Department of Diagnostic & Biomedical Sciences, University of Texas School of Dentistry at Houston, USA
The objective of this presentation is to introduce a catalogue of salivary proteins that are altered secondary to carcinoma of the breast. The catalogue of salivary proteins is a compilation of twenty years of research by the author and consists of 233 high and low abundant proteins which have been identified by LC-MS/MS mass spectrometry, 2D-gel analysis and by enzyme-linked immunosorbent assay. Many of the identified proteins are present in the majority of cancer related pathways. Consequently, the body of this research suggests that saliva is a fluid suffused with solubilized by-products of oncogenic expression and that these proteins may be useful in the study of breast cancer progress, treatment efficacy and the tailoring of individualized patient care.
Biography:
Dr. Charles F. Streckfus is currently a professor in the Department of Diagnostic & Biomedical Sciences at the University of Texas School of Dentistry at Houston and formerly the Assistant Dean of Research at the University of Mississippi Medical center Dental School. He received his Bachelor of Science degree in Biology from Johns Hopkins University and he graduated with a DDS degree from the University of Maryland School of Dentistry. Dr Streckfus was a senior post-doctoral fellow at NIDCR and P.I. of the Oral Physiology component of the Baltimore Longitudinal Study on Aging.
Dr. Streckfus has over 100 peer-reviewed journal articles and has been invited to speak at numerous national and international conferences. He has received many honors and awards which include the prestigious Presidentʼs Award for Scientific Excellence, Presented by the International Society for Preventive Oncology, awarded at the Pasteur Institute, Paris, France, the NIH Award of Merit for his statistical analysis of the NHANES III Study, the ADA recognition award for services on the Council of Scientific Affairs, the American Academy of Oral Medicine Service Award and the Mayor of Baltimore City Baltimoreʼs Best Award for rendering dental services to the underserved citizens of Baltimore. He was granted 4 patents for his work in breast cancer biomarker research all which were assigned to the University of Mississippi Medical Center and the University of Texas Health Science Center.
The University of Texas MD Anderson Cancer Center, USA
Less than 20 years ago the only weapons in the arsenal of breast oncologists were chemotherapy and tamoxifen. Today there are many molecules that can potentially target the known oncogenes. The discovery of HER2 and the development of trastuzumab pioneered the field of targeted therapy in breast cancer. Breast imagers partner with their oncology colleagues to screen for breast cancer and to evaluate response to therapy. Although mammography, breast ultrasound, and breast MRI are excellent imaging tools, molecular breast imaging (MBI) has the potential to become a screening modality.
Biography:
Tanya W. Moseley, MD has distinguished herself as an outstanding breast radiologist, clinician, and educator. Dr. Moseley received her Doctorate of Medicine with Honors at the University of Iowa College of Medicine in Iowa City, Iowa. She entered a Clinical Residency in Diagnostic Radiology at the Mayo Clinic Graduate School of Medicine in Rochester, Minnesota, and continued on at the Mayo Clinic in a Clinical Fellowship in Mammography and Thoracic Imaging. After completing her fellowship, Dr. Moseley joined Mayo Clinic as a Senior Associate Consultant, and then joinedthe Division of Diagnostic Imaging at MD Anderson Cancer Center in 2001. She serves the institution as a Professor of Diagnostic Imaging.
Berlin Institute for Medical Systems Biology at the MDC Berlin, Germany
Metabolic reprogramming is a required step during oncogenesis. It is triggered by activation of oncogenes and loss of tumor suppressors and leads to an activation of central metabolic pathways to support cell growth and proliferation.
In order to quantify the usage and activity of metabolic pathways in vitro and in vivo we have developed pulsed stable isotope resolved metabolomics (pSIRM). The applied GC-MS based technology enables the absolute quantification of metabolites and at the same time the determination of stable isotope incorporation.
Using pSIRM we have characterized the action of inhibitors of glycolysis in cell cultures. We observed that the commonly used compound 2-deoxyglucose is not a specific glycolytic inhibitor, the action of 3-bromopyruvate as glycolytic inhibitor could be confirmed. We next analyzed the metabolic program of hepatocellular carcinoma using quantitative proteomics and in vivo isotope labelling. We further characterized the action of glycolytic inhibitors in a HCC-mouse model. Finally, we compared the metabolic phenotype of HCC between mice and humans. And observed striking similarities at the metabolic level.
Biography:
Stefan Kempa is group leader at the Berlin Institute for Medical Systems Biology BIMSB at the Max Delbruck Center for Molecular Medicine in Berlin, Germany. The group established gas chromatography coupled mass spectrometry (GC-MS) as well as liquid chromatography coupled mass spectrometry (LC-MS) based techniques to monitor the metabolome and the proteome. In addition they have developed pulsed stable isotope resolved metabolomics (pSIRM) as a tool for a dynamic metabolic characterization of cellular metabolism. Using this technology they investigate cancer metabolism aiming to improve the understanding of cancer. The specific interest is to understand metabolic dependencies of cancer cells and to improve cancer treatment.
Department of Radiology, School of Medicine, University of Pennsylvania USA
We are exploring metabolic information obtainable from nuclear magnetic resonance (NMR) and mass spectrometry (MS) to correlate cellular and tumor response to targeted signaling inhibitors. 13C NMR and MS of mantle cell lymphoma cells after incubation with13C-labeled glucose or glutamine provided isotope enrichment of several key metabolites. The enrichment information was converted to metabolic fluxes including glycolysis, pentose phosphate pathway, TCA cycle, glutaminolysis and de novo fatty acids synthesis, by using a novel bonded cumomer metabolic flux analysis. The alteration in metabolic fluxes following signaling inhibitors correlated with changes in associated gene expression as analyzed from RNA sequencing data. There was a four-fold decrease in glycolysis in RL cells vs a two-fold decrease in Jeko cells after same amount of ibrutinib, a Bruton tyrosine kinase inhibitor. Also, there was a two-fold decrease in glutaminolysis in RL cells while no change in Jeko cells. De novo fatty acids productiondecreased by two-fold in RL cells vs no change in Jeko cells. The results suggest metabolic targets of additional drugs for ibrutinib-resistant Jeko cells. The glucose uptake decreased similarly in both RL and Jeko cells after ibrutinib while there was a two-fold difference in lactate production change between RL and Jeko cells. This result suggests lactate as a promising marker of the tumor response to this signaling inhibitor. It is particularly significant because FDG-PET has been failing to distinguish responding patients from non-responding patients at interim scans during treatment. We have developed a novel 1H magnetic resonance spectroscopy (MRS) lactate imaging technique for cancer patients and pursuing its application to detecting response to signaling inhibitor therapy in lymphoma patients.
Biography:
Dr. Lee is a research assistant professor of the department of radiology, University of Philadelphia. He obtained PhD from department of physics, KAIST, Korea and had postdoc training in in vivo NMR of cells and tumors from Korea Basic Science Institute and University of Pennsylvania. His research focus is NMR/MRI based metabolic investigation of cancer in cells, animal models and human patients for the purpose of detecting early therapeutic response to novel targeted drugs. He is a recipient of ACS-IRG, ITMAT and McGaberesearch funds.
1Department of BioMolecular Sciences, National Center for Natural Products Research, University of Mississippi, and Department of Radiation Oncology, Medical Center Cancer Institute, USA
2Department of Radiology, University of Mississippi Medical Center, USA
3Department of Neuroscience, Joan C. Edwards School of Medicine, Marshall University, USA
4Department of Anatomy and Pathology, Joan C. Edwards School of Medicine, Marshall University, USA
5Department of Biology, Marshall University, USA
#These authors equally contributed.
Introduction: Prognosis of glioblastoma (GBM) treated with standard-of-care maximal surgical resection and concurrent adjuvant temozolomide (TMZ)/radiotherapy is still very poor (median survival =14.2 months). It has been observed that glioblastomas contain a small population of cancer stem cells (CSCs) that contribute to tumor propagation, maintenance, and treatment resistance. Administration of ineffective anticancer therapy is associated with unnecessary toxicity and development of resistant cancer cell clones.
We have developed a drug sensitivity assay (ChemoID) that identifies the most effective chemotherapy management against CSCs and bulk of tumor cells offering great promise for individualized anticancer treatments. A prospective study was conducted evaluating the use of the ChemoID drug sensitivity assay in glioblastoma patients treated with standard-of-care.
Methods: 30 glioblastoma patients, 18-years and older, male/females, eligible for a surgical biopsy, were enrolled in an IRB approved protocol, and fresh tissue samples were collected for drug sensitivity testing. All patients were treated with standard-of-care TMZ plus radiation with or without maximal surgery, depending on the status of the disease. Each treatment was classified by the assay as: sensitive (S = >60% cell kill), intermediate (I= 30-60% cell kill), or resistant (R= <30 cell kill). Patients were prospectively monitored for tumor response, time to recurrence, progression-free survival (PFS), and overall survival (OS). Associations of assay response for the standard-of-care TMZ selected treatment with tumor response, time to recurrence, PFS, and OS were analyzed.
Results: The median follow-up analysis was 8 months (3-49 months). ChemoID assay on CSCs demonstrated a sensitivity of 100% and a specificity of 95.83%, with a positive predictive value of 80%, and a negative predictive value of 100%. The ChemoID assay on bulk of tumor demonstrated instead a sensitivity of 100% and a specificity of 87.50%, with a positive predictive value of 57.14%, and a negative predictive value of 100%.
Overall, patients treated with assay-sensitive or -intermediate (S+I) TMZ against CSCs demonstrated significantly improved tumor response withincreased medianand mean time to recurrence, improved median PFS, and prolonged mean OS, when compared to patients treated with assay-resistant TMZ to CSCs or with assay-sensitive or –intermediate TMZ to bulk of tumor cells.
Conclusions: This prospective study compared the sensitivity of patient derived GBM CSCs and bulk of tumor cells to variouschemotherapies, demonstrating that GBM patients treated with TMZwhose CSCs were found sensitive (S+I) to TMZ, experienced improved tumor response; extended mean and median time to recurrence; improved median PFS, and prolonged mean OS.
Biography:
Dr. Claudio completed his medical and graduate training at the University “Federico II” in Naples, Italy. He then completed two postdoctoral fellowships in molecular biology and cancer biology at Temple University and at Jefferson University in Philadelphia, USA.
In 2006 he moved at Marshall University in West Virginia where he became tenured Associate Professor in the Department of Biochemistry and Microbiology and director of the Translational Laboratories at the Translational Genomic Research Institute, Edwards Comprehensive Cancer Center. There he developed the ChemoID®drug response assay, which compares the sensitivity of cancer stem cells vs. bulk of tumor cells to chemotherapy. Three international patents cover the ChemoID®procedure, which is a second-generation functional drug response assay that uses a patientʼs live tumor cells to indicate which chemotherapy agent (or “combinations”) will kill the bulk of the cancer tumor and the cancer stem cells (CSCs) that are known to cause cancer to recur. In 2010 he co-founded Cordgenics, LLC a US company that is focused on cancer stem cells diagnostics and discovery of novel therapeutics.
He moved to the University of Mississippi in 2015 as tenured Professor in the Department of BioMolecular Sciences, National Center for Natural Products Research (NCNPR), and Department of Radiation Oncology, where he became the Director of the Translational Laboratories at the Medical Center Cancer Institute.
Dr. Claudio has authored 143 publications in biomedical journals to date. He has served or serves on numerous grant review panels for NIH, NCI, DOD, and foreign research funding agencies from Italy, Germany, The Netherlands, Neurasia, and the European Commission. He serves as Editor or Associate Editor of a number of biomedical journals, and has served as an advisor to several pharmaceutical and biotechnology companies.
School of Psychological Sciences, Tel-Aviv University, Israel
Assessed psychological tendencies and attitudes identified in pretest Previous studies about psychosocial correlates of cancer patients led to inconclusive results Studies by Kreitler et al. (2002) showed that focusing on theoretically-relevant factors provides new insights into psychosocial correlates of cancer patients that have the potential of being shown to be risk factors for cancer. This approach is grounded in the Cognitive Orientation (CO) theory of health behavior and wellness which enables identifying relevant factors in cancer patients. The major constructs of this theory are beliefs of four types (about oneself, reality, goals and norms) that refer to specific themes representing underlying meanings identified by a procedure of targeted interviewing in pretest subjects. The utility of the CO approach has been proven in regard to colorectal cancer. The goal of the present talk is to examine whether psychosocial correlates grounded in the CO theory can be identified in adult breast cancer patients (Study 1) and in pediatric leukemia patients (Study 2). On the basis of previous findings it was expected that characteristic themes will be identified in each group and that they would differ in the two groups.
Study 1: The participants were250 breast cancer patients and 180 matched healthy controls. They were administered the CO questionnaire assessing psychosocial tendencies and attitudes identified in pretests as relevant for breast cancer. Discriminant and logistic regression analyses showed that patients and controls differed significantly in most of the assessed variables (belief types and themes), referring to themes, such as concern with controlling oneself and others, dependence on othersʼ evaluations, emotional blocking, and conflicts about self identity and giving to others. Some of these variables were related to medical features, none to demographic ones.
Study 2: The participants were 32 pediatric patients with leukemia (AML, CML), 27 pediatric cancer patients with solid tumors, and 30 healthy controls (age 5-10). The CO questionnaire they were administered assessed psychological tendencies and attitudes identified in pretests with children with leukemia. Analyses of variance and discriminant analyses showed significant differences between the three groups. The major discriminating themes referred to needs for freedom, routine, pleasing others, and avoidance of criticism.
Conclusions: The CO theory and methodology enable identifying sets of psychological correlates characteristic for different cancer diseases in both adults and children. These correlates have the potential of being psychological risk factors for the different diseases and could serve as basis for adjuvant psychological interventions.
Biography:
Shulamith Kreitler was born in Tel-Aviv, has studied psychology, philosophy and psychopathology in Israel, Switzerland and the USA. She got her PhD in BernSwitzerland. Has worked as a professor of psychology in different universities, including Harvard, Princeton and Yale in the USA, as well as in Argentina and Vienna, Austria. She has been a full professor of psychology at Tel-Aviv University since 1986. She is a certified clinical and health psychologist. She is the head of the psychooncology research center at ShebaMedicalCenter. Has published about 200 papers and 10 books in motivation, cognition, psychopathology and health psychology. She has created the theory of meaning, the cognitive orientation theory of behavior and wellness, and an innovative approach to psychological risk factors of physical disorders. Some of her publications: The Psychology of Art (1972), Cognitive Orientation and Behavior (1976), The Cognitive Foundations of Personality Traits (1990), Handbook of Chronic Pain (2007), Pediatric Psycho-Oncology: Psychosocial Aspects and Clinical Interventions (2004, 2012 2nd Edition), Cognition and Motivation (2012).
