use of the centric splints and the importance to use the distraction splints with the help of the physiotherapy
Biography:
Firas Hamzeh started his postgraduate training program at the university of Nantes -France in 1994. He obtained his first certificate of advanced studies in dental materials used in dentistry in December 1995 and his certificate of high studies in dento facial orthopedics in 1997. At the same university, while he was studying this certificate he started his diploma in orthodontics in 1996 and he obtained his Masters in 1999. Hamzeh moved to Dubai in 2000 and he started his practice in the private sector, he started to use the self ligating brackets with the Damon system in the year 2004 and he continued his advanced training with Damon system with best ormco”s educators then he became an exclusive user of Damon system in his practice Since the year 2008. Heʼs one of KOL with Damon system and Insignia in the middle east. Firas Hamzeh had advanced knowledge in Orthodontic digital solutions. Hamzeh is recognized as an early adopter and advocate of innovative orthodontic systems including aligners and digital custom brackets INSIGNIA BRACES (he was also the first Insignia user in the middle east ) his first case was in 2012. In addition to being KOL ( key opinion leader ) for ORMCO and an international Ormco speaker on INSIGNIA the Damon system. In addition to this he loves to treat the TMD cases because he has been following a lot of training program in occlusion and TMJ including the ROTH Williams philosophy. He completed his postgraduate training program in TMJ, occlusion and orthodontics – San Sebastian, Spain. Since 2013 heʼs treating patients with temporomandibular joint disorders.
Dr. Hamzeh has presented in so many international orthodontic conferences, his main focus in his lectures is the digital orthodontics.
Orthodontist, UAE
The orthodontic treatment of a 16 years old patient with Crohnʼs Disease (CD) is reported. The patient was diagnosed since the age of 10 years with CD and was undergoing therapy with immunosuppressant agents. She had a severe high-angle skeletal Cl II with gummy smile and a retruded profile. Treatment with 2 posterior and 2 anterior mini-screws with 4 premolar extractions was conducted. Oral breakouts of the disease were triggered by the orthodontic treatment that had to be progressively molded to fit the patientʼs health conditions. A counter-clockwise rotation of the mandible and enhancement of patientʼs profile were achieved. Gummy smile was fully corrected. The interactions of the therapy with immunosuppressant agents, and oral breakouts of CD with treatment progress, results and duration are discussed.
Biography:
Hajjis a specialist in Orthodontics and Dento-facial Orthopedics. She is currently working as lead orthodontist in Palmira Specialized Medical Center, Abu Dhabi, UAE, while also operating a private practice in Lebanon. Dr. Hajj graduated in 2012 with a Masters in Orthodontics from the University of Saint Joseph Beirut, Lebanon. She was on the Deanʼs Honor List throughout her academic career and was recognized with the highest honors award upon graduation for being on top of her class during the complete dental program. Dr. Hajj also received a Diploma in 3-Dimensional Imaging in 2013 from the University of Toulouse III-Paul Sabatier, Toulouse, France. She was awarded the “Edgard Chaar International Prize of Periodontology” in 2008, Beirut, Lebanon. Dr. Hajj areas of expertise include mini-screws, aligners, 3-D Imaging, fixed and removable orthodontics.
Champions-Implants GmbH, Germany
Autologous bone grafting, biomaterials, invasive techniques, lengthy procedures, etc. are often necessary when traditional implants are selected to reach the therapeutic goal. In Europe, beginning in 1995, Armin Nedjat and Ernst Fuchs-Schaller developed an innovative, minimally invasive surgical approach based on ‘Bioactive Containerʼ which supports the ‘Power of the Natureʼ also in narrow and atrophic jaws. The results of a study of 550 patients operated on between 1995 and 2015 reveal the validity, the long-term safety, and the excellent cosmetic outcome obtained with this MIMI-Flapless I - V protocols, which is also applicable when bone grafting has failed or has proven insufficient. Minimally invasive procedures without mucoperiostal flaps are the future in our daily work in the clinics!
