Case Report
Dual Pathology in a Single Nasal Cavity-A Clinical Case Report
Department of ENT and Head & Neck Surgery, J.N.Medical College, KLE Academy of Higher Education and Research, Belagavi, Karnataka, India
*Corresponding author: Rajesh R Havaldar, Senior Resident, Department of ENT & Head and Neck Surgery, J. N. Medical College, KLE Academy of Higher Education & Research, Belagavi, Karnataka, India, Tel: +91-7090095006
Received: November 15, 2019 Accepted: November 22, 2019 Published: November 29, 2019
Citation: Patil PH, Ankle NR, Havaldar RR, Padmavathy O, Kumar AD. Dual Pathology in a Single Nasal Cavity-A Clinical Case Report. Madridge J Case Rep Stud. 2019; 4(1): 163-166. doi: 10.18689/mjcrs-1000143
Copyright: © 2019 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Nasal obstruction is one of the most common rhinological problems. It can be either unilateral or bilateral. Nasal polyposis and inverted papilloma are two differential diagnosis of unilateral nasal obstruction. Both of these are different in terms of clinical features and appearance. A condition of co-existence of both these pathologies in a single nasal cavity is a rare finding. Moreover, radiological assessment often fails to determine the presence of both these pathologies due to the similar appearance on Computed Tomography. Hence a high index of suspicion and complete clearance of the disease with a histopathological confirmation is of paramount importance to avoid disease related morbidity and mortality.
Keywords: Inverted papilloma; Nasal polyp; Nasal obstruction.
Introduction
Inverted papilloma is a benign epithelial growth of nasal cavity and paranasal sinuses usually arising from the lateral nasal wall and the middle meatus and may extend to the ethmoid and maxillary sinuses with an incidence rate of 0.6 cases/100,000 people/year. It comprises 0.5–4% of all primary nasal tumours commonly seen in males during the fifth to seventh decade of life [1]. In advanced cases, it may extend into the ipsilateral peripheral nervous system whereas intracranial growth and dural penetrations are rare [2].
On the other hand nasal polyposis is inflammation of the mucosa of nose and paranasal sinuses associated with multifactorial origin and are frequently associated with asthma, cystic fibrosis and other conditions. It presents macroscopically with a smooth surface which is pliable and light-colored - gray or pink, with body and pedicle covered by non-keratinized pseudo stratified epithelium. It is usually located in the middle meatus and superior meatus [3].
Case Report
A 60 year old male patient presented to our Otolaryngology clinic with complaints of unilateral nasal obstruction since one and half years associated with epistaxis and decreased perception of smell.
On anterior rhinoscopic examiination, a single, pink, irregular, firm mass was noted in the right nasal cavity. On probing, it was attached to the lateral wall of the right nasal cavity and it did not bleed on touch. Posterior rhinoscopy was clear. Left nasal cavity was free. There were no lymph nodes palpable on neck examination. Patient was subjected to routine blood investigations and radiological imaging.
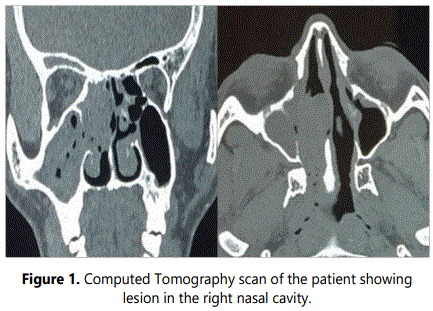
CT paranasal sinus revealed a hyperdense lesion in the right nasal cavity suggestive of right maxillary and ethmoidal sinusitis with enlargement of the osteo-meatal region with no signs of bone lysis (Figure 1). Patient was subjected to biopsy and histopathological examination revealed benign exophytic papilloma. Further clearance of the disease was planned.