Dept. of Biochemistry and Molecular Biology, University of Maryland School of Medicine, USA
Obscurins, encoded by the single OBSCN gene, are giant cytoskeletal proteins containing tandem adhesion and signaling domains. The OBSCN geneis highly mutated in multiple types of cancer, including breast cancer, resulting in a 2-fold reduction of its mRNA levels. Consistent with this, obscurin proteins are nearly lost from human breast cancer cell lines and advanced stage biopsies, independently of their hormonal status or molecular differentiation. Loss of giant obscurins from breast epithelial cells confers them with a survival and growth advantage following exposure to common chemotherapies. Obscurin-depleted breast epithelial cells fail to form adhesion junctions, undergo epithelial-to-mesenchymaltransition (EMT), and generate primary and secondary mammospheres bearing markers of cancer-initiating cells. Moreover, obscurin-deficient breast epithelial cells display markedly increased motility as a sheet in 2-dimensional (2D) substrata and individually in confined spaces, and increased invasion in3D matrices. They are also capable ofextending microtentacles mediating the attachment of circulating tumor cells to the endothelium, an advantage that persists even after paclitaxel treatment. More importantly, loss of giant obscurins from breast epithelial cells promotes primary tumor formation and lung colonization in vivo. These major phenotypic alterations appear to be the result, at least in part ofincreased PI3K activity, a key regulator of tumorigenesis and metastasis. Pharmacological and molecular inhibition of the PI3K/Akt pathway in obscurin-depletedbreast epithelial cells results in reversal of EMT, (re)formation of cell-cell junctions, diminished mammosphere formation, and decreased cell migration and invasion. Coimmunoprecipitation, pull-down, and surface plasmon resonance assays revealedthat obscurins are in a complex with the PI3K/p85 regulatory subunit, and that theirassociation is direct and mediated by the obscurin-PH domain and the PI3K/p85-SH3domain with a KD of ~50 nM. We therefore postulate that giant obscurins act upstreamof the PI3K/Akt cascade in normal breast epithelial cells, regulating its activation throughbinding to the PI3K/p85 regulatory subunit.
Biography:
Aikaterini Kontrogianni-Konstantopoulos received her Ph.D. from the Department of Cell Biology at Baylor College of Medicine in Houston, TX. After graduating from Baylor, she joined the laboratory of Dr. E.J. Benz, Jr., in the Division of Hematology, at Johns Hopkins University, School of Medicine as a post-doctoral fellow. In 2007, she joined the Department of Biochemistry and Molecular Biology in the University of Maryland School of Medicine as Assistant Professor, and in 2012 was promoted to Associated Professor. Her research focuses on the elucidation of the roles of cytoskeletal and membrane-associated proteins as structural and signaling mediators. Using the muscle and epithelial cell as model systems, my laboratory has pioneered the molecular and functional characterization of the obscurin subfamily and its binding partner Myosin Binding Protein-C slow in health and disease. Her research has been funded by several organizations, including NIH, Muscular Dystrophy Association and American Heart Association.
1Department of Microbiology, Medical Laboratories Sciences, Omdurman Islamic University, Sudan
2National Ribat University College of Medical Laboratories Sciences, Sudan
3Radiation and Isotope Centre Khartoum (RICK) Khartoum, Sudan
The research studies the etiology of Leukemia. No single known cause for all of the different types of leukemia exists. Controversial hypotheses was proposed suggesting the role of physical as well as chemical and even biological factors as being responsible for Leukemia incidents. The actual cause of Leukemia which is a serious cancer in Sudan is still under scrutiny. We hypothesized that EBV could be involved in the etiology of leukemia. We describe here the results of our attempt to find a possible link between leukemia and EBV. It is generally accepted that the (EBV) is an important etiologic factor in various tumors. Virtually little was reported about the relationship between EBV genes and leukemia. However, no full-length analysis of any substrain of EBV in Sudan area has been reported. The main objective of this study is to assess the incidence and the significance of EBV in patients with leukemia disorder using diagnostic parameters including cell Morphology, immunologic markers, and molecular investigations. Our findings provided evidence of the involvement of EBV in patients with leukemia. The results suggested that EBV DNA genome encoding the non-glycosylated membrane protein BNRF1 pl43 was observed in a significant proportion of patients with ALL. We could not exclude a correlation between these viral infections and later leukemogenesis in childhood ALL in Sudan. Further investigation on the link between maternal EBV reactivation and the development of ALL in offspring needs to be explored. Neither latent infection nor congenital infection could be excluded.
Biography:
Dr. Haitham Eltigani Mohammed Alawad is currently serving as an assistant professor in virology and immunology. He is the Executive editor of Sudan medical laboratory Journal (SMLJ).
Clinical Pathologist, Assistant Professor, Dire Dawa and Haromaya University, Ethiopia
In order to know the Epidemiology of cancer in Eastern Ethiopia datas from pathology departments of Dilchora Hospital and HiwotFana Hospital were analysed. Data from Dilchora Hospital was collected for 128 cancer cases diagnosed during the year 2015 G.C.
Results on the cancer incidence by site and sex for the region was - for women the three most common malignancies in descending order of frequency are breast cancer (27.3%), hematologic malignancies (16.7%), and soft tissue sarcoma (15.2).
The figure in men in descending order of frequency is GI malignancies (18%), hematologic malignancies (17.5) and secondaries of carcinomas in cervical lymphnodes (16%).
GI malignancies are more prevalent in males (18%) than in females (6%).
Hematologic malignancies showed equal number of cases in either sexes (n=11).
The life style of men in the region like khat chewing, chronic alcoholism and cigarrete smoking seem to contribute to the higher incidence of GI malignancies and secondaries of carcinoma in the cervical lymphnodes.
The comparable risk of developing hematologic malignancies in both sexes may stem from a common environmental carcinogen which needs further intensive study.
Biography:
Getamesay Kebede is an Assistant Professor of Clinical Pathology has been working professionally since 2010 at Haromaya University, Ethiopia. He is energetic and enthusiastic on his work and researches. He has written a paper on breast cancer and has ongoing studies on tuberculosis and on infant mortality. Getamesay received his doctorate degree in medicine at Gondar University in Gondar, Ethiopia and speciality in Clinical Pathology at Addis Ababa University, Ethiopia.
1University of Milano-Bicocca, Italy
2The Netherlands Cancer Institute, Netherlands
3University of Padova, Italy
4Biotech Research and Innovation Centre, Denmark
We recently identified p65BTK, a novel oncogenic isoform of Bruton tyrosine kinase abundantly expressed in colon cancer cell lines and tissues (Grassilli et al, Oncogene 2016) and showed that its inhibition affects growth and survival of colon cancer cells.
Here we report that p65BTK expression significantlyincreases with the stage and the grade of colon carcinoma and correlates with cancer progression. In addition, p65BTK is strongly expressed in organoidsderived from stem cells purified from patientsʼ colon cancer tissues and in cancer stem cellsisolated from colon cancer specimens.
In vitro, p65BTK silencing (by siRNA or shRNA) and its inhibition by different specific inhibitors (Ibrutinib, AVL-292, RN486) sensitize drug-resistant p53-null colon cells and patient-derived organoidsto 5FU. At variance, blocking p65BTK does not restore the response of resistant cells to anti-EGFR receptor antibodies (panitumumab, cetuximab) and inhibitors (afatinib, poziotinib) or to bevacizumab. Conversely, p65BTK overexpression (but not overexpression of a kinase-dead mutant) protects p53-wt colon cancer cells from 5FU-induced cytotoxicity. Accordingly, p65BTK inhibition restores the apoptotic response to 5FU of drug-resistant p53-null colon cancer cellsvia imbalancing the anti-/pro-apoptotic ratio of Bcl-2 family members. In particular, p65BTK inhibition blunts 5FU-stimulated induction of the TGF-β pathway (anti-apoptotic) and induces E2F-mediated transcriptional regulation (apoptotic).
Finally, in xenograft experiments we confirmed that the combinationof 5FU with a BTK inhibitor (Ibrutinib) significantly reduced tumor volume in mice compared to the use of 5FU alone.
In conclusion, our data indicate that p65BTK targeting restores the apoptotic response to chemotherapy of p53-null drug-resistant colon cancer cells and suggest that the addition of BTK inhibitors to classic chemotherapy may represent a novel approach to bypass drug resistance.
Biography:
Dr. Grassilli received her Ph.D. degree from the University of Modena, Italy, and pursued her post-doctoral research at Thomas Jefferson University, Philadelphia and European Institute of Oncology, Milan, Italy studying the molecular mechanisms of apoptosis and their relevance in the response to chemotherapy. More recently, she co-founded Bionsil, a spin-off of the University of Milano-Bicocca, Italy, aimed at identifying and characterizing novel targets for molecular diagnosis and therapy of drug-resistant cancers. From 2014 she is Assistant Professor at the University of Milano-Bicocca where she continues her work on p65BTK, a novel Brutonʼs Tyrosine isoform previously identified as a new target of therapy in colon cancers.
1Escuela Nacional de Ciencias Biológicas, Instituto Politécnico Nacional, México
2Escuela Superior de Medicina, Instituto Politécnico Nacional, México
Cervical cancer is the largest cancer incidence in Mexico and is the leading cause of cancer death among Mexican women. Risk factors involve early onset of sex, having multiple sex partners and having had sexually transmitted diseases, besides the poor hygiene, use of snuff, alcohol or contraceptives, and late detection, are main causes in the acquisition, manifestation and progression of cervical cancer.
Objective: To determine the anticancer activity of 6-10 and 11-15 fractions of ethanolic extract of Sternocereusgriseus H in a model cell lines HeLa.
The main objective of this work is to determine the cytotoxic activity of secondary metabolites obtained from various fractions of ethanol extract of Sternocereusgriseuss. the fruits in the Merced Market, which came from the State of Veracruz were purchased. The fruit was placed in a percolator and 6.5 liters of ethanol was added 96°, the mixture was allowed to stand at room temperature for 5 days. Then it evaporated under reduced pressure to a crude extract, which she underwent preliminary chemical tests. Will extract was subjected to various chromatography techniques, using different stationary and mobile phases. Fractions had similar Rf gathered. To determine the cytotoxic activity of Vero cells culture and HeLa cells was performed by incubating for 12 hours, the time elapsed proceeded to add the extract fractions Sternocereusgriseuss H at different concentrations and incubated for 12 hours. At the end of this time, the cells were recovered and preceded to staining with annexin V-FITC and propyl iodide to determine the antitumor activity of fractions. Inextract Sternocereusgriseuss H were identified xanthones, flavones, aurones, coumarins and other phenolic compounds, triterpenes and reducing sugars. Column chromatography of fractions 1-5 and 11-15 two cytotoxic activities in the HeLa cell line were isolated. The two isolated fractions produced apoptotic activity and fraction 11 -15 showed higher activity necrosis and apoptosis.
Biography:
Rafael Silva Torres has completed his PhD. from EscuelaNacional de CienciasBiológica of National Polytechnic Institute and abroad studies M. Phil. from Loughborough University of Technology Great Britain and sabbatical year from Museum National D`HistoireNaturelle Paris France. He has published more than 15 papers in reputed journals and 4 book chapters and has been serving as editorial board member of repute journals. He was director of 49 Bsc. Thesis and he was participated in more than 150 national and international congresses. He is membership of National Association of Pharmaceutical Sciences and American Chemical Society. He is investigating the properties antitumor of medicinal plants such as: Sedum praealtumDC., Sechiumedule and Stenocereusgriseus H.
1University of Maryland Marlene and StewartGreenebaum NCI Cancer Center, USA
2University of Maryland Graduate Program in Life Sciences, Program in Molecular Medicine, USA
3Department of Physiology, University of Maryland School of Medicine, USA
Patients diagnosed with triple negative breast cancer (TNBC) develop detectable metastatic disease within an average of only three years, and virtually all women with metastatic TNBC will die of their disease despite treatment. The short time period for developing metastases is due to presence of disseminated disease. Disseminating tumor cells circulate within the bloodstream during an intermediate step of the metastatic cascade. An increase in disseminating tumor cells correlates with disease progression and thus the number of circulating tumor cells are used for diagnostic purposes. However, very little is known about their biology. When in the bloodstream, these tumor cells are in a detached and free-floating state. Recently, we demonstrated that the regulation of the actin cytoskeleton differs in attached versus detached cells, leading to the conclusion that there are crucial targetable cytoskeletal signaling changes specific to detached, disseminating cells. In only detached cells, we determined that PTEN regulates the actin severing protein, cofilin, via a PI3K-independent mechanism. PTEN loss promotes cofilin activation leading to a weakened actin cortex. The weakening of the actin cortex increases cell deformability to enhance both tumor cell survival and cell reattachment. Our objective is to elucidate the mechanism by which PTEN regulates cofilin in detached cells to gain a greater understanding of how disseminating tumor cells control deformability. We hypothesize that PTEN loss weakens the actin cortex which enhances disseminated tumor cell deformability to promote metastatic efficiency. An improved understanding of the biochemical signals which modulate cytoskeletal alterations specifically in detached TNBC cells will provide new insight into the development of pharmacologic approaches for inhibiting metastasis by regulating cell deformability.
Biography:
After attending Franklin and Marshall College, Dr. Vitolo began her career as a laboratory technician. After a few years, she returned to school to obtain her Ph.D. in Biochemistry from the University of Maryland Baltimore where she is currently an Assistant Professor.
Dr. Vitolo has a long-standing interest in the molecular genetics of cancer. Her work focuses on the loss of the tumor suppressor PTEN and the progression of breast cancer. Over the years she has co-authored 29 publications and has acquired funding from numerous sources including the American Heart Association, Susan G. Komen Organization, American Cancer Society, and the National Cancer Institute.
