Research Article
Investigation of Area under the Curves for Insulin Secretion in Diabetes
Running title: AUC of insulin secretion in diabetes
1 Tokushima University/Medical Research, Tokushima, Japan
2 Japan Low Carbohydrate Diet Promotion Association, Kyoto, Japan
3 Takao Hospital, Kyoto, Japan
4 Muneta Maternity Clinic, Chiba, Japan
5 Department of Nutrition and Metabolism, Institute of Biomedical Sciences, Tokushima University, Graduate School, Tokushima, Japan
6 Anti-Aging Medical Research Center, Graduate School of Life and Medical Sciences, Doshisha University, Kyoto, Japan
*Corresponding author: Hiroshi Bando, Tokushima University /Medical Research, Nakashowa 1-61, Tokushima 770-0943, Japan, Cell: +81-90-3187-2485 E-mail: pianomed@bronze.ocn.ne.jp
Received: July 11, 2018 Accepted: July 15, 2018 Published: July 20, 2018
Citation: Bando H, Ebe K, Muneta T, Bando M, Yonei Y. Investigation of Area under the Curves for Insulin Secretion in Diabetes. Int J Biotechnol Recent Adv. 2018; 1(1): 24-29. doi: 10.18689/ijbr-1000105
Copyright: © 2018 The Author(s). This work is licensed under a Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Background
Concerning diabetic nutritional therapy, Calorie Restriction (CR) and Low Carbohydrate Diet (LCD) have been on discussion. Authors continue clinical research related to CR, LCD, Morbus(M) value and insulin secretion.
Subjects and Methods
Subjects were 42 patients (63.4 years on average) with type 2 diabetes mellitus (T2DM) with its immunoreactive insulin (IRI) =<5µU/mL. Methods included CR breakfast with carbohydrate 70g (Carbo70), Insulinogenic Index (IGI) calculation and daily profile of blood glucose.
Results
Subjects showed median data; M value 207, HOMA-R 1.0, Delta Ratio of IGI for Carbo70 is 0.12 [0.08–0.22], Area under the Curves (AUC) Ratio of IGI-Carbo70 is 3.0 [2.2-4.8]. Divided into 3 groups due to HbA1c, median glucose and M value was 133mg/dL, 227 mg/dL, 345mg/dL and 15.8, 207, 587, respectively. Delta and AUC Ratio of IGICarbo70 in 3 groups were 0.17, 0.10, 0.10and5.2, 2.9, 1.9, respectively. There were significant correlations between M value and Delta ratio / AUC ratio, in which the latter has higher degree of significance.
Discussion and Conclusion
Among 3 groups, the distribution was overlapped in Delta-IGI, and was rather divided in AUC-IGI. Consequently, the latter method seems to be rather superior. These results would be the fundamental data, and further development of research is expected.
Keywords: Area Under the Curves (AUC), Insulinogenic index (IGI), type 2 diabetes mellitus (T2DM), Morbus value (M value), Delta ratio of IGI, AUC ratio of IGI
Abbreviation
AUC: Area under the Curve
IGI: Insulinogenic Index
T2DM: Type 2 diabetes mellitus
M value: Morbus value
IRI: immunoreactive insulin
Introduction
On the historical point of view, noteworthy medical problems have changed from infectious diseases to noncommunicable diseases. For some decades, metabolic syndrome (Met-S) has been more prevalent worldwide [1,2,3]. They are crucial medical and social problems with lots of influencing factors such as lifestyle, age, meal, exercise, habitual status, socioeconomic status, and others [4]. Met-S has increasing and leading to several arteriosclerotic diseases such as hypertension and diabetes [5].
As to Diabetes, it is also increasing rapidly in developed countries and also developing countries. It has macro- and micro-angiopathic complications, including large vessels of brain, heart, lower leg, as well as retinopathy, neuropahy and nephropaphy [6].
