Clinical Image
Leonine Facies: The Face of a Forgotten Disease
Department of Dermatology, Hassan II University Hospital, Fès, Morocco
*Corresponding author: Safae Zinoune, Doctor,, Department of Dermatology, Hassan II University Hospital, Fès, Morocco, E-mail: zinounesafae@gmail.com
Received: March 6, 2019 Accepted March 12, 2019 Published: March 18, 2019
Citation: Zinoune S, Chaouche M, Douhi Z, et al. Leonine Facies: The Face of a Forgotten Disease. Madridge J Case Rep Stud. 2019; 3(1): 118-120. doi: 10.18689/mjcrs-1000129
Copyright: © 2019 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Image Description
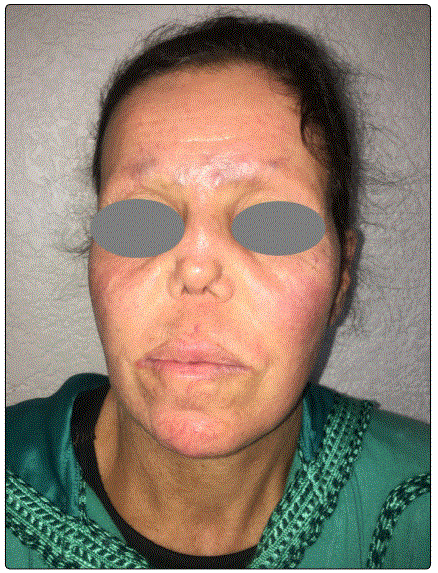
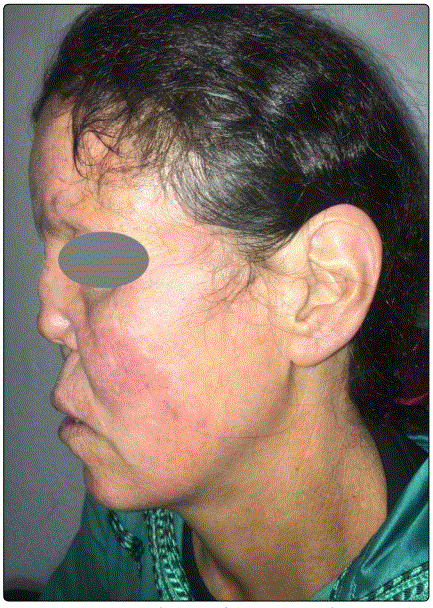
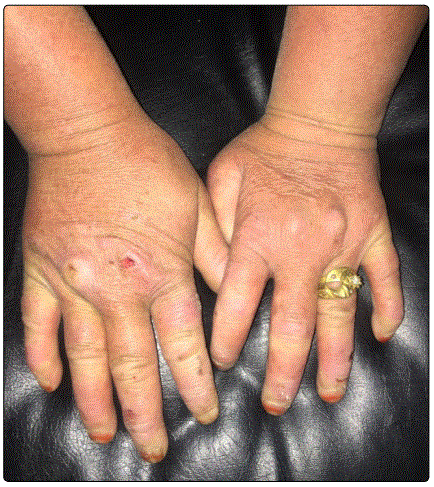
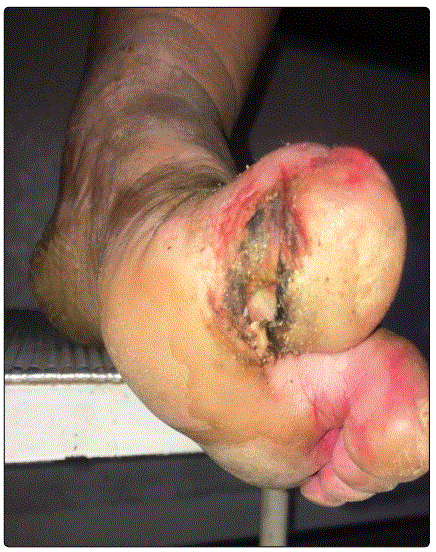
A 45-year-old woman presented with a five-year history of paresthesia of both hands and feet, along with modification of facial features. On physical examination, she had coarse ‘leonine like’ facies, with thickened skin of face and eyelids, her face had multiple nodular lesions that coalesced into plaques, especially on the forehead. She had madarosis and a saddle-nose (Figures 1 and 2). We also observed strabismus, ulcers on hands and feet with a swan neck deformity of fingers (Figures 3 and 4).
After the strongly suggestive hypothesis of lepromatous leprosy, we performed a skin biopsy which confirmed the disease. The patient underwent standard anti-bacillary multidrug therapy for 12 months, with good improvement.
Discussion
Leprosy is caused by Mycobacterium leprae and has been known since biblical times. It is still endemic in many regions of the world [1]. The mechanism of transmission of leprosy consists of prolonged close contact between susceptible and genetically predisposed individuals and untreated multibacillary patients [2]. Transmission occurs through inhalation of bacilli present in upper airway secretion. The nasal mucosa is the main entry or exit route of Mycobacterium leprae [1].
The disease course is determined by individual host immunity. Lepromatous leprosy occurs in infected individuals with impaired T-cell immunity resulting in energy. Clinically, this multibacillary form is characterized by multiple red-brown nodular infiltrates (lepromas) in the skin and mucous membranes. Predilection site for these diffuse infiltrates is the face and auricles. The symmetrical centrofacial distribution of lesions and the loss of the eyelashes and eyebrows (madarosis) are referred to as “leonine facies”. Involvement of the nasal mucosa leads to destruction of the septum and deformity of the nasal skeleton (saddle nose). Subsequently, this destructive inflammatory process may include the entire nasopharynx, clinically characterized by mucosal ulcerations of the palate and larynx [3].
One complication that is particularly feared with regard to the multibacillary forms of leprosy is ocular involvement, which leads to complete blindness. Lymphatic and hematogenous spread can lead to involvement of the kidneys, the liver, the bone, and to acute orchitis.
The gold standard for the diagnosis of lepromatous leprosy is histological examination of skin biopsy in correlation with the bacteriological indices [3]. Delay in diagnosis may have been due to the rarity of this condition. The treatment of leprosy involves multi-drug therapy. The three drugs of first choice are: dapsone, rifampicin, and clofazimine [4].
References
- Lastória JC, Abreu MA. Leprosy: review of the epidemiological, clinical, and etiopathogenic aspects - part 1. An Bras Dermatol. 2014; 89(2): 205-218.
- Gaschignard J, Grant AV, Van Thuc N, et al. Pauci- and Multibacillary Leprosy: Two Distinct, Genetically Neglected Diseases. PLoS Negl Trop Dis. 2016; 10(5): e0004345. doi: 10.1371/journal.pntd.0004345
- Fischer M. Leprosy - an overview of clinical features, diagnosis, and treatment. J Dtsch Dermatol Ges. 2017; 15(8): 801-827. doi: 10.1111/ddg.13301