Sidney Kimmel Comprehensive Cancer Center, Johns Hopkins, USA
Perturbations in the adipocytokines-profile, especially higher levels of leptin, are a major cause of breast tumor progression and metastasis. The focus of this talk is to discuss the impact of obesity on cancer with a special focus on breast cancer, discuss the underlying molecular mechanisms and discuss the potential therapeutic opportunities
Biography:
Sharma attained her Ph.D. in Oncology followed by postdoctoral training at University of Maryland and Johns Hopkins University. Dr. Sharma is an Associate Professor of Oncology at Sidney Kimmel Comprehensive Cancer Center at Johns Hopkins. Her lab focuses on investigating the molecular links between obesity and cancer, emphasizing aspects that have potential clinical significance. They are exploring new strategies to disrupt obesity-cancer connection using a variety of approaches. Their overall goal is to understand the molecular networks by which obesity affects carcinogenesis and discover novel agents to effectively disrupt obesity-cancer axis.
National Institute of Cancer Research, National Health Research Institutes, Taiwan
Gemcitabine has been a first-line therapeutic agent for pancreatic ductal adenocarcinoma (PDAC); however, the acquisition of resistance to gemcitabine remains a major challenge. Here, we investigated the metabolite profiles by liquid chromatography-mass spectrometry between gemcitabine–resistant PDAC and parental PDAC cells, and found that lactic acid amount and lactate dehydrogenase activity were increased in gemcitabine–resistant PDAC cells. We observed the elevated lactate dehydrogenase A (LDHA) expression significantly correlated with recurrent pancreatic cancer patients following gemcitabine treatment and with cancer stem cell (CSC) properties. By approachingthe comparative array-based microRNA (miRNA)expression and miRNA transcription analysis, we further identified that FOXO3a-induced miR-4259 directly targeted the 3ʼuntranslated region of LDHA and reduced LDHA expression, leading to decreased gemcitabine resistance and a reduction in the CSC phenotypes of pancreatic cancer in vitro and in vivo. Our findings suggest that LDHA might serve as a potential prognostic markerand therapeutic target for pancreatic cancer, particularly gemcitabine-resistant pancreatic cancer, and may provide evidence of an underlying epigenetic regulation of LDHA by FOXO3a/miR-4259, which appears to be involved in cancer stemness and the chemoresistance of pancreatic cancer.
Biography:
Ching-Feng Chiu has completed his Ph.D from National Cheng Kung University of Taiwan and postdoctoral studies from Taipei Medical University and National Health Research Institutes. Now he serves as an Independent-Postdoctoral Fellowship of National Institute of Cancer Research in National Health Research Institutes, and hisstudies focus onthe roles of microRNAs and metabolism in tumor metastasisand drug resistance from basic research to clinical application. Over the past 5 years, he has published more than 12 original research papers, and he was awarded the9th National Innovation Award in 2012 and obtainedthe three-year research grant of Ministry of Science & Technologyof Taiwan in 2015.
1Computer-Aided Drug Design Center, University of Maryland, School of Pharmacy, Department of Pharmaceutical Sciences, USA
2Weill Cornell Medical College, Department of Hematology/Oncology, USA
3University of California San Francisco, Department of Laboratory Medicine, USA
4University of Michigan, Department of Pathology, USA
5Department of Pathology and Laboratory Medicine, Weill Cornell Medical College, USA
The BCL6 oncogene is constitutively activated by chromosomal translocations and amplification in ABC-DLBCLs, a class of DLBCLs that respond poorly to current therapies. BCL6 mediates its effects by recruiting corepressors to an extended groove motif thereby repressing expression of selected proteins, including those in checkpoint pathways and IRF4 and PRDM1, thereby blocking plasma cell differentiation. Accordingly, we have undertaken a drug design campaign to develop inhibitors of BCL6-corepressor interactions. Towards this goal we applied the Site Identification by Ligand Competitive Saturation (SILCS) methodology in conjunction with synthetic chemistry, structural biology and biological evaluation. SILCS involves the calculation of functional group affinity maps of proteins; these “FragMaps” take into account protein flexibility, protein and functional group desolvationpenalties as well as protein-functional group interactions. FragMaps may be used to qualitatively direct ligand design as well as quantitative predict relative binding affinities of 1000s of compounds on a daily basis, at an accuracy comparable to free energy perturbation, thereby allowing SILCS to lead the drug design process. Based on the SILCS approach, the role of functional groups to affinity was determined for the lead compound, 79-6, targeting BCL6, acting as the basis for the design and in silico evaluation of lead compound analogs. Subsequent synthesis and experimental evaluation of the predicted compounds showed them to bind to BCL6 in the predicted binding orientation. Notably, the new compound, termed FX1, has an affinity for BCL6 higher than that of the corepressors indicating its potential as a drug candidate. FX1 disrupts BCL6 repression complex formation, reactivates BCL6 target genes, and mimics the phenotype of mice engineered to express BCL6 with lateral groove mutations. This compound eradicated established DLBCLxenografts at low doses. Most strikingly, FX1 suppressed ABC-DLBCL cells as well as primary human ABC-DLBCL specimens ex vivo.
Biography:
Alex MacKerell received an A.S. in Biology from Gloucester County College, a B.S. in Chemistry from the University of Hawaii and a Ph.D. in Biochemistry from Rutgers University. Subsequent training involved postdoctoral fellowships in the Department of Medical Biophysics, KarolinskaIntitutet, Stockholm, Sweden in experimental and theoretical biophysics and in the Department of Chemistry, Harvard University in theoretical chemistry. MacKerell is currently the Grollman-Glick Professor of Pharmaceutical Sciences in the School of Pharmacy, University of Maryland, Baltimore and the Director of the University of Maryland Computer-Aided Drug Design Center. MacKerell is also Co-founder and Chief Scientific Officer of SilcsBio LLC. Research interests include the development of theoretical chemistry methods, with emphasis on empirical force fields, including the CHARMM additive and Drude polarizable force fields, structure-function studies of proteins, carbohydrates and nucleic acids, and drug design and development.
Northern Institute for Cancer Research, School of Chemistry, Newcastle University, UK
The cellular response to DNA double-strand break (DSB) formation is an essential component of normal cell survival, following exposure to DNA-damaging chemicals (e.g. cisplatin and doxorubicin) and ionising radiation.1 The serine/threonine kinase DNA-dependent protein kinase (DNA-PK) is a member of the phosphatidylinositol (PI) 3-kinase related kinase (PIKK) family of enzymes, and plays an important role in DNA DSB repair via the non-homologous end-joining (NHEJ) pathway.2 DNA-PK inhibitors may, therefore, be useful as agents to improve the activity of radio- and chemo-therapy in the treatment of cancer.3 Identification of the lead benzo[h]chromen-4-one DNA-PK inhibitor NU7026 (IC50 = 0.23 μM), guided the subsequent development of the potent and selective ATP-competitive chromenone NU7441 (DNA-PK IC50 = 30 nM).4 Although proof-of-principle studies with NU7441 confirmed promising activity in vitro as a chemo- and radio-potentiator in a range of human tumour cell lines,5 further biological studies with NU7441 were hampered by sub-optimal pharmaceutical properties.
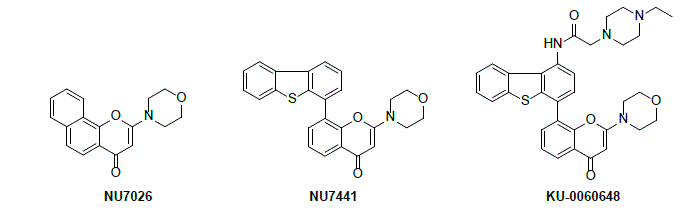
In collaboration with AstraZeneca Pharmaceuticals, structure-activity relationship studies for DNA-PK inhibition by chromenone-derivatives were conducted in conjunction with homology modelling. This approach predicted several positions on the pendant dibenzothiophen-4-yl substituent of NU7441 as tolerant to substitution, without detriment to DNA-PK inhibitory activity. We will describe the rational design and syntheses of analogues that optimised the physicochemical and pharmacokinetic properties of NU7441. These studies resulted in the identification of compounds that combined potent DNA-PK inhibition with excellent aqueous solubility (20-40 mg/mL as acid salts), without compromising cellular activity. Prominent amongst these derivatives is KU-0060648 (DNA-PK IC50 = 8.6 nM), which exhibits 20-1000 fold selectivity for DNA-PK over related PIKK enzymes and PI3K family members. The discovery and further development of KU-0060648 and analogues will be described, including in vivo efficacy and combination studies.6-8
Biography:
Dr. Celine studied Organic Chemistry at the University of Poitiers (France) where she received her Ph.D. degree in 2004 for research on the synthesis of biomolecules by 1,3-dipolar cycloadditions with carbohydrates. From 2004-5, she carried out post-doctoral work in the group of Professor John A. Joule at the University of Manchester working on the synthesis of analogues of cofactors of oxomolybdoenzymes. In November 2005 she joined the Northern Institute for Cancer Research at Newcastle University as a research associate, working along Professors Roger Griffin and Bernard Golding on the synthesis of inhibitors of DNA-dependent protein kinase (DNA-PK). She was appointed to a lectureship at Newcastle in 2008, promoted to senior lectureship in 2013, and has since played a key role in helping to establish Newcastle as an internationally recognised centre for anti-cancer drug development.
Departments of Internal Medicine and Molecular Biology, UT Southwestern Medical Center, USA
Histone lysine demethylase KDM4/JMJD2s are overexpressed in many human tumors including prostate cancer (PCa). KDM4s are co-activators of androgen receptor (AR) and are thus potential therapeutic targets. Yet to date few KDM4 inhibitors that have anti-prostate tumor activity in vivo have been developed. Here, we report the anti-tumor growth effect and molecular mechanisms of three novel KDM4 inhibitors (A1, I9, and B3). These inhibitors repressed the transcription of both AR and BMYB-regulated genes. Compound B3 is highly selective for a variety of cancer cell lines including PC3 cells that lack AR. B3 inhibited the in vivo growth of tumors derived from PC3 cells and ex vivo human PCa explants. We identified a novel mechanism by which KDM4B activates the transcription of Polo-like kinase 1 (PLK1). B3 blocked the binding of KDM4B to the PLK1 promoter. Our studies suggest a potential mechanism-based therapeutic strategy for PCa and tumors with elevated KDM4B/PLK1 expression.
Biography:
Dr. Zhi-Ping Liu obtained her PhD in Biophysics and post-doctoral training in Molecular Biology at UT Southwestern Medical Center. She is now an associate professor in the department of internal medicine, UT Southwestern. Her research focuses on the transcriptional regulation of genes involved in cancer and cardiovascular diseases.
Istituto Italiano di Tecnologia (IIT), Italy
Disruption of the circadian clock has been associated with a variety of human pathologies, including metabolic dysfunctions and cancer. Nevertheless, whether pharmacological targeting of circadian regulators is a viable approach to cancer therapy remained to be determined. We recently reported that the circadian regulator REV-ERBβ is overexpressed in many tumor cells and it plays an unexpected role in sustaining cancer cell survival when the autophagy flux is compromised. Our studies also identified the first compound with a dual inhibitory activity toward autophagy and REV-ERBβ, which showed a more potent anticancer activity than the clinically relevant autophagy inhibitor, chloroquine (CQ), against different human tumor tissue cells. Further structure-activity relationship (SAR) analysis on the hit compound identified a class of molecules with a higher inhibitory potency toward REV-ERBβ, resulting in higher cancer-specific cytotoxicity. Notably, in a number of CQ-resistant cancer cell lines, our dual REV-ERB/autophagy inhibitors inhibited growth at low micro-molar concentration, suggesting their use as novel anticancer agents for the treatment of chloroquine-resistant tumors. In addition, we obtained preliminary data indicating a REV-ERBβ-mediated regulation of cancer metabolism, which it has recently become one of the most exciting and promising areas for the development of antitumor drugs. As a consequence, REV-ERBβ inhibition may be suitable for combinatorial therapy with a number of metabolic-related anticancer agents.
In addition to provide a scaffold for the development of novel anticancer agents, these dual inhibitors can be used as valuable pharmacological tool for elucidate novel crosstalk between circadian rhythm, cancer metabolism and autophagy.
Biography:
Dr. Benedetto Grimaldi obtained in 2001 the degree in Biological Science with a summa cum laude from the University of Rome “La Sapienza”.
After obtained a PhD in Genetics and Molecular Biology at University of Rome, specializing in the study of epigenetics and signal transduction, Dr. Grimaldi transitioned into a postdoctoral fellowship under the mentorship of Prof. Sassone-Corsi (University of California, Irvine, USA), a leader in the field of circadian clock, metabolism and epigenetics. Since 2015, Dr. Grimaldi works as a Senior Researcher at the IstitutoItaliano di Tecnologia (Italy), focusing on the study of the links between clock factors and human pathologies, and on the identification and evaluation of novel molecules with “clock modulator” activity for therapeutic applications.
1Korea Research Institute of Bioscience & Biotechnology, Korea
2Department of Pharmacology, DongKook University, Korea
Hypoxia induces HIF1α expression, leading to the malignant cell transformation. In screening of inhibitors against HIF1α expression using a reporter gene assay system, a moracin derivative, MOA, was found to strongly reduce the level of HIF1α in HeLa cellsboth in hypoxia-mimetic CoCl2treatment and under hypoxic conditions. Identification of binding proteins using agarose-bead conjugated MOA(AC-685) combined with subsequent MS data revealed several proteins affected by MOA. AC-685 co-localized with a nuclear hnRNPX protein in CoCl2 treated HeLa cells. Amongst several cytoplasmic or nuclear proteins, hnRNPX was only found to be responsible for CoCl2-induced HIF1α expression as supported by siRNA depletion of the protein. Cancer growth was also found to be reduced in a genograft animal model. This study suggests that regulation of HIF1α expression by MOA under the control of hnRNP would be a novel approach to cancer treatment in hypoxic environment.
Biography:
Dr. Bo Yeon Kim got Ph.D degree at Seoul National University in 1996. After the research fellow experience at Georgetown University, 2000-2003, he continued his work at Korea Research Institute of Bioscience & Biotechnology (KRIBB) for about 26 yrs so far. Major research focuses on identification of new cancer signaling pathways and development of a new anticancer drug with low side effect. In recent 5 years, He has made more than 65 publications, including Nature Cell Biology (2015), Autophagy (2016, 2013), Proc Natl Acad Sci, USA (2013), J Am Chem Soc (2011), J Biol Chem (2013, 2012), and under revision papers (Nature Communicaitons, EMBO Reports, Autophagy) as a corresponding author.