For diabetes management, there have been recently changes of comments from medical society such as American Diabetes Association (ADA) and American College of Physicians (ACP) [7, 8]. The main point for the controversy was concerning the ideal HbA1c level in various situations. On contrast, standards of medical care were proposed by International Diabetes Federation (IDF). Among them, the intake and counting amount for carbohydrate would be emphasized [9].
The problem of carbohydrate intake has been continued for long. Nutritional therapy for diabetes can be generally classified into 2 patterns. One is Calorie Restriction (CR) diet, and another is Low Carbohydrate Diet (LCD) [10,11].The former means fat and calorie restriction, and the latter means decreased amount of carbohydrate which has been known for its clinical effects such as weight reduction and others.
Originally, LCD was initiated by Bernstein and others in Western countries, and has been spread widely after that [12]. On contrast in Japan, authors and colleagues began LCD in early period [13]. We have treated lots of diabetic patients on LCD, and continued to present clinical research on CR and LCD [14, 15]. Moreover, we had reported the efficacy of LCD, useful three types of LCD (super, standard, petit), pathphysiological role of ketone bodies in the axis of fetus, placenta, newborn and pregnant mother [16].
Through our clinical research on CR and LCD, we have provided formula diet of CR and LCD and performed the examination. Taking the most advantages of our research protocol, we have reported the trial of breakfast including 70g of carbohydrate for the evaluation of pancreas function, similar to 75g OGTT [17]. In previous study, we analyzed the method using the Delta (increment) of glucose and immunoreactive insulin (IRI).
In current study, we have developed the research furthermore, by calculating by area under the curves (AUC) for the responses of blood glucose and IRI. The purpose of this report would be the comparison of the analysis methods between AUC and Delta, as well as the comparison of the meal tolerance test (MTT) developing in recent clinical studies.
Subjects and Methods
In this study, subjects were 42 patients with type 2 diabetes mellitus (T2DM). They were admitted to the hospital for further evaluation and treatment for T2DM. As to the background of the patients, we enrolled the subjects who are compatible to the following condition: i) the diagnosis is T2DM, ii)T1DM or slow progressive type of DM are excluded, iii) IRI is 5µU/mL and less than 5 IU/ml in the morning after overnight fasting, iv) body mass index (BMI) is 35 and less than 35. According to the value of HbA1c, subjects were divided into 3 groups and analyzed.
Methods are on our protocol for diabetes with the meal of CR and LCD. In this study, the following procedures were used as follows.
- As to our research protocol, patients are to take CR on day 1 and 2, and LCD after day 3, with 1400 cal/day each. This study includes carbohydrate loading test on day 2 and daily profile of blood glucose 7 times a day on day 2.
- After overnight fasting on the morning of Day 2, basal biomarkers were measured such as complete blood count, liver and kidney function, lipids, blood glucose, IRI and so on.
- After drawing blood samples, patients took breakfast with 70g of carbohydrate. Regarding this breakfast, its PFC ratio was protein 15%, fat 25%, carbohydrate 60%, with 1400 kcal/day. It is along to the standard guideline in nutritional therapy which was proposed by Japan Diabetes Society (JDS) [18].
- Thirty minutes after breakfast, blood sample was drawn for blood glucose and IRI. During 30 minutes from the breakfast, patients were told to keep still on sitting position.
- Daily profile of blood glucose was investigated on Day 2. The clock time was 08, 10, 12, 14, 17, 19, 22h, 7 times a day. Average blood glucose value and also Morbus(M) value were calculated.
Ratio of insulin/glucose response
From the data of glucose and IRI on 0 and 30 min, two ratios were calculated and investigated.
Insulinogenic index (IGI) has been known to evaluate insulin secretion and pancreas function. Its formula is delta (increment) of insulin (30min – 0 min) / delta (increment) of blood glucose (30min – 0min). In this paper, we call it ‘Delta Ratio of IGI for Carbo70’.
In response to glucose loading, IRI and glucose increase. Another evaluating method includes usage of Area under the Curves (AUC) of the both. The ratio between IRI and glucose would be called as ‘AUC Ratio of IGI for Carbo70’.
