Review Article
Flash from the Back; Molecular and Epidemiological aspects of Breast Cancer in Last 15 Years
Saleem University of Central Punjab, Lahore, Pakistan
*Corresponding author: Sadia Zia, University of Central Punjab, Lahore, Pakistan, E-mail: sadia.zia@ucp.edu.pk
Received: April 19, 2018 Accepted: May 31, 2018 Published: June 07, 2018
Citation: Zia S, Rahman Z, Baig S, Saleem MA. Flash from the Back; Molecular and Epidemiological aspects of Breast Cancer in Last 15 Years. Madridge J Cancer Stud Res. 2018; 2(1): 47-54. doi: 10.18689/mjcsr-1000106
Copyright: © 2018 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Breast cancer is one of the most abundant forms of cancer among the women and men worldwide. The common phenotypic abnormality of breast cancer cells is due to the dysregulation of cell cycle control. The breast cancer genes includes; BRCA-1, BRCA-2 and P53. The relative incident rate of breast cancer in Asian countries is low than the Non-Asian/ western countries. However, the rate is increasing at a more rapid rate in Asian countries. The increasing incidence rate in West indicates many factors including childbirth trends, age, diet plans and nulliparity.
Keywords: breast cancer, Asia, carcinoma, Epidemiology, Molecular biology, BRCA-1, BRCA-2, P53.
Introduction
Cancer occurs as a result of mutations and abnormal changes majorly due to genetics basis and also from environmental effects. Normally, the cells of our bodies replace themselves through an orderly process of cell growth; healthy cells replaced the old cells [1]. The mammalian cell cycle plays a crucial role in "turn on" and "turn off" the genes. The cell cycle is divided in different phases includes; G0, G1, S, G2 and M. The S phase is called as Synthesis phase and M is Mitotic phase, both these phases are preceded by Gap phases (G1 and G2). The cell cycle is also checked by the mechanism of checkpoints at each transition during cell cycle. These checkpoints provide the information to the intracellular compartments to sense the favorable and unfavorable condition [2].
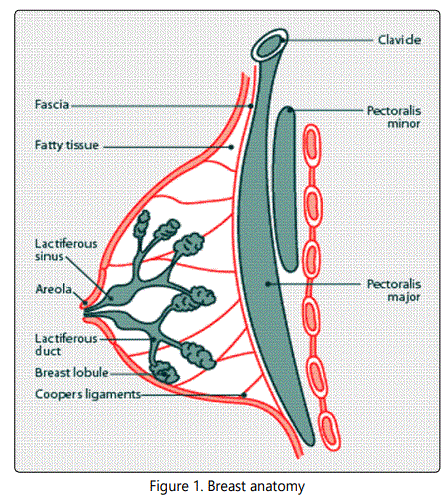
In breast carcinoma, the lobules of cells are the emerging points, which are milk producing glands or ducts. Less commonly breast cancer can begin in the stromal tissues, which include the fatty and fibrous connective tissues of the breast (Fig.1). The cancerous cells with the passage of time can invade nearby healthy breast tissues and make their way in to underarm lymph nodes. The early breast cancer usually does not cause pain and may exhibit asymptomatic [3]. After the progress of cancer, symptoms can include; lump near the breast, change in shape and size of breast, tenderness or retraction (turning inward), and skin irritation. If the cancerous tumors invade surrounding tissues and spread to other parts of the body, they are more often appears in bones, liver, lungs, and brain [4].
