Case Report
Oncocytic Schneiderian Papilloma of the Maxilla; The Report of a Case with Evident Malignant Foci
1Professor, Department of Oral Pathology, Faculty of Dentistry, Alexandria University, Alexandria, Egypt
2Lecturer, Department of Oral Medicine, Diagnosis and Radiology, Faculty of Dentistry, Pharos University, Alexandria, Egypt
3Assistant lecturer, Department of Oral Pathology, Faculty of Dentistry, Alexandria University, Alexandria, Egypt
4Demonstrator, Department of Oral Medicine and Diagnosis Department, Faculty of Dentistry, Alexandria University, Alexandria, Egypt
*Corresponding author: Manal Ibrahim Elnouaem, Professor, Department of Oral Pathology, Faculty of Dentistry, Alexandria University, Alexandria, Egypt, Tel: (03) 4868066, E-mail: elnouaemmanal@gmail.com
Received: March 17, 2017 Accepted: April 12, 2017 Published: April 17, 2017
Citation: Sharaf RA, Youssef HA, Ali Basha SM, Elnouaem MI. Oncocytic Schneiderian Papilloma of the Maxilla; The Report of a Case with Evident Malignant Foci. Madridge J Case Rep Stud. 2017; 1(1): 7-10. doi: 10.18689/mjcrs-1000102
Copyright: © 2017 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Schneiderian papillomas (SPs) are benign tumors found in the Sino-nasal tract. They present tendency to recur and have been reported to be associated with malignancy in approximately 4-17% of the cases. We hereby report a case of SP showing dysplastic changes rendering it premalignant.
In the present case resection of the tumor was done after an endoscopic in scional biopsy was taken earlier and was diagnosed as Schneiderian papilloma with malignant foci.
The present report might improve the understanding of the sino-nasal papillomas and consider putting them in the differential diagnosis of maxillary sinus tumors of aggressive behavior which may extend intra-orally and reach the roots of the teeth.
Keywords: Schneiderian papilloma; Maxillary sinus tumors; Malignant changes.
Introduction
The ectodermally derived ciliated respiratory mucosa that lines the Sino-nasal tract so called Schneiderman membrane, gives rise to three morphologically distinct papillomas; these are the fungiform, inverted, and oncocytic papillomas as known individually or collectively designated as Schneiderian paillomas (SPs) [1].
Schneiderman papillomas are uncommon endophytic, locally aggressive tumors, though benign;still they characteristically invade local tissues and have tendency to recur. They may also show malignant transformation [2-5].
SP are characterized by downward growth of the neoplastic epithelium into the underlying stroma with an intact basement membrane rather than epithelial proliferation[2].
The etiology of SP is debatable as various factors such as allergy, chronic inflammation, occupational pollutants and infection with HPV have been suggested [3,6]. Human Papilloma virus (HPV) type 6 and 11 and to a lesser extent types 16, 18 and 57 would be implicated in the etiology. Despite this, there is a debate around the viral etiology as viral inclusions have never been demonstrated by light or electron microscopy and showed negative results with immuno-peroxidase techniques. The HPV genome varied in the different types of schneiderian papillamas where in inverted papillomas the results using insitu hybridization and / or polymerase chain reaction varied from 0-100% [1].
Radiographically the findings varied according to the extent of the disease. In the early stages they appeared as soft tissue densities within the nasal cavity and / or paranasal sinuses. In the late stages or severe cases there is unilateral pacification and thickening of one or more of the sinuses; there are also expansion and displacement of adjacent structures as seen by conventional radiography or by computed tomography [7,8]. Bone sometimes shows erosions and it should be differentiated from bone lesions associated with malignancy. With extensive bone destruction the possibility of carcinoma on top of schneiderian papillomas should be expected [1,7,8].
Case Study
A 40 year old male was complaining of proptosis of left eye Figure (1&2) when he arrived to the Maxillofacial Department for examination, he suffered from this since a year with excessive lacrimation and discharge from the left nostril. The patient reported, he was a heavy smoker with history of 20 year of cigarette and hookah smoking.