Biography:
Armin Nedjat, German, obtained his DDS (1993) in Frankfurt/ Main, Specialized in Esthetic Dentistry 1997 Certificate of specialization in Implantologie DGZI (1999), Certificate of specialization in Implantologie ICOI as a ‘Diplomateʼ (2000) and PhD in Dental Surgeryin several universities worldwide. He has been in private practice of Implantologie and prosthodontics since 1994 with more than 23.000 implants in Flonheim/ Frankfurt. He worked as well in Paris, Boston, San Antonio/ Texas, Palma/ Mallorca. Currently, since 2013, he is the Scientific Chairman and first president of the VIP-ZM (Association of innovative practicing dentists in Germany). His main topic is the MIMI-Flapless procedure in Implantologie: This “Key-whole”-surgery without flaps also in narrow bones won the ‘Best Innovation in Medicineʼ in Dubai 2013. He is the founder and CEO of Champions-Implants GmbH, one of the largest implant systems in Germany/Austria. He is anactive member of the DGZI, DGI, BDIZ, DGOI, ICOI, DGL, and DGP. He holds several patents, in particular for materials and instruments for the MIMI-Flapless procedures. Dr. Nedjat lectures internationally and has authored over 250 publications in German, French and English.
European University College, Germany
Scientific Paper discuss the differences ‘in function and aesthetic prospectiveʼ between three restorative materials “Composite, Gold, Ceramic” and the parameters of selection.
Which on of the three Materials serve as a best filling material based upon there properties ? which one of them is the best aesthetically and functionally in dental practice. what are the factors that affect the selection of restorative material ?
Results: Composite fillings are strong, but may not be as hard wearing as amalgam fillings. Gold inlay and onlay can be used in most areas of the mouth. Gold is the most long-lasting it does not tarnish and has great strength. one disadvantage of Gold restorative Material is that, is made in a laboratory, an impassion of the prepared one which make it uncomfortable choice for most patients, as well as its expense.
Porcelain inlays with the help of digital technology (called CADCAM) which can be used to design and prepare perfectly fitted porcelain inlays in just one or two visits. Porcelain can be hard wearing and long lasting with superior colour matching to tooth which making it quite expensive.
Conclusion: We have come a long way in dentistry with different materials that have been offered to patients, from amalgam, which is not used anymore to Gold, to Resin-based filling materials and laser cavity preparation and one visit Onlay and inlay!
The selection of an appropriate restorative material depends on the case selection. several parameters must be taken in consideration, like “aesthetic, function durability, and skills of practitioner, as well as the financial ability of the patient”.
Biography:
Huda Masoud is a general dentist, Dedicated, energetic licensed D.D.S with 4 years experience with vast knowledge of clinical procedures and medical and dental terminology. Prosthodontics, Endodontics, Periodontics and cosmetic Dentistry expert. Highly motivated, dedicated and committed to providing the best possible care with the best possible service. Experienced in all varieties of procedures desired in a professional family.
She have studied in Dental school for 5 years and made an internship in her home town Benghazi\Libya, after that she worked for about year and half at private clinic there until she moved to Dubai in 2013 and made her Diploma in advanced dentistry in European Dental College, Dubai, UAE. Before that she volunteered with the ‘Red crest’ as general dentist for homeless and Handicapped. In 2015 she moved to Germany to achieve more educational goals. She worked now as a general Dentist in one private clinic in Hamburg, Germany.
Uppsala University, Sweden
Aim: The aim of this studies was to investigate the prevalence of alveolar bone loss (ABL), manifest caries and the influence of socioeconomic factors and smoking using data from four cross-sectional epidemiological studies in an adult population, 35-85 year of age in 1983, 2003, 2008 and 2013.
Material and Methods: A random sample of 1012-2243 individuals answered a questionnaire regarding e.g. socio-economic, tobacco habits and oral hygiene habits. A clinical examination was performed including radiographs. Severity of ABL was classified into three categories depending on the amount of bone loss measured on radiographs; no; moderate or severe ABL and manifest caries lesions was registered. Complete data in the different study years were obtained from 78% - 52%.
Results: The prevalence of severe ABL the different study years was 7% in 1983, 5% in 2003, 10% in 2008 and 7% in 2013. The increase between 2003 and 2008 was statistically significant as well as the decrease between 2008 and 2013 (p<0.05).
The prevalence of moderate ABL was 45% in 1983 and decreased significantly to 16% in 2008 but increased significantly to 35% in 2013 (p<0.05).
Calculus seen on radiographs increased significantly from 13% in 2003, 22% in 2008 and 32% in 2013.
The proportion of individuals with at least one manifest caries lesion was 58% in 1983 and decreased significantly to 34% in 2008 and was in 2013 33%. In the age group 85 years, the mean number of decayed surfaces was somewhat higher in 2013 than in 2008 (2.4 vs. 1.2).