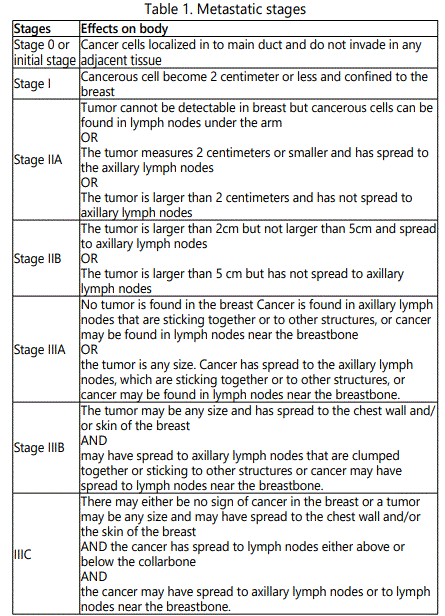
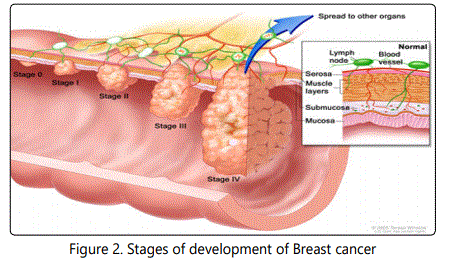
Breast cancer is always caused by a genetic abnormality; however, only 5-10% of cancers are due to an abnormality inherited from parents. The breast carcinoma is developed step by step in the body (Fig 2.). There are certain stages of breast cancer as follows table. 1. [5].

Genetic Analysis of Breast Carcinoma
Breast cancer can be categorized according to its genetic alterations in to two classes; the oncogenes and tumor suppressor genes. The mutation in oncogenes results in a gain of function mutation of a proto-oncogene that generates an uncontrolled and undifferentiated tumor production. But the mutation in tumor suppressor genes causes a loss of function ability to restrain the cell growth. The most important oncogenes and tumor suppressor genes are which take part in breast carcinoma are [6].
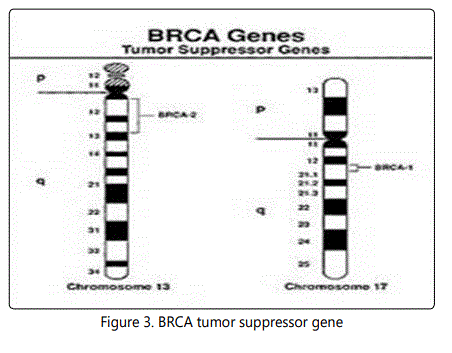
BRCA-1 and BRCA-2
In 1994, the gene Breast cancer 1 (BRCA-1) was isolated from chromosome number 17. It was proposed that an altered BRCA-1 has been linked to the development of breast cancer and ovarian cancer. The altered BRCA-1 gene appears in only 5% of the 182,000 breast cancer cases that develop. [7]. The BRCA-2 gene was isolated from Chromosome number 13. It is also a cancer causing gene when altered. BRCA-2 appears as a triggering breast cancer agent in males. The mutation in BRCA-2 causes one type of Fanconi anemia in people. This condition is caused by the low levels of BRCA-2 protein in cells. This lead to the accumulation of damaged DNA in cell [8].
P53
There are many genes in our body cells that normally prevent tumors formation. P53 is one of them. It's a tumor suppressor gene. The trade of P53 is to prevent or suppressor cells from growing. When it has been damaged or altered, P53 loses its ability to suppress cell growth. Changes to gene result in an increased risk of cancer, almost 50 percent of human cancer cells contain P53 mutations. In breast cancer, p53 mutation is associated with more aggressive disease and worse overall survival. The frequency of mutation in p53 is, however, lower in breast cancer. Changes, both genetic and epigenetic, have been identified in regulators of p53 activity and in some downstream transcriptional targets of p53 in breast cancers that express wild-type p53 [9].
Inheritance of Breast Carcinoma
As the breast cancer results from multiple gene mutations, the initial mutation can be inherited from one`s parents or occur after conception. Inherited gene mutations play a role in about 27%bof all cases of breast cancers. Breast cancer is inherited and family members of families are at greater than average risk of breast cancer. Simply finding several cases of breast cancer doesn't mean a pattern of genetic inheritance. Breast cancer families are frequently described as families with three or more close relatives with breast cancer. Members of these families are at high risk for developing breast cancer at young age that may affect both breasts [10]. Having family history of breast cancer is not alarming in developing a breast cancer. Women with a family history of breast cancer make up only 5-7 percent of all women with breast cancer. The mutated genes associated with a strong family history of breast cancer are known to be a possible factor of breast carcinoma [11].