Molecular Therapeutics Group, Fox Chase Cancer Center
The tumor suppressor protein p53 is mutated or deleted in more than half of human cancers. The most frequently occurring of these loss-of-function mutations are localized to the p53 “core domain,” but do not involve surface residues directly responsible for function. Rather, these point mutants reduce the thermodynamic stability of this marginally stable protein, such that cellular activity is diminished because an insufficient amount of p53 is correctly folded. We sought to identify compounds that bind and stabilize correctly folded p53, expecting that stabilization through this mechanism will restore activity to this most frequently occurring class of p53 point mutants, and further will restore activity to these destabilized mutants.
Using new computational tools developed in my lab, we have discovered a new druggable site on the surface of the p53 core domain, and identified compounds designed to interact with this surface. Through biochemical assays we find that these compounds are effective at stabilizing multiple different p53 mutants. We further find that these compounds can restore transcriptional activity in cell lines harboring destabilized mutants of p53, without affecting cells that have wild-type p53.
Thus, this new druggable site may provide a starting point for developing a new class of therapeutics that selectively re-activate p53 – regardless of precisely which mutation is responsible for the underlying loss of protein function. We also expect that refinement of our novel screening platform will additionally enhance its utility for identifying reactivators of other select proteins that are frequently deactivated in human cancers by destabilizing mutations.
Biography:
John Karanicolas is currently an Associate Professor at the Fox Chase Cancer Center, in the Molecular Therapeutics Program. He was granted a PhD from Charlie Brooksʼ lab at The Scripps Research Institute in 2003, for his work using molecular dynamics simulations to study protein folding. He then moved to a postdoc in David Bakerʼs lab at the University of Washington, where he studied protein design and added a wetlab component to his research. He started his lab at the University of Kansas in 2008, focusing on developing structure-based approaches for modulating protein function using small-molecules. He moved his lab to Fox Chase in 2016, where his research follows two parallel themes: the first is re-engineering proteins so that a small-molecule can be used to “turn on” function, and the second is identifying small-molecules that naturally complement and occlude a protein interaction sites to “turn off” function.
Division of Magnetic Resonance Research, Russell H. Morgan Department of Radiology and Radiological Sciences, Johns Hopkins University School of Medicine, USA
Institute for Cellular Engineering, Johns Hopkins University School of Medicine, USA
NeuroRepair Department, Mossakowski Medical Research Centre, Poland
Neurological disorders constitute one of the biggest medical challenges. Although there has been rapid progress in the treatment of peripheral malignancies over the last 20 years, the prognosis for brain tumors is imperturbably grim. However, many drugs, including melphalan, are highly effective in vitro. Moreover, intra-arterial delivery of high-dose melphalan radically changed the treatment of retinoblastoma, with a frequent cure rate, without the need for eye removal. However, melphalan, as well as many other antineoplastic agents, cannot effectively cross the blood-brain barrier, thus limiting their efficacy for the treatment of brain tumors. The opening of the blood brain barrier (BBB) to facilitate tumor penetration by drugs has been attempted for many years. Intraarterial administration of hyperosmotic agents (IAHA) has been shown safe, but high variability of results was discouraging and the method has been almost abandoned. We have found that MRI contrast agents are sufficiently sensitive to report on the brain territory supplied by a catheter thus MRI is critically needed to guide the intra-arterial delivery of therapeutic agents to the brain. Superparamagnetic iron oxide nanoparticles (SPIO) are very attractive as contrast agents due to their very strong signal, which allows for a very short MRI acquisition time, e.g., two to three seconds, using a GE-EPI pulse sequence. This actually enables real-time monitoring of the territory supplied by the catheter. In addition, the SPIO clears rapidly after infusion discontinuation, which, in turn, allows for precise adjustments of the territory supplied by the catheter through manipulation of the speed of infusion and the catheter tip position. Moreover, we have shown that the delineation of the brain territory supplied by the catheter also allows for precise prediction of the subsequent BBB opening area, which, in turn, overcomes the previously reported problems with the variability of the BBB opening territory after IAHA. This then, allows for a new era of predictable and precise intra-arterial drug delivery to the brain (Janowski et al. 2015). Thus, in our opinion, the intra-arterial delivery of therapeutic agents through a predictable and precise blood brain barrier opening should always be attempted before the agent is deemed ineffective. Our method can also be potentially useful for other neurological disorders, such as neuroinflammatory and neurodegenerative conditions.
1. Janowski M, Walczak P and Pearl MS (2015). Predicting and optimizing the territory of blood-brain barrier opening by superselective intra-arterial cerebral infusion under dynamic susceptibility contrast MRI guidance. J Cereb Blood Flow Metab.2016 Mar;36(3):569-75
Biography:
Dr Janowski completed residency in neurosurgery at the Medical University of Warsaw, Poland and then moved to Department of Radiology at the Johns Hopkins University, USA where he holds a position of Associate Professor. His research is focused on the development of the precise methods to deliver high doses of therapeutic agents including drugs and stem cells to the desired areas of the brain. He has published over 40 papers in peer reviewed journals, edited a book on experimental neurosurgery, served as a program chair for workshop, chaired multiple sessions at international conferences and gave over 15 invited talks worldwide. His research is funded by NIH, DoD and Maryland Stem Cell Research Fund.
Université de Lyon, Centre de Recherche en Cancérologie de Lyon, France
Local invasion can be considered as an initial and essential step in the malignancy of carcinomas, leading to the generation of distant metastasis. Metastasis remains the major cause of cancer-related mortality and currently, there is a lack of therapies that can efficiently prevent this process. The molecular mechanisms governing tumor progression, including metastasis development, are still poorly understood. During this process, cells acquire apoptosis resistance which is often correlated with alteration of Bcl-2 family proteins status. Bcl-2 family members are the main regulators of apoptosis. Upregulation of the anti-apoptotic members in wide range of cancers including breast cancer is often correlated with chemotherapy resistance and poor prognosis. Thus targeting the activity of Bcl-2 family proteins represents promising strategies for the elaboration of cancer therapeutic.
Bcl-2 proteins have been studied intensively for the past two decades owing to their importance in the regulation of apoptosis, tumorigenesis and cellular responses to anti-cancer therapy. However, increasing data suggest additional roles, including regulation of the cell cycle, metabolism and cytoskeletal dynamics. Using zebrafish as a vertebrate model we demonstrated that two Bcl-2 homologs, Nrz and Bcl-wav, orchestrate morphogenic movements by controlling the intracellular Ca2+ trafficking during early development. Nrz silencing causes development arrest followed by detachment of the entire blastomeres from the yolk sac. Time-lapse and confocal microscopy experiments demonstrated that this phenotype is due to the premature formation of actin-myosin complexes, giving rise to a contractile structure that squeezes the embryo margin and prevents epiboly progression. At the ER membranes, Nrz interacts with the IP3 binding domain of the IP3R1 Ca2+ channel. This interaction regulates the time course of Ca2+ transients in the yolk sac that consecutively controls the formation of actin-myosin cables via the CaMKII-MLCK pathway.
Put into a broader context our results established for the first time that members of the Bcl-2 family are able to control cell migration in a calcium dependent manner via their direct interaction with intracellular Ca2+ channels and thus independently of their involvement in the regulation of cell death. Together our results may also contribute to a better understanding of the molecular mechanisms underlying metastasis formation.
Biography:
Dr. Germain GILLET is a Professor in the Université Claude Bernard Lyon 1 (UCBL), France and Chair, Scientific Council UCBL ; Group leader at CRCL. His current research is focused on The molecular mechanisms governing tumor progression, including metastasis development, are still poorly understood. We showed that some members of the Bcl-2 family are able to control cell migration in a Ca2+-dependent manner via their direct interactions with Ca2+ channels, independently of their involvement in apoptosis. Using genetically engineered mouse and zebrafish models, we are analyzing the molecular mechanisms by which members of the Bcl-2 family influence cell survival and cell migration. We intend to (i) identify the signaling networks that lead to the modulation of Ca2+ homeostasis and cell movements by Bcl-2 family proteins (ii) identify the factors involved in apoptosis progression and cell migration (iii) review the roles played by these factors, depending on the pathophysiological context.
It is anticipated that this work will lead to the identification of novel prognosis markers and might deliver potential molecular targets for the control of tumor-growth and formation of metastases.
Developmental Therapeutics Branch, National Cancer Institute, NIH, USA
Whole-chromosomal instability (CIN), manifested as unequal chromosome distribution during cell division, is a distinguishing feature of most cancer types. CIN is generally considered to drive tumorigenesis, but a threshold level exists whereby further increases in CIN frequency in fact hinder tumor growth. While this attribute is appealing for therapeutic exploitation, drugs that increase CIN beyond this therapeutic threshold are currently limited. In our previous work, we developed a quantitative assay for measuring CIN based on the use of a non-essential human artificial chromosome (HAC) carrying a constitutively expressed EGFP transgene. Here, we used this assay to rank 62 different anticancer drugs with respect to their effects on chromosome transmission fidelity. Drugs with various mechanisms of action such as antimicrotubule activity, histone deacetylase (HDAC) inhibition, mitotic checkpoint inhibition, and targeting of DNA replication and damage responses were included in the analysis. Ranking of the drugs based on their ability to induce HAC loss revealed that paclitaxel, gemcitabine, dactylolide, LMP400, talazoparib, olaparib, peloruside A, GW843682, VX-680, and cisplatin were the top ten drugs demonstrating HAC loss at a high frequency. Therefore, identification of currently used compounds that greatly increase chromosome mis-segregation rates should expedite the development of new therapeutic strategies to target and leverage the CIN phenotype in cancer cells.
Biography:
Natalay Kouprina received her M.Sc. in physical chemistry from the St. Petersburg State University, Russia, and her Ph.D. and Dr.Sc. in cell biology from the Institute of Cytology, Russian Academy of Sciences. While in Russia, she worked on the identification of genes that control the replication and segregation of chromosomes in budding yeast. In 1991 she moved to the United States and focused her interests on human genome. Her current interest is to combine a transformation-associated recombination (TAR) cloning technology for selective isolation of a large segments from complex genomes with the human artificial chromosome (HAC) –based vectors to develop a novel system for delivery and expression of full-length mammalian genes for functional genomics that has a great potential for gene therapy. At present she is a staff scientist at the National Cancer Institute, NIH, USA. She has 101 publications in many leading international journals and 7 US patents. She is an editorial board member of several international journals. She was an Invited Guest Editor of special issues of few journals. Natalia Kouprina was a co-organizer of several international conferences.
Stanford University School of Medicine, SBI Company, USA
Background: HER2 is overexpressed in aggressive breast. We are using extracellular vesicles (EVs)for targeting our novel prodrug/Enzyme (CNOB/ChrR6) regimen specifically to HER2 positive cancer; the cytotoxic product of this regimen, MCHB, can be visualized noninvasively in living mice. We are using mRNA for gene delivery which is superior to DNA, as it eliminatestranscription issues. This therapeutic approach may lead to personalized medicineusing EVsfrom a patientʼs own dendriticcells (DCs).
Aim: To use HER2-targeting EVs for specific and effective delivery ofthe prodrug therapyto HER2 cancer, and characterize pharmacokinetics/pharmacodynamics (PK/PD)aspects of the regimen.
Methodology: Usingexosome-display technology, weconstructed a chimeric protein, anti-HER2(ML39) scFv conjugated to the lactadherin C1C2 domain. After 4-day incubation of transiently transfected HEK293 cells, EVswereharvested, andpurechimeric protein was isolated using His-tag columns. Naïve HEK293 or DC EVswere reconstituted with the chimeric protein. ELISA quantified the specificity of the resultingEVs. For cell binding assays, CFSE-labeled targeted EVs (or EVs displaying the targeting antibody and a C1-C2-linked reporter) were incubated with BT474(strongly HER2+ve)or MCF7 cells(little HER2 expression), and visualized by fluorescence microscopy. To determine mRNA transfer capability, the directed EVs were loaded with ChrR6 mRNA by XPort-based technology, and incubated with BT474 cells followed by CNOB treatment. MCHB production was quantified by fluorescence, andcell viability was determined by the MTT assay. In vivo PK/PD was examined by using imaging and LC/MS/MS for tissue drug quantification, followed by modeling and simulation via Phoenix WinNonlin software.
Results: Transfected HEK293 cells generated EVs expressing the anti-HER2 scFv/C1C2 protein (“directed EVs”). DCs lack lactadherin and generate naïve EVs. These were incubated with the chimeric protein. The resulting directed EVs showed 10 times greater targeting capacity than EVs from the transfected HEK293 cells; such EVs bound BT474 cells, while their binding to MCF7 cellswas negligible. Directed, loaded EVs specifically conferred transcription-independent capacity on BT474 cells to activate CNOB (MCHB fluorescence generation), showing successful delivery of translationally-competent ChrR6 mRNA; they also generated much greater killing ofBT474 cells than the non-directed EVs. Early in vivo results corroborate these findings. The PK/PD studies pointed to an effective in vivo dosing regimen of CNOB/ChrR6for cancer treatment.
Conclusions: We have successfully engineered EVs, which arecapable of specific high level HER2 binding capacity, functional delivery of therapeutic of mRNA, and generating CNOB mediated specific killing of HER2+ cells.
Biography:
Professor Matin has been affiliated with Stanford Medical School for several years and is also a member of the faculty of several other Stanford programs. He is an elected member of the American Academy of Microbiology and has been an invited member of several programs and organizations. Besides cancer, he has contributed extensively to bacterial antibiotic resistance mechanisms, molecular basis of life in extreme acidic environments, and the molecular and biological adaptations that enable bacteria to survive nutrient dearth and other stresses. Currently he is working also with NASA to test bacterial antibiotic resistance during space flight.