After adjustment for age, number of teeth and a number of socioeconomic factors, current/former smoking was the variable that correlated significantly with ABL in all study years (odds ratios ranging from 2.53-3.22). Manifest caries lesions was, after adjustment correlated with irregular dental visits, financial limits for dental care, smoking, low education, daily medication and male gender (odds ratios ranging from 1.24-2.03).
Conclusion: During this period of 30 years ABLand manifest caries decreased significantly. However, between 2008 and 2013 a significantly increase in ABL was found and the positive trend in a decrease in manifest caries ceased. The amount of calculus visible on radiographs increased significantly between 2003 and 2013. Socioeconomic factors was found to have limited impact on ABL but was correlated to manifest caries. Smoking was the overall strongest factor associated with ABL and was also correlated to manifest caries.
Biography:
Kristina Edman, RDH since 1983. I have the past 13 years been working at the Center for Oral Rehabilitation, Falun, Sweden, a specialist clinic in periodontology. My special interest is epidemiology of oral health, in particular periodontitis and dental caries. In April 2016, I defended my thesis
“Epidemiological studies of Oral Health, development and influencing factors in the county of Dalarna, Sweden 1983-2013”.
Helmis Specialized Dental Center, UAE
The use of dental implants to restore missing teeth has steadily increased over the past three decades. It is perhaps not surprising, then, that the number of implant-related complications has grown as well. Numerous clinical studies involving dental implants have revealed encouraging outcomes; however, there is an element of risk associated with all clinical procedures, and these encouraging results may have given rise to unrealistic expectations. Despite careful planning, there is always a potential for surgical complications. Nevertheless, carrying out routine tasks with care and attention, choosing minimally invasive techniques when indicated, recognizing evidence of a developing problem, and giving prompt attention will reduce postoperative and prosthetic complications. The successful outcome of any surgical and or prosthetic procedure requires attention to a series of patient-related and procedure-dependent parameters. Sound knowledge of surgical anatomy and experience and training in the prosthetic dentistry and implantology are important prerequisites for predictable implant surgery. Also, adequate presurgical planning, good primary stability, a sufficient healing period, and detailed postoperative instructions are all factors that play a vital role in the success of dental implant surgery and osseointegration. Aging, changing health conditions, wear and tear, and inadequate professional maintenance are important variables influencing prognosis. Some hints that we can follow will avoid us many unwanted future complications.
Biography:
Helme Altaee, a consultant maxillofacial surgeon and dental implantologist. Post Doctorat Degree in Dental Implantology, Athens/Greece-January 2013. Ph.D Dental Implantology and biomaterials, 2004, University of Athens-Greece (1999-2004) with grade Excellent. High Diploma Degree in Maxillofacial Traumatology and Corrective Orthognathic surgery Dept. of Traumatology, AglaiaKyriakou Hospital (Athens-Greece, 2000-2003). M.Sc. Oral and Maxillofacial Surgery, 1992, Dentistry College-University of Baghdad (1990-1992) with grade Very Good. Bachelor of Dental Surgery (B.D.S), 1987, Graduated from Dentistry College-Mosul University, Iraq (1983-1987), Rank 1st with Grade Good.
Ajman University, UAE
Early in the recorded History there were references to dental variations and to the role that orderly transition of the primary to permanent dentition plays in normal development; Celsus observed in 25 B.C. That over retention of primary teeth could Cause Displacement of developing permanent teeth and that finger pressure seemed to help guid the permanent tooth into place after the primary tooth was removed, it is accepted that normal primary dentition and a normal transition from the primary to permanent dentition are necessary to establish a normal adult occlusion.
In the past, children are to begin orthodontic treatment when they reach age 12 to 14 years since all the permanent teeth have erupted by this time. Most dentist extract a tooth to correct bite problem or teeth crowding. However, according to the American Academy of Orthodontics, all children should be brought to the dentist for proper orthodontic assessment by age 7 when the first set of permanent molars had erupted. A prime example of preventive treatment involves space maintenance from premature loss of teeth. Depending on the clinical situation, several techniques can be used to maintain space; The orthodontist who has a much better conception of the possibilities of the prevention of malocclusion unfortunately does not see his patients until the case is ready for corrective measures rather than preventive. Treating children at much earlier ages, say between 7 to 11 years, will take advantage of the childʼs continuing growth and they are more compliant and receptive with treatment at this age.