The mutated genes with strong family history of breast cancer are called as high penetrance genes. A person with high penetrance breast cancer gene has a high risk of breast cancer. Inherited breast cancer risk seen in families with only few cases of breast cancer results from second type of mutated genes called low penetrance genes [12].
Countries or Racial Groups with High Risk of Breast Carcinoma
The incidences of breast cancer vary from country to country and also within races. The 6-10 percent of breast cancers is related to BRCA-1 and BRCA-2 mutations. In Russia, about 80% of cases of breast cancers are related to BRCA1 and 2 mutations. But in the European countries, less the 30% families are affected due to mutations in these genes. In United States and Canada, 40%of familial cases have the BRCA-1 mutations. In Israel, 50 % familial cases are involved BRCA-1 mutations in Ashkenazi Jewish population [13].
The different racial groups have different prevalence of BRCA-1 and 2 mutations. The best studies racial group is Ashkenazi Jews. The population of Ashkenazi Jews in United States is 90%. There is two BRCA-1 and one BRCA-2 mutation is observed among them [14].
Risk Factors of Breast Carcinoma
The exact reasons of breast cancer are still unknown. It is also not possible that a single factor trigger the disease. This is possible that there are combinations of genetic and environmental factors which are responsible for this. The established factors that can predict the incidence of breast cancer includes;
Sex/Gender
The breast cancer is most common cancer in women in developed Western countries and Asian developing countries. So, women are also the biggest risk factor for this disease. About 1 % of breast cancer each year in the United States is reported in males. According to 2005 estimation, almost 1,690 new cases are found among the men annually, it is also estimated that about 460 of these patients were died. In the Western countries, the majority of male breast cancer patients are between the 50s and 60s [15]. In Malaysia, in the year of 2002, 56 and in 2003, 24 new cases were reported [16]. The 22 new cases were reported in Chinese male [17] and 26 in Indian men [18].
Age
Age is a common risk factor of Breast cancer. Increase in age will increase the risk of breast carcinoma. From the age of 30-39 the risk is 1 in 233 or 43%. This value can jump to 1 in 27 or almost 4% till the age of 60 [19].
Prior History of Breast Cancer
The people who are already been affected with breast cancer are at the risk of developing the breast cancer again either in the same breast or in the other one [20].
Previous History and Family History of Breast Cancer
The previous history of breast cancer does matter. If any person had breast cancer of one breast, the risk of developing breast cancer in the opposite breast is more. Another important risk factor is of family history. A woman with a mother or sister which are considered to be first degree relatives are affected with breast cancer at younger age has more chances to develop the breast cancer in herself [21].
The male have the breast cancer risk if the father or brother or son gas had a breast cancer. Female relatives of men with breast cancer often have an increased risk of breast cancer. In some reports 60% of men with breast cancer have female relatives with breast cancer [22].
Menstrual Cycle or Reproductive Cycle
The period of onset of menstruation (menarche) and late menopause are associated with 2-3 times increased risk of breast cancer. This is related to the cumulative numbers of ovulatory cycles. It's also believed that the prolonged exposure to oestrogens may play a role in causation of breast cancer [23].
NulliParity
NulliParity is a condition when females avoid childbirth throughout the life or the late age childbirth. This condition increases the risk of breast cancer. The relation of nulliparity with breast cancer is thought due to number of uninterrupted menstrual cycles [24].
Socio-economic status and Diet
The socio-economic status is strictly associated with breast cancer. This is seen through studies that the women of higher socio-economic status are at greater risk of breast cancer as compared to the women of lower status. The major causes are; menarche age, menopause age, age at first child birth [25].