From described above, two ratios are defined in the following. Delta Ratio of IGI for Carbo70 is calculated as (IRI at 30min – IRI at 0min) (µU/mL) / (Glucose at 30min – Glucose at 0min) (mg/dL).
Similarly, AUC Ratio of IGI for Carbo70 is calculated as (AUC of IRI for 0-30min) (µU/mL x h)/ (AUC of glucose for 0-30min) (mg/dL x h).
Daily profile of blood glucose
Regarding to the glucose variability, we checked the daily profile of blood glucose on day 2 for 7 times a day. The clock time was 08, 10, 12, 14, 17, 19, 22h. According to these data, average blood glucose in a day on Day 2 and also M value were calculated. There were previous data concerning the comparison between sampling of 7 times and 20 times. From this result, both would have compatible data with similar data from continuous glucose monitoring (CGM) [19-21].
Morbus value
Morbus (M) value has been known as one of the biomarker indicating average blood glucose level and also the mean amplitude of glycemic excursions (MAGE) [22, 23]. In other words, it can suggest how high the blood glucose is and how large the swinging degree of blood glucose is. The level of M value is calculated by the method of logarithmic transformation, which means the deviation of glucose from ideal glucose value [23, 24].
The formula of the M value is as follows: Firstly, M = MBS + MW: M value is the total of MBS and MW. In addition, MW is maximum blood glucose-minimum glucose)/20. Thirdly, MBS is the mean of MBSBS. Summarized above, MBSBS is the individual M-value for each blood glucose, calculated as (absolute value of [10 × log (blood glucose level/120)])3 [22-24].
Generally, the obtained data of the M value is evaluated in the following: less than 180 would be normal range, from 180 to 320 would be borderline, more than 320 would be abnormal.
Statistical analysis
In this study, obtained data were shown by mean and standard deviation, and also the median and quartile of 25% / 75% due to the biomarkers. The latter are described as median [25%–75%]. Regarding the statistical calculation, we used the correlation coefficients, according to the Spearman test, which has been utilized on analytical evaluation [25].
Ethical Standard
Current research was conducted in compliance with the ethical principles based upon the Declaration of Helsinki. Moreover, additional commentary was performed in 2004 General Assembly Tokyo, Japan. It was conducted with Personal Information Protection Law and in reference to “Standards for the Implementation of Clinical Trials (GCP), an ordinance of the Ministry of Health, Labour and Welfare No. 28 of March 27, 1997. In addition, there was the “Ethical Guidelines for Epidemiology Research” by the Ministry of Education, Culture, Sports, Science and Technology and the Ministry of Health, Labour and Welfare.
Authors and colleagues had an ethical committee including physician, nurse, pharmacist and other experts in the legal specialty. We have discussed and confirmed that current study is valid and agreed with all members. Moreover, informed consents and written paper agreements have been taken from the subjects. This study has been registered by National University Hospital Council of Japan (ID: #R000031211).
Results
Basal data
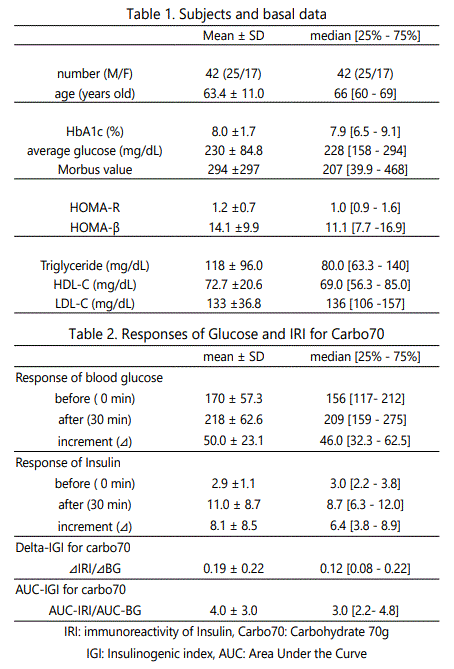
Basal data of the subjects were shown in Table 1. Average data was 63.4 years in age, 8.0% in HbA1c, 230 mg/dL in glucose, respectively. Median data was 207 in Morbus value, 1.0 in HOMA-R, 80 mg/dL in Triglyceride, respectively. Responses of Glucose and insulin for Carbo70 were shown in Table 2. From the data of 0 min and 30 min, Delta Ratio of IGI for Carbo70 and AUC ratio of IGI for Carbo70 were 0.12[0.08–0.22] and 3.0 [2.2-4.8], respectively.