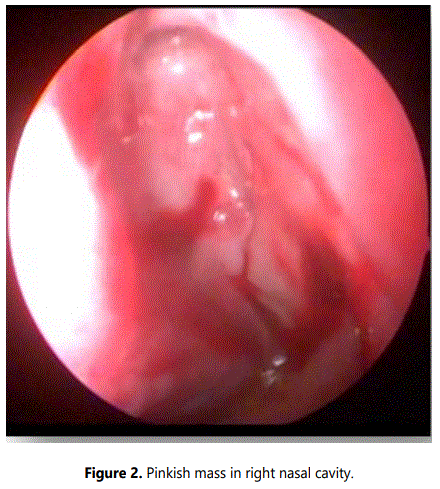
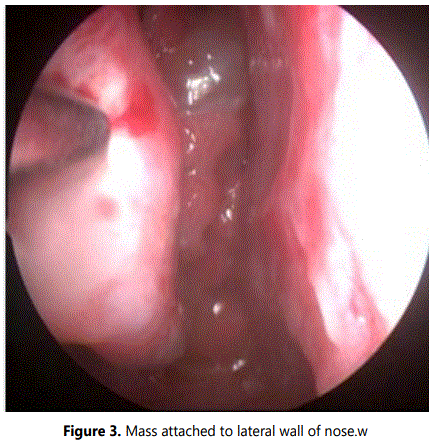
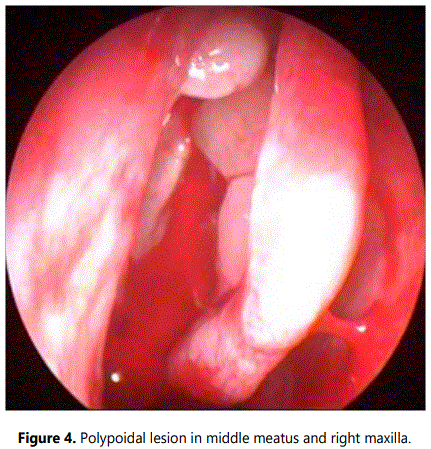
A microdebrider assisted functional endoscopic sinus surgery with clearance of mass was done. Intraoperatively, a pinkish firm mass was seen occupying the right nasal cavity, the surface was smooth and on probing gently, it was attached only to the lateral wall of the nasal cavity (Figures 2 and 3). After clearing the mass, to our surprise there were multiple pale polyps which were present in the middle meatus with polypoidal changes involving the middle turbinate and in the maxillary sinus (Figure 4). Polyps were debrided and a middle meatal antrostomy was done.
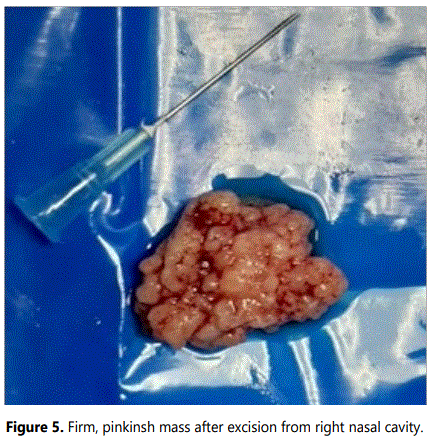
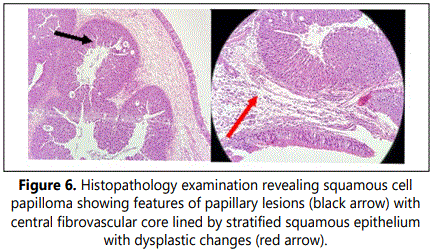
The specimens of mass in the nasal cavity (Figure 5) and the polypoidal tissue from the middle meatus and maxilla were sent for histopathological examination separately. Whilst the mass in the nasal cavity was reported as squamous cell papilloma showing features of papillary lesions with central fibrovascular core lined by stratified squamous epithelium with dysplastic changes (Figure 6), the tissue from the maxillary sinus was reported as inflammatory polyps showing loose connective tissue and inflammatory cells covered by pseudo stratified ciliated columnar epithelium respectively.
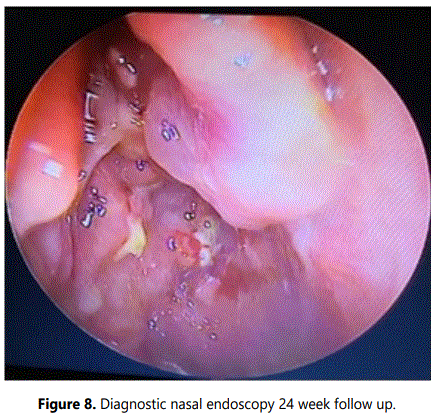
On follow-up, endoscopic cleaning of the nasal cavities were done, which showed no evidence of residual or remnant tumour (Figures 7 and 8) at 12 and 24 weeks respectively and the patient felt symptomatically better with improvement in smell perception.

Discussion
Inverted papilloma has multiple synonyms. Khandekar S et al. in their report mentions Ringertz tumour, transitional cell papilloma, fungiform papilloma, cylindrical cell papilloma, schneiderian cell papilloma, epithelial papilloma, papillary sinusitis, soft papilloma and sino nasal-type papillomas as different names of the same pathology being used interchangeably. It is a benign neoplasm arising from the sinonasal (Schneiderian) mucosa which is composed of squamous or columnar epithelial proliferation with associated mucous cells [1].
Lawson W et al. studied the etiology of inverted papilloma and the role of human papillomavirus as a causative factor. Some of the causes included chronic sinusitis, viral infections, allergies, and human papillomavirus. Although, significant association has been identified between the presence of human papillomavirus DNA in inverted papilloma and recurrence of the disease after surgical resection, the results are inconclusive. HPV 16 and 18 are associated with malignant transformation of inverted papilloma [2].