The composition of diet has been thought to influence the risk of breast cancer. It also account for the differences in incidence rates between countries. However, week and nonexistent associations have been found in case control studies. But this has been reported that evidence of alcohol consumption results in a slight increase in risk of breast cancer [26].
Mechanism and Pathway of Breast Cancer
The body is made up of trillions of living cells. Normal body cells grow, divide and form new cells. The deaths of grown cells are also happened in orderly fashion. Cancer begins when cells in a part of the body start to grow out of control, there are many types of cancers including breast cancer, but all start because of out of control growth of abnormal cells [27]. Cancer cell growth is different from the normal cell growth. The cancer cell instead of dying, continue to grow and form new abnormal cells. DNA in every cell directs all its actions. In a normal cell, when DNA gets damaged, the cell either repairs the damage or dies. In cancerous cell the damaged DNA is not repaired and does not die like it should [28].
Metabolism and Breast Cancer
According to new report of National Cancer Institute, a protein that is associated with the conditions of metabolic imbalance which includes; obesity and diabetes may play their role in development of breast cancer. This metabolic imbalance may take place by the elevated carbohydrate intake, which can over activate a molecule called C-terminal binding protein; this over activation can increase the risk of breast cancer [29]. This has been also reported that CtBP repressed the expression of a gene associated with breast cancer called BRCA1 at an early stage; this led to processing large amount of carbohydrates in the body. This study indicated that obesity and weight gain may contribute to breast cancer by decreasing the level of tumor suppressing gene BRCA1in response to high carbohydrate intake [30].
Influence of Insulin in Breast Cancer
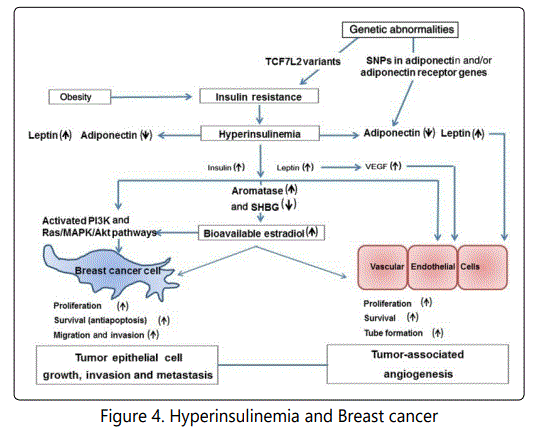
A study reported regarding the relation of hyperinsulinemia and type 2 diabetes to an increased risk of breast cancer as indicated in fig 4. Insulin proliferate the some human breast cancer cell lines in vitro by mechanism that use both the phosphatidylinositol-3 kinase and mitogen-activated protein kinase signaling pathway. Hyperinsulinemia affects the breast cancer cells by endocrine system [31].
Types of Breast Cancer
Breast cancer can begin in different areas of breast; the ducts, lobes and tissues between them.
Ductal carcinoma in Situ (DCIS)
This is a common type of non-invasive type of breast cancer; it starts from the inside the milk ducts. This is called as carcinoma because any cancer that begins from the skin or tissue and cover the internal organs called as carcinoma. The word In Situ refers to its original place. This is also non-invasive because it never spreads from the milk ducts to adjacent tissues [32].
Invasive Ductal Carcinoma (IDC)
This carcinoma refers to the cancer that has broken through the wall of the milk duct and begun to invade in the tissues of the breast. With the passage of time, invasive ductal carcinoma spread to the lymph nodes and possibly to other areas of the body [33].
Tubular carcinoma of breast (TCB)
It is a subtype of IDC. They are usually small may b about 1cm or less and made the tube like structures called as tubules. At once, TC accounted for about 1-4% of all breast cancers. Now that screening mammography is widely used, however, the TC are more diagnosed frequently [34].