Harvard TH Chan School of Public Health, USA
A bimodal pattern of hazard of relapse among early stage breast cancer patients has been identified in multiple databases from US, Europe and Asia. We are studying these data to determine if this can lead to new ideas on how to prevent relapse in breast cancer. Using computer simulation and access to a very high quality database from Milan for patients treated with mastectomy only, we proposed that relapses within 3 years of surgery are stimulated somehow by the surgical procedure. Most relapses in breast cancer are in this early category. Retrospective data from a Brussels anesthesiology group suggests a plausible mechanism. Use of ketorolac, a common NSAID analgesic used in surgery was associated with far superior disease-free survival in the first 5 years after surgery. The expected prominent early relapse events in months 9-18 are reduced 5-fold. Transient systemic inflammation accompanying surgery (identified by IL-6 in serum) could facilitate angiogenesis of dormant micrometastases, proliferation of dormant single cells, and seeding of circulating cancer stem cells (perhaps in part released from bone marrow) resulting in early relapse and could have been effectively blocked by the perioperative anti-inflammatory agent. If this observation holds up to further scrutiny, it could mean that the simple use of this safe, inexpensive and effective anti-inflammatory agent at surgery might eliminate early relapses. We suggest this would be most effective for triple negative breast cancer and be especially valuable in low and middle income countries. Similar bimodal patterns have been identified in other cancers suggesting a general effect.
Biography:
Michael Retsky (PhD in Physics from University of Chicago) made a career change to cancer research thirty years ago. He is on staff at Harvard TH Chan School of Public Health and faculty at University College London. He was on Judah Folkmanʼs staff at Harvard Medical School for 12 years. Retsky is Editor of a Nature/Springer book on breast cancer to be published in 2016 and Editor-in-Chief of the Journal of Bioequivalence and Bioavailability. He is a founder and on the Board of Directors of the Colon Cancer Alliance and has published more than 60 papers in physics and cancer.
Biomedical Center and Peter the Great St.Petersburg Polytechnic University, Russia
Earlier I formulated the hypothesis of the possible evolutionary role of tumors. This hypothesis suggests that tumors supply evolving multicellular organisms with extra cell masses for the expression of newly evolving genes. After expression of novel genes in tumor cells, tumors differentiate in new directions and give rise to new cell types, tissues and organs.
In the presentation, the bulk of data supporting the positive evolutionary role of tumors will be reviewed, obtained both in the lab of the author and from the literature sources.
The following issues will be addressed: the widespread occurrence of tumors in multicellular organisms; features of tumors that could be used in evolution; the relationship of tumors to evo-devo; examples of recapitulation of some tumor features in recently evolved organs; the types of tumors that might play the role in evolution; examples of tumors that have played the role in evolution.
The discussion of experimental confirmation of nontrivial predictions of the hypothesis will include the analysis of evolutionary novelty of tumor-specifically expressed EST sequences; ELFNI – AS1, a human gene with possible microRNA function expressed predominantly in tumors and originated in primates; PBOV1, a human gene of the recent de novo origin with predicted highly tumorspecific expression profile; the evolutionary novelty of human cancer/testis antigen genes; etc.
The conclusion is made that expression of protogenes, evolutionarily young and/or novel genes in tumors might be a new biological phenomenon, a phenomenon of TSEEN (Tumor Specifically Expressed, Evolutionarily New) genes, predicted by the hypothesis of evolution by tumor neofunctionalization.
Biography:
Andrei P. Kozlov, Ph.D., Dr.Sci., Professor of Molecular Biology, was born in Leningrad in 1950. In 1972 he graduated with honors from St. Petersburg State University (Department of Biochemistry). During the period 1972-1975, he completed postgraduate studies at the N.N. Petrov Research Institute of Oncology and successfully defended his Ph.D. thesis devoted to the studies of low molecular weight nuclear RNAs in normal and tumor tissues. In 1978-1979 Dr. Kozlov served in a tenured Research Training Fellowship awarded by the International Agency for Research on Cancer at the laboratory of Robert Gallo at the National Cancer Institute.
1Virginia Tech Carilion Research Institute, USA
2Department of Biological Sciences and Pathobiology, Virginia-Maryland College of Veterinary Medicine, Virginia Tech, USA
3Virginia Tech Carilion School of Medicine, USA
4Faculty of Health Science, Virginia Tech, USA
5Virginia Tech-Wake Forest University School of Biomedical Engineering and Sciences, USA
6Department of Emergency Medicine, Virginia Tech Carilion School of Medicine, USA
7Department of Neurosurgery, Carilion Clinic, USA
8Department of Biological Sciences, Virginia Tech, USA
The dismal prognosis of glioblastoma is, at least in part, attributable to the difficulty in eradicating glioblastoma stem cells (GSCs). However, whether this difficulty is caused by the differential responses of GSCs to drugs remains to be determined. To address this, we isolated and characterized ten GSC lines from established cell lines, xenografts, or patient specimens. Six lines formed spheres in a regular culture condition, whereas the remaining four lines grew as monolayer. These adherent lines formed spheres only in plates coated with poly-2-hydroxyethyl methacrylate. The self-renewal capabilities of GSCs varied, with the cell density needed for sphere formation ranging from 4 to 23.8 cells/well. Moreover, a single non-adherent GSC either remained quiescent or divided into two cells in four-seven days. The stem cell identity of GSCs was further verified bythe expression ofnestin or glial fibrillary acidic protein. Of the two GSC lines that were injected in immunodeficient mice, only one line formed a tumor in two months. The protein levels of NOTCH1 and platelet derived growth factor receptor alpha positively correlated with the responsiveness of GSCs to γ-secretase inhibitor IX orimatinib, two compounds that inhibit these two proteins, respectively. Furthermore, a combination of temozolomide and a connexin 43 inhibitor robustly inhibited the growth of GSCs. Collectively, our results demonstrate that patient-derived GSCs exhibit different growth rates in culture, possess differential capabilities to form a tumor, and have varied responses to targeted therapies. Our findings underscore the importance of patient-derived GSCs in glioblastoma research and therapeutic development for precision medicine.
Biography:
Dr. Sheng obtained his PhD at the State University of New York Downstate Medical Center in 2005. He conducted his postdoc research focusing on delineating cancer cell survival pathways in leukemia and glioblastoma in Dr. Michael Greenʼs laboratory at the University of Massachusetts Medical School. He is currently an assistant professor at the Virginia Tech Carilion Research Institute. His research team has recently identified several new survival pathways in glioblastoma and they are investigating how to translate their findings into precision therapies for glioblastoma.
1The University of Texas MD Anderson Cancer Center, USA
2Baylor College of Medicine, USA
3University of Texas Medical School, USA
Objective: To investigate the association of ED with other malignancies.
Methods: A case-control trial was conducted to investigate prevalence of ED with other malignancies. Cases represented patients who are diagnosed with elastofibeoma (52 patients). Control cases were randomly selected from patients who did CT scan in our institution (150 patients).
Results: 10 ED patients and 15 control patients did not have any neoplastic process. 19 malignant diseases affecting 8 systems were found in ED patients. Hematological malignancies; namely diffuse large B-cell lymphoma (DLBCL) were the most common malignant disease in elastofibroma patients followed by genitourinary malignancies.
56 neoplastic diseases were found in the control group affecting 11 systems; 3 were benign and 53 were malignant. Lung and colon cancers were the most common malignancies in the control group followed by prostate cancer.
ED patients had a significantly higher probability of having hematological malignancies than the control group (P-value = 0.002). ED patients were at a higher risk of having DLBCL than the control group (P-value = 0.029 and 0.001 when using non-cancer and other cancers as a reference respectively).
When genitourinary cancers were used as a reference group for comparison of ED patients with the control group, ED patients were not at a high of having genitourinary cancers (P-value = 0.39 and 0.27, on comparison with non-cancer and other system cancers respectively).
Conclusion: ED patients at a higher risk of developing hematological malignances especially DLBCL and clinical surveillance is needed.
Biography:
Mohamed Elshikh is a postdoctoral fellow in Diagnostic Radiology Department at The University of Texas MD Anderson Cancer Center. He is currently investigating role of CT and PET-CT in assessing treatment response in hematological malignancies patients.
Department of Biochemistry, College of Medicine, University of Saskatchewan, Canada
Breast cancer is a heterogeneous disease that can be stratified based on the expression of molecular markers such estrogen receptor (ER), progesterone receptor and epidermal growth factor receptor 2. The movement toward targeted therapies has led to the development of drugs that block the function of some of these receptors as well as proteins associated with cancer formation and progression, including some non-receptor tyrosine kinases. Breast tumor kinase (BRK) is a non-receptor tyrosine kinase expressed in the majority of human breast tumors and breast cancer cell lines, but its expression has not been detected in normal mammary gland. The overexpression of BRK has been shown to sensitize mammary epithelial cells to mitogenic signaling and to promote cell proliferation and tumor formation. However, there are still several unanswered questions about the cellular and physiological roles of BRK and its clinical implications in breast cancers. I will discuss our recent data highlighting the role of BRK in breast tumor progression, as well as the potential clinical implications of BRK in anti-hormonal drug resistant ER-positive breast cancers.
Biography:
Dr. Kiven Erique Lukong received his Ph.D. degree in biochemistry from the University of Montreal in Canada and pursued his post-doctoral training first at Harvard Medical School, U.S.A. and later at McGill University (Canada). He is currently an Associate Professor in the Department of Biochemistry at the University of Saskatchewan (U of S, Canada) since 2009 and a member of the Cancer Research Cluster at the U of S. Since beginning his independent academic career at the U of S, Dr. Lukonghas obtained career awards from the Saskatchewan Health Research Foundation (SHRF, Top New investigator 2010) and from the Canadian Institutes of Health Research (CIHR, New investigator salary award). Dr. Lukongʼs research broadly involves elucidating the signaling mechanisms that control growth of normal and cancer cells. His lab is investigating the cellular and physiological roles, and the mechanisms of action and modes of regulation of the breast tumor kinase (BRK) family of non-receptor tyrosine kinases in breast cancer and glioblastoma. The Lukong lab is also characterizing the diagnostic, prognostic and therapeutic potential of the BRK family proteins in breast cancer. Dr. Lukong holds or has held funding from SHRF, CIHR and the Canadian Breast Cancer Foundation.
1Genetics Branch, Center for Cancer Research
2Laboratory of Cancer Biology and Genetics, National Cancer Institute, Bethesda Maryland, USA,
3Chemical Biology Laboratory, Center for Cancer Research, National Cancer Institute, Frederick Maryland, USA
5Basic Science Program, Chemical Biology Laboratory, Leidos Biomedical Research Inc., Frederick National Laboratory for Cancer Research, USA
4National Institute of Minority Health and Health Disparities, USA
The C-terminal binding protein (CtBP) is a family of dimeric nuclear proteins whose levels are increased in cancers of the colon, ovaries, prostate and breast. Elevated CtBP expression is associated with poor cancer survival. As a dimer, CtBP provides a scaffold that couples multiple different DNA-binding or DNA bound transcriptional regulators with a variety of chromatin modifying protein complexes to alter the epigenetic landscape throughout the nucleus. These properties provide the rationale for pharmacological targeting of CtBP to alter epigenetically changed and dysregulated genes in cancer cells. We employed computer assisted drug design to screen for optimal quantitative structure-activity relationships (QSARs) between small molecules and CtBP. Functional screening of these compounds identifies 4 lead compounds with low toxicity and high water solubility. Treatment at micro-molar concentrations of these small compounds induces significant de-repression of epigenetically silenced pro-epithelial genes and repression of drug resistance mechanisms in the mesenchymal triple negative breast cancer cell line, MDA-MB-231. This epigenetic re-wiring of gene expression is associated with eviction of CtBP from its respective gene promoters, disrupted recruitment of CtBP-chromatin modifying protein complexes, altered deposition of activating epigenetic histone marks, and upregulation of pro-epithelial gene expression. In functional assays, CtBP inhibition by these small molecule inhibitors disrupts CtBP dimerization, decreases cell migration, abolishes cellular invasion, improves DNA repair, and increases chemotherapeutic drug influx. These findings implicate a broad role for this class of compounds in strategies for therapeutic intervention that will increase the drug efficacy and decrease the acquired resistance to targeted therapeutic intervention through the targeting of CtBP.
Biography:
Dr. Jung S. Byun received her Ph.D. in chemistry and biochemistry from the University of Maryland, College Park. She pursued postdoctoral studies with Dr. Kevin Gardner at NCI, National Institutes of Health. During her postdoctoral residency, Dr. Byun carried out studies to define how histone acetyltransferase, p300, and the elongation factor, ELL, work in concert to control eukaryotic transcription by demonstrating the role of dynamic bookmarking by p300 RNA polymerase II complexes in transcriptional memory. She also discovered a new role for ELL (Eleven-nineteen Lysine-rich Leukemia protein), that it is required for early elongation and facilitating pol II pause site entry. Dr. Byun is currently a staff scientist with Dr. Kevin Gardnerʼs laboratory. The labʼs research interests focus on characterizing other potential transcription regulatory targets important in mammalian cancer cell biology that define a molecular link between metabolic imbalance and breast cancer and how this can modify risk and outcome to decrease health disparities in cancer.
National Institutes of Health, USA
Biography:
Dr. Karen T. Adams has over twenty years of professional practice since receiving her Masters of Science in Nursing from Syracuse University in 1996, and her Doctorate in Nursing from Chamberlain College in 2016. In 2003, after working in a low-income public health clinic and performing volunteer work with the Mission of Mercy in Central Pennsylvania and working as an associate nursing professor at Gettysburg Community College, she joined the Pheochromocytoma/Paraganglioma protocol at the National Institutes of Health in January2004. Dr. KarenAdams helped increase the number of patients treated each year by more than 500%. In addition to her clinical responsibilities, she helped organize the first International Symposium on Pheochromocytoma in 2005, and organized the 1 st National Pheochromocytoma/Paraganglioma Patient Conference in 2006, an event she continues to organize annually. Dr. Adams currently serves as Secretary to the Pheochromocytoma Research Support Organization PRESSOR, an international organization of pheochromocytoma/paraganglioma physicians and researchers. In 2007, Dr. Adams founded the Pheo Para Alliance, a not for profit organization that brings awareness of the disease through advocacy, fundraising, and education. She is on the organizing committee for the 2017 International Symposium on Pheochromocytoma (ISP), which will be held in Sydney, Australia.