Comparison among 3 groups
Subjects were divided into 3 groups due to the value of HbA1c with 14 cases each. HbA1c value in Low, Middle and High group was 5.4%–6.8%, 6.9%-8.5% and 8.6%-11.8%, respectively. Median value was 6.3%, 7.9% and 9.8%, respectively.
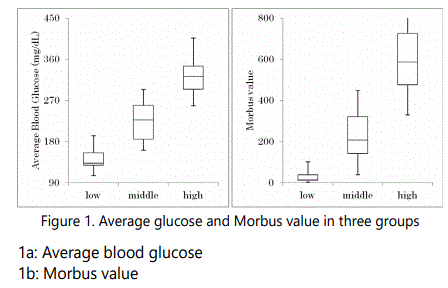
Glucose and Morbus value in three groups were shown in Figure 1. In the 3 groups, the median level in average glucose was 133mg/dL, 227 mg/dL and 345 mg/dL, respectively. The median level in M value was 15.8, 207, 587, respectively.
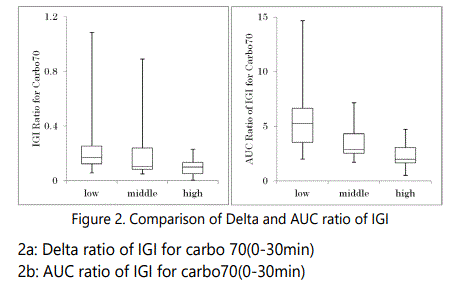
Delta ratio of IGI for Carbo70 and AUC ratio of IGI for Carbo70 in 3 groups were shown in Figure 2. In the 3 groups, the median level in Delta ratio of IGI was 0.17, 0.10, and 0.10, respectively. Similarly, the median level in AUC ratio of IGI was 5.2, 2.9, 1.9, respectively. Compared the distribution of the data in both ratios, the former revealed rather overlapped, while the latter revealed rather clear difference among 3 groups.
Delta ratio vs AUC ratio
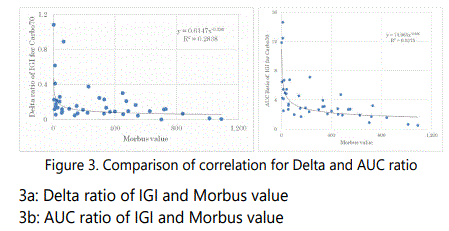
Correlations between M value and Delta ratio of IGI / AUC ratio of IGI were shown in Figure 3.There were significant correlations in both, where Delta ratio is p<0.05, and AUC ratio is p<0.01. The latter has higher degree of significance.
Discussion
Concerning diabetes, research for pathophysiological function and practice for nutritional treatment have been important and crucial for future therapy. In these aspects, authors have continued clinical practice for lots of patients with T2DM so far. Authors and colleagues have developed useful LCD meal education through the activity of Japan Low Carbohydrate Diet Promotion Association [13]. For example, we proposed three types of LCD for everyone. They are petitLCD, standard-LCD, super-LCD. These 3 LCD include the ratio of carbohydrate as 40%, 26%, 12%, respectively.
Regarding the medical research reports about diabetes, LCD and CR, we have already investigation from several aspects including the usefulness of M value [14, 15, 26].
Our previous achievements have been involved in this report. In the case of CR diet, breakfast has 70g of carbohydrate due to the standard CR formula by Japanese Diabetes Association (JDA) [18]. This carbohydrate load seems to stimulate the responses of glucose and insulin to the enough degree, although it includes not only carbohydrate but also fat and protein.