Medullary Carcinoma of Breast (MCB)
This is also the subtype of IDC and account for 3-5 % of all cases of breast cancer. The tumor is called medullary because it is soft, fleshy mass and resembles with the part of brain called medulla. This can occur at any age, but usually affects women in late 40s and 50s [35].
Invasive Lobular Carcinoma
ILC also called as infiltrating lobular carcinoma, this carcinoma is the second most common type of breast cancer after IDC, according to American society of cancer; more than 180,000 women in US having ILC each year. This carcinoma spread to the adjacent tissues and begin in milk producing lobules which empty out in the duct that carry the milk to nipple [8].
Inflammatory Breast Cancer
Inflammatory breast cancer usually starts with the reddening and swelling of the breast instead of the breast instead of a distinct lump. IBC grows and spreads quickly. This is a rare formof breast cancer. According to National Cancer Institute, about 1-5% of all breast cancer cases in US are inflammatory breast cancers [36].
Trends of Occurrence of Breast Cancer
Breast carcinoma incidence has been dramatically increased all over the globe. The Asian countries were considered as low risk countries, but now, the rate is sharply increased. Breast cancer is painstaking in US and other western countries. 29% of all malignant tumors arise in US. American cancer society estimated 150,000 new cases for last 5 years. The national cancer institute estimated that approximately every 1 in 9 women will develop breast cancer [37].
Asian Countries
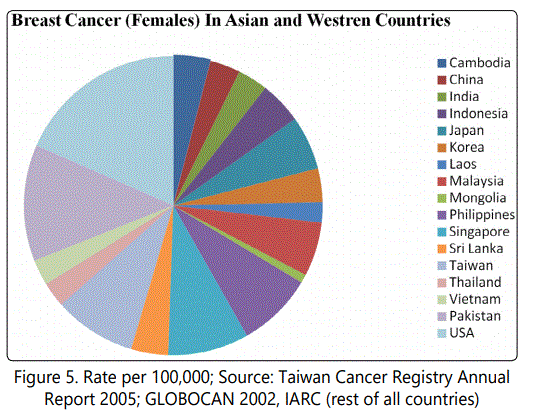
Accordingto a study in 2002, about 4.2 million new cancer cases in 48% of world population living in fifteen most highly developed countries in South, East and Southeast Asia including Japan, Taiwan, Singapore, South Korea, Malaysia, Thailand, China, Philippines, Sri Lanka, Vietnam, Indonesia, Magnolia, India Laos and Cambodia. China and India accounting 37% of the worldwide population [34].
In Asia, Taiwan, Singapore and Philippines has a high incidence rate of breast cancer in females. The incidence rate is same in China and India on about 19 per 100,000. The breast cancer incidence rate in US is much higher than that in any of the Asian countries. According to estimation its 101 per 100,000 in females and the ratio is less in men [38].
Incidence in Cambodia
Cambodia is one of the poorest nations of the world where there has been a sharp increase in the incidence of breast cancer. Although the mortality rate is more about 41%- 25% as compared to incidence rate due to poverty, less facilities of diagnosis and poor awareness [35].
Incidence in China
Breast cancer as a global issue also hits the Chinese women. One out of forty women is diagnosed with breast cancer in china during their life time. The maximum age of the women at the time of diagnosis is under 50 according to estimated data but the mortality rate is rising in Chinese women [17]. In 2008, there were 151,870 total cases were reported with reference to breast cancer, the estimated cases in 2013 are 189,500 and in 2018 the number will be 228,830 [39].
Incidence in India
India faces potential breast cancer epidemic over the next decade as women adopt western lifestyles. Studies indicated that the incidence rate of breast cancer is increasing as India is becoming more westernized [40]. Currently, there are 100,000 new cases annually but in 2015 the rate will be 3% increased and there would be 250,000 cases [18].
Incidence in Pakistan
Pakistan is also facing the highest incidence of breast cancer especially in Karachi. According to Karachi Cancer Registry suggests that the age-standardized annual rate of breast cancer in Pakistan is 69.1 per 100,000. It is reported that Pakistani population boasts the highest rate of breast cancer among all the Asian countries excluding Jews in Israel. The average survival rate of breast cancer patient in Pakistan is 57% where as in USA its 73% [41].