Chairman, Chief Scientific Officer &Chief Technology Officer,
ACIAM-BFSRI, USA-Canada-Switzerland-Japan
Cancers initiate and develop from rare population of stem-like cells termed as cancer stem cells (CSC). Our goal is to identify and define the single normal and cancer stem cell of every human tissue in order to succeed in cancer and stem cell therapy, organ engineering, reconstructive and cosmetic surgery. The exact phenotype of CSC and their counterparts in normal mammary gland is not well characterized. We show that CSC are predominantly CD49f + proposing the use of CD44high/CD24low in combination with Ep-CAM/CD49f cell surface markers to further enrich for CSC. Our profiling demonstrates that both normal and breast cancer cells with the CD44high/CD24low phenotype have the highest stem/progenitor cell ability when used in combination with Ep-CAM/CD49f reference markers. Our protocols help understand breast cancer, cancers heterogeneity, drug resistance, towards eradicating the roots of all cancers.
Biography:
Chaker Adra is investigating health, disease, and pioneering the field of organ engineering and regenerative medicine. He is discovering the Laws of Physics & Chemistry as manifested in The Language of Genomes and Living Organisms. He contributed to the emergence of the field of stem cell biology & tissue engineering. He cloned, characterized the family of phosphoglycerate kinase (PGK) genes and pseudogenes. He identified the PGK-1 promoter which has proven to be a powerful and widely used promoter. He designed and constructed The PGK1-Neo Shuttle which is being used around the world for gene therapy, to engineer, from embryonic stem cells, transgenic and knockout animals to understand the causes and mechanisms of all human diseases and find cures. He cloned the pgk-2 gene, showing for the first time that gene duplication, by retroposition more than 100 million years ago, have been used as a mechanism for evolutionary diversification and that mammalian genomes are fluid creating new species. He identified chromosomal regions containing asthma and atopy susceptibility genes. He described functional polymorphisms in Interleukin-4, IL-13 and their receptors, thus making these molecules, with STAT 6, targets for therapeutic treatment of allergic patients and preventive strategies. He discovered several cancer and stem cell specific biomarkers. In a series of groundbreaking experiments, he discovered several universal gene families and biochemical and/or physiological pathways operating in bacteria, yeast, plants, animals and humans (PGK, D4GDI/RhoGDI2/ARHGDIB, RhoGDI3/
ARHGDIG, RTEF-1, HTm4/CD20L/MS4A Gene Family, LAPTM5, SMARCAD1 Helicase Gene Family, and SMARCAD1, The Fingerprints Gene). Dr. Chaker Adra is a philanthropist and the inventor of 19 USA and International Patents.
1Department of Otolaryngology-Head and Neck Surgery, Johns Hopkins School of Medicine, Johns Hopkins University, USA
2Department of Oncology, Johns Hopkins School of Medicine, Johns Hopkins University, USA
A large body of evidence indicates that cancer stem cells (CSCs) is the driving force of tumorigenesis, metastases and treatment resistance. However, the underlying mechanisms responsible for the urothelial CSC traits remain elusive. Here, we show that COX2/PGE2 and YAP1 signaling pathways are required to accelerate SOX2 that acts not only as a critical oncogene linked with malignant stemness properties, but also as a master regulator to govern and maintain urothelial CSCs. Moreover, we identify CD133+/CD24+ as a potent marker to enrich SOX2-expressing CSCs. Mechanistically, COX2/PGE2 signaling induces promoter methylation of let-7 host gene via promoting DNA methyltransferases, resulting in downregulated let-7 expression and subsequent SOX2 expression. YAP1 also activates COX2/PGE2 signaling-independent of SOX2 expression, and these signaling mutually compensate via negative feedback mechanism of SOX2, indicating that dual blockade of these signaling is indispensable to eradicate urothelial CSCs. Combined treatment with COX2 and YAP1 inhibitors elicits long-lasting therapeutic response by subverting CSCs expansion following chemotherapy or EGFR inhibitor for basal type urothelial carcinoma (UC) cells. Thus, our findings provide a rationale to concurrently target these pathways as an effective therapeutic strategy.
Significance
Improvement in survival of UCB has been stagnant over two decades and none of molecular-targeted agents has been approved to date. Here, we show that COX2/PGE2 and YAP1 signaling promotes urothelial CSCs generation via activating SOX2, leading to acquired resistance to systemic therapy such as chemotherapy or EGFR-targeted therapy for basal type UC. Concurrent inhibition of these signaling together with systemic therapy elicits robust therapeutic response by eradicating both the urothelial CSC pool and bulk of tumor, shedding light on progress in an effective therapeutic strategy for UC of bladder, including EGFR-targeted therapy for basal type UC.
Biography:
Dr. Hoque is an Associate Professor of Otolaryngology-Head & Neck Surgery, Urology and Oncology at Johns Hopkins University School of Medicine. His major research interests includes: a) To understand molecular biologic basis of head and neck, lung and genitourinary cancer b) To develop and validate genetic and epigenetic approach for early cancer diagnosis, cancer risk assessment and cancer prognosis and c) To identify molecular alterations due to environmental exposures such as active smoking, passive smoking and arsenic. He has published over 95 papers in reputed journals and has been serving as an editor and/or editorial board member of several bio-medical journals.
Department of Pediatrics, University of Maryland School of Medicine, U.S.A
The diterpenoid lactone andrographolide (AGP) isolated from a plant, Andrographis paniculata, is known to possess multiple pharmacological activities. It has also been demonstrated to possess anticancer activity in vitro and in vivo. Frequent epigenetic silencing of tumor suppressor genes plays a pivotal role in the development of cancer and several recent reports suggest that suppression of RASSF1A is associated with the advanced grade and stage of many cancers including colon cancer. The goal of the present study was to investigate AGP anticancer activity due to the induction of tumor suppressor genes. T84, Colo 205 and HCT-116 colon cancer cells were treated with AGP IC50 and evaluated for expression of tumor suppressor genes by QRT-PCR and immunoblot. Inhibition studies were performed by transfection with gene specific siRNA prior to AGP treatment. AGP induced significantly higher expression of RASSF1A, PTEN, and CDKN2A in colon cancer cells whereas all other tumor suppressor genes tested were either unchanged or suppressed. Similar expression of RASSF1A was also observed in gastric, breast, lung, and prostate cancer cells. Whereas AGP treatment typically down-regulates cyclinD1, transfection of colon cancer cells with RASSF1A specific siRNA resulted in a loss of cyclin D1 suppression. RASSF1A is regulated through the epigenetic methylation of its promoter by DMNT activity which itself is activated by phosphorylated akt. Since Akt is a crucial element of the angiogenesis pathway, we examined the inhibition of this pathway by AGP on T84 and COLO 205 cells. AGP inhibited the transcriptional level of VEGF165 in both cell lines as well as vascular epithelial growth factor receptor 1 (VEGFR1) and VEGFR2. Additionally, downstream events including Akt activation and FoxM1 expression were significantly suppressed by AGP. FoxM1 is known to transactivate PTTG1, a major cause of colon cancer cell metastasis. Consistent with FoxM1 suppression, AGP also decreased transcriptional levels of PTTG1. Furthermore, we elucidated the AGP-dependent up regulation of anti-angiogenic molecule TSP-2, is a potent endogenous inhibitor of angiogenesis. These results demonstrate that AGP is a potent inducer of tumor suppressor genes, most notably RASSF1A and that RASSF1A is largely responsible for the cell cycle arrest induced by AGP treatment. These data also demonstrate the anti-angiogenic activity of AGP which may, through suppression of Akt activation, contribute to the up-regulation of RASSF1A.
Biography:
Aditi Banerjee received her Ph.D. from the University of Kalyani, India, in Zoology. She have a track record of driving advanced research by using a natural or synthetic compound to treat for different types of cancer and have extensive experience in cell biology with a focus on developing biomarkers for preclinical and clinical research against gastric ulcer, rheumatoid arthritis, breast cancer. Her early publications directly addressed in the area of basic and translational inflammatory diseases such as rheumatoid arthritis and gastric ulcer. At present, she is interested in the molecular mechanisms underlying the anticancer properties of phytochemicals andrographolide, labdane diterpenoid. Her current research is probing the effect of andrographolide on growth inhibiting, survival and apoptosis signal transduction pathway in colon cancer cells. In 2016, she joined the Department of Pediatrics, Division of Gastroenterology, and University of Maryland School of Medicine as an Assistant Professor.
Department of Pharmaceutical, Social and Administrative Sciences, School of Pharmacy, DʼYouville College, USA
Gap junctions promote intercellular communication that mediate the passage of molecules up to 1 kDa between cells. These molecules have been demonstrated to either inhibit or promote cell growth, thus defining gap junctions as either tumor suppressors or promoters of growth and metastasis. Although various defining molecular and clinical studies have been reported, there has been limited data to explain these seemingly conflicting results. In this report, the mechanism for how different connexins selectively promote growth through redistribution of cAMP is elaborated. In addition, the selective roles of gap junctions in migration which can affect metastasis is expanded and the key molecular molecules are defined including the mechanism for promotion of the epithelial to mesenchymal transition (EMT) and metastasis. Another role for gapjunctions is to transfer molecules that promote oxidative stress and apoptosis. This occurs by a mechanism known as the bystander effect by which stress applied directly to cells can affect adjacent and distal cells through gap junction communication. This can affect cancer therapy and identify novel ways to target cancer cells with limited side effects. We propose a novel therapeutic approach which has been demonstrated to decrease tumor volume in mice and may have clinical potential.
Biography:
Shoshanna N. Zucker received her PhD in Molecular Pharmacology at Albert Einstein College of Medicine in the laboratory of Dr. Susan B. Horwitz who is well known for the discovery of the mechanism of action of taxol. Dr. Zucker did her postdoctoral work at the University at Buffalo where she focused on gap junctions in cancer. She was a recipient of an NIH NRSA fellowship. She specialized in melanoma research at Roswell Park Cancer Institute where she was a first author of several papers including a Molecular Cell study of oxidative stress in melanoma. In 2013, Dr. Zucker became an Assistant Professor at the DʼYouville School of Pharmacy. Dr. Zucker established her independent research in the area of novel therapeutic approaches to cancer therapy utilizing oxidative stress-inducing mechanisms. She supervises many students and continues active collaborations with the University at Buffalo and Roswell Park Cancer Institute.
1Laboratory of Stem Cell Biology, State Key Laboratory of Biotherapy/Collaborative Innovation Center of Biotherapy, West China Hospital, Sichuan University, China
2Department of Gastrointestinal Surgery, West China Hospital, Sichuan University, China
3Institute of Digestive Surgery, State Key Laboratory of Biotherapy/Collaborative Innovation Center of Biotherapy, West China Hospital, Sichuan University, China
4Laboratory of Gastric Cancer, State Key Laboratory of Biotherapy/Collaborative Innovation Center of Biotherapy, West China Hospital, Sichuan University, China
The supporting tissues, including blood vessels, connection tissues and nerve tissues, are indispensablefor all the steps, such as tumorigenesis, growth, progression and metastasis, of cancer development in human. The extracellular matrix applies essential roles in cancer progress and metastasis. The nervous system acts as a crucial part of cancer microenvironment. Infiltration of nerve fibers into cancer microenvironment plays an important active role in cancer progression. The stimulation of both cancer growth and metastasis by members of nervous system such as neurons and glial cells has been demonstrated. The growth of cancers depends on the formation of blood vessels that provide the supply of nutrients and oxygen. The angiogenesis and vasculogenesis are essential during cancer progression. Previous data show that the glioblastoma stem cells are able to give rise to vascular cells to constitute the functional vessels in tumor tissues. However, which kinds of vascular cells generated from glioblastoma stem cells are largely debated. In addition, there are few evidences to show that the stem cells from other kinds of tumors including carcinoma produce vascular cells to constitute the functional blood vessels in tumor tissues. Therefore, how the components of supporting tissues originate and how the supporting tissues constitute in cancer need to be addressed. Here, we found that a fraction of cancer stem cells (CSCs) derived from patients with gastric carcinoma and colorectal carcinoma are capable to give rise to neurons that are involved in tumor neurogenesis and tumor growth. A single cancer stem cell is able to generate neurons including sympathetic and parasympathetic cells to take part in the nervous system in cancer tissues. Knocking down the neural generating capabilities of the human CSCs inhibited the growth of tumors in the mouse models. We also identified that cancer stem cells of human colorectal carcinomas (CoCSCs) give rise to vascular endothelial cells and compose the vasculatures in cancer tissues. CoCSC derivedendothelial cell incorporated blood vessels were functional. In addition, we identified that theextracellular matrix partially originated from cancer cells. Our data show that many components of supporting tissues originate from the cancer itself and provide an insight to understand how the cancer constitutes when the cancer occurs and progress.
Biography:
Xianming Mo, M.D. is the Professor, Director, Laboratory of Stem Cell Biology, State Key Laboratory of Biotherapy, West China Hospital, Sichuan University. He identified a mechanism how the virus protein v-Myb is involved in the development of leukemia and how Akt pathway is involved in lung carcinomas. He did pioneering work on the cancer stem cells in periphery blood of patients with gastric carcinoma and evaluated the features of the circulating gastric cancer stem cells from patients. He also developed the methods to enrich the cancer stem cells from tumor masses removed from patients with gastric, colon rectal and lung carcinomas for further analysis. Now one of his works focuses on the biology of the cancer stem cells in human patients. He serves as director of Laboratory of Stem Cell Biology, State Key Laboratory of Biotherapy, West China Hospital, Sichuan University in Chengdu, China.