Thus, the research for diabetic patients using the meal of CR and LCD has been performed so far. It always included the analyses of useful biomarker of the M value, which represents both average blood glucose level and the mean amplitude of glycemic excursions (MAGE) [17, 27].
Regarding current study, biomarkers were classified into three groups due to HbA1c value and investigated. In the box plot analysis for average blood glucose, the median glucose in 3 groups was 133 mg/dL, 227 mg/dL, 345 mg/dL, respectively. These median value and also quartile values (25% and 75%) indicate that the distribution of 3 groups would be divided in rather satisfactory degree with less overlapped region, suggesting the compatible relationship between HbA1c and average blood glucose.
In the case of M value, the median level in 3 groups was 15.8, 207, 587, respectively. The characteristic point of M value would be the large difference in numerical values. This is from the mathematic reason of the M value, in which the degree of elevated glucose and increased swinging of glucose are described. It is useful for us to evaluate by one numerical value for two factors.
There are some differences of distribution of 3 groups in Delta ratio and in AUC ratio, respectively. In Delta ratio of IGI, 3 groups seem to be rather overlapped. On the other hand, In AUC ratio of IGI, 3 groups seems to be rather divided. From these difference, both research ways have been useful in the clinical research, but AUC ratio seems to be a little superior to Delta ratio as an analysis method of IGI.
Several methods are available for examining the insulin response to carbohydrate loading in order to examine pancreatic function or secretion of insulin [28]. Conventionally, Intravenous Glucose Tolerance Test (IVGTT) and oral glucose tolerance test (OGTT) has been widely known [29]. In recent years, a method of ingesting a meal including protein, fat and carbohydrate has been introduced and adopted in clinical practice and research.
This research method has been called as a mixed-meal test (MMT). There was a representative report of MMT [30]. Participants ingested high-protein Boost-HP (237ml, Vevey, Switzerland) consisting of 33 g of carbohydrate, 15 g of protein, and 6 g of fat. This liquid has the PFC ratio which is 25:20:55. In this report, patients with positive auto antibodies showed the results that Delta IGI for Carbo 33g would be 1.6 in average.
In addition to MMT, there is another technical term, meal tolerance test (MTT). This is similar to 75g oral glucose tolerance test (GTT). There were MTT reports for the clinical research studies [31]. MTT has been usually provided as breakfast. One example of breakfast of MTT includes 450 kcal including PFC = 15:35:50, with salt 1.6g [31]. Calculated from this information, carbohydrate dose would be estimated 56g in the served breakfast.
In other MTT report, the protocol was that breakfast of 500-kcal meal with 55% carbohydrate was given to patients with T2DM [32]. The amount of carbohydrate 69g is similar to our protocol with 70g of carbohydrate. Then, these data would become useful reference in comparison with our data. According to their results, glucose and IRI (0 to 30min) would be 167 to 230mg/dL, 12 to 37µU/mL, respectively. Calculated from these, Delta ratio of IGI is 0.39, and AUC ratio of IGI is 12.3. These data seems to be similar to our results in the low HbA1c group.
There is a recent report during 120 min for OGTT [33]. According to the responses of glucose and insulin, subjects were categorized into four groups, which are normal, insulinlate, insulin/glucose-late and insulin-very late. The results showed that AUC-glucose significantly differed among 4 groups, but AUC-IRI did not significantly differed [33]. These findings could become reference data for the future MTT research.
Regarding the limit of our research, several factors would be considered. Our study is involved in the analyses for the insulin secretion concerning the study in this area. However, the existence of insulin resistance will be explored, using some relevant biomarkers. For example, both HOMA-R and HOMA-ß will be applied to the investigation. Consequently, the relationship among related factors would be explored in the future study.
Conclusion
In summary, we examined the reaction of blood glucose and insulin for a meal containing 70g of carbohydrate utilizing standard CR breakfast. Although Delta and AUC analyses are both meaningful, the latter method may be somewhat with superiority. These results would be the fundamental related data in this field, and further development of related research is expected.