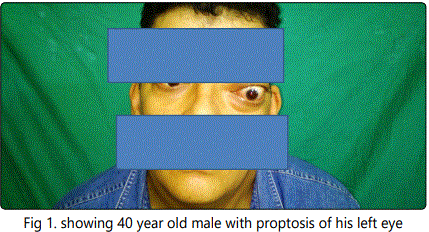
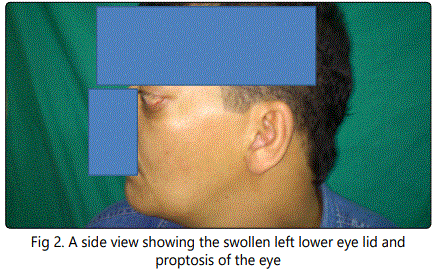
His computed tomography (CT) showed a unilateral opacification originating from the left nostril, ethmoidal sinus reaching the left orbit and showing an intra cranial extension. Figure (3,4)
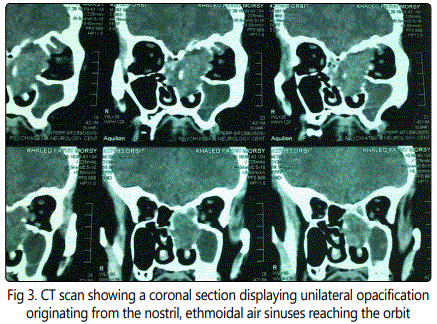
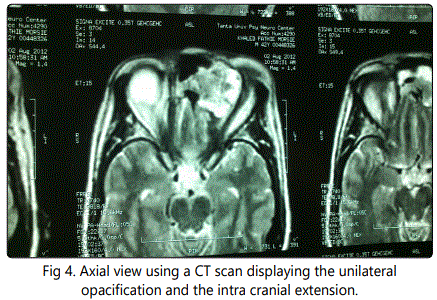
An endoscopic inscisional biopsy was taken from nose giving the diagnosis of SP.
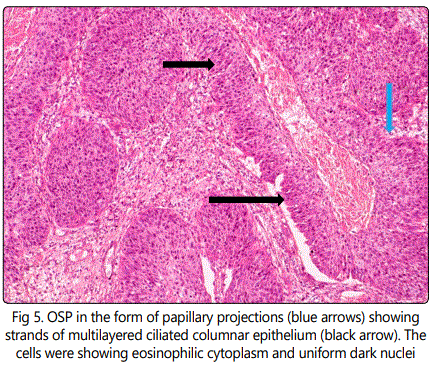
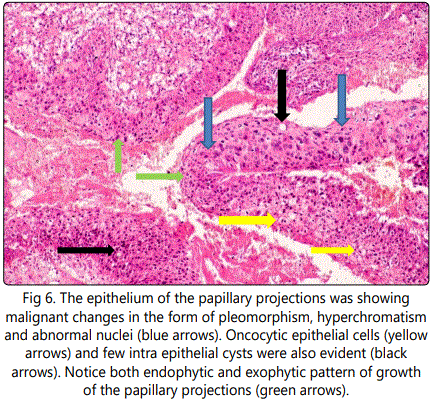
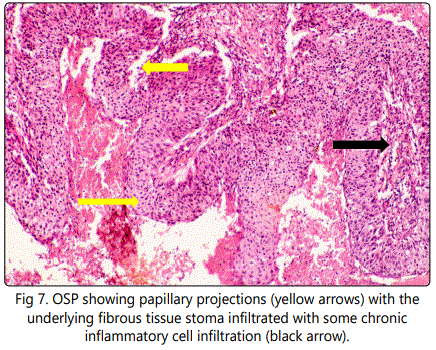
Resection of the tumor was done later and specimen was processed and slides were stained with hematoxylin and eosin and diagnosis was confirmed as oncocytic schneiderian papilloma (OSP) with malignant foci. Histopathological examination revealed bands and strands of multilayered columnar epithelial cells with eosinophilic finely granular cytoplasm and uniform dark nuclei which are occasionally slightly vesicular; The papilloma exhibited exophytic and endophytic patterns of growth Figure (5), The epithelium showed some malignant changes as pleomorphism cells as well as hyperchromatism; some areas showed abnormal nuclei. Oncocytic epithelial cells together with few intra epithelial cysts were evident Figure (6). The ciliated epithelium showed papillary projections within the underlying connective tissue which showed areas of hemorrhage and chronic inflammatory infiltrate Figure(7). Final diagnosis was consistent with (OSP) with malignant foci. Skin of forehead and the eyes was free of tumor cells.