With interceptive orthodontics, fewer teeth are extracted and there are better results, early Interceptive orthodontics will use patient growth to get best outcome and limit comprehensive face of fixed orthodontic treatment.
For a dentist seeing a young patient with malocclusion the first question is wether orthodontic treatment is needed. if so, the next question is: when should it be done?finally, who should do it? Dose this patient need referral to a specialist?
In this presentation we will cover our current understanding of preventive and interceptive orthodontics; indications, limitations and current procedure done under both categories. Referral concept will be discussed with great emphasis on day to day clinical scenarios that will face general dental practitioner, an example of that patients presenting with posterior or anterior cross bite, impacted teeth and space loss due to premature loss of primary counterpart.
Management of oral habits i.e., (thump sucking, mouth breathing) is essential toward normal development of both dental arches and dentition; ectopic eruption of teeth, supernumerary teeth and delayed eruption all of the above mentioned conditions come under title of interceptive orthodontic treatment which should be an established concept in a successful dental practice.
Understanding normal growth and development of dentitions is key factor in understanding preventive and interceptive orthodontic Treatment; The three major factors involved in development of dentition are Eruption, Drift and Equilibrium, will be covered in the presentation, knowledge of some of the causes of the development of malocclusion and the interceptive measures that may be undertaken during development to limit or reduce the severity of the malocclusion, The rationale and limitations of these procedures will also be discussed.
Mosul University, Iraq
Introduction: magnetic resonance imaging have been used nowadays as one of the accepted tool for diagnosis, estimation, and evaluation of many of human been disease; in dentistry, many of prosthodontics patients and "maxillofacial-prosthesis" patients may fall under the category who might be subjected to routine "MRI" check-up either for follow-up of certain disease or cancer patient for determination the degree of healing or metastasis, thus, there has been growing interest in the research of the possible effect of "MRI" procedure on different component of "dental appliances" wears by those patients and one of these components is "heat cured acrylic resin".
Aim: the aims of this study were to evaluate the effects of "magnetic resonance imaging" on mechanical (tensile strength, hardness) physical (color change) chemical (FTIR, NMR) properties at different periods of time exposure.
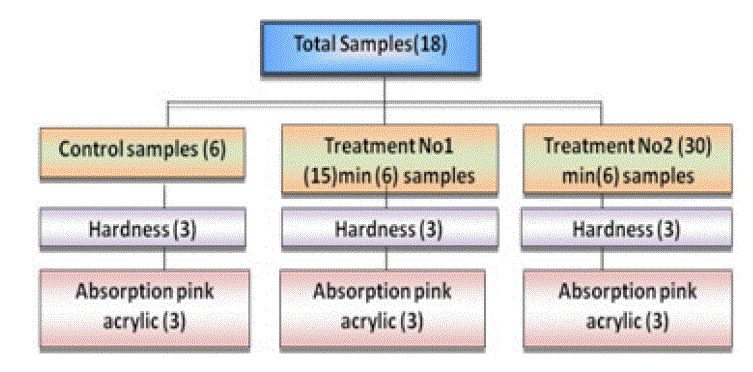
Material and Methods: total samples of (454) were prepared from acrylic based heat cured denture material, which divided into two main groups "Clear, Pink", each main group was subdivide, into four groups according to exposure to "MRI" control;(5,15, 30) minute each of the four sub-groups undergo different tests" tensile strength, hardness(Rockwell) test, dimensional accuracy test, color change by spectrophotometery, surface roughness, water sorption, residual monomer release "FTIR" and "NMR".
Conclusions: it was concluded that exposure to "MRI" at different periods of time lead to altering of some physical properties at different level of significant with the exception for one to two experiments water sorption and residual monomer which showed less significant than other tests done. Also, FTIR and NMR tests demonstrated a change in vibration of bonds between two, atoms but without rotation of molecule without alter the main chemical structure of material.
Biography:
Ahmed I. AL-Khyet is an Assistant lecturer of prosthodontic dentistry at Mosul University, Iraq. He has Msc. degree in prosthodontic dentistry, he published more than 8 researches papers in national and international academic journals, authored 1 book. He has expertise in Oral-health and dental field. His specific work deal with effects of (MRI) on polymers and dental products, his M.Sc. Thesis consider the 1st one all over middle east, and available on more than 10 search –engine on internet.