1Pennsylvania State University College of Medicine, USA
2Loma Linda University, USA
B-cell acute lymphoblastic leukemia (B-ALL) is the most common childhood malignancy. High-risk B-ALL remains a therapeutic challenge. Relapse occurs in 20% of B-ALL cases and the overall survival ofrelapsed B-ALL is only 50%. This survival rate has remained unchanged over the last 40 years. Thus, there is an urgent need to understand the pathogenesis of high-risk B-ALL and to develop targeted treatment for this disease. Clinical studies using next-generation sequencing showed that the chance for relapse in B-ALL is increased 12-fold when there is deletion/mutation of one copy of the IKZF1 gene that encodes the Ikaros tumor suppressor protein. Here, we present recent advances in understanding the tumor suppressor function of Ikaros, and the development of targeted therapy that aims to restore Ikaros activity as tumor suppressor. Ikaros is a zinc finger DNA binding protein, that binds to the upstream regulatory elements of its target genes and regulates their transcription. DNA-binding analysis, along with functional studies, showed that Ikarossuppresses leukemia by repressing transcription of genes that are essential for cell cycle progression and for the PI3K signaling pathway. Our results also demonstrated that Ikaros function in B-ALL is impaired by Casein Kinase II (CK2), a pro-oncogenic kinase that directly phosphorylates Ikaros, resulting in the loss of Ikaros activity as a transcriptional regulator. In B-ALL, the ability of Ikaros to control cell cycle progression and the PI3K pathway is impaired by CK2, which is overexpressed in leukemia. Inhibition of CK2 with a novel, specific inhibitor, CX-4945, restoresIkaros function as a regulator of cell cycle progression and PI3K and results in a strong anti-leukemia effect. The therapeutic efficacy of CK2 inhibition and its ability to restore Ikaros tumor suppressor function have been demonstrated in vivo, in preclinical models of high-risk B-ALL. These include primary xenografts derived from patients with high-risk B-ALL, including B-ALL with deletion of one Ikaros allele. In conclusion, this is the first demonstration that Ikaros tumor suppressor function can be reactivated, even in cases of high-risk B-ALL with deletion of a single Ikaros allele. These results present a novel treatment mechanism for high-risk B-ALL – restoration of Ikaros tumor suppressor activity – and provide a mechanistic rationale for the use of CK2 inhibitor for treatment of B-ALL.
Biography:
Dr. Dovat completed his clinical training in Pediatrics at Pennsylvania State University, and in Pediatric Hematology/Oncology at UCLA-Childrenʼs Hospital. He received his research training at Cornell University Graduate School of Medical Sciences and at Howard Hughes Medical Institute at UCLA. As an independent investigator at the University of Wisconsin, Dr. Dovat focused his work on the regulation of the tumor suppression in childhood leukemia. Dr. Dovat is the recipient of The Young Investigator Award by The American Society of Pediatric Hematology/Oncology and has been included in the Best Doctors in America list. Since September 2010, Dr. Dovat has served as the Four Diamond Endowed Chair and Director of Translational Research and Developmental Therapeutics in Pediatric Hematology/Oncology at Pennsylvania State University College of Medicine, Hershey, PA. Dr. Dovatʼs research interests include epigenomic regulation and transcriptional control of cellular immortalization and senescence in leukemia and experimental therapy of malignant diseases.
Department of Biochemistry, School of Life Sciences, Queenʼs Medical Centre, University of Nottingham, UK
Survivin is an essential protein with established roles in mitosis and the inhibition of cell death. It is overexpressed in all cancers, its abundance correlating with tumour resistance to irradiation (IR). In normal cells, survivin expression is confined to the G2 and M phases; however, it is also present during interphase in the nucleus, the cytosol and the mitochondria of cancer cells PE is a phospholipid with a small head-group that facilitates negative curvature of membranes, thereby increasing their accommodation of proteins; thus it is enriched in specific membranes, such as the mitochondrial cristae and the cytokinetic furrow. Here we report the remarkable discovery that mitochondrial survivin regulates PE biosynthesis. The data suggest that survivin can govern mitochondrial integrity and metabolism, cell division and resistance to IR by limiting PE availability. This novel molecular insight suggests that many of the apparently disparate roles of this “multitasking” protein may be fundamentally linked to membrane architecture, and offers a completely unexpected perspective on its contribution to cancer and other metabolic disorders.
Biography:
Sally Wheatley is originally from Scotland, Sally studied Zoology (Bsc hons) at St. Andrews University, before going to University College London where she studied (PhD) cell division cycle mutants in the fission yeast, S. pombe. After several post-doctoral positions, in France, the US and Edinburgh, she was awarded a Cancer Research UK Senior Fellowship and started her independent lab at the University of Sussex (2003-2009), where she focused her work primarily on the mitotic roles of survivin. Since 2009 she has been an Assistant Professor at the University of Nottingham where she teaches Biochemistry, and continues her research into the multiple roles and signaling pathways that involve survivin, from mitochondrial health to tumour metastasis.
Department of Pathology and Anatomical Sciences, University at Buffalo, USA
Due to developments in imaging, there has been a significant diminution to the volume of tissue obtained for diagnostic purposes. While this has been of benefit to the patient, the miniscule amounts of tissue received havebeen strained to keep up with the increasing demands for molecular testing. Most developments in this field have concentrated on modifications to the tissue specimen after it has been fixed in formaldehyde, this despite the fact it has been known for years this fixative negatively impacts the integrity and recovery of nucleic acids. Alternative approaches to processing and triaging diminutive tissue specimens may be needed to address this burgeoning problem in the pathology laboratory. Recently, an up-front step involving washing of the biopsy specimen was incorporated into the processing of the sample and found to be able to recover diagnostic cells for molecular testing. This simple step allowed for the retrieval of unfixed cells that are normally lost during routine processing, yet preserved the tissue core for traditional pathologic analysis. Sufficient amounts of high quality, high molecular weight DNA can be recovered from these cells for molecular testing. To carry these findings to the next step, and as proof of concept, we recently subjected the DNA from these cells to molecular testing on a pre-determined, 144 gene panel. The end goal was to demonstrate the ability to provide informative data that would guide a treating physicianʼs treatment strategies. We found that this triaged approach not only provided a level of molecular testing on par with recommendations, butpreserved the core tissue for enough sections to includeroutine morphologic evaluation, standard immunohistochemical profiling and ancillary testing for immunotherapeutic decisions. By utilizing such a processing approach, a more comprehensive, diagnostic picture can be derived from these traditionally minute tissue sources.
Biography:
Dr. Mojica is a practicing surgical pathologist and Assistant Clinical Professor with the Department of Pathology and Anatomical Sciences at the University at Buffalo. He completed his MD degree from the St. Louis University School of Medicine and is trained and board certified in both Anatomic and Clinical Pathology. He heads the immunohistochemistry section within the Kaleida Health Laboratory. He has published over 30 peer review manuscripts related to translational research and pathologic biospecimens.
Chairman, Chief Scientific Officer & Chief Technology Officer, ACIAM-BFSRI, USA-Canada-Switzerland-Japan
Mesenchymal stem cells have properties that make them amenable to therapeutic use. However, the acceptance of mesenchymal stem cells in clinical practice such as in the treatment of diabetes and autoimmune diseases, cardiovascular disease, cancer therapy, and repair of birth defects require standardized techniques for their specific isolation. To date, there are no conclusive marker (s) for the exclusive isolation of mesenchymal stem cells. Our aim was to identify markers differentially expressed between mesenchymal stem cell and non-stem cell mesenchymal cell cultures. Examination and comparison of the phenotypes of mesenchymal stem cell and non-stem cell mesenchymal cell cultures revealed three differentially expressed markers - CD24, CD108 and CD40. We indicate the importance of establishing differential marker expression between mesenchymal stem cells and non-stem cell mesenchymal cells in order to determine stem cell specific markers, isolate and define Mesenchymal Stem Cells.
Biography:
Chaker Adra is investigating health, disease, and pioneering the field of organ engineering and regenerative medicine. He is discovering the Laws of Physics & Chemistry as manifested in The Language of Genomes and Living Organisms. He contributed to the emergence of the field of stem cell biology & tissue engineering. He cloned, characterized the family of phosphoglycerate kinase (PGK) genes and pseudogenes. He identified the PGK-1 promoter which has proven to be a powerful and widely used promoter. He designed and constructed The PGK1-Neo Vector which is being used around the world for gene therapy, to engineer, from embryonic stem cells, transgenic and knockout animals to understand the causes and mechanisms of all human diseases and find cures. He cloned the pgk-2 gene, showing for the first time that gene duplication, by retroposition more than 100 million years ago, have been used as a mechanism for evolutionary diversification and that mammalian genomes are fluid creating new species. He identified chromosomal regions containing asthma and atopy susceptibility genes. He described functional polymorphisms in Interleukin-4, IL-13 and their receptors, thus making these molecules, with STAT 6, targets for therapeutic treatment of allergic patients and preventive strategies. He discovered several cancer and stem cell specific biomarkers. In a series of groundbreaking experiments, he discovered several universal gene families and biochemical and/or physiological pathways operating in bacteria, yeast, plants, animals and humans (PGK, D4GDI/RhoGDI2/ARHGDIB, RhoGDI3/
ARHGDIG, RTEF-1, HTm4/CD20L/MS4A Gene Family, LAPTM5, SMARCAD1 Helicase Gene Family, and SMARCAD1, The Fingerprints Gene).
Dr. Chaker Adra is a philanthropist and the inventor of 19 USA and International Patents.
*Tom Baker Cancer Centre, ‡, University of Calgary 1331, 29th Street NW, Calgary, Canada. #Calgary Laboratory Services, Calgary, Canada
*Department of pathology, Ohio State University, USA
۴Mayo clinic, Scottsdale, Arizona, USA
Introduction: Multiple myeloma (MM) is a plasma cell neoplasm that is considered incurable. Despite the advent of new agents the majority of MM patients relapse secondary to therapy resistance. The potential of reovirus (RV) as a novel therapeutic agent for MM under in vitro, in vivo and ex vivo conditions has been demonstrated by us and a phase I clinical trial of MM with RV therapy has shown indications of efficacy. Utilizing the syngeneic transplantable Vk*MYC bortezomib (BTZ) resistant MM mouse model, we demonstrate that mice harbouring BTZ insensitive MM tumors significantly respond to RV+BTZ combined treatment better than monotherapy. Our data indicate that this RV+BTZ synergy is manifested via, direct oncolysis in conjunction with enhanced immune activation.
Methods: C57BL/6 wt mice were divided into 2 groups and transplanted with Vk*MYC myeloma (Vk12598) and were treated as follows, (N=8): 1) vehicle control (VC), 2) live reovirus (LV), 3) dead reovirus (DV), 4) BTZ, 5) LV+BTZ, 6) DV+BTZ. Mice in group 1 were sacrificed after 4 days of treatment and their spleens and bone marrow (BM) were formalin fixed and paraffin embedded. These were assessed for CD138+ MM tumour as well as viral RNA and protein in the tumour microenvironment (TME) and a variety of immune correlates as well as apoptotic markers. Mice in group 2 were assessed for serum gamma globulins (M-spike)on a weekly basis and overall survival analysis was conducted.
Results: Mice treated with RV+BTZ demonstrated highly significant (P<0.001) reductions in their M-spikes at 3 and 4 weeks post treatment and superior overall survival (P<0.001). Analysis of tumour viral delivery/replication and immune activation in the TME as early as 4 days post treatment initiation indicated significant (P<0.01) viral replication, caspase 3 activity, CD3+ and NK cell accumulation in the RV+BTZ treatment.
Conclusions: Our data indicate that this RV+BTZ synergy is manifested by enhanced apoptosis, successful viral delivery via tumour associated endothelial and follicular dendritic cells and immune modulation. Since the progression of MM is associated with concomitant immune suppression and drug resistance, these results have significant implications for shaping future clinical trials.
Biography:
Dr. Chandini Thirukkumaran is a Research Associate Professor at the Tom Baker Cancer Centre, University of Calgary, Calgary, Alberta. She received her PhD in microbiology in 1994 from the University of Calgary. Following completion of a post doctoral fellowship in signal transduction at the University of Calgary she joined the Translational Research Laboratories at the Tom Baker Cancer Centre, Calgary as a Research Assistant Professor in 1999. Since then her work has focused on oncolytic viruses as treatment modality for cancer. Presently she is conducting research on multiple myeloma and breast cancer and the effects of oncolytic viruses on immune modulation when given in conjunction with “standard of care therapies” for these malignancies.
Jude Childrenʼs Research Hospital, USA
Antigen-specific CD8 T cells play a critical role in controlling chronic infections and cancer, but progressively lose their effector functions during prolonged antigen exposure. Repression of CD8 T cell effector functions, commonly referred to as T cell exhaustion, limits the ability of the immune system to purge the chronic pathogen from the host. It has recently become recognized that CD8 T cell exhaustion programs can be reinforced and heritably maintained. Therefore in order to develop and/or improve current therapeutic approaches that utilize host antigen-specific T cells to treat chronic infections or cancer a major challenge for the field is to identify mechanisms that stabilize T cell exhaustion. We have recently found that epigenetic modifications acquired in pathogen-specific CD8 T cells during prolonged antigen exposure reinforce T cell exhaustion. Using the LCMV model system of chronic viral infection we investigated the role of Dnmt3a mediated de novo DNA methylation in regulating CD8 T cell exhaustion. Strikingly, conditional deletion of Dnmt3a in activated CD8 T cells blocked the cells from becoming exhausted. Longitudinal analysis of whole-genome methylation programming of WT and Dnmt3a cKO CD8 T cells from chronically infected animals reveals progressive acquisition of Dnmt3a-dependent DNA methylation programs in genes, including interferon gamma, that are coupled to the progressive decline of effector functions. These results have significant implications for therapeutic strategies that utilize reactivation of host pathogen-specific CD8 T cells to control chronic viral infections or cancerand provide a nucleotideresolution map of epigenetic programs progressively acquired during T cell exhaustion.
Biography:
Dr. Benjamin Youngblood, an assistant-member of the Department of Immunology at St Jude Childrenʼs Research Hospital, investigates epigenetic mechanisms that regulate the functional impairment of CD8 T cells during chronic viral infections and cancer. Ben received his bachelor of science in Biochemistry from Oregon State University in 2001 and went on to do his graduate training in Biochemistry studying enzyme specificity of DNA methyltransferases at the University of California Santa Barbara. He joined Professor Rafi Ahmedʼs laboratory in 2007 for postdoctoral training focused on investigating epigenetic regulation of memory CD8 T cell differentiation. In 2014 he joined the faculty at St Jude Childrenʼs Research Hospital.
aSpecialized Chemistry Center, The University of Kansas, USA
bNIH Chemical Genomics Center, National Center for Advancing Translational Sciences, NIH, USA
cDepartment of Cell and Molecular Biology, Northwestern University, Feinberg School of Medicine, USA
dThoracic and GI Oncology Branch, Center for Cancer Research, NCI, USA
eDevelopmental Therapeutics Core facility, Northwestern University and the Robert Lurie Comprehensive Cancer Center, USA
Metastasis is the leading cause of cancer mortality. However, the development of effective anti-cancer drugs able to specifically block metastasis has been hampered by the complexity and poor understanding of the cellular mechanisms that regulate this process. To identify small molecules that selectively target metastatic development, a large diverse chemical library was screened searching for compounds able to eliminate the perinucleolar compartment (PNC). The PNC is a subnuclear structure, whose formation positively correlates with the metastatic potential of cancer cells. PNC prevalence in several cancers inversely correlates with clinical outcome. Metarrestin, a compound obtained through medicinal chemistry optimization of a hit from the screen, disassembles PNCs in cancer cells at submicromolar concentrations and inhibits cancer cell migration and invasion in vitro. In vivo, metarrestin effectively inhibits metastatic growth in murine xenograft models of metastatic disease using human pancreatic, prostate, and breast cancer cells. At doses able to disassemble PNCs, metarrestin selectively disrupts nucleolar structure and inhibits Pol I transcription without affecting Pol II transcription or protein translation and without eliciting DNA damage-repair and apoptotic responses. Affinity purification using a biotin-conjugated analog of metarrestin identified eEF1A as a binding partner. Manipulation of EEF1A levels by overexpression significantly enhance PNCs. Metarrestin is a well-tolerated molecule with a desirable pharmacokinetic profile and a novel mode of action, representing a new therapeutic approach to the treatment of metastatic cancer.