During the period of 2010-2012, A total of 15 840 cancers were diagnosed in 15 825 patients belonging to the district of Lahore and registered against the corresponding years; 9069 (57.3%) were female and 6771 (42.7%) were male patients. Multiple primary cancers, up to two, were identified in 15 patients [42]. According to the recent data in rural areas of Pakistan, socio-economic conditions are responsible for the poor health of the women. At some stage of life, 1 in 9 Pakistani women has become the patient of breast cancer [43].
Western Countries
Breast cancer is most common form of in women in many western countries after lung cancer. Breast carcinoma is considered as most common cause of death in Hispanic women and second most common cause of death in white, black, and Asian/Pacific Islander and American Indian/Alaska Native women. In2004, 186,772 women and 1,815 men were diagnosed with breast cancer in US, and 40,954 women and 362 men died from breast cancer [44].
In UK, breast cancer also affecting the women. It is estimated that it kills more than one thousand women each month. The steady rise is seen in women to contract with this disease. From 1996-2001 it was estimated that chances were raised from 1 in 12 to 1 in 9. According to cancer research UK and office of national statistics 2007, breast cancer can affect almost a quarter of million women in UK [43].
The breast cancer incidence and mortality rate is very much related to age n most of the American and European countries. The risk of getting breast cancer is increased with age. If women are 60 years old, than 3.5% of women of 60 years can get breast cancer in next 10 years. This accounts for 3 out of 4 of every 100 women. Likewise, the risk of death is also increased with age. In US, 0.7% of women of 60 years can have death chances in next 10 years and it is 1 women out of 100 [44]. In 2017, an estimated 3.5 billion women in US were with the history of breast cancer [47].
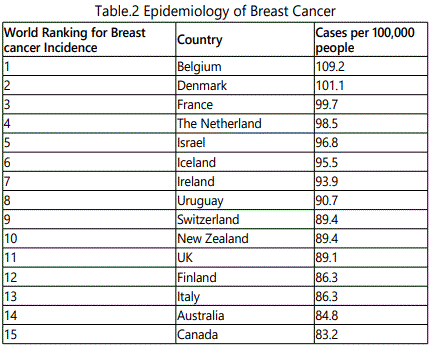
According to world health organization project 2010, UK was among the top 11 countries which have more incidence and mortality rates. The shocking statistics was seen in Belgium which is top country among the 50 countries.
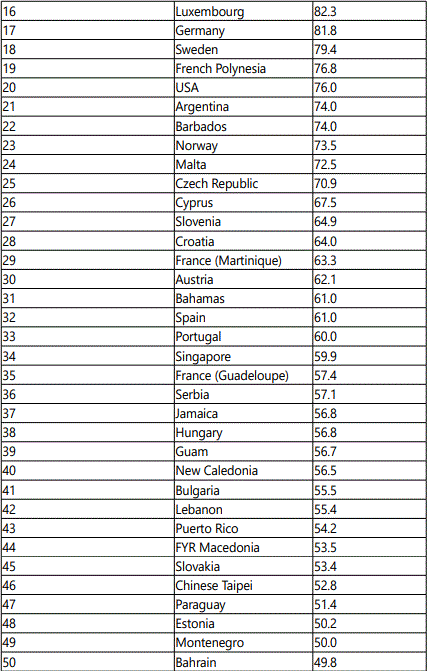
High Incidence Facts in Western Countries than Asia
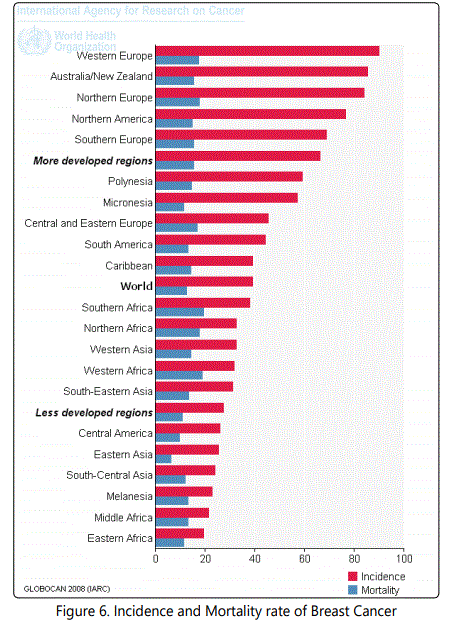
As the details showed that developed countries have more incidence rate than the developing Asian countries but the mortality rate is still increasing in Asian countries. The reason is probably less facilities for diagnosis and treatments are available in developing countries. The alarming situation in developed countries regarding incidence rate is due to many factors. These include reproductive history, breast feeding, body weight, physical activities, alcohol consumption, shift work, and smoking [33].