Antrochoanal polyp, nasal cavity squamous polyp, allergic fungal sinusitis, juvenile angiofibroma, nasal glioma, SCC, lymphoma, adenocarcinoma and esthesioneuroblastoma all are the differential diagnosis of a suspected case of inverted papilloma [1].
Nasal polyps (NP) are benign lesions arising from the mucosa of the nose and paranasal sinuses. Many factors contribute to the formation of nasal polyps and the commonly observed finding is a scenario of dysregulated interaction between the sinus epithelium and the lymphoid system [3].
Morphologically, nasal polyps arise from the lateral wall of the nose around the osteo-meatal complex. These are edematous, with grape like pojections. The surface is smooth and consists of pale tissue which helps in differentiating it from the more vascular mucosa of the nasal cavity. Histologically, they consist of loose connective tissue, inflammatory cells and fluid, and are usually covered by pseudostratified, columnar, ciliated epithelium. Polyps form when oedematous connective tissue stroma ruptures and herniates through the basement membrane [3].
Epithelial alterations are a commonly encountered feature of Inverted papilloma unlike inflammatory polyps. The most important diagnostic clue for an inverted papilloma is unilateral tumour localization involving the lateral nasal wall and the middle meatus [4].
Computed Tomography (CT) and Magnetic Resonance Imaging (MRI) play an important role in diagnosis of inverted papilloma. CT offers superior bony definitions and MRI gives superior soft tissue delineation. Typical CT finding of inverted papilloma is unilateral opacification of the paranasal sinuses. The site of origin of the lesion as well as site of recurrence can be gauged by the presence of bony changes on computed tomography [1]. Chronic sinusitis on computed tomography shows diffuse bone thickening unlike focal hyperostosis. Differentiation of the two requires CT scan [5,6]. But when there is a coexisting polyps with inverted papilloma it is difficult for imaging modality to differentiate as encountered in this case report.
The primary and preferred treatment of inverted papilloma is surgery. The key element for successful treatment is proper intra-operative determination of extent and attachment of the tumour, subperiosteal dissection of involved areas, wide removal of the tumour origin along the subperiosteal plane, complete removal of all the diseased mucosa with creation of wide cavities. Regular long term follow up is very important [7,8].
There is also association of malignancy with inverted papilloma. In our case there was mild to moderate dysplastic changes which was observed. Therefore proper follow up with the patient to look for recurrence and complete excision of the tumour as achieved in this case are the mainstay of treatment.
Conclusion
Unilateral nasal obstruction is a common rhinological problem. Differential diagnosis includes nasal polyposis, inverted papilloma, benign and malignant conditions. Existence of inverted papilloma with nasal polyposis is rare. Imaging modalities play an important role in diagnosing a inverted papilloma. But when there is an associated polyp, imaging does not differentiate between the two conclusively. A proper intraoperative look out for coexistence of any other disease is important which determines the management of the disease and helps in optimal disease clearance.
References
- Khandekar S, Dive A, Mishra R, Upadhyaya N. Sinonasal inverted papilloma: A case report and mini review of histopathological features. J Oral Maxillofac Pathol. 2015; 19(3): 405. doi: 10.4103/0973-029X.174644
- Lawson W, Schlecht NF, Brandwein-Gensler M. The role of the human papilloma virus in the pathogenesis of Schneiderian inverted papillomas: an analytic overview of the evidence. Head Neck Pathol. 2008; 2(2): 49-59. doi: 10.1007/s12105-008-0048-3
- Chaaban MR, Walsh EM, Woodworth BA. Epidemiology and differential diagnosis of nasal polyps. Am J Rhinol Allergy. 2013; 27(6): 473-478. doi: 10.2500/ajra.2013.27.3981
- Andrade GC, Fujise LH, Fernandes AM, Azoubel R. Rhinosinusal Polyposis and Inverted Papilloma: A Morphometric Comparative Study. Int Arch Otorhinolaryngol. 2015; 19(3): 196-199. doi: 10.1055/s-0035-1547521
- Sharma S, Sonkhya D, Sonkhya N. Skull Base Inverted Papilloma: A Case Report. Ann Clin Case Rep. 2016; 1: 1219.
- Visvanathan V, Wallace H, Chumas P, Makura ZG. An unusual presentation of inverted papilloma: case report and literature review. J Laryngol Otol. 2010; 124(1): 101-104. doi: 10.1017/S0022215109990703
- Lee DK, Chung SK, Dhong HJ, Kim HY, Kim HJ, Bok KH. Focal hyperostosis on CT of sinonasal inverted papilloma as a predictor of tumor origin. AJNR Am J Neuroradiol. 2007; 28(4): 618-621.
- Loevner LA, Sonners AI. Imaging of neoplasms of the paranasal sinuses. Neuroimaging Clin N Am. 2004; 14(4): 625-646. doi: 10.1016/j.nic.2004.07.005