Acknowledgement
In regard to this report, some part was presented at 90th Annual Congress of Japan Diabetes Society (JDS), Tokyo, 2018. The authors appreciate all staffs and patients for their understanding and cooperation.
Conflicts Of Interest
The authors declare that they have no conflicts of interest.
References
- Varghese JF, Patel R, Yadav UCS. Novel Insights in the Metabolic Syndromeinduced Oxidative Stress and Inflammation-mediated Atherosclerosis. Curr Cardiol Rev. 2018; 14(1): 4-14. doi: 10.2174/1573403X13666171009112250
- Yamagishi K, Iso H. The criteria for metabolic syndrome and the national health screening and education system in Japan. Epidemiol Health. 2017; 39: e2017003. doi: 10.4178/epih.e2017003
- Reaven GM. Role of insulin resistance in human disease. Diabetes. 1988; 37(12): 1595-607.
- Cornier MA, Dabelea D, Hernandez TL, Lindstrom RC, Steig AJ, et al. The metabolic syndrome. Endocr Rev. 2008; 29(7): 777-822. doi: 10.1210/er.2008-0024
- Mendonça FM, de Sousa FR, Barbosa AL, Martins SC, Araújo RL, et al. Metabolic syndrome and risk of cancer: which link?. Metabolism. 2015; 64(2): 182-9. doi: 10.1016/j.metabol.2014.10.008
- Ojo O. An overview of diabetes and its complications. Diabetes Res Open J. 2016; 2(2): e4-e6.
- American College of Physicians. Clinical Guidelines and Recommendations. 2017.
- American Diabetes Association. Pharmacologic Approaches to Glycemic Treatment: Standards of Medical Care in Diabetes. Diabetes Care. 2018; 41(Suppl 1): S73-S85. doi: 10.2337/dc18-S008
- International Diabetes Federation (IDF). Standards of Medical Care in Diabetes. Diabetes Care. 2015; 38: S1-S94.
- Accurso A, Bernstein RK, Dahlqvist A, Draznin B, Feinman RD, et al. Dietary carbohydrate restriction in type 2 diabetes mellitus and metabolic syndrome: time for a critical appraisal. Nutr Metab. 2008; 5: 9. doi: 10.1186/1743-7075-5-9
- Meng Y, Bai H, Wang S, Li Z, Wang Q, et al. Efficacy of low carbohydrate diet for type 2 diabetes mellitus management: A systematic review and meta-analysis of randomized controlled trials. Diabetes Res Clin Pract. 2017; 131: 124-131. doi: 10.1016/j.diabres.2017.07.006
- Bernstein RK. Dr. Bernstein’s Diabetes Solution. Little.Brown and company, New York. 1997.
- Ebe K, Ebe Y, Yokota S, Matsumoto T, Hashimoto M, et al. Low Carbohydrate diet (LCD) treated for three cases as diabetic diet therapy. Kyoto Medical Association Journal. 2004; 51: 125-129.
- Bando H, Ebe K, Muneta T, Bando M, Yonei Y. Effect of low carbohydrate diet on type 2 diabetic patients and usefulness of M-value. Diabetes Res Open J. 2017; 3(1): 9-16.
- Ebe K, Bando H, Yamamoto K, Bando M, Yonei Y, et al. Daily carbohydrate intake correlates with HbA1c in low carbohydrate diet (LCD). J Diabetol. 2018; 1(1): 4-9.
- Muneta T, Kawaguchi E, Nagai Y, Matsumoto M, Ebe K, et al. Ketone body elevation in placenta, umbilical cord, newborn and mother in normal delivery. Glycative Stress Research. 2016; 3(3): 133-140. doi: 10.24659/gsr.3.3_133
- Bando H, Ebe K, Muneta T, Bando M, Yonei Y, et al. Proposal for Insulinogenic Index (IGI)-Carbo70 as Experimental Evaluation for Diabetes. J Clin Exp Endocrinol. 2017; 1: 102.