Treatments
Fortunately, breast cancer one of the highly treated cancers in developed and somehow in developing countries, as the treatments are present which are playing important role in minimizing the mortality rate all over the globe. There are many treatment methods regarding Breast Cancer including.
Lumpectomy or Partial mastectomy
The surgical treatments are often used for early stage breast cancers. But in some patients, in can result in breast of different sizes and shapes. This typically involves the reshaping the breast at the time of the initial surgery and may mean operating on the other breast as well to make them more symmetrical [45].
Reconstruction Surgery
The breast reconstruction or conservation therapy is increasing steadily. This surgery rebuilds the breast mound so that it is about the same size and shape as it was before [46].
Radiation Therapy
After the breast conserving surgery, sometimes patient needs the hypofractionated radiations or accelerated partial breast irradiation. The high energy rays or particles are being targeted to the specific areas and cancer cells are destroyed. Normally, radiations are used to treat those cancers which have been spread to bones and brain [47].
Denosumab
Xgeva and Prolia (Denosumab) are used to help and strengthen and also reduce the risk of fractures in bone that have been weakened by metastatic breast cancer [48].
Chemotherapy
Chemotherapy is a treatment that uses chemicals to destroy cancer cells by targeting rapidly dividing cells in the body. Chemotherapy can be used before surgery to shrink large tumours, after surgery to kill cancer cells that may have spread to other parts of the body, or independently of surgery to slow the growth of secondary cancer. As chemotherapy is not specific to cancer cells it can destroy other rapidly dividing cells such as hair follicles and the lining of the gut, and this causes some of the side effects associated with treatment such as hair loss and nausea. Treatment is given in the form of tablets or by injection every two to four weeks over a four to six month period [47].
Anti Hormone Therapy
Some breast cancers are stimulated to grow by the hormone oestrogen, which attaches to receptors on the surface of cancer cells. These cancers are known as oestrogen receptor positive (ER+). Anti-hormone therapies block oestrogen from binding with oestrogen receptors, or stop the body from producing oestrogen altogether. Treatment is taken as a tablet once a day to reduce the long term risk of breast cancer coming back after surgery or chemotherapy. Tests can also be done to see if cancer cells are progesterone receptor positive (PR+), although the benefits of anti-hormone therapy for cancers that are only progesterone receptor positive is less clear.
Conclusion
Comparisons and contrasting data outcomes shown that there are significant similarities between Asian and western countries. The major difference is of age, peak age in Asia is between 40 to 59 but 60 to 70 is west. The incidence is although increasing in west but mortality is decreasing as compare to Asian countries. Women in Asian countries, although related to not high socio-economic status, but they give the birth to more child as compared to Western women. The breast feeding is more common in Asian women at least for 2 years to the newborn. The diet plan is also much important as Asian women do not consume much alcohol as compared to the trends in western countries. These may include the significance role in low incidence of breast cancer in Asia.
Reference