Department of Clinical Science, Intervention and Technology, Karolinska Institutet, Sweden
In the majority of all human cancer cases, the cancer suppressor protein p53 is lost or mutated. p53 belongs to a family of proteins that includes p73 and p63. The latter two can be categorized into two main groups: TA isoforms, which, like p53, act as tumor suppressors; and ΔN isoforms, which act like oncogenes and affect the functions of p53, TAp63, and TAp73.
TP53 mutations lead to gain of function, which promotes more metastatic and fatal disease that are extremely difficult to cure. As reconstitution of p53 suppresses established tumors in vivo, current targeted therapies focus on the activation of p53 but this strategy is still difficult to implement therapeutically. A promising strategy to overcome p53 deficiency and restore p53 pathway functioning is to manipulate the p53 family members, TAp63 and TAp73.
In our on-going efforts we identified small moleculesthat restore the p53 pathway and inhibit proliferation of cancer cells in tumors with various TP53 gene mutations. TAp73 has been identified as a factor that engages pro-apoptotic signaling and inhibits migration of metastatic cancer cells.
We propose a hypothesis that targeting interactions of TAp73 with its inhibitors with simultaneous inhibition of synthetic sick factors to those inhibitors can provide a therapeutic advantage over currently developed strategies to target tumors with TP53 loss or mutations.
Biography:
Dr Joanna Zawacka-Pankau is a Principle Investigatorat KarolinskaInstittuet. She has done her Ph.D. at University of Gdansk, Poland under supervision of Prof. Anna J. Podhajska. Her research focused on activation of p53 tumor suppressor by small molecules and photodynamic therapy in colon cancer. In 2005 she joined Prof. Galina Selivanova Lab from the Department of Microbiology, Tumor and Cell biology, KarolinskaInstitutet as a postdoctoral fellow to study the mechanism and outcome of activation of wild-type p53 by small molecules. Then, she was appointed Assistant Professor at the Department of Biotechnology, Intercollegiate Faculty of Biotechnology, Gdansk, Poland where she focused on exploring the mechanism of tumor suppression upon pharmacological activation of p53 family members in p53 deficient and mutant tumors.
In 2012 she took up a position of Assistant Professor at the Department of Microbiology, Tumor and Cell Biology and in 2016 she joined the Department of Clinical Science, Intervention and Technology.
1Cooper Medical School of Rowan University, Department of Obstetrics and Gynecology, Division of Reproductive Endocrinology & Infertility, Camden, NJ
2Cooper Institute for Reproductive Hormonal Disorders, P.C., Mt. Laurel, NJ
There is evidence that rapidly growing cancer cells, similar to rapidly growing trophoblast cells utilize a unique protein, not present in normal tissue, to help evade immune surveillance. This protein known as the progesterone induced blocking factor (PIBF) has been found to stabilize perforin granules in natural killer (NK) cells, thus abrogating their mechanism for cytolysis and help cause a shift of TH1 to TH2 cytokines. PIBF has been found to be overexpressed in biopsies of uterus, breast, stomach, and brain cancer and in several cancer cell lines including leukemia, glioblastoma multiforme, and adenocarcinoma of the ovary, cervix, and breast. The parent form of PIBF measures 90 kDa and is associated with centrosome on chromosome 13 in the vicinity of BRCA-1 and P53. Isoforms of PIBF are produced by alternative splicing and includes ones measuring 34 kDa, 57 kDa, 67 kDa. Progesterone has been found to up-regulate the 34 kDa splice variant of PIBF on human leukemia cell lines and the 57 kDa isoform in human glioblastoma cells lines. PIBF, though present intracellularly in both the rapidly growing trophoblast cells and cancer cells, one distinction between pregnancy vs. cancer is that serum PIBF rises abruptly after progesterone exposure (even when not pregnant) in the serum but not increased in the serum even in tumors that are positive for progesterone receptors or even BRCA-1 breast cancer, which by making a mutated ubiquitin is associated with diminished capacity to degradate the progesterone receptor. Adding the progesterone receptor modulator mifepristone to culture media causes down-regulation of the 34 isoforms in leukemia and glioblastoma multiforme cell lines. However, mifepristone fails to lower serum PIBF. There is evidence that suppressing the conversion of the 90 kDa nuclear parent form to the intracellular isoforms can provide significant palliative benefit to a large variety of metastatic human cancers including colon, renal cell carcinoma, small and non-small cell lung cancer, glioblastoma multiforme, breast cancer, transitional cell carcinoma of the renal/pelvis and thymic epithelial cell cancer. It is suggested, but not proven for sure, that the mechanism for causing improved longevity and quality of life by retarding tumor growth is by inhibiting the production of intracellular PIBF which allows natural killer cells (and possibly T-cells also) to attack the cancer cells. Measuring serum PIBF does not appear to be a worthwhile test to determine who would benefit from mifepristone treatment nor the knowledge of progesterone receptor status.
Biography:
Jerome H. Check, M.D., Ph.D. has been a Professor of Obstetrics and Gynecology and Division Head of Reproductive Endocrinology and Infertility at Cooper Medical School of Rowan University (formerly known as University of Medicine and Dentistry of Robert Wood since 1989. He is also board certified in internal medicine and medical endocrinology and metabolism. He received his Ph.D. in reproductive biology in 1997 and his thesis was
“The role of progesterone in promoting implantation and inhibiting spontaneous abortions may be through the stimulation of immunomodulatory proteins”. He has published over 750 publications in peer review journals involving obstetrics/gynecology, reproductive and medical endocrinology and infertility, internal medicine, and cancer research. Much of his present cancer research relates to his concept published in the journal Medical Hypothesis in 2011 entitled “A model for potential tumor immunotherapy based on the knowledge of immune mechanism responsible for spontaneous abortion.
MD Anderson Cancer Center (Houston-Texas), USA
Introduction: Cancer immunotherapy is one of the best therapies compared to traditional therapies that may cause potential toxicities such as chemotherapy and radiation. The potential use of immunotherapy is to restore the immune system of patients in attempt to stimulate it to reject and destroy cancer cells. With the recent approval of the monoclonal antibodies against CTLA-4 and PD-1 for the treatment of melanoma, renal carcinoma cancer and non-small cell lung have attracted wide interest for strategies that enhance T-cell-mediated response against cancer. A complex network of biological pathways governs interactions between the immune system and cancer cells. The balance of signaling via co-inhibitory or co-stimulatory molecules expressed on T cells has demonstrated to be a powerful approach to intensify antitumor immune responses. This approach has been used effectively for the generation of a new class of anticancer therapies called checkpoint-blocking antibodies. Exploiting on the success of CTLA-4 blockade, agents that target a second co-inhibitory receptor, PD-1 (Programmed cell death protein 1), or its ligand, PD-L1, are in clinical development.
Research: The presence of several inhibitory pathways that block T cell responses offers particular strategies for mobilizing the immune system to attack cancer cells. There are some strategies to modulate the microenvironment - targeting regulatory cells, blocking differentiation or recruitment, blocking immunosuppressive enzymes, regulatory cell depletion, re-programming immunosuppressive cells, modifying the chemokine and cytokine profile are some examples. The attractively of new strategies for immunotherapy is driven by immune response and microenvironment discovery. Usually, scientists have relied on conventional laboratory research tools to identify several biomarkers, for example, altered genes transcription factors changes in mRNA and protein expression. To put these cancer biomarkers in the context the researchers can use several strategies to find a good parameter to take care of patient and drug development. As more and more immunotherapies are made available, the overall goal will be to screen patients and determine which of the immunotherapies will be more effective for each cancer type and each patient, including the analysis of new immune cell population.
Results: Currently there are several Clinical Trials across more than 20 different cancers including, melanoma, ovarian, prostate, breast, lung, gastric, kidney, bladder, cervical, anal, colorectal and pancreatic cancers, as well as in leukemia, lymphoma, sarcoma and glioblastoma. Inhibitory molecules like CTLA-4, PD-1, LAG-3, TIM-3, VISTA and BTLA besides co-stimulatories molecules such as ICOS, OX40 and 4-1BB are potent agents for combination therapy in order to improve antitumor responses. The analysis of tissue and blood samples from cancer patients is being conducted with new technologies as Flow Cytometry (FACS) and mass cytometry (Cytof). Here, we will share some strategies in order to pursuit molecules that could help us to better understand cancer immunotherapy responses.
Conclusion: A harmonized struggle to assess the value biomarkers that address different aspects of the cancer-immunity cycle in T cell checkpoint blockade will allow us to integrate information on individual aspects of tumor-immune interaction.
Biography:
Dr. Jorge Augusto Borin Scutti is currently Research Scientist of Immunotherapy Platform (Immunology Department) at the MD Anderson Cancer Center (Houston-Texas). As Research Scientist hisworks focuses onanalyzing the activity of innate and adaptive cell populations like T cells, B cells, tumor cells, Myeloid Derived Suppressor Cells (MDSC) and Natural Killer (NK) cells that are critical on immune response against cancer and then might regulate positively or negatively T-cell responses. Dr. Scutti earned his Master and PhD in Microbiology and Immunology Department at Federal University of São Paulo (UNIFESP) working on cancer vaccines and peptides derived proteins to stimulate immune system against melanoma. Postdoctoral at MD Anderson Cancer Center (MDACC) - Pediatrics Department, where he began evaluating pediatrics cancer - DIPG (Diffuse Intrinsic Glioma Pontine) its microenvironment, Natural killer cells and histone deacetylase inhibitors (iHDAC) as cancer immunotherapy tool. Experience in cancer immunology and immunotherapy in experimental studies and clinical research.
1SE “Dnipropetrovsk medical academy of Health Ministry of Ukraine”
Department of oncology and medical radiology
VolodymyrVernadskii str., 9, Dnipro, 49044, Ukraine
Background: Breast cancer is the most common cancer diagnosed among women in the world. Current information on the prognostic importance of body mass index (BMI) for patients withbreast cancer is based on a variety of equivocal reports. Few have data on BMI in relationship to systemictreatmenthas not been explored so far. The aim of this retrospective study is to evaluate the relation between patientsʼ Breast cancer to Obesity and the prognosis of treatment.
Materials and Methods: The study included 130 patients with breast cancer between the ages of 30 and 77 (57,6 ± 1) years of age who were treated according to our clinic, department of oncology and medical radiology. Dnipropetrovsk medical academy at Municipal Institution “Dnipropetrovsk City Multi-field Clinical Hospital #4”, Dnepropetrovsk state medical academyfrom 2005-2015. All patients were evaluated according to the following data: stage of the disease, age and BMI at the time of diagnosis, the size, histological typeand metastases. Tumor size was evaluated after measuring its maximal diameter and distributed in accordance with the International TNM-classification (7th edition, 2009). The histological type and degree of differentiation of the tumor was evaluated respectively by the National Standards of diagnostics and treatment of malignant neoplasms, reflecting the recommendations of leading international organizations. BMI is calculated by the formula: I = m×h2, where m - body weight (kg); h - height (m). According to these calculations the patients were divided in accordance with the WHO criteria into the following groups: those with a BMI <25 kg/m2 - normal or underweight; from 25 to 29.9 kg/m2 - overweight; > 30 kg/m2 - obese. The material for the histopathological study was obtained during surgery. We examined the relative risk of relapse and death with regard to the BMIcategories adjusting for eight factors known to be predictors of disease-freesurvival (DFS) and overall survival (OS): menopausal status, nodal status tumor size, vessel invasion, estrogen receptor (ER) status, progesterone receptorstatus, tumor grade and treatment regimens.
Results: In this retrospective study, among 130 patients with breast cancer, 45% were identified with excess body weight, and 31% - of various obesity degree. Patients with a BMI <25 kg/m2 were significantly more diagnosed with stage 2 breast cancer triple negative. BMI> 30 kg/m2, 10% more often associated with metastatic RLN, which is anindirect sign of higher metastatic potentials. Patients with normal BMI had significantly longer overall survival (OS) and disease-free survival (DFS) than patients with intermediate or obese BMI in pairwise comparisons adjusted for other factors. We found a strong correlation betweenobesity and lymph node involvement These observationssuggest that obesity may potentiate the metastatic spread of breast tumors. Distant metastases were also foundmore often in obese patients in bone or visceral sites in patients <45 years of age at diagnosis.
Conclusions: In conclusion, this retrospective investigation our patient demonstrates that BMI is an independent prognostic factor for OS in patients with breast cancer. We have supporting evidencethat obese BMI represents a poor risk feature for outcome, especially in pre-/premenopausal patients, most of whom receivedchemotherapy without hormonal therapy.
Keywords: body mass index, breast cancer, obesity, overall survival
Biography:
Mohammad Hojouj is an Assistant Professor, MD, MSo, Oncologist, Master of medicine, a member of The National Comprehensive Cancer Network NCCN, a member of the European Association of Physicians in Germany (NGO), member of the international conference, Speaker of the international conference in the United Arab Emirates 2015, a member of the Association of Arab doctors in Ukraine. Actual Member of the American Association of Clinical Oncology (ASCO). Has experience of more than 9 international clinical researches as Sub investigator. He gives great attention to the educational process, organization and conduction of clinical trials in oncology practice.