- Japan Diabetes Association. Diabetes clinical practice guidelines Based on scientific evidence. 2013.
- Siegelaar SE, Holleman F, Hoekstra JBL, Devries JH. Glucose Variability; Does It Matter? . Endocrine Reviews. 2010; 31(2): 171-182. doi: 10.1210/er.2009-0021
- Moberg E, Kollind M, Lins PE, Adamson U. Estimation of blood-glucose variability in patients with insulin-dependent diabetes mellitus. Scand J Clin Lab Invest. 1993; 53: 507-514. doi: 10.3109/00365519309092547
- McDonnell CM, Donath SM, Vidmar SI, Werther GA, Cameron FJ, et al. A novel approach to continuous glucose analysis utilizing glycemic variation. Diabetes Technol Ther. 2005; 7: 253-263. doi: 10.1089/dia.2005.7.253
- Service FJ, Molnar GD, Rosevear JW, Ackerman E, Gatewood LC, et al. Mean amplitude of glycemic excursions, a measure of diabetic instability. Diabetes. 1970; 19: 644-655. doi: 10.2337/diab.19.9.644
- Molnar GD, Taylor WF, Ho MM. Day-to-day variation of continuously monitored glycaemia: A further measure of diabetic instability. Diabetologia. 1972; 8(5): 342-348. doi: 10.1007/BF01218495
- Schlichtkrull J, Munck O, Jersild M. The M-value, an index of blood sugar control in diabetics. Acta Med Scand. 1965; 177: 95-102. doi:10.1111/j.0954-6820.1965. tb01810.x
- Yanai H. Four steps excel statistics. 4th Edition, Seiun-sha Publishing Co. Ltd, Tokyo. 2015.
- Bando H, Ebe K, Muneta T, Bando M, Yonei Y, et al. Urinary C-Peptide Excretion for Diabetic Treatment in Low Carbohydrate Diet (LCD). Journal of Obesity and Diabetes. 1: 13-18.
- Monnier L, Colette C, Owens DR. Glycemic variability: The third component of the dysglycemia in diabetes. Is it important? How to measure it? . J Diabetes Sci Technol. 2008; 2(6): 1094-1100. doi: 10.1177/193229680800200618
- Cersosimo E, Solis-Herrera C, Trautmann ME, Malloy J, Triplitt CL, et al. Assessment of pancreatic ß-cell function: review of methods and clinical applications. Curr Diabetes Rev. 2014; 10(1): 2-42.
- Veijola R, Koskinen M, Helminen O, Hekkala A. Dysregulation of glucose metabolism in preclinical type 1 diabetes. Pediatr Diabetes. 2016; 17(22): 25-30. doi: 10.1111/pedi.12392
- Bacha F, Gungor N, Lee S, delas Heras J, Arslanian S. Indices of insulin secretion during a liquid mixed-meal test in obese youth with diabetes. J Pediatr. 2013; 162(5): 924-9. doi: 10.1016/j.jpeds.2012.11.037
- Yoshino G, Tominaga M, Hirano T, Shiba T, Kashiwagi A, et al. The test meal A:A pilot model for the international standard of test meal for an assessment of both postprandial hyperglycemia and hyperlipidemia. J Jpn Diabetes Soc. 2006; 49: 361-371. doi: 10.11213/tonyobyo.49.361
- Cozma LS, Luzio SD, Dunseath GJ, Underwood PM, Owens DR. Beta-cell response during a meal test: a comparative study of incremental doses of repaglinide in type 2 diabetic patients. Diabetes Care. 2005; 28(5): 1001-7. doi: 10.2337/diacare.28.5.1001
- Takahashi K, Nakamura H, Sato H, Matsuda H, Takada K, et al. Four Plasma Glucose and Insulin Responses to a 75g OGTT in Healthy Young Japanese Women. J Diabetes Res. 2018; 30; 2018: 5742497. doi: 10.1155/2018/5742497


