Case Report
A Vietnamese Case of Hematohidrosis
1National Hospital of Dermatology and Venereology, Hanoi, Vietnam
2Department of Dermatology, Hanoi Medical University, Hanoi, Vietnam
*Corresponding author: Ngo Minh Thao, Dermatologist, National Hospital of Dermatology and Venereology, Hanoi, Vietnam, E-mail: ngothao2609.hmu@gmail.com
Received: May 24, 2019 Accepted: June 1, 2019 Published: June 7, 2019
Citation: Thao NM, Thach Lam TH, Doanh LH, Linh TT, Khang TH. A Vietnamese Case of Hematohidrosis. Madridge J Case Rep Stud. 2019; 3(2): 148-150. doi: 10.18689/mjcrs-1000139
Copyright: © 2019 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Hematohidrosis is a rare clinical entity of sweating blood. It may occur in an individual who is suffering from extreme levels of stress, strain or any sort of exertion with underlying bleeding disorders. A limited reports of hematohidrosis was published. We describe a case where bloody sweat was discharged from a whole body episodically in a 26-year-old healthy male with no bleeding disorders or any other underlying cause. The patient was reported with no abnormal investigations and has marked improvement in severity with propranolol, diazepam and vitamin C therapy.
Keywords: Hematohidrosis; Hematidrosis; Hemidrosis; Sweating Blood; Propranolol; Diazepam; Improvement; Therapy.
Introduction
Hematohidrosis is a very rare clinical condition characterized by recurrent episodes of self-limited bleeding from intact skin. It also known as hematidrosis and hemidrosis. Exact etiology is not known. Some factors including hysterical mechanisms and psychosomatic disorders are believed to induce bleeding, particularly acute physical or emotional stress. Other causes are considered, such as: a component of systemic disease, vicarious menstruation and unknown factors. Very few cases of hematohidrosis have been reported in literature. Up to date, there is no report of hematohidrosis in Vietnam in literature. Here, we report a case of hematohidrosis in a Vietnamese man based on clinical and laboratory tests that was good response with propranolol, diazepam and vitamin C (acid ascorbic).
Case Report
A 26-years-old male Vietnamese patient presented to our hospital with spontaneous bleeding from skin for one month. After marriage three weeks, he found that sweating blood from his neckʼ and shoulderʼs shirt. Two days later, similar characteristics were appeared on his face and sole. The patient had no history of bleeding tendencies, any indication of systemic diseases, nor of using colored food or drinks, no ingestions of anticoagulants and other drugs. He also reported that not using of any topical application of medication or exposure to dyes. There was no evidence of any trauma, purpura, scratch marks, fever or any sign suggestive of bleeding. His family history had a normal conditions related to systemic disease. He has suffered from continuous mental stress for years due to his work and the pressure of marriage recently.
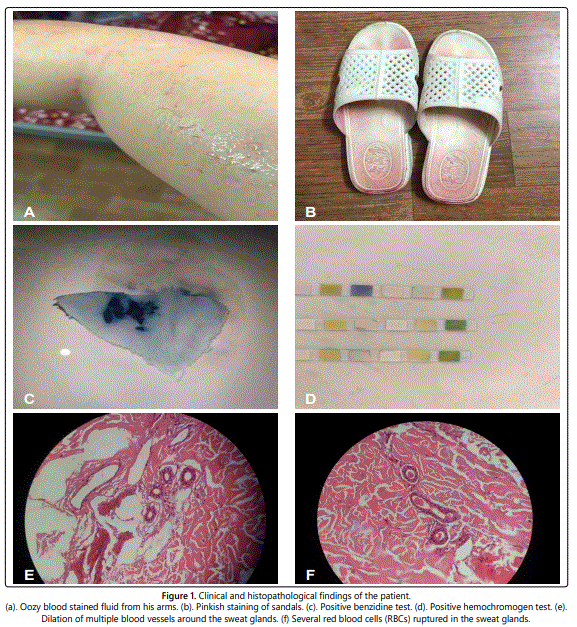
Clinical examination revealed oozy blood stained fluid from the whole body, particularly on the neck, shoulder, arms (Figure 1a). On mopping, it disappeared immediately leaving behind no signs of trauma or any abnormal skin conditions. The pinkish staining of clothing and sandals which were contacted with neck and soles were also presented (Figure 1b). No sign of bleeding, injury or any systemic disease was found. Blood pressure and body temperature were within normal limits.
Laboratory tests were investigated. Complete blood count, platelet function tests, liver function tests, renal function tests, urine routine and bleeding tendencies test were all normal. Hematohidrosis was suspected based on clinical aspects and confirmed by benzidine test, in which hemoglobin in blood reacts with hydrogen peroxide liberating oxygen, which then reacts with organic reagent producing a green to blue colored compound. In this our case, the result of benzidine test was positive (Figure 1c). Hemochromogen test for confirming the blood pigment to be human blood pigment was performed then and the result is also positive (Figure 1d). Skin biopsy was conducted then. The histopathological manifestations showed that dilation of multiple blood vessels around the sweat glands in which there are several red blood cells (RBCs) ruptured (Figures 1e and 1f).