Discussion
The SPs are benign tumors that have the tendency to recur and the propensity to be associated with malignancy. Their tendency to maligant transformation change has been described in approximately 4-17% of the cases [1,3,9].
OSP is the rarest of the three morphologic variants of schneiderian papillomas. It shows many features in common with inverted papillomas; as a matter of fact some regards it as a variant of inverted papilloma [9].
Inverted papillomas (IP)mostly occur in Caucasian males with mean age of 50 showing symptoms of nasal obstruction, nasal discharge, epistaxis, epiphora and proptosis [3,9] while OSP occurs almost equally in both sexes with most of patients being above 50 years at the time of diagnosis.
In the present study the patient was a 40 year Caucasian male whose main complaint was proptosis of his left eye with excessive lacrimation and discharge from left nostril and his age was 10 years younger than the commonly encountered age. A possible hypothesis for high rate occurrence in Caucasians may be evolutionary [3].
The exact etiology is not clear, but there is high evidence of smoking, occupational exposure and human papilloma virus have been implicated [2]. Being a heavy smoker may have played a role in the occurrence of the current case. Unlike the IP the OSP very rarely or even completely lacks the presence of HPV as an etiological cause where it showed negative results with insitu hybridization and/or polymerase chain reaction although it could be due to defects in sampling still it does suggest that OSP is not virus related [10]; and hence smoking here is pointed to as an etiological factor.
The patient in this study showed nasal airway obstruction with enlargement of his face on the left side, this was shown on the CT tomography as a soft tissue tumor causing unilateral pacification originating from left nasal cavity, ethmoidal air cell reaching the left maxillary and frontal sinuses and showing retained secretion. Anterior skull was intact with no intracranial extension identified.
The radiographic findings are common in SPs but do not indicate malignant transformation .This is in accordance with the findings of Egger's et a [6-8], on their work on inverted papilloma of the paranasal sinuses.
Histopathological findings after endoscopic incisional biopsy from nose revealed oncocytic schneiderian papilloma of the nasal cavity and paranasal sinuses. OSP was documented to show carcinomatous changes in 4-17% of cases [1,9]. In the current study malignant changes in the form of scattered malignant foci with abnormal pleomorphic hyperchromatic nuclei. As with IP, OSP showed a range of histologic changes ranging from dysplasia to carcinoma insitu to invasive carcinoma [1]. Our histological findings were in accordance with other studied cases which showed the same histopathological features [3,9,11].
The presence of SP in association with malignancy could be metachronous where malignant changes occur on top of a previously diagnosed benign inverted papilloma or synchronous where both tumors are diagnosed simultaneously [3]. We believe the former type is the one associated in the present case.
Prognosis of SP always depends on histologic type, degree of invasion and the extent of tumor.
No consent form was used as patients coming to the Maxillofacial Surgery Department were considered as educational cases and his or her information was used for research service. The patient in the present case was informed with this information and our main concern here was the histopathological and radiographic features of the present case.
Conclusion
OSP is the rarest of the three types of SPs. In this case we report a 40 year old male with oncocytic schneiderian papilloma, which histologically showed malignant changes thus rendering it premalignant. Surgical excision was the line of treatment and follow up of patient was recommended. We highly recommend close follow up for patients diagnosed with OSPs even after the surgical treatment to find out if any malignant changes have occurred. Also SPs must be considered in differential diagnosis of maxillary tumors.
Conflicts of interest
Authors declare no conflict of interest.
References