Based on clinical and laboratory findings, the patient was diagnosed with hematohidrosis. He was advised rest, change of lifestyle and managed with diazepam, propranolol and vitamin C. The symptoms disappeared after 10 days of treatment but relapsed after three months at the end of treatment. During next five months of follow-up periods, the patient had only one recurrent course of disease. It could be controlled with the same regimen in short term. Up to date, he was stable without any recurrence.
Discussion
A few theories have been proposed regarding the etiopathogenesis of hematohidrosis. According to Frederick Zugibe, under the pressure of stress, multiple bloods vessels which present in a net-like form around the sweat glands constrict and as the anxiety passes out, vessels dilate to point of rupture that induces RBCs released from blood vessels, go into the sweat glands and push to the surface [1]. In our case, the extreme levels of pressure of work and marriage play important role as a factor activated sympathetic system to induce vasoconstriction. This causes hemorrhage of the vessels supplying the sweat glands into the ducts of the sweat glands. The blood then pushed along with sweat to the outside, presenting as bloody sweat. Another perspective of Zhang concluded that a specific vaculitis might be the pathological basis for hematohidrosis due to the presence of some intradermal bleeding and obstructed capillaries without abnormality in sweat glands, hair follicles and sebaceous glands [2], but in our case, direct immunofluorescence technique did not reveal any abnormality. In other side, Manonukul suggested that there are maybe some dermal defects or some distinctive substances damaged the vessels supplying sweat glands [3]. Other researchers believed that this phenomenon could be related to some chronic underlying disease, namely Hemochromatosis [4,5]. Lack of evidence basis led to the difficulty in determination the cause of this disease.
Currently, there are no convincing specific modalities that could well managed hematohidrosis. All the treatment mainly focus on controlling symptoms of the disease. Several studies reported successful treatment with propranolol [6-8], antianxiety medication and relaxation techniques [9]. Recently, Biswas et al. have reported successful treated with topical atropine application [10].
Conclusion
We report this case for its rarity and also for its clinical response to propranolol, diazepam and vitamin C. In our case, the precipitating factor namely stress was identified. No evidence of vasculitis or any dermal defects or abnormality in sweat glands was detected.
Declaration of Patient Consent
The authors certify that they have obtained all appropriate patient consent forms including his/her images and other clinical information. The patients understand that their names would not be published.
Conflicts of Interest
There are no conflicts of interest.
References
- Zhang FK, Zheng YL, Liu JH, et al. Clinical and laboratory study of a case of hematidrosis. Zhonghua Xue Ye Xue Za Zhi. 2004; 25(3): 147-150.
- Manonukul J, Wisuthsarewong W, Chantorn R, Vongirad A, Omeapinyan P. Hematidrosis: A pathologic process or stigmata. A case report with comprehensive histopathologic and immunoperoxidase studies. Am J Dermatopathol. 2008; 30(2): 135-139. doi: 10.1097/DAD.0b013e318164cf4b
- Carvalho AC, Machado-Pinto J, Nogueira NC, Almeida LM, Nunes MB. Hematidrosis: a case report and review the literature. Int J Dermatol. 2008; 47(10): 1058-1059. doi: 10.1111/j.1365-4632.2008.03746.x
- Jerajani HR, Jaju B, Phiske MM, Lade N. Hematohidrosis – A rare clinical phenomenon. Indian J Dermatol. 2009; 54(3): 290-292. doi: 10.4103/0019-5154.55645
- Arakkal GK, Poojari S, Netha GN, Kumar BU. Hematohidrosis: A rare case of a female child who sweat blood. Indian Journal of Pediatric Dermatology. 2017; 18(4): 327-329. doi: 10.4103/2319-7250.193031
- Wang Z, Yu Z, Su J, et al. A case of hematidrosis successfully treated with propranolol. Am J Clin Dermatol. 2010; 11(6): 440-443. doi: 10.2165/11531690-000000000-00000
- Bhattacharya S, Das MK, Sarkar S, De A. Hematidrosis. Indian Pediatr. 2013; 50: 703-704.
- Raksha MP, Stuti M. Hematohidrosis: a rare clinical entity. Indian Dermatol Online J. 2010; 1(1): 30-32. doi: 10.4103/2229-5178.73256
- Biswas S, Surana T, De A, Nag F. A curious case of sweating blood. Indian J Dermatol. 2013; 58(6): 478-480. doi: 10.4103/0019-5154